Abstract
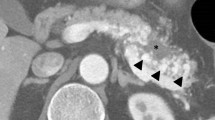
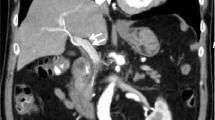
A 60-year-old man with an unruptured cerebral aneurysm and family history of moyamoya disease was admitted to our hospital with epigastric pain since the previous day. Serum levels of pancreatic enzyme were elevated and abdominal contrast-enhanced computed tomography showed localized enlargement of the pancreatic tail in the arterial phase and revealed numerous areas of fine mesh-like vascular hyperplasia consistent with an enlarged pancreatic tail. We diagnosed pancreatic arteriovenous malformation (P-AVM) with acute pancreatitis. Furthermore, in the pancreatic body, endoscopic ultrasonography showed lobularity (honeycombing type) and hyperechoic foci (non-shadowing), which suggests chronic pancreatitis. Acute management was performed with conservative treatment including administration of replacement fluids and proteolytic enzyme inhibitor. Distal pancreatectomy for P-AVM was performed because P-AVM is associated with acute pancreatitis recurrence, development of portal hypertension, progression of chronic pancreatitis, and refractory duodenal bleeding. Histological findings on the resected specimens revealed the anastomosis of abnormal arteries and veins, which suggested P-AVM. In addition, inflammation accompanied by fat necrosis due to ischemic infarction in the pancreatic tail, which suggested acute pancreatitis, and mild fibrosis in the pancreatic body, which suggested chronic pancreatitis, were shown. Although P-AVM is associated with various complications, symptomatic P-AVM should be considered a chronic and progressive disease.





Similar content being viewed by others
References
Halpern M, Turner AF, Citron BP. Hereditary hemorrhagic telangiectasia. An angiographic study of abdominal visceral angiodysplasias associated with gastrointestinal hemorrhage. Radiology. 1968;90:1143–9.
Kanno A, Satoh K, Kimura K, et al. Acute pancreatitis due to pancreatic arteriovenous malformation: 2 case reports and review of the literature. Pancreas. 2006;32:422–5.
Song KB, Kim SC, Park JB, et al. Surgical outcomes of pancreatic arteriovenous malformation in a single center and review of literature. Pancreas. 2012;41:388–96.
Chou SC, Shyr YM, Wang SE. Pancreatic arteriovenous malformation. J Gastrointest Surg. 2013;17:1240–6.
Gomes AS, Mali WP, Oppenheim WL. Embolization therapy in the management of congenital arteriovenous malformations. Radiology. 1982;144:41–9.
Ohtani N, Kimoto K, Yoshida S, et al. Pancreatic arteriovenous malformation with pancreatitis involving a pancreatico-venous fistula. Gastroenterol JPN. 1992;27:115–20.
Koito K, Namieno T, Nagakawa T, et al. Congenital arteriovenous malformation of the pancreas: its diagnostic features in images. Pancreas. 2001;22:267–73.
Aida K, Nakamura H, Kihara Y, et al. Duodenal ulcer and pancreatitis associated with pancreatic arteriovenous malformation. Eur J Gastroenterol Hepatol. 2002;14:551–4.
Lee M, Marusawa H, Yamashita Y. Education and imaging. Gastrointestinal: recurrent pancreatitis due to pancreatic arteriovenous malformation. J Gastroenterol Hepatol. 2015;30:2.
Cassinotto C, Lapuyade B. Pancreatic arteriovenous malformation embolization with onyx. J Vasc Interv Radiol. 2015;26:442–4.
Frenk NE, Chao TE, Cui J, et al. Staged particle and ethanol embolotherapy of a symptomatic pancreatic arteriovenous malformation. J Vasc Interv Radiol. 2016;27:1734–5.
Yokoe M, Takada T, Mayumi T, et al. Japanese guidelines for the management of acute pancreatitis: Japanese Guidelines 2015. J Hepatobiliary Pancreat Sci. 2015;22:405–32.
Shovlin CL, Guttmacher AE, Buscarini E, et al. Diagnostic criteria for hereditary hemorrhagic telangiectasia (Rendu–Osler–Weber syndrome). Am J Med Genet. 2000;91:66–7.
Sato K, Monden K, Ueki T, et al. A case of pancreatic arteriovenous malformation indentified by investigating the cause of upper abdominal pain associated with acute pancreatitis (in Japanese). Nihon Shokakibyo Gakkai Zasshi. 2016;113:1223–9.
Kume K, Masamune A, Ariga H, et al. Alcohol consumption and the risk for developing pancreatitis: a case–control study in Japan. Pancreas. 2015;44:53–8.
Samokhvalov AV, Rehm J, Roerecke M. Alcohol consumption as a risk factor for acute and chronic pancreatitis: a systemic review and a series of meta-analyses. EbioMedicine. 2015;2:1996–2002.
Whitcomb DC, Frulloni L, Garg P, et al. Chronic pancreatitis: an international draft consensus proposal for a new mechanistic definition. Pancreatology. 2016;16:218–24.
Kloppel G, Maillet B. Chronic pancreatitis: evolution of the disease. Hepatogastroenterology. 1991;38:408–12.
Whitcomb DC. Value of genetic testing in the management of pancreatitis. Gut. 2004;53:1710–7.
Takiguchi N, Ichiki N, Ishige H, et al. Pancreatic arteriovenous malformation involving adjacent duodenum in a patient with gastrointestinal bleeding. AM J Gastroenterol. 1995;90:1151–4.
Ikezaki K, Han DH, Kawano T, et al. A clinical comparison of definite moyamoya disease between South Korea and Japan. Stroke. 1997;28:2513–7.
Liu W, Morito D, Takashima S, et al. Identification of RNF213 as a susceptibility gene for moyamoya disease and its possible role in vascular development. PLoS One. 2011;6:e22542.
Bang OY, Ryoo S, Kim SJ, et al. Adult Moyamoya disease: a burden of intracranial stenosis in East Asians? PLoS One. 2015;30:e0130663.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical standards
All procedures followed have been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments.
Informed consent
Informed consent was obtained from the patient for being included in the study.
Rights and permissions
About this article
Cite this article
Seike, T., Komura, T., Shimizu, Y. et al. A case of chronic pancreatitis exacerbation associated with pancreatic arteriovenous malformation: a case report and literature review. Clin J Gastroenterol 12, 135–141 (2019). https://doi.org/10.1007/s12328-018-0901-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12328-018-0901-1