Abstract
Background
We analyzed the clinical and radiographic evolution of patients with knee unicompartmental osteoarthritis and axis alteration and osteochondral lesions in the femoral condyle, treated with tibial plateau and meniscus allograft and cultured autologous chondrocyte implantation in the femur in two steps.
Purpose
To analyze the clinical results with the first patients treated with this two-stage technique to avoid knee prosthesis in patients with unicompartmental osteoarthritis.
Material and methodology
Sixteen patients, average age 56 years, were included in a cohort study. We performed an osteotomy with tibia plateau allograft, including the meniscus. In a second surgery, the chondrocyte fibrin scaffold was placed in the femur. Clinical symptoms and function were measured using KSSR and KOOS scores. Wilcoxon's test was performed to compare the results over the 2-year follow-up period.
Results
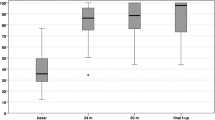
Mean KSSR before surgery was 35.69 (SD: 3.75) points, rising to 67 (SD: 15.42) at 3 months, 95.88 at 12 months (SD: 2.68) and 96.31 at 24 months (SD: 2.24). The KOOS before surgery was 65.14 (SD: 16.34), rising to 72.68 after 3 months (SD: 19.15), 76.68 at 12 months (SD: 18.92) and 64.28 at 24 months (SD: 11.79). Four of 5 patients returned to engaging in the activity that they had stopped practicing. Three patients experienced collapse of the tibia allograft, and they needed later a prosthesis.
Conclusions
Simultaneous tibia plateau allograft and autologous chondrocyte implantation in the femur, after correction of the angular deformity, were performed, restoring the anatomy of the medial compartment and knee function in 82% of the patients 2 years after the operation.
Level of evidence
IV.




Similar content being viewed by others
References
Bhan S, Malhotra R, Kiran EK, Shukla S, Bijjawara M (2005) A comparison of fixed bearing and mobile-bearing total knee arthroplasty at a minimum follow-up of 4.5 years. J Bone Jt Surg (Am) 87-A:2290–2296
Coventry MB (1965) Osteotomy of upper portion of the tibia for degenerative arthritis of the knee a preliminary report. J Bone Jt Surg (Am) 47-A:984–990
Insall J, Shoji H, Mayer V (1974) High tibial osteotomy: a five-year evaluation. J Bone Jt Surg (Am) 56:1397–1405
Luna-Pizarro D, Moreno-Delgado F, De la Fuente-Zuno JC, Meraz-Lares G (2012) Distal femoral dome varus osteotomy: surgical technique with minimal dissection and external fixation. Knee 19:99–102. https://doi.org/10.1016/j.knee.2011.01.005
Gardiner A, Richmond JC (2013) Periarticular osteotomies for degenerative joint disease of the knee. Sports Med Arthrosc 21:38–46. https://doi.org/10.1097/JSA.0b013e31826d2f5d
Backstein D, Morag G, Hanna S, Safir O, Gross A (2007) Long-term follow-up of distal femoral varus osteotomy of the knee. J Arthroplasty 22(Suppl 1):2–6
Moseley JB, O’Malley K, Petersen NJ, Menke TJ, Brody BA, Kuykendall DH et al (2002) A controlled trial of arthroscopic surgery for osteoarthritis of the knee. N Engl J Med 347:81–88
Shasha N, Krywulak S, Backstein D, Pressman A, Gross AE (2003) Long-term follow-up of fresh tibial osteochondral allografts for failed tibial plateau fractures. J Bone Jt Surg (Am) 85-A(Suppl 2):33–39
Hurley ET, Davey MS, Jamal MS, Manjunath AK, Kingery MT, Alaia MJ et al (2020) High rate of return-to-play following meniscal allograft transplantation. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-020-05956-z
Toanen C, Dhollander A, Bulgheroni P, Filardo G, Zaffagnini S, Spalding T et al (2020) Polyurethane meniscal scaffold for the treatment of partial meniscal deficiency: 5-year follow-up outcomes: a european multicentric study. Am J Sports Med 8:1347–1355. https://doi.org/10.1177/0363546520913528
Searle H, Asopa V, Coleman S, McDermott I (2020) The results of meniscal allograft transplantation surgery: what is success? BMC Musculoskelet Disord 21:159. https://doi.org/10.1186/s12891-020-3165-0
Puzzitiello RN, Liu JN, Garcia GH, Redondo ML, Christian DR, Yanke AB et al (2020) Return to sport and outcomes after concomitant lateral meniscal allograft transplant and distal femoral varus osteotomy. Arthroscopy 36:253–260. https://doi.org/10.1016/j.arthro.2019.07.022
Rucinski K, Cook JL, Crecelius CR, Stucky R, Stannard JP (2019) Effects of compliance with procedure-specific postoperative rehabilitation protocols on initial outcomes after osteochondral and meniscal allograft transplantation in the knee. Orthop J Sports Med. https://doi.org/10.1177/2325967119884291
Abolghasemian M, León S, Lee PTH, Safir O, Backstein D, Gross AE (2019) Long-term results of treating large posttraumatic tibial plateau lesions with fresh osteochondral allograft transplantation. J Bone Jt Surg Am 101:1102–1108. https://doi.org/10.2106/JBJS.18.00802
Gross AE, Shasha N, Aubin P (2005) Long-term followup of the use of fresh osteochondral allografts for posttraumatic knee defects. Clin Orthop Relat Res 435:79–87
Krettek C, Clausen J, Omar M, Noack S, Neunaber C (2017) Two-stage late reconstruction with a fresh large osteochondral shell allograft transplantation (FLOCSAT) for a large ostechondral defect in a non-union after a lateral tibia plateau fracture 2-year follow up. Injury 48:1309–1318. https://doi.org/10.1016/j.injury.2017.05.010
Bullens PH, Minderhoud NM, de Waal Malefijt MC, Veth RP, Buma P, Schreuder HW (2009) Survival of massive allografts in segmental oncological bone defect reconstructions. Int Orthop 33:757–760. https://doi.org/10.1007/s00264-008-0700-2
Anract P, Coste J, Vastel L, Jeanrot C, Mascard E, Tomeno B (2000) Proximal femoral reconstruction with megaprosthesis versus allograft prosthesis composite: a comparative study of functional results, complications and longevity in 41 cases. Rev Chir Orthop Reparatrice Appar Mot 86:278–288
Felson DT (2000) Osteoarthritis: new insights. Part 1: the disease and its risk factors. Ann Intern Med 133:635–646
Loughlin J, Dowling B, Mustafa Z, Southam L, Marcelline L, Räinä SS et al (2002) Association of the interleukin-1 gene cluster on chromosome 2q13 with knee osteoarthritis. Arthritis Rheum 46:1519–1527
Ball S, Amiel D, Williams SK, Tontz W, Chen AC, Sah RL et al (2004) The effects of storage on fresh human osteochondral allografts. Clin Orthop Rel Res 418:246–252
Forriol F, Longo UG, Alvarez E, Campi S, Ripalda P, Rabitti C et al (2011) Scanty integration of osteochondral allografts cryopreserved at low temperatures with dimethyl sulfoxide. Knee Surg Sports Traumatol Arthrosc 19:1184–1191
Gharedaghi M, Taghi Peivandi M, Mazloomi M, Shoorin HR, Hasani M, Seyf P et al (2016) Evaluation of clinical results and complications of structural allograft reconstruction after bone tumor surgery. Arch Bone Jt Surg 4:236–242
Mora G, Alvarez E, Ripalda P, Forriol F (2003) Articular cartilage degeneration after frozen meniscus and achilles tendon allograft transplantation: experimental study in sheep. Arthroscopy 19:833–841
Niinimäki TT, Eskelinen A, Mann BS, Junnila M, Ohtonen P, Leppilahti J (2012) Survivorship of high tibial osteotomy in the treatment of osteoarthritis of the knee: finnish registry-based study of 3195 knees. J Bone Jt Surg (Br) 94-B:1517–1521. https://doi.org/10.1302/0301-620X.94B11.29601
Williams SK, Amiel D, Ball S, Allen RT, Wong VW, Chen AC et al (2003) Prolonged storage effects on the articular cartilage of fresh human osteochondral allografts. J Bone Jt Surg (Am) 85-A:2111–2120
Minas T (2001) Autologous chondrocyte implantation for focal defects of the knee. Clin Orthop Rel Res 391(Suppl):S349–S361
Getgood A, Gelber J, Gortz S, De Young A, Bugbee W (2015) Combined osteochondral allograft and meniscal allograft transplantation: a survivorship analysis. Knee Surg Sports Traumatol Arthrosc 23:946–953. https://doi.org/10.1007/s00167-015-3525-8
Peterson L, Minas T, Brittberg M, Nilsson A, Sjögren-Jansson E, Lindahl A (2000) Two- to 9-year outcome after autologous chondrocyte transplantation of the knee. Clin Orthop Rel Res 374:212–234
Richardson JB, Caterson B, Evans EH (1999) Repair of human articular cartilage after implantation of autologous chondrocytes. J Bone Jt Surg (Br) 81B:1064–1068
Assenmacher AT, Pareek A, Reardon PJ, Macalena JA, Stuart MJ, Krych AJ (2016) Long-term outcomes after osteochondral allograft: a systematic review at long-term follow-up of 12.3 years. Arthroscopy 32:2160–2168. https://doi.org/10.1016/j.arthro.2016.04.020
Johal S, Nakano N, Baxter M, Hujazi I, Pandit H, Khanduja V (2018) Unicompartmental knee arthroplasty: the past, current controversies, and future perspectives. J Knee Surg 31:992–998. https://doi.org/10.1055/s-0038-1625961
Chawla H, Ghomrawi HM, van der List JP, Eggman AA, Zuiderbaan HA, Pearle AD (2017) Establishing age-specific cost-effective annual revision rates for unicompartmental knee arthroplasty: a meta-analysis. J Arthroplasty 32:326–335. https://doi.org/10.1016/j.arth.2016.08.019
Hamilton TW, Pandit HG, Jenkins C, Mellon SJ, Dodd CAF, Murray DW (2017) Evidence-based indications for mobile-bearing unicompartmental knee arthroplasty in a consecutive cohort of thousand knees. J Arthroplasty 32:1779–1785. https://doi.org/10.1016/j.arth.2016.12.036
Tyagi V, Farooq M (2017) Unicompartmental knee arthroplasty: indications, outcomes, and complications. Conn Med 81:87–90
Murray DW, Parkinson RW (2018) Usage of unicompartmental knee arthroplasty. Bone Jt J 100-B:432–435. https://doi.org/10.1302/0301-620X.100B4.BJJ-2017-0716.R1
El-Galaly A, Kappel A, Nielsen PT, Jensen SL (2019) Revision risk for total knee arthroplasty converted from medial unicompartmental knee arthroplasty: comparison with primary and revision arthroplasties, based on mid-term results from the Danish knee arthroplasty registry. J Bone Jt Surg Am 101:1999–2006. https://doi.org/10.2106/JBJS.18.01468
Santoso MB, Wu L (2017) Unicompartmental knee arthroplasty, is it superior to high tibial osteotomy in treating unicompartmental osteoarthritis? a meta-analysis and systemic review. J Orthop Surg Res 12:50. https://doi.org/10.1186/s13018-017-0552-9
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest for this study.
Ethical approval
The study was approved by the Ethical Committee of Hospital Universitario Dr. Jose E. González, Universidad Autónoma de Nuevo León (UANL), Monterrey, N.L., Mexico (approval included). All procedures performed in studies involving human participants were in accordance with the ethical standards of the Institutional Research Committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
The patients clinical study was performed in the Hospital Universitario Dr. Jose E. González, Universidad Autónoma de Nuevo León (UANL), Monterrey, N.L., Mexico. Prof. Forriol was in this university for a long time to prepare the chondrocyte culture and surgical technique details.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Álvarez-Lozano, E., Luna-Pizarro, D., Meraz-Lares, G. et al. Two-stage bone and meniscus allograft and autologous chondrocytes implant for unicompartmental osteoarthritis: midterm results . Musculoskelet Surg 106, 133–143 (2022). https://doi.org/10.1007/s12306-020-00680-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12306-020-00680-w