Abstract
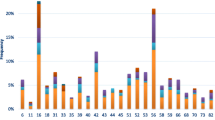
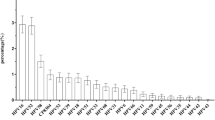
Although cytology screening has reduced the incidence and mortality rate of cervical cancer significantly, its usefulness is limited to samples from the site of the lesion, resulting in its low sensitivity and unsuitability for use in medical checkups. The purpose of the present study was to evaluate the prevalence of HPV infection using genotype distribution and to analyze the correlation of the HPV DNA test results with cytological results. We also evaluated the benefits of quantitative information obtained from cyclic-catcher melting temperature analysis (CMTA) in screening for cervical cancer. We performed cyclic-CMTA using Anyplex™ II HPV28 Detection in combination with cervical cytology for 2,181 subjects. The following HPV positivity types were detected using cyclic-CMTA and HPV positivity was found to increase together with the severity of the cytology results: (1) For 419 HPV positive specimens, HPV DNA was detected in 18.1% of normal specimens, 78.3% of ASCUS, and all of LSIL and HSIL; (2) high-risk HPV DNAs were detected in 63.3% of normal (N=547), 65.9% of ASCUS (N=41), 76.9% of LSIL (N=13), and 88.9% of HSIL (N=9) among total detected HPV DNA regardless multiple detection; (3) multiple HPV genotypes were detected in 4.8% of normal specimens (N=2,146), 52.2% of ASCUS (N=23), 57.1% of LSIL (N=7), and 40.0% of HSIL (N=5). In addition, a high level of viral DNA was observed using cyclic-CMTA in all specimens beyond the LSIL stage according to cytology, while only 6% of specimens with normal cytology showed a correlation with viral quantitation by cyclic-CMTA. The combination of HPV genotyping with a quantitative assay and cytology will allow for a more accurate diagnosis of cervical cancer.
Similar content being viewed by others
References
Bachtiary, B., Obermair, A., Dreier, B., Birner, P., Breitenecker, G., Knocke, T.H., Selzer, E., and Pötter, R. 2002. Impact of multiple HPV infection on response to treatment and survival in patients receiving radical radiotherapy for cervical cancer. Int. J. Cancer102, 237–243.
Bae, J.H., Lee, S.J., Kim, C.J., Hur, S.Y., Park, Y.G., Lee, W.C., Kim, Y.T., Ng, T.L., Bock, H.L., and Park, J.S. 2008. Human papillomavirus (HPV) type distribution in Korean women: a meta-analysis. J. Microbiol. Biotechnol.18, 788–794.
Bulkmans, N.W., Berkhof, J., Bulk, S., Bleeker, M.C., van Kemenade, F.J., Rozendaal, L., Snijders, P.J., and Meijer, C.J. 2007. POBASCAM Study Group. High-risk HPV type-specific clearance rates in cervical screening. Br. J. Cancer96, 1419–1424.
Burd, E.M. 2003. Human papillomavirus and cervical cancer. Clin. Microbiol. Rev.16, 1–17.
Chen, H.C., Schiffman, M., Lin, C.Y., Pan, M.H., You, S.L., Chuang, L.C., Hsieh, C.Y., Liaw, K.L., Hsing, A.W., Chen, C.J., and CBCSP-HPV Study Group. 2011. Persistence of type-specific human papillomavirus infection and increased long-term risk of cervical cancer. J. Natl. Cancer Inst.103, 1387–1396.
Dalstein, V., Riethmuller, D., Prétet, J.L., Le Bail Carval, K., Sautière, J.L., Carbillet, J.P., Kantelip, B., Schaal, J.P., and Mougin, C. 2003. Persistence and load of high-risk HPV are predictors for development of high-grade cervical lesions: a longitudinal French cohort study. Int. J. Cancer106, 396–403.
Ho, G.Y., Bierman, R., Beardsley, L., Chang, C.J., and Burk, R.D. 1998. Natural history of cervicovaginal papillomavirus infection in young women. N. Engl. J. Med.338, 423–428.
Ho, G.Y., Burk, R.D., Klein, S., Kadish, A.S., Chang, C.J., Palan, P., Basu, J., Tachezy, R., Lewis, R., and Romney, S. 1995. Persistent genital human papillomavirus infection as a risk factor for persistent cervical dysplasia. J. Natl. Cancer Inst.87, 1365–1371.
Hwang, I.T. 2012. Cyclic-CMTA: An innovative concept in multiplex quantification. Seegene Bulletin1, 11–15.
Jung, K.W., Park, S., Kong, H.J., Won, Y.J., Lee, J.Y., Seo, H.G., and Lee, J.S. 2012. Cancer statistics in Korea: Incidence, Mortality, Survival, and Prevalence in 2009. Cancer Res. Treat.44, 11–24.
Kim, Y.T. 2009. Current status of cervical cancer and HPV infection in Korea. J. Gynecol. Oncol.20, 1–7.
Lee, D.H. 2012. TOCE: Innovative Technology for High Multiplex Real-time PCR. Seegene Bulletin1, 5–10.
Nobbenhuis, M.A., Walboomers, J.M., Helmerhorst, T.J., Rozendaal, L., Remmink, A.J., Risse, E.K., van der Linden, H.C., Voorhorst, F.J., Kenemans, P., and Meijer, C.J. 1999. Relation of human papillomavirus status to cervical lesions and consequences for cervical-cancer screening: a prospective study. Lancet354, 20–25.
Oh, J.K., Franceschi, S., Kim, B.K., Kim, J.Y., Ju, Y.H., Hong, E.K., Chang, Y.C., Rha, S.H., Kim, H.H., Kim, J.H., andet al. 2009. Prevalence of human papillomavirus and Chlamydia trachomatis infection among women attending cervical cancer screening in the Republic of Korea. Eur. J. Cancer Prev.18, 56–61.
Sasagawa, T., Basha, W., Yamazaki, H., and Inoue, M. 2001. High-risk and multiple human papillomavirus infections associated with cervical abnormalities in Japanese women. Cancer Epidemiol. Biomarkers Prev.10, 45–52.
Sasieni, P.D., Cuzick, J., Lynch-Farmery, E., The National Co-ordinating Network for Cervical Screening Working Group. 1996. Estimating the efficacy of screening by auditing smear histories of women with and without cervical cancer. Br. J. Cancer73, 1001–1005.
Saslow, D., Solomon, D., Lawson, H.W., Killackey, M., Kulasingam, S.L., Cain, J., Garcia, F.A.R., Moriarty, A.T., Waxman, A.G., Wilbur, D.C., andet al.; the ACS-ASCCP-ASCP Cervical Cancer Guideline Committee. 2012. American Cancer Society, American Society for Colposcopy and Cervical Pathology, and American Society for Clinical Pathology Screening Guidelines for the prevention and early detection of cervical cancer. CA Cancer J. Clin.62, 147–172.
Shin, H.R., Franceschi, S., Vaccarella, S., Roh, J.W., Ju, Y.H., Oh, J.K., Kong, H.J., Rha, S.H., Jung, S.I., Kim, J.I., andet al. 2004. Prevalence and determinants of genital infection with papillomavirus, in female and male university students in Busan, South Korea. J. Infect. Dis.190, 468–476.
Shin, H.R., Lee, D.H., Herrero, R., Smith, J.S., Vaccarella, S., Hong, S.H., Jung, K.Y., Kim, H.H., Park, U.D., Cha, H.S., andet al. 2003. Prevalence of human papillomavirus infection in women in Busan, South Korea. Int. J. Cancer103, 413–421.
Shin, H.R., Park, S., Hwang, S.Y., Kim, J.E., Jung, K.W., Won, Y.J., Hwang, S.S., Yim, S.H., Choi, K.S., Park, E.C., andet al. 2008. Trends in cervical cancer mortality in Korea 1993-2002: Corrected mortality using national death certification data and national cancer incidence data. Int. J. Cancer122, 393–397.
Snijders, P.J., van den Brule, A.J., and Meijer, C.J.L.M. 2003. The clinical relevance of human papllomavirus testing: relationship between analytical and clinical sensitivity. J. Pathol.201, 1–6.
Trottier, H., Mahmud, S., Costa, M.C., Sobrinho, J.P., Duarte-Franco, E., Rohan, T.E., Ferenczy, A., Villa, L.L., and Franco, E.L. 2006. Human papillomavirus infections with multiple types and risk of cervical neoplasia. Cancer Epidemiol. Biomarkers Prev.15, 1274–1280.
Walboomers, J.M.M., de Rosa Husman, A.-M., Snijders, P.J.F., Stel, H.V., Risse, E.K.J., Helmerhorst, T.J.M., Voorhorst, F.J., and Meijer, C.J.L.M. 1995. Human papillomavirus in false negative archival cervical smears: implications for screening for cervical cancer. J. Clin. Pathol.48, 728–732.
Wallin, K.L., Wiklund, F., Angström, T., Bergman, F., Stendahl, U., Wadell, G., Hallmans, G., and Dillner, J. 1999. Type-specific persistence of human papillomavirus DNA before the development of invasive cervical cancer. N. Engl. J. Med.341, 1633–1638.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Supplemental material for this article may be found at http://www.springerlink.com/content/120956.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Kim, YJ., Kwon, MJ., Woo, HY. et al. Prevalence of human papillomavirus infection and genotype distribution determined by the cyclic-catcher melting temperature analysis in Korean medical checkup population. J Microbiol. 51, 665–670 (2013). https://doi.org/10.1007/s12275-013-3160-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12275-013-3160-3