Abstract
Adenosine triphosphate (ATP) is well-known as a universal source of energy in living cells. Less known is that this molecule has a variety of important signaling functions: it activates a variety of specific metabotropic (P2Y) and ionotropic (P2X) receptors in neuronal and non-neuronal cell membranes. So, a wide variety of signaling functions well fits the ubiquitous presence of ATP in the tissues. Even more ubiquitous are protons. Apart from the unspecific interaction of protons with any protein, many physiological processes are affected by protons acting on specific ionotropic receptors—acid-sensing ion channels (ASICs). Both protons (acidification) and ATP are locally elevated in various pathological states. Using these fundamentally important molecules as agonists, ASICs and P2X receptors signal a variety of major brain pathologies. Here we briefly outline the physiological roles of ASICs and P2X receptors, focusing on the brain pathologies involving these receptors.
Similar content being viewed by others
Introduction
Since water is an essential attribute of life, protons are essential ions for the most fundamental biological processes such as pH homeostasis, synaptic transmission, and the mitochondrial respiratory chain [1]. Slight fluctuations in intracellular or extracellular pH can have marked effects on protein function, synaptic vesicle trafficking, and the electrical machinery of neuronal and glial cells [1]. Apart from nonspecific interactions with biological molecules, numerous physiological processes are triggered by protons acting on their highly specific effectors—acid-sensing ion channels (ASICs) [2, 3].
Adenosine triphosphate (ATP) is well known to be a universal source of energy in cells. Less known, but also a very important function of this molecule, is the activation of specific receptors on the cell membrane, in particular, ionotropic receptors such as P2X (ATP-gated receptor cation channel family).
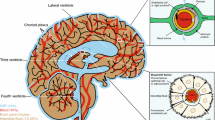
Both ASICs and P2X receptors are involved in numerous physiological functions [2,3,4,5]. Although the amino-acid sequences of ASICs and P2X are substantially different, both channels are trimeric complexes (Fig. 1) sharing a similar pore architecture and conducting monovalent cation currents [6].
Structures of ASIC1 in complex with psalmotoxin at a high pH (A) and the P2X4 channel in the closed state (B). Different colors correspond to different subunits of the channels. TM, transmembrane domain; EC, extracellular domain. Images 4fz1 and 3h9v from the Orientations of Proteins in Membranes database of the University of Michigan (CC BY 3.0) with changes.
Both ASICs and P2X receptors mediate a variety of pathologies [5, 7], the majority of which have a considerable social impact [8,9,10,11] (Table 1). Several recent reviews have summarized findings on the role of ASICs in the peripheral nervous system, in particular in nociception and proprioception [2, 12]. The structure–function relationship of ASICs [4, 13] and their evolution [14] has been described as well as developing pharmacology [15]. Similarly, the importance of P2X receptors in the peripheral nervous system, smooth muscle, vascular physiology, and pathology has been the subject of several recent reviews [16,17,18,19].
The roles of ASICs and P2X receptors in the brain have also been summarized in several reviews devoted to each of these receptors [20,21,22,23,24,25]. On the other hand, it is reasonable to review their roles in the framework of the same work. Protons and ATP serve as co-transmitters in specific brain areas, and consequently, both ASICs [26,27,28,29,30] and P2X receptors [31, 32] mediate some components of the postsynaptic response. ASICs [26, 28, 33, 34] and P2X receptors [35] are also involved in synaptic plasticity, which makes them important players in this brain function. Furthermore, ASICs and P2X receptors have been shown to form molecular complexes with one another, suggesting the possibility of their functional interaction(s) [36, 37]. In this review, we briefly outline the physiological roles of ASICs and P2X receptors and the brain pathologies involving these receptors.
General Information on ASICs and P2X Receptors
ASICs
ASICs are proton-gated voltage-independent ion channels that are ubiquitous in the nervous system. The existence of receptors for protons was first revealed in 1980 as currents activated by extracellular acidification of the neuronal membrane [38]. They were named acid-sensing ion channels after being cloned in 1997 [39]. ASICs are members of the epithelial Na+ channel/degeneration family of amiloride-sensitive ion channels [3].
Currently, at least eight subunits encoded by five genes (ASIC1-5) are known. Splice variants of the ASIC1 gene give ASIC1a, ASIC1b, and ASIC1b2 subunits; and those of ASIC2 give ASIC2a and ASIC2b subunits [40,41,42,43]. There are no known splice variants of the ASIC3–5 genes. Almost all subunits of these channels are expressed in the mammalian brain, except for ASIC1b [44] and ASIC1b2 [45]. Of them, the most common are ASIC1a, ASIC2a, and ASIC2b [46]. The subunits form homo- or heterotrimeric complexes working as channels with pH-sensing properties [46].
ASIC1a homomers are more sensitive to extracellular protons than other subunits and their combinations [41, 47, 48]. ASIC2b, ASIC4, and ASIC5 are not activated by protons at all [40, 49, 50].
ASICs are found in most regions of the mammalian brain: cerebral cortex, cerebellum, brain stem, amygdala, hippocampus, diencephalic structures, striatum, and olfactory bulb, among other brain structures [24].
Under physiological conditions, the main stimulus known so far to activate ASICs is a rapid drop in pH. ASIC1a is of particular importance since it can be activated by acidosis in the physiological range. In a laboratory setting, the activity of ASICs can be altered by several natural or synthetic substances: amiloride and A-317567 (non-discriminative low-affinity blockers), 2-guanidine-4-methylquinazoline (a pH-independent activator), ammonium ions (an activator), the spider peptide psalmotoxin-1 (PcTx1, complex state-dependent effects on ASIC1), the snake venom components mambalgins (blockers), novel compound 5b (an orthosteric antagonist of ASIC1a), and others [7, 51,52,53]. Several endogenous substances such as spermine [54], histamine, or corticosterone [55] also modulate the activity of ASICs.
At the periphery, ASICs are primarily expressed in sensory neurons that innervate tissues and organs, and participate in sensory processes, including mechanotransduction, chemoreception, and nociception [2]. Within the brain, ASICs appear to play important roles in synaptic transmission, and its modulation and plasticity [24]. Briefly, the rapid acidification occurring during synaptic transmission [26, 56] activates ASICs on postsynaptic neurons in several brain structures [26,27,28,29,30, 57], implying that some component of postsynaptic current is mediated by ASICs with protons acting as co-transmitters. Before this component was identified, it was already known that ASICs play a functional role in central synapses. Their activation regulates the synaptic strength of glutamatergic and GABAergic synapses and/or contributes to use-dependent synaptic plasticity [24]. Depending on the pattern of neuronal activity, the structure of a given brain region, and downstream signaling pathways, ASICs may contribute to both short-term [29, 58, 59], and long-term [26, 33, 34, 52, 58, 60, 61] plasticity. The involvement of ASICs in the functioning of synapses in the amygdala, hippocampus, striatum, and cingulate cortex determines their role in higher-order functions like learning, memory, and fear conditioning. A detailed review of the behavioral effects of ASIC activation or inactivation can be found in [24]; here we describe the main known effects.
Pharmacological inhibition or genetic elimination of ASICs negatively affects motor performance in tests of high difficulty [57], and, interestingly, this effect decreases after training. Also, ASICs contribute to the freezing component of innate fear reactions. Disruption of ASICs in the amygdala decreases the ability to form long-term potentiation (LTP), which manifests as deficits in both cue and context fear conditioning [33, 44, 62]. In the ventral hippocampus, inhibition of ASIC1a leads to impairment of fear extinction [63], which is mediated by the alteration of NMDA receptors. ASICs influence not only the negative reinforcement system but also the positive. Global (genetic) disruption of ASIC1a leads to a decrease in learning performance in the classical conditioning paradigm based on positive stimuli [64]. In the nucleus accumbens, ASIC1a emphasizes cocaine-seeking behavior [65, 66].
The pH-sensing properties of ASICs determine their role in controlling brain homeostasis related to CO2 concentration. Systemic blockade or deletion of ASIC1a decreases hypercarbia-induced freezing [62, 67]. Reconsolidation of related memories also depends on the proper functioning of ASICs [68]. Interestingly, suppressing the activity of ASIC2 and ASIC3 in the locus coeruleus disturbs sleep structure [69]. This region is known to be a CO2-dependent modulator of respiration and sleep-wakefulness cycles.
In general, the contribution of ASICs to complex forms of behavior and brain homeostasis is essential, modulatory, and region-dependent.
P2X
The idea of ATP-mediated intercellular signaling appeared almost immediately after the discovery of this molecule in 1929 [70]. The first information on the release of ATP from sensory nerves was obtained by Pamela Holton in the 1950s [71, 72]. In 1972, Geoffrey Burnstock proposed the existence of "purinergic" nerves [73], thus founding a new research field. We now know that extracellular ATP signaling is widespread among different physiological systems [74]. Much of the early data on purinergic signaling were obtained from experiments on smooth muscles. In 1983, it was shown that extracellular ATP causes depolarizing ionic current in mammalian sensory neurons [75, 76] due to the opening of the membrane ion channels [77, 78] and can mediate rapid synaptic transmission in both peripheral and central parts of the nervous system [74]. Extracellular ATP activates both inotropic P2X and metabotropic P2Y receptors [74]; the latter are not reviewed here.
P2X receptors are ligand-gated ion channels that trigger their open state by binding ATP or related agonists. In mammals, seven genes encoding P2X receptor subunits are known [79]. Their amino-acid sequences are 40%–50% identical. The length of P2X1–6 subunits is 388–471 amino-acids, while the P2X7 receptor is larger (595 amino-acids). Each subunit contains two hydrophobic transmembrane domains separated by an ectodomain (~ 280 amino-acids). Functional channels are formed as trimers. The pore is formed by six transmembrane domains (two from each subunit). The cytoplasmic part of the channel is formed by the N- and C- termini of the subunits [79]. Due to the larger size of the P2X7 subunit, its intracellular part contains additional domains [80]. The trimers can be homomeric (P2X1, P2X2, P2X3, P2X4, P2X5, or P2X7, but not P2X6) or heteromeric (except P2X7). Common heteromeric variants are P2X1/2, P2X1/4, P2X1/5, P2X2/3, P2X2/6, and P2X4/6 [81]. P2X receptors are widely expressed in the cells of various tissues: smooth (P2X1) and skeletal (P2X5) muscles, immune cells (P2X7), as well as, critical for this review, neurons, glial cells, and brain microvessels (P2X2, P2X3, P2X4, and P2X6) [79, 82].
All P2X receptors are permeable to small monovalent cations, while some have significant permeability to Ca2+ (the highest reported for P2X4) [79, 83]. Homomeric P2X7 receptors can transmit even relatively large organic cations such as some fluorescent dyes [83]. However, P2X5 receptors are permeable to Cl– anions too [84].
After activation, P2X receptors undergo desensitization. Based on the speed of this process, we distinguish two groups: with fast (< 1 s; P2X1 and P2X3) and slow (> 20 s; P2X2, P2X4, P2X5, and P2X7) onset [79, 83, 85]. The molecular mechanisms controlling desensitization are insufficiently studied. The available data indicate that this process is determined mainly by the properties of the channel's cytoplasmic cup [80, 86].
The main physiological agonist of P2X receptors is ATP. The efficient concentration range to activate most P2X receptors is 0.5–12 μmol/L. The exception is P2X7, which requires a significantly higher concentration of up to 100 μmol/L [79]. Other efficient agonists of P2X receptors are ATP derivatives: 2-meSATP, ATPγS, α,β-meATP, βγ-meATP, BzATP, and the like. Many novel compounds act as non-selective (suramin, PPADS, and RB-2) or selective antagonists. A detailed review of the pharmacological properties of P2X receptors can be found in [79].
The wide expression of P2X receptors, in particular their presence on smooth muscle cells (including blood vessels), immune cells, neurons, and glia, determines the broad variety of their physiological effects. Numerous ATP effects are carried out in both the efferent and sensory parts of the peripheral nervous system. ATP is released as the co-transmitter in the terminals of autonomic fibers (along with acetylcholine or norepinephrine), where it acts mainly through the activation of P2X1 receptors. P2X2 and P2X3 receptors of gustatory afferents detect the ATP released from taste receptor cells [87]; modulate the activity of the auditory system [88]; and induce the excitation of nociceptors [89]. In the central nervous system (CNS), P2X receptors contribute to excitatory intercellular communication in the locus coeruleus [90, 91], hippocampus [31, 35, 92], spinal cord [93], hypothalamus [94, 95], and cortex [32, 96]. Of particular interest are P2X4-containing receptors, which have the highest permeability to Ca2+. In the presynapse, their activation may trigger Ca2+-dependent signaling, enhancing, for example, the release of glutamate [97]. The release of ATP under physiological conditions facilitates LTP in the hippocampus, and this facilitation is mediated by Ca2+ entry through P2X4 receptors followed by the downregulation of postsynaptic NMDA receptors [98]. Also, P2X4 receptors are significantly expressed in microglial cells and are involved in immune function [99].
P2X receptors are involved in the interaction of neurons and glial cells and hence may play a role in the development, maintenance, and plasticity of neuronal circuits [100]. In particular, astrocytic P2X7 receptors have the potential to cause rapid non-vesicular glutamate release [101]. Microglial P2X7 receptors are important for immune responses, particularly in the CNS. The role of P2X receptors in pathological processes is discussed in more detail in the following section.
ASICs in Brain Pathology
As outlined in the previous section, ASICs are widely expressed in the mammalian nervous system in general and the brain in particular. The list of established functions of this receptor family is already long and is rapidly increasing (for instance, reviewed in [102, 103]). ASICs are involved in many important physiological functions, as well as contributing to a variety of pathologies. This is not surprising given that tissue acidosis is a key contributor to neuronal cell death in many neurological diseases, whereas ASICs, namely subtype ASIC1a, are pivotal in acidosis-induced damage to brain neurons. [104, 105]. Chronic pain [106], ischemic stroke [4], epileptic seizures [106, 107], degenerative disorders including multiple sclerosis (MS), Parkinson’s disease (PD), and even neonatal hyperbilirubinemia [108] are just a few examples of pathologies involving ASICs. Interestingly, apart from the well-established role of peripheral ASICs in pain, there is emerging evidence that ASIC1a located in the brain is an important player in pain processing [28].
Some of these pathologies affect millions of people worldwide and are still awaiting adequate pharmacological tools for their cure (for instance up to 40% of epilepsy cases are resistant to currently available drug therapy). Emerging evidence from intensive research strongly suggests that the pharmacological modulation of ASICs is a very promising strategy for the treatment of these pathologies.
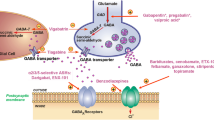
In this section, we briefly review evidence regarding the role of ASICs in acid-induced toxicity in relation to some brain pathologies. In addition, we outline a potential explanation for the following paradox. ASICs, especially ASIC1a, are typically activated by a rapid drop in pH, whereas slow acidification results in steady-state desensitization without inducing detectable currents [109, 110] (Fig. 2). On the other hand, acidification associated with pathological states is prolonged and typically slow, and thus should not activate ASICs. Still, inhibition of ASICs (especially ASIC1a), is protective in multiple models of pathological states reported in numerous studies. How to account for this contradiction?
Slow acidification results in the steady-state desensitization of ASIC currents. ASIC-currents are evoked by acidification with similar amplitudes (from pH 7.4 to pH 6.0) but with different rise times. Upper panel, the pH of the applied solution was measured using pH-sensitive fluorescent dye; the 10–90% fall-time of the fluorescence change corresponds to the interval between the two squares (corresponding values are shown above the traces). Lower panel, ASIC currents evoked by these acidifications. Notice the striking reduction of the amplitudes of ASIC currents evoked by slower acidification. Adapted from [110] (part of Figure 4) published under the terms of the Creative Commons Attribution License (CC BY).
Ischemic Stroke
Acidosis is a common feature of ischemia and is assumed to play a critical role in brain injury [111]. Important evidence regarding the role of Ca2+-permeable ASICs in acidosis-induced brain injury was reported in 2004 by Xiong et al. [104]. In particular, it was found that in focal ischemia, intracerebroventricular injection of ASIC1a blockers or knockout of the ASIC1a gene protects the brain from ischemic injury more potently than glutamate antagonism [104]. Since then, the pathological role of ASIC1a in stroke has been confirmed in many studies and extensively reviewed [7, 111, 112]. Still, the exact mechanism of involvement of ASIC1a in stroke requires further investigation because at least two studies [105, 113] that do confirm the important role of ASIC1a in an in vitro model of acidotoxicity and an in vivo model of ischemic stroke, suggesting that this role involves an ion-conducting independent function of ASIC1a [105]. Authors [105] have reported that extracellular protons trigger a novel form of neuronal necroptosis via ASIC1a. Indeed, they identified serine/threonine kinase receptor interaction protein 1 (RIP1) as a critical component of this form of neuronal necroptosis. Acid stimulation recruits RIP1 to the ASIC1a C-terminus, causing RIP1 phosphorylation and subsequent neuronal death [105]. Arguments used to support the point that the role of ASIC1a is independent of the ion-conducting function include the following [105]:
-
1.
Pretreatment of cultured mouse cortical neurons with mild acidification (pH 6.8) greatly suppresses the ASIC currents evoked by greater acidification (pH 6); however, this fails to prevent acid-induced neuronal death [105].
-
2.
Removing Ca2+ from the treatment solution has no clear protective effect on acid-induced neuronal death [105].
-
3.
Although co-administration of the non-specific ASIC blocker amiloride with acid significantly inhibits ASIC-currents, it does not show neuroprotection [105].
This study has been recently expanded by revealing an auto-inhibitory mechanism that regulates interactions between the N-terminus (NT) and C-terminus (CT) of the ASIC1a protein, in particular, by using fluorescence resonance energy transfer [113]. Disruption of this auto-inhibition underlies conformational signaling of ASIC1a to induce neuronal necroptosis; a synthetic membrane-penetrating peptide representing the distal NT of ASIC1a has been identified as protective in both acidosis-induced necroptosis in vitro and a mouse model of ischemic stroke [113]. These results suggest a therapeutic potential of targeting the auto-inhibition of ASIC1a for neuroprotection against acidotoxicity [113]. This study also provided additional evidence that the role of ASIC1a in necroptosis is independent of the ion-conducting activity. Indeed, acid treatment mediates cell death in mutants with non-conducting ASIC1a just as in wild-type animals [113].
Chronic Pain
Chronic pain is a challenging clinical problem affecting millions of people worldwide. It is well established that ASICs play important roles in nociception at peripheral and spinal neurons [2, 12]. However, the role of these channels in pain perception at the supraspinal level is less studied. Still, recent findings [28] indicate that brain ASIC1 does contribute to pain perception, making it an attractive therapeutic target for chronic pain management. Several lines of evidence support an important role of cortically-located ASIC1a channels in pain hypersensitivity by promoting long-term synaptic potentiation in the anterior cingulate cortex [28]. In particular, region-specific genetic deletion or pharmacological blockade of ASIC1a results in attenuated heat and mechanical hypersensitivity in the CFA model of inflammatory pain, while at the cellular level it reduces the probability of LTP induction in this brain area [28]. It has been concluded that ASIC1a critically gates pain sensitivity by regulating the probability of cingulate LTP induction, in which PKCλ serves as a crucial mediator [28].
Epilepsy
Epilepsy, a disorder of unprovoked seizures, is a multifaceted disease affecting individuals of all ages with a particular predilection for the very young and old [114]. In addition to seizures, many patients often report cognitive and psychiatric problems associated with both the seizures themselves and their therapy [114]. About 1% of the human population suffers from chronic epilepsy disorder and 30–40% of patients develop drug-resistant epilepsy. Therefore, finding new targets for pharmacological intervention to treat patients with epilepsy is very important.
During and following seizures, lactic and glutamic acids are released into the extracellular space, causing a significant fall in pH that activates ASICs [115,116,117]. These results imply that ASICs may be involved in the regulation of epileptic discharges. On the other hand, the exact role of ASICs in such discharges is rather controversial. Some authors suggest that acidification diminishes seizure severity due to the more pronounced ASIC-dependent activation of inhibitory GABAergic interneurons by acidification as compared to excitatory glutamatergic cells [118]. Consistent with this idea, ASIC density on hippocampal inhibitory neurons is higher than on principal neurons, and the loss of ASIC1a reduces postictal depression [118]. Other studies have demonstrated that inhibition of ASIC activity reduces epileptic manifestations in in vitro models of epilepsy: perfusion of hippocampal slices with amiloride or PcTx1 reduces the epileptic discharges evoked by electrical stimulation or removal of extracellular Mg2+ and hippocampal slices from ASIC1a-knockout mice are less susceptible to seizures [119]. Similarly, the application of the novel ASIC1 antagonist compound 5b to rat hippocampal slices during epileptic activity significantly and reversibly reduces the frequency of seizure discharges [107]. In addition, in an in vivo model of epilepsy, selective ASIC antagonists reduce the seizure-like activity evoked by the injection of kainic acid into the amygdala or hippocampus [107, 119].
Neurodegenerative Diseases
In spite of many differences, neurodegenerative diseases have several similarities including accumulation of misfolded proteins, damage to specific neuronal populations, neuroinflammation, and persistent acidification [120]. Neuroinflammation is a complex process that occurs in various neurodegenerative diseases such as Alzheimer's disease (AD), PD, MS, and Huntington's disease (HD) [120]. Moreover, there is growing evidence suggesting that neuroinflammation is among the important causes of neurodegenerative diseases [120,121,122]. Inflammatory stimuli, such as ATP, lactic acid, arachidonic acid (AA), agmatine, and hypertonicity, are able to enhance the proton-induced ASIC current [121], whereas persistent acidification accompanies neurodegenerative diseases.
In addition, it has been demonstrated that ASICs: (1) mediate a component of synaptic current at glutamatergic synapses as postsynaptic ionotropic receptors for protons [26,27,28,29]; (2) play a role in the regulation of synaptic transmission at glutamatergic [59, 123] and GABAergic [107, 124], synapses; and (3) are involved in short- and long-term plasticity [26, 28, 52, 59].
Therefore, ASICs are considered to be potential targets for the treatment of neurodegenerative diseases, and promising results have been obtained as briefly outlined below.
Alzheimer’s Disease
AD is a progressive neurodegenerative disorder, the most common form of dementia, accounting for 60–70% of all cases [125]. In spite of many attempts, currently there are still only symptomatic treatments available for this disease; no drugs capable of arresting or reversing it have so far been identified [125, 126].
While the question regarding the primary cause of the disease is still debated, it is widely accepted that the progression of AD occurs due to multiple factors. There is emerging evidence that the activation of ASICs may be one of these factors (reviewed recently [22, 120]). Here, we only note that observational studies in humans, though indirect, corroborate this view. Amiloride, a non-specific blocker of ASICs, is a well-known K+-sparing diuretic used in medical practice. The use of diuretics, including amiloride, is associated with a reduced risk of AD [127, 128]. Moreover, while all antihypertensive drugs are associated with a decrease in AD risk, K+-sparing diuretics (including amiloride) are associated with the greatest reduction of this risk [127].
A selective antagonist of ASIC1a, PcTx1, inhibits the mGlu receptor-dependent long-term depression recorded in hippocampal slices, which were either treated with Aβ oligomers or obtained from the Tg2576 mouse model of AD [129]. Curcuminoids, considered a treatment for AD [126], block ASICs [130]. In this regard, it is also interesting to note that memantine, one of the very few drugs approved for the amelioration of AD, apart from its blocking action on NMDA receptors (believed to be its primary mechanism of action) also affects ASICs [131].
Multiple Sclerosis
MS is a chronic autoimmune inflammatory disease of the CNS that involves demyelination and axonal degeneration [132]. ASIC1a is upregulated in the brain tissue of patients with MS [133]. Similarly, ASIC1a is upregulated in oligodendrocytes and axons in a mouse model of MS (acute autoimmune encephalomyelitis, EAE) [133]. The enhanced expression of ASIC1 is associated with axonal damage while blocking these channels with amiloride protects both myelin and neurons from damage in this model [133]. These results are in line with evidence obtained elsewhere [134]. After induction of EAE, ASIC1-/- mice show both a markedly reduced clinical deficit and reduced axonal degeneration compared to wild-type animals [134]. ASIC1 disruption is also protective against acidosis-mediated injury in nerve explants in vitro [134]. Importantly, evidence supporting the neuroprotective effect of amiloride has been obtained from a cohort of MS patients [135].
Parkinson’s Disease
PD is a progressive neurodegenerative disorder resulting from a pathological loss or degeneration of dopaminergic neurons in the substantia nigra of the midbrain and the development of neuronal Lewy bodies [136]. The potential role of ASICs in PD has been studied in a mouse model of degeneration induced by 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine (MPTP) [137]. Amiloride has been found to protect substantia nigra neurons from MPTP-induced degeneration. Administration of the selective ASIC1a antagonist PcTx1 is also protective, resulting, however, in a much more modest effect [137].
Huntington’s Disease
HD is a neurodegenerative disease caused by CAG (cytosine, adenine, and guanine) repeat expansion in the huntingtin gene and involves multiple pathogenic mechanisms [138]. There is evidence indicating that acidification-induced activation of ASIC1a may be one of these mechanisms [139]. In particular, in the R6/2 mouse model of HD, it has been shown that the amiloride derivative benzamil increases the activity of the ubiquitin–proteasome system, resulting in enhanced degradation of soluble huntingtin–polyglutamine aggregation [139]. Similarly, blocking the expression of ASIC1a leads to an enhancement of ubiquitin–proteasome system activity and this blockade also decreases huntingtin–polyglutamine aggregation in the striatum of R6/2 mice [139].
Psychiatric Disorders
There is not much data on the role of ASICs in psychiatric disorders. Nonetheless, ASIC1a inhibition (genetic or pharmacological) reduces depression-like behavior in mice [140] and rats [141]. Thus, ASIC1a has been proposed as a potential target to combat depression. At the same time, there is no evidence of the role of ASICs in anxiety or depressive behavior in patients. Despite this fact, using the ASIC blocker amiloride in the form of a nasal spray is considered to be a treatment for anxiety disorders [142].
ASIC1/2 inhibition reduces the freezing response to hypercarbia [62, 67]. An increase in CO2 in the inhaled air can induce a panic attack. Interestingly, the genetic variation of ASIC1a and ASIC2 structure is related to the individual differences in the panic response to an increased CO2 concentration [143]. In addition, a specific ASIC1 polymorphism (rs685012) is more frequent in patients with panic disorder than in healthy controls [144].
Protective Effects of Blocking ASICs in Spite of Slow Acidification in Pathologies: Potential Explanations
The roles of ASICs in several fundamental physiological processes as well as in numerous pathologies have been well documented. However, in contrast to pathologies, the roles of ASICs in physiological processes are easier to explain because rapid (though brief) changes in pH occur under physiological conditions. In particular, the latter is applicable to synapses ([56, 145, 146], but see [147] for conflicting evidence), where rapid acidification occurring during synaptic vesicle release can activate ASICs on both pre- and postsynaptic neurons [24]. Pathologies, on the other hand, are typically associated with slow and prolonged acidification, raising the question of how rapidly inactivating ASICs can contribute substantially to these pathologies.
Evidence regarding potential mechanisms relevant to this question can be subdivided into two broad categories: (1) conformational signaling of the ASIC independent of its ion-conducting function (as suggested for the role of ASIC1a in necroptosis [105, 113]), and (2) activation and decreased steady-state desensitization of ASICs by pro-inflammatory and algesic endogenous mediators.
Regarding conformational signaling via ASIC1a, the above results of Wang and colleagues [105, 113] indicate that conformational signaling involving ASIC1a induces neuronal necroptosis in in vitro and in vivo models of ischemic stroke. This signaling recruits RIP1 and is independent of the ion-conducting function of ASIC1a [113]. At the same time, these studies do not exclude the therapeutic potential of targeting ASIC1a in ischemic stroke with known blockers of this channel. Indeed, in contrast to co-administration, pretreatment with amiloride did show neuroprotection in the same study [105]. PcTx1, which is believed to inhibit ASIC1a activation by causing steady-state channel desensitization at neutral and alkaline pH (in contrast to mild acidification) is also neuroprotective [105]. An explanation of these results taken altogether is not straightforward. In addition, it should be noted that, while no clear protective effect of removing Ca2+ from the treatment solution on acid-induced neuronal death was reported by Wang et al. [105], the opposite results were reported in another study [104]. Thus, further studies are required to address these controversial issues.
As for pro-inflammatory and algesic endogenous mediators that enhance the activity of ASICs, there is growing evidence that numerous endogenous substances (such as lactate, AA, FMRFamide-related peptides—peptides related to mammalian RFamide transmitters, dynorphins, nitric oxide, and histamine), up-modulate ASICs, and the extracellular levels of these substances are increased in pathological states (see [121, 148, 149] for reviews). For instance, endogenous cationic polyamine spermine enhances ASIC1a and ASIC1b currents by decreasing the pH sensitivity of channel steady-state desensitization [54]. Moreover, via its effect on ASIC1a, increased extracellular spermine exacerbates neuronal damage following ischemic stroke [54]. AA, a polyunsaturated fatty acid, involved in cellular signaling activities as a lipid second messenger, plays a critical role in pathological conditions such as inflammation and neurological disorders [149]. AA regulates the activity of ASICs [150]. Indeed, in the cerebellum, AA significantly enhances the sustained component of current induced by acidification and increases the fraction of cells exhibiting a sustained component [150]. It should be noted, however, that this sustained component of current is insensitive to amiloride [150], raising the question of whether it is mediated by ASICs. The ASIC currents are also potentiated by lactate, and released in ischemia, and by FMRFamide [150]. Another endogenous mediator, histamine, directly and selectively potentiates ASIC1a homomers, most effectively when applied at modest levels of acidification [151].
P2X Receptors in Brain Pathologies
P2X receptors are widely expressed by both neurons and glia in various brain regions, indicating their crucial role in physiological and pathophysiological brain function. Following world pharma’s patent applications [152, 153] and recent numerous studies [154, 155], the P2X7 receptor is the most prominent drug target for numerous CNS diseases, especially those accompanied by inflammation [155, 156]. Brain P2X7 and P2X3 receptors participate in central pain transmission. P2X7 receptors are involved in the modulation of diabetes-induced neuropathic pain [157], whereas P2X3 (traditional primary nociception receptor) expressed in the midbrain periaqueductal gray is involved in the modulation of central post-stroke pain [158]. One could think that the P2X7 subunit is the sole one involved in almost all brain disorders. However, we suggest that the role of other subtypes of these receptors in brain disorders, particularly P2X4, which is more sensitive to ATP than P2X7 [79], is still underestimated.
Neuroinflammation, Ischemia, Stroke, Epilepsy, and COVID-19
Under healthy conditions, the concentration of extracellular ATP in tissues is in the nanomolar range [159]. However, under stress, hyperexcitability, ischemia, and cellular damage, the ATP concentration increases considerably, resulting in the activation of P2X receptors. In high concentrations, extracellular ATP activates P2X7 receptors that are highly expressed in microglial cells [159,160,161]. This results in the activation of transcription factor NF-κB, which consequently promotes the upregulation of the pro-inflammatory cytokines, pro-IL-1β and pro-IL-18, and NLRP3 protein. It has been shown that the P2X7 receptor is one of the most potent activators of the NRLP3-associated inflammasome [160]. The latter triggers the activation of caspase-1, which causes the maturation of IL-1β and IL-18 and, consequently, increases pro-inflammatory cytokine release [160, 162]. A recent study demonstrated that inhibition of P2X7 by the selective antagonist, JNJ-55308942, suppresses the development of neuroinflammation induced in different rodent models by lipopolysaccharide, Bacillus Calmette–Guerin, or chronic stress [162].
Brain ischemia induces ATP release and the subsequent activation of P2X receptors that conduct inward cationic current through the plasma membrane. However, despite their higher sensitivity to ATP than P2X7 [79], the contribution of P2X4 receptors to this current is virtually undetermined. Acute ischemia promotes the upregulation of P2X4 receptors in microglia or infiltrating macrophages [163, 164]. Activation of these receptors modulates the inflammatory response after stroke [165]. Correspondingly, a potent inhibitor of inflammation, minocycline, attenuates the upregulation of P2X4 receptors induced by hypoxia-ischemia [166]. Specific deletion of P2X4 is acutely neuroprotective and leads to a substantial reduction of infarct volume [165]. On the other hand, it predisposes depression-like behavior chronically after stroke due reduced expression of brain-derived neurotrophic factor (BDNF) [165]. Recent data show that P2X4 receptors are required for ischemic tolerance following middle cerebral artery occlusion in mice [167]. In contrast, blocking P2X4 receptors by TNP-ATP (but not PPADS that presumably inhibits P2X1-3 and P2X5-7 receptors) in a rat model of neonatal hypoxia shows a profound neuroprotective effect, pointing to the differences in P2X receptor function in ontogenesis [168].
There is a growing body of evidence for the role of ATP as well as P2X receptors in status epilepticus (SE) and epilepsy. Some studies report that extracellular ATP increases during SE and seizures, but this effect requires further examination [169]. Mice lacking P2X4 receptors display a decrease in neuronal death after SE, although seizure activity is not altered by the knockout of the corresponding gene [170]. In addition, the administration of P2X7 antagonists has been shown to have anticonvulsive effects in several experimental models of SE and acute seizures [171,172,173,174,175]. Genetic deletion of P2X7 receptors and inhibition of their activity by antibodies also suppress seizures in the kainic acid model of epilepsy [171]. Following SE, there is a prominent increase in P2X7 receptors and downregulation of P2X2 receptors in hippocampal neurons, particularly granule neurons, and microglia [171, 176]. It has also been reported that P2X4 receptors are upregulated in hippocampal microglia after SE in rats [170]. Upregulation of P2X3 receptor expression has also been shown in the LiCl-pilocarpine rat model of chronic epilepsy, as well as in patients with temporal lobe epilepsy [177]. The authors found that activation of P2X3 receptors accelerates sustained repetitive firing, while their inhibition results in relatively low-frequency discharges [177]. These data were later confirmed using the pentylenetetrazole-induced animal model of epilepsy. Administration of the P2X3 antagonist NF110 significantly and dose-dependently ameliorates pentylenetetrazole-induced impairments in behavior, learning, memory, locomotion, motor activity, discrimination, neuronal damage, hippocampal inflammation, oxidative stress, and mitochondrial dysfunction. These effects of NF110 are notably abolished by administration of the selective P2X3 agonist α,β-methylene ATP [178]. Growing data indicate that certain P2X receptors may be novel drug targets for seizure control.
The ATP release induced by the SARS-CoV-2 virus has recently been proposed to play a key role in the genesis of both the main symptoms and sequelae of the novel coronavirus disease COVID-19 [179]. According to recent findings, COVID-19 is associated with a number of severe consequences, including "brain fog", depression, confusion, stroke, and more [180,181,182]. The metallopeptidase named angiotensin-converting enzyme 2 has been identified as the functional receptor for SARS-CoV-2. It is highly expressed in lung alveolar epithelial cells and enterocytes of the small intestine, being also present in the brain neurons, glial cells, and microglia [181,182,183,184]. P2X7 receptors, which are known to induce the secretion of pro-inflammatory cytokines in response to elevated ATP levels, are abundantly expressed in both macrophages and microglia, suggesting that these receptors can be a potential target for treating COVID-19 [185].
Neurodegenerative Disorders
Alzheimer’s Disease
Some authors have proposed that ATP participates in the inflammatory process widely described in AD [186, 187] while others suggest that ATP, leaking through cell membrane pores made by soluble amyloid-β (Aβ) peptide, could participate directly through some P2X receptors [188, 189]. Numerous reports indicate that the P2X7 receptor plays a crucial role in AD, and its inhibition ameliorates the neuronal damage induced by both neuroimmune response activation [190,191,192] and reactive oxygen species production [193, 194]. There has been some conflicting information on the effect of these receptors on α-secretase activity, which cleaves amyloid precursor protein within the Aβ domain, thereby preventing the generation of Aβ. Two studies have shown that inhibition of P2X7 receptors leads to an increase in α-secretase activity through inhibition of glycogen synthase kinase 3 [195, 196]. However, results from Delarasse et al. revealed the opposite effect: P2X7 receptor stimulation may enhance α-secretase activity [197]. It has been reported that systemic administration of a P2X7 receptor antagonist, Brilliant Blue G, diminishes the spatial memory impairment and cognitive deficits induced by the injection of soluble Aβ1-42 into the hippocampal CA1 region of mice, which is an animal model of AD [198]. P2X4 overexpression in the neurons enhances the toxic effect of Aβ1-42, whereas its silencing decreases cellular death after exposure to Aβ1-42, indicating that this P2X subtype also contributes to the neuronal cell death induced by Aβ [199]. A recent paper suggests that P2X2 receptor expression increases in the brain of patients with AD, so it may participate in the toxic cellular and molecular events induced by Aβ [200]. In addition, the overexpression of P2X2 increases Aβ levels in a cellular model of AD [200]. We can conclude that the P2X4 and P2X7 receptors are important prospective targets in the treatment of AD.
Parkinson’s Disease
The cause and pathogenesis of PD remain elusive. The neurotoxin 6-hydroxydopamine (6-OHDA) is widely used to induce models of PD. Recently it has been shown that 6-OHDA increases ATP release and its extracellular conversion into adenosine through CD73 upregulation in SH-SY5Y cells [201]. P2X7 receptor inhibition has neuroprotective and neuroregenerative effects in various models of PD through anti-inflammatory actions along with modulation of the microglial activation state and cytokine release [202,203,204,205]. Also, overexpression of P2X4 receptors upregulates IL-6 and exacerbates 6-OHDA-induced dopaminergic degeneration in the rat model of PD [206]. A very recent paper suggests that P2X4 receptor activation might inhibit neuronal autophagy through regulation of the BDNF/TrkB signaling pathway, leading to dopaminergic neuron damage in the substantia nigra and the further inhibition of P2X4-mediated autophagy [207]. A role for P2X1 receptors in PD pathogenesis has also been reported, perhaps identifying a new therapeutic target [208, 209]. Consequently, P2X7, P2X4, and P2X1 receptors are interesting research subjects and might be possible targets for PD treatment.
Huntington’s Disease
We found only a few reports on the role of P2X receptors in HD. The first study demonstrated that P2X7 receptor expression is substantially increased in two HD animal models, also its channel pore has augmented Ca2+ permeability, and finally, its inhibition with Brilliant Blue G lessens the motor coordination deficits and cachexia and decreases neuronal loss [210]. The most recent paper reported elevated expression of the P2X7 receptor in the human postmortem striatum as well as alteration of its splicing [211], pointing to the important role of this receptor in HD.
Amyotrophic Lateral Sclerosis
The first experimental findings on the role of P2X receptors in ALS demonstrated a significant increase in P2X7 immunoreactivity in active microglia from postmortem spinal cords of patients with sporadic ALS [212]. Similarly, increased immunoreactivity for P2X7 has been found in an animal model of familial ALS, the SOD1-G93A mouse [213], while increased P2X4 receptor immunoreactivity is associated with degenerating neurons [214]. In addition, it has been shown that the allosteric modulator of the P2X4 receptor ivermectin extends the lifespan of SOD1-G93A mice by almost 10% [215]. P2X7 is known to play a complex role in ALS [216]: while knockout of P2X7 accelerates the disease in SOD1-G93A mice [217], antagonism immediately preceding the onset of symptoms partially ameliorates the motor neuron loss and inflammation [217]. Later it has been reported that P2X7 participates in ALS pathogenesis by directly modulating autophagy and particularly the expression of autophagosome component LC3-II and the autophagy receptor p62 in SOD1-G93A microglia [218]. These findings support the idea that P2X7 receptors might be one of the top targets in a multidrug strategy for ALS treatment.
Multiple Sclerosis
MS is an autoimmune disease with an unknown etiology. It is characterized by massive infiltration of immune cells, demyelination, axonal loss, and chronic inflammation that induces ATP release in lesions. It has been reported that both P2X4 [219] and P2X7 [220] receptors are strongly overexpressed in MS lesions in humans. Recently-found genetic mutations of P2X receptors support their role in MS: a rare P2X7 variant, Arg307Gln, with absent pore formation and function protects against neuroinflammation in MS [221]; and a rare P2X7 Gly150Arg–P2X4 Tyr315Cys haplotype which inhibits P2X7-mediated phagocytosis has been suggested as a risk factor for MS [222]. EAE has been extensively used as a model of MS for many decades. It has been shown that in chronic EAE in mice, inhibition of P2X4 receptors with TNP-ATP leads to exacerbation of the clinical signs, whereas their allosteric potentiation with ivermectin has the opposite effect [223]. Blockade of P2X7 receptors results in suppression of demyelination and axonal damage, reduction of gliosis, and amelioration of neurological symptoms in chronic EAE [224,225,226]. These data support the crucial role of P2X4 and P2X7 in MS pathology.
Psychiatric Disorders
There is growing evidence of a possible role of P2X receptors in various psychiatric disorders including major depressive disorder (MDD), bipolar disorder (BD), schizophrenia (SCZ), anxiety, and autism spectrum disorder (ASD) [99, 154, 227, 228]. For several psychiatric diseases, such as MDD, SCZ, and BD, it has been postulated that activation of the P2X7 receptor by ATP release mediates brain inflammation [229,230,231].
Both P2X2 and P2X7 receptors play an important role in depression disorders. P2X2 receptors in the medial prefrontal cortex mediate the antidepressant-like effects of ATP [232], whereas P2X7 receptors activated by synaptic ATP release stimulate the hyperactivation of microglia and interleukin-1β production reported in depressive-like behaviors [231]. In turn, their inhibition by Brilliant Blue G as well as knockout of the corresponding gene has antidepressant effects [233,234,235]. Only a few data are available on the role of P2X7 receptors in SCZ, One study showed that the tricyclic antipsychotics prochlorperazine and trifluoperazine induce allosteric inhibition of human P2X7 receptor activity [236]. Therefore, one may speculate that the antipsychotic-induced inhibition of the P2X7 receptor contributes to therapeutic efficacy [230, 237]. P2X receptors are also involved in BD: the animal model of mania induced by chronic administration of amphetamine, pharmacological blockade with A-438079 and genetic deletion of P2X7 receptor completely reverses the increased locomotor activity induced by amphetamine [229]. A-438079 also abolishes the release of the pro-inflammatory cytokines IL-1β and TNF-α as well as lipid peroxidation in the hippocampus [229]. P2X receptor actions have also been implicated in ASD. Genetic deletion of the P2X4 receptor results in a significant reduction in sensory and social task performance, vocalization responses, and plausible deficit in the ability to extract and filter relevant information from the external milieu, suggesting that P2X4 receptors regulate information processing [238] as well as perceptual and socio-communicative functions [239]. Downregulation of P2X7 and P2Y2 receptor expression has been described as a compensatory response in an animal model of ASD [240].
In summary, the role of P2X receptors in psychiatric disorders requires additional studies, especially regarding P2X2, P2X3, P2X4, and P2X7 subtypes that are strongly associated with neurodevelopment and psychiatric disorders [241, 242].
A Plausible Link between ASICs and P2X Receptors in Brain Disorders
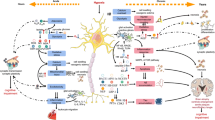
Apart from the differences between ASICs and P2X receptors, as previously stated, there are also similarities, including trimeric structure, similarity in the pore architecture, and ionic permeability [6]. While emerging evidence indicates interactions of ASICs and P2X receptors in sensory neurons [36, 37], their possible roles in brain functions and pathologies are still virtually unexplored. The overlap of brain pathologies mediated (potentially) by ASICs/P2X receptors (Table 2, Fig. 3) suggests that such interactions may be relevant to brain pathologies as well.
In this regard, it seems to be of interest to study the following questions: are ASICs and P2X co-localized in the brain? Are there interactions between ASICs and P2X in the brain? In particular, it may be of interest to study whether such interactions could contribute to the enigma noted above as to how rapidly inactivating ASICs can substantially contribute to the pathologies that are typically associated with slow acidification. Regarding these issues, it should be emphasized that although interactions of ASIC3 with P2X receptors have been a major focus of research in sensory neurons [36], nevertheless, “ASIC1 can also be sensitized through P2X receptors” [36].
Furthermore, given that novel technologies for investigating functional cell-surface ASIC1a channels have recently been developed and used to investigate the physiological roles of these channels in brain neurons [243], the application of such tools to investigating brain pathologies would be fascinating.
Conclusions
We felt the necessity of this review due to the quickly-expanding evidence on the physiological significance of the two receptor/channel families. This seems especially relevant for the ASICs.
Both families entered the “market of knowledge” substantially later than the more canonical families like cholino- or adrenoreceptors. In both cases, the path to recognition of ASICs or P2 receptors was quite difficult and long. Geoffrey Burnstock made prolonged efforts to demonstrate the importance of the dual metabo- and ionotropic roles of purinoreceptors. After being cloned [39], ASICs became a subject of widespread interest 14 years after their initial discovery [38].
The last decade demonstrated that this subject was a long shot: it became clear that every neuron in the mammalian nervous system expresses at least one member of the ASIC family. Correspondingly, we are bound to expect a great variety of functional roles and new possibilities for pharmacology. Thus, new pharmacological tools, not only ASIC-specific but ASIC subunit-specific, will allow the specification of new roles of these receptors in known functions or even reveal new functions.
Both receptor families examined here provide intriguing opportunities in the novel realm of research connected with the roles of receptors traditionally regarded as ion channels. Growing evidence indicates that these receptors play important roles connected with intimate intermolecular machinery in the brain rather than just allowing ions passage.
References
Zeng WZ, Xu TL. Proton production, regulation and pathophysiological roles in the mammalian brain. Neurosci Bull 2012, 28: 1–13.
Carattino MD, Montalbetti N. Acid-sensing ion channels in sensory signaling. Am J Physiol Renal Physiol 2020, 318: F531–F543.
Hill AS, Ben-Shahar Y. The synaptic action of Degenerin/Epithelial sodium channels. Channels 2018, 12: 262–275.
Vullo S, Kellenberger S. A molecular view of the function and pharmacology of acid-sensing ion channels. Pharmacol Res 2020, 154: 104166.
Burnstock G, Kennedy C. P2X receptors in health and disease. Adv Pharmacol 2011, 61: 333–372.
Gonzales EB, Kawate T, Gouaux E. Pore architecture and ion sites in acid-sensing ion channels and P2X receptors. Nature 2009, 460: 599–604.
Baron A, Lingueglia E. Pharmacology of acid-sensing ion channels—Physiological and therapeutical perspectives. Neuropharmacology 2015, 94: 19–35.
Donkor ES. Stroke in the 21st century: A snapshot of the burden, epidemiology, and quality of life. Stroke Res Treat 2018, 2018: 3238165.
Goldberg DS, McGee SJ. Pain as a global public health priority. BMC Public Health 2011, 11: 770.
Walton C, King R, Rechtman L, Kaye W, Leray E, Marrie RA. Rising prevalence of multiple sclerosis worldwide: Insights from the Atlas of MS, third edition. Mult Scler 2020, 26: 1816–1821.
World Health Organization. Epilepsy, https://www.who.int/news-room/fact-sheets/detail/epilepsy. 2022.
Lee CH, Chen CC. Roles of ASICs in nociception and proprioception. Adv Exp Med Biol 2018, 1099: 37–47.
Rook ML, Musgaard M, MacLean DM. Coupling structure with function in acid-sensing ion channels: Challenges in pursuit of proton sensors. J Physiol 2021, 599: 417–430.
Pattison LA, Callejo G, St John Smith E. Evolution of acid nociception: Ion channels and receptors for detecting acid. Philos Trans R Soc Lond B Biol Sci 2019, 374: 20190291.
Uchitel OD, González Inchauspe C, Weissmann C. Synaptic signals mediated by protons and acid-sensing ion channels. Synapse 2019, 73: e22120.
Inoue K, Tsuda M. Nociceptive signaling mediated by P2X3, P2X4 and P2X7 receptors. Biochem Pharmacol 2021, 187: 114309.
Martin-Aragon Baudel M, Espinosa-Tanguma R, Nieves-Cintron M, Navedo MF. Purinergic signaling during hyperglycemia in vascular smooth muscle cells. Front Endocrinol (Lausanne) 2020, 11: 329.
Aslam M, Gündüz D, Troidl C, Heger J, Hamm CW, Schulz R. Purinergic regulation of endothelial barrier function. Int J Mol Sci 2021, 22: 1207.
Shokoples BG, Paradis P, Schiffrin EL. P2X7 receptors: An untapped target for the management of cardiovascular disease. Arterioscler Thromb Vasc Biol 2021, 41: 186–199.
Agostinho P, Madeira D, Dias L, Simões AP, Cunha RA, Canas PM. Purinergic signaling orchestrating neuron-glia communication. Pharmacol Res 2020, 162: 105253.
Zhang RJ, Yin YF, Xie XJ, Gu HF. Acid-sensing ion channels: Linking extracellular acidification with atherosclerosis. Clin Chimica Acta 2020, 502: 183–190.
Gonzales EB, Sumien N. Acidity and acid-sensing ion channels in the normal and Alzheimer’s disease brain. J Alzheimers Dis 2017, 57: 1137–1144.
Wang JJ, Xu TL. Acid-sensing ion channels as a target for neuroprotection: Acidotoxicity revisited. Sheng Li Xue Bao 2016, 68: 403–413.
Storozhuk M, Cherninskyi A, Maximyuk O, Isaev D, Krishtal O. Acid-sensing ion channels: Focus on physiological and some pathological roles in the brain. Curr Neuropharmacol 2021, 19: 1570–1589.
Duveau A, Bertin E, Boué-Grabot E. Implication of neuronal Versus microglial P2X4 receptors in central nervous system disorders. Neurosci Bull 2020, 36: 1327–1343.
Du J, Reznikov LR, Price MP, Zha XM, Lu Y, Moninger TO, et al. Protons are a neurotransmitter that regulates synaptic plasticity in the lateral amygdala. Proc Natl Acad Sci U S A 2014, 111: 8961–8966.
Kreple CJ, Lu Y, Taugher RJ, Schwager-Gutman AL, Du J, Stump M, et al. Acid-sensing ion channels contribute to synaptic transmission and inhibit cocaine-evoked plasticity. Nat Neurosci 2014, 17: 1083–1091.
Li HS, Su XY, Song XL, Qi X, Li Y, Wang RQ, et al. Protein kinase C lambda mediates acid-sensing ion channel 1a-dependent cortical synaptic plasticity and pain hypersensitivity. J Neurosci 2019, 39: 5773–5793.
González-Inchauspe C, Urbano FJ, di Guilmi MN, Uchitel OD. Acid-sensing ion channels activated by evoked released protons modulate synaptic transmission at the mouse Calyx of held synapse. J Neurosci 2017, 37: 2589–2599.
Mango D, Nisticò R. Acid-sensing ion channel 1a is involved in N-methyl D-aspartate receptor-dependent long-term depression in the Hippocampus. Front Pharmacol 2019, 10: 555.
Pankratov Y, Castro E, Miras-Portugal MT, Krishtal O. A purinergic component of the excitatory postsynaptic current mediated by P2X receptors in the CA1 neurons of the rat hippocampus. Eur J Neurosci 1998, 10: 3898–3902.
Pankratov Y, Lalo U, Krishtal O, Verkhratsky A. P2X receptor-mediated excitatory synaptic currents in somatosensory cortex. Mol Cell Neurosci 2003, 24: 842–849.
Chiang PH, Chien TC, Chen CC, Yanagawa Y, Lien CC. ASIC-dependent LTP at multiple glutamatergic synapses in amygdala network is required for fear memory. Sci Rep 2015, 5: 10143.
Li WG, Liu MG, Deng S, Liu YM, Shang L, Ding J, et al. ASIC1a regulates insular long-term depression and is required for the extinction of conditioned taste aversion. Nat Commun 2016, 7: 13770.
Pankratov YV, Lalo UV, Krishtal OA. Role for P2X receptors in long-term potentiation. J Neurosci 2002, 22: 8363–8369.
Birdsong WT, Fierro L, Williams FG, Spelta V, Naves LA, Knowles M, et al. Sensing muscle ischemia: Coincident detection of acid and ATP via interplay of two ion channels. Neuron 2010, 68: 739–749.
Stephan G, Huang L, Tang Y, Vilotti S, Fabbretti E, Yu Y, et al. The ASIC3/P2X3 cognate receptor is a pain-relevant and ligand-gated cationic channel. Nat Commun 2018, 9: 1354.
Krishtal OA, Pidoplichko VI. A receptor for protons in the nerve cell membrane. Neuroscience 1980, 5: 2325–2327.
Waldmann R, Champigny G, Bassilana F, Heurteaux C, Lazdunski M. A proton-gated cation channel involved in acid-sensing. Nature 1997, 386: 173–177.
Gründer S, Geissler HS, Bässler EL, Ruppersberg JP. A new member of acid-sensing ion channels from pituitary gland. Neuroreport 2000, 11: 1607–1611.
Lingueglia E, de Weille JR, Bassilana F, Heurteaux C, Sakai H, Waldmann R, et al. A modulatory subunit of acid sensing ion channels in brain and dorsal root ganglion cells. J Biol Chem 1997, 272: 29778–29783.
Price MP, Snyder PM, Welsh MJ. Cloning and expression of a novel human brain Na+ channel. J Biol Chem 1996, 271: 7879–7882.
García-Añoveros J, Derfler B, Neville-Golden J, Hyman BT, Corey DP. BNaC1 and BNaC2 constitute a new family of human neuronal sodium channels related to degenerins and epithelial sodium channels. Proc Natl Acad Sci U S A 1997, 94: 1459–1464.
Wemmie JA, Askwith CC, Lamani E, Cassell MD, Freeman JH Jr, Welsh MJ. Acid-sensing ion channel 1 is localized in brain regions with high synaptic density and contributes to fear conditioning. J Neurosci 2003, 23: 5496–5502.
Ugawa S, Ueda T, Takahashi E, Hirabayashi Y, Yoneda T, Komai S, et al. Cloning and functional expression of ASIC-beta2, a splice variant of ASIC-beta. Neuroreport 2001, 12: 2865–2869.
Zha XM. Acid-sensing ion channels: Trafficking and synaptic function. Mol Brain 2013, 6: 1.
Baron A, Waldmann R, Lazdunski M. ASIC-like, proton-activated currents in rat hippocampal neurons. J Physiol 2002, 539: 485–494.
Wemmie JA, Taugher RJ, Kreple CJ. Acid-sensing ion channels in pain and disease. Nat Rev Neurosci 2013, 14: 461–471.
Coscoy S, de Weille JR, Lingueglia E, Lazdunski M. The pre-transmembrane 1 domain of acid-sensing ion channels participates in the ion pore. J Biol Chem 1999, 274: 10129–10132.
Akopian AN, Chen CC, Ding Y, Cesare P, Wood JN. A new member of the acid-sensing ion channel family. Neuroreport 2000, 11: 2217–2222.
Cristofori-Armstrong B, Saez NJ, Chassagnon IR, King GF, Rash LD. The modulation of acid-sensing ion channel 1 by PcTx1 is pH-, subtype- and species-dependent: Importance of interactions at the channel subunit interface and potential for engineering selective analogues. Biochem Pharmacol 2019, 163: 381–390.
Buta A, Maximyuk O, Kovalskyy D, Sukach V, Vovk M, Ievglevskyi O, et al. Novel potent orthosteric antagonist of ASIC1a prevents NMDAR-dependent LTP induction. J Med Chem 2015, 58: 4449–4461.
Joch M, Ase AR, Chen CXQ, MacDonald PA, Kontogiannea M, Corera AT, et al. Parkin-mediated monoubiquitination of the PDZ protein PICK1 regulates the activity of acid-sensing ion channels. Mol Biol Cell 2007, 18: 3105–3118.
Duan B, Wang YZ, Yang T, Chu XP, Yu Y, Huang Y, et al. Extracellular spermine exacerbates ischemic neuronal injury through sensitization of ASIC1a channels to extracellular acidosis. J Neurosci 2011, 31: 2101–2112.
Gobetto MN, González-Inchauspe C, Uchitel OD. Histamine and corticosterone modulate acid sensing ion channels (ASICs) dependent long-term potentiation at the mouse anterior cingulate cortex. Neuroscience 2021, 460: 145–160.
Krishtal OA, Osipchuk YV, Shelest TN, Smirnoff SV. Rapid extracellular pH transients related to synaptic transmission in rat hippocampal slices. Brain Res 1987, 436: 352–356.
Yu Z, Wu YJ, Wang YZ, Liu DS, Song XL, Jiang Q, et al. The acid-sensing ion channel ASIC1a mediates striatal synapse remodeling and procedural motor learning. Sci Signal 2018, 11: eaar4481.
Wemmie JA, Chen J, Askwith CC, Hruska-Hageman AM, Price MP, Nolan BC, et al. The acid-activated ion channel ASIC contributes to synaptic plasticity, learning, and memory. Neuron 2002, 34: 463–477.
Cho JH, Askwith CC. Presynaptic release probability is increased in hippocampal neurons from ASIC1 knockout mice. J Neurophysiol 2008, 99: 426–441.
Liu MG, Li HS, Li WG, Wu YJ, Deng SN, Huang C, et al. Acid-sensing ion channel 1a contributes to hippocampal LTP inducibility through multiple mechanisms. Sci Rep 2016, 6: 23350.
Mango D, Braksator E, Battaglia G, Marcelli S, Mercuri NB, Feligioni M, et al. Acid-sensing ion channel 1a is required for mGlu receptor dependent long-term depression in the hippocampus. Pharmacol Res 2017, 119: 12–19.
Price MP, Gong H, Parsons MG, Kundert JR, Reznikov LR, Bernardinelli L, et al. Localization and behaviors in null mice suggest that ASIC1 and ASIC2 modulate responses to aversive stimuli. Genes Brain Behav 2014, 13: 179–194.
Wang Q, Wang Q, Song XL, Jiang Q, Wu YJ, Li Y, et al. Fear extinction requires ASIC1a-dependent regulation of hippocampal-prefrontal correlates. Sci Adv 2018, 4: eaau3075.
Ghobbeh A, Taugher RJ, Alam SM, Fan R, LaLumiere RT, Wemmie JA. A novel role for acid-sensing ion channels in Pavlovian reward conditioning. Genes Brain Behav 2019, 18: e12531.
Jiang Q, Wang CM, Fibuch EE, Wang JQ, Chu XP. Differential regulation of locomotor activity to acute and chronic cocaine administration by acid-sensing ion channel 1a and 2 in adult mice. Neuroscience 2013, 246: 170–178.
Gutman AL, Cosme CV, Noterman MF, Worth WR, Wemmie JA, LaLumiere RT. Overexpression of ASIC1A in the nucleus accumbens of rats potentiates cocaine-seeking behavior. Addict Biol 2020, 25: e12690.
Ziemann AE, Allen JE, Dahdaleh NS, Drebot II, Coryell MW, Wunsch AM, et al. The amygdala is a chemosensor that detects carbon dioxide and acidosis to elicit fear behavior. Cell 2009, 139: 1012–1021.
Lin B, Alganem K, O’Donovan SM, Jin Z, Naghavi F, Miller OA, et al. Activation of acid-sensing ion channels by carbon dioxide regulates amygdala synaptic protein degradation in memory reconsolidation. Mol Brain 2021, 14: 78.
Mir FA, Jha SK. Locus coeruleus acid-sensing ion channels modulate sleep–wakefulness and state transition from NREM to REM sleep in the rat. Neurosci Bull 2021, 37: 684–700.
Khakh BS, Burnstock G. The double life of ATP. Sci Am 2009, 301(84–90): 92.
Holton FA, Holton P. The capillary dilator substances in dry powders of spinal roots; a possible role of adenosine triphosphate in chemical transmission from nerve endings. J Physiol 1954, 126: 124–140.
Holton P. The liberation of adenosine triphosphate on antidromic stimulation of sensory nerves. J Physiol 1959, 145: 494–504.
Burnstock G. Purinergic nerves. Pharmacol Rev 1972, 24: 509–581.
Khakh BS, North RA. Neuromodulation by extracellular ATP and P2X receptors in the CNS. Neuron 2012, 76: 51–69.
Krishtal OA, Marchenko SM, Pidoplichko VI. Receptor for ATP in the membrane of mammalian sensory neurones. Neurosci Lett 1983, 35: 41–45.
Jahr CE, Jessell TM. ATP excites a subpopulation of rat dorsal horn neurones. Nature 1983, 304: 730–733.
Benham CD, Tsien RW. A novel receptor-operated Ca2+-permeable channel activated by ATP in smooth muscle. Nature 1987, 328: 275–278.
Kolb HA, Wakelam MJO. Transmitter-like action of ATP on patched membranes of cultured myoblasts and myotubes. Nature 1983, 303: 621–623.
Illes P, Müller CE, Jacobson KA, Grutter T, Nicke A, Fountain SJ, et al. Update of P2X receptor properties and their pharmacology: IUPHAR Review 30. Br J Pharmacol 2021, 178: 489–514.
McCarthy AE, Yoshioka C, Mansoor SE. Full-length P2X7 structures reveal how palmitoylation prevents channel desensitization. Cell 2019, 179: 659-670.e13.
Burnstock G. Introduction and perspective, historical note. Front Cell Neurosci 2013, 7: 227.
Loesch A. On P2X receptors in the brain: Microvessels. Dedicated to the memory of the late Professor Geoffrey Burnstock (1929–2020). Cell Tissue Res 2021, 384: 577–588.
North RA. Molecular physiology of P2X receptors. Physiol Rev 2002, 82: 1013–1067.
Ruppelt A, Ma W, Borchardt K, Silberberg SD, Soto F. Genomic structure, developmental distribution and functional properties of the chicken P2X(5) receptor. J Neurochem 2001, 77: 1256–1265.
Hausmann R, Kless A, Schmalzing G. Key sites for P2X receptor function and multimerization: Overview of mutagenesis studies on a structural basis. Curr Med Chem 2015, 22: 799–818.
Mansoor SE, Lü W, Oosterheert W, Shekhar M, Tajkhorshid E, Gouaux E. X-ray structures define human P2X3 receptor gating cycle and antagonist action. Nature 2016, 538: 66–71.
Taruno A, Nomura K, Kusakizako T, Ma Z, Nureki O, Foskett JK. Taste transduction and channel synapses in taste buds. Pflugers Arch Eur J Physiol 2021, 473: 3–13.
Mittal R, Chan B, Grati M, Mittal J, Patel K, Debs LH, et al. Molecular structure and regulation of P2X receptors with a special emphasis on the role of P2X2 in the auditory system. J Cell Physiol 2016, 231: 1656–1670.
Krajewski JL. P2X3-containing receptors as targets for the treatment of chronic pain. Neurotherapeutics 2020, 17: 826–838.
Nieber K, Poelchen W, Illes P. Role of ATP in fast excitatory synaptic potentials in locus coeruleus neurones of the rat. Br J Pharmacol 1997, 122: 423–430.
Silinsky EM, Gerzanich V, Vanner SM. ATP mediates excitatory synaptic transmission in mammalian neurones. Br J Pharmacol 1992, 106: 762–763.
Mori M, Heuss C, Gähwiler BH, Gerber U. Fast synaptic transmission mediated by P2X receptors in CA3 pyramidal cells of rat hippocampal slice cultures. J Physiol 2001, 535: 115–123.
Bardoni R, Goldstein PA, Lee CJ, Gu JG, MacDermott AB. ATP P2X receptors mediate fast synaptic transmission in the dorsal horn of the rat spinal cord. J Neurosci 1997, 17: 5297–5304.
Jo YH, Donier E, Martinez A, Garret M, Toulmé E, Boué-Grabot E. Cross-talk between P2X4 and gamma-aminobutyric acid, type A receptors determines synaptic efficacy at a central synapse. J Biol Chem 2011, 286: 19993–20004.
Jo YH, Role LW. Coordinate release of ATP and GABA at in vitro synapses of lateral hypothalamic neurons. J Neurosci 2002, 22: 4794–4804.
Pankratov Y, Lalo U, Verkhratsky A, North RA. Quantal release of ATP in mouse cortex. J Gen Physiol 2007, 129: 257–265.
Gu JG, MacDermott AB. Activation of ATP P2X receptors elicits glutamate release from sensory neuron synapses. Nature 1997, 389: 749–753.
Lalo U, Palygin O, Verkhratsky A, Grant SGN, Pankratov Y. ATP from synaptic terminals and astrocytes regulates NMDA receptors and synaptic plasticity through PSD-95 multi-protein complex. Sci Rep 2016, 6: 33609.
Montilla A, Mata GP, Matute C, Domercq M. Contribution of P2X4 receptors to CNS function and pathophysiology. Int J Mol Sci 2020, 21: 5562.
Ge WP, Yang XJ, Zhang Z, Wang HK, Shen W, Deng QD, et al. Long-term potentiation of neuron-glia synapses mediated by Ca2+-permeable AMPA receptors. Science 2006, 312: 1533–1537.
Duan S, Anderson CM, Keung EC, Chen Y, Chen Y, Swanson RA. P2X7 receptor-mediated release of excitatory amino acids from astrocytes. J Neurosci 2003, 23: 1320–1328.
Boscardin E, Alijevic O, Hummler E, Frateschi S, Kellenberger S. The function and regulation of acid-sensing ion channels (ASICs) and the epithelial Na+ channel (ENaC): IUPHAR Review 19. Br J Pharmacol 2016, 173: 2671–2701.
Sivils A, Yang F, Wang JQ, Chu XP. Acid-sensing ion channel 2: Function and modulation. Membranes 2022, 12: 113.
Xiong ZG, Zhu XM, Chu XP, Minami M, Hey J, Wei WL, et al. Neuroprotection in ischemia: Blocking calcium-permeable acid-sensing ion channels. Cell 2004, 118: 687–698.
Wang YZ, Wang JJ, Huang Y, Liu F, Zeng WZ, Li Y, et al. Correction: Tissue acidosis induces neuronal necroptosis via ASIC1a channel independent of its ionic conduction. eLife 2016, 5: e14128.
Sluka KA, Winter OC, Wemmie JA. Acid-sensing ion channels: A new target for pain and CNS diseases. Curr Opin Drug Discov Devel 2009, 12: 693–704.
Ievglevskyi O, Isaev D, Netsyk O, Romanov A, Fedoriuk M, Maximyuk O, et al. Acid-sensing ion channels regulate spontaneous inhibitory activity in the hippocampus: Possible implications for epilepsy. Philos Trans R Soc Lond B Biol Sci 2016, 371: 20150431.
Lai K, Song XL, Shi HS, Qi X, Li CY, Fang J, et al. Bilirubin enhances the activity of ASIC channels to exacerbate neurotoxicity in neonatal hyperbilirubinemia in mice. Sci Transl Med 2020, 12: eaax1337.
Bolshakov KV, Essin KV, Buldakova SL, Dorofeeva NA, Skatchkov SN, Eaton MJ, et al. Characterization of acid-sensitive ion channels in freshly isolated rat brain neurons. Neuroscience 2002, 110: 723–730.
Alijevic O, Bignucolo O, Hichri E, Peng Z, Kucera JP, Kellenberger S. Slowing of the time course of acidification decreases the acid-sensing ion channel 1a current amplitude and modulates action potential firing in neurons. Front Cell Neurosci 2020, 14: 41.
Xiong ZG, Chu XP, Simon RP. Acid sensing ion channels—novel therapeutic targets for ischemic brain injury. Front Biosci 2007, 12: 1376–1386.
Xiong ZG, Chu XP, Simon RP. Ca2+-permeable acid-sensing ion channels and ischemic brain injury. J Membrane Biol 2006, 209: 59–68.
Wang JJ, Liu F, Yang F, Wang YZ, Qi X, Li Y, et al. Nat Commun 2020, 11: 475.
Sirven JI. Epilepsy: A spectrum disorder. Cold Spring Harb Perspect Med 2015, 5: a022848.
Simon RP, Benowitz N, Hedlund R, Copeland J. Influence of the blood-brain pH gradient on brain phenobarbital uptake during status epilepticus. J Pharmacol Exp Ther 1985, 234: 830–835.
Somjen GG. Acidification of interstitial fluid in hippocampal formation caused by seizures and by spreading depression. Brain Res 1984, 311: 186–188.
Chesler M, Kaila K. Modulation of pH by neuronal activity. Trends Neurosci 1992, 15: 396–402.
Ziemann AE, Schnizler MK, Albert GW, Severson MA, Howard MA III, Welsh MJ, et al. Seizure termination by acidosis depends on ASIC1a. Nat Neurosci 2008, 11: 816–822.
Xiong ZG, Pignataro G, Li M, Chang SY, Simon RP. Acid-sensing ion channels (ASICs) as pharmacological targets for neurodegenerative diseases. Curr Opin Pharmacol 2008, 8: 25–32.
Mango D, Nisticò R. Neurodegenerative disease: What potential therapeutic role of acid-sensing ion channels? Front Cell Neurosci 2021, 15: 730641.
Ortega-Ramírez A, Vega R, Soto E. Acid-sensing ion channels as potential therapeutic targets in neurodegeneration and neuroinflammation. Mediators Inflamm 2017, 2017: 3728096.
Salter MW, Stevens B. Microglia emerge as central players in brain disease. Nat Med 2017, 23: 1018–1027.
Ma CL, Sun H, Yang L, Wang XT, Gao S, Chen XW, et al. Acid-sensing ion channel 1a modulates NMDA receptor function through targeting NR1/NR2A/NR2B triheteromeric receptors. Neuroscience 2019, 406: 389–404.
Storozhuk M, Kondratskaya E, Nikolaenko L, Krishtal O. A modulatory role of ASICs on GABAergic synapses in rat hippocampal cell cultures. Mol Brain 2016, 9: 90.
Hynd MR, Scott HL, Dodd PR. Glutamate-mediated excitotoxicity and neurodegeneration in Alzheimer’s disease. Neurochem Int 2004, 45: 583–595.
Zholos AV, Moroz OF, Storozhuk MV. Curcuminoids and novel opportunities for the treatment of Alzheimer’s disease: Which molecules are actually effective? Curr Mol Pharmacol 2019, 12: 12–26.
Khachaturian AS, Zandi PP, Lyketsos CG, Hayden KM, Skoog I, Norton MC, et al. Antihypertensive medication use and incident Alzheimer disease: The Cache County Study. Arch Neurol 2006, 63: 686–692.
Chuang YF, Breitner JCS, Chiu YL, Khachaturian A, Hayden K, Corcoran C, et al. Use of diuretics is associated with reduced risk of Alzheimer’s disease: The Cache County Study. Neurobiol Aging 2014, 35: 2429–2435.
Mango D, Nisticò R. Role of ASIC1a in aβ-induced synaptic alterations in the hippocampus. Pharmacol Res 2018, 131: 61–65.
Wu Y, Qin D, Yang H, Fu H. Evidence for the participation of acid-sensing ion channels (ASICs) in the antinociceptive effect of curcumin in a formalin-induced orofacial inflammatory model. Cell Mol Neurobiol 2017, 37: 635–642.
Shteinikov VY, Tikhonova TB, Korkosh VS, Tikhonov DB. Potentiation and block of ASIC1a by memantine. Cell Mol Neurobiol 2018, 38: 869–881.
Goldenberg MM. Multiple sclerosis review. P T 2012, 37: 175–184.
Vergo S, Craner MJ, Etzensperger R, Attfield K, Friese MA, Newcombe J, et al. Acid-sensing ion channel 1 is involved in both axonal injury and demyelination in multiple sclerosis and its animal model. Brain 2011, 134: 571–584.
Friese MA, Craner MJ, Etzensperger R, Vergo S, Wemmie JA, Welsh MJ, et al. Acid-sensing ion channel-1 contributes to axonal degeneration in autoimmune inflammation of the central nervous system. Nat Med 2007, 13: 1483–1489.
Arun T, Tomassini V, Sbardella E, de Ruiter MB, Matthews L, Leite MI, et al. Targeting ASIC1 in primary progressive multiple sclerosis: Evidence of neuroprotection with amiloride. Brain 2013, 136: 106–115.
Beitz JM. Parkinson’s disease: A review. Front Biosci (Schol Ed) 2014, 6: 65–74.
Arias RL, Sung MLA, Vasylyev D, Zhang MY, Albinson K, Kubek K, et al. Amiloride is neuroprotective in an MPTP model of Parkinson’s disease. Neurobiol Dis 2008, 31: 334–341.
Tabrizi SJ, Flower MD, Ross CA, Wild EJ. Huntington disease: New insights into molecular pathogenesis and therapeutic opportunities. Nat Rev Neurol 2020, 16: 529–546.
Wong HK, Bauer PO, Kurosawa M, Goswami A, Washizu C, Machida Y, et al. Blocking acid-sensing ion channel 1 alleviates Huntington’s disease pathology via an ubiquitin-proteasome system-dependent mechanism. Hum Mol Genet 2008, 17: 3223–3235.
Coryell MW, Wunsch AM, Haenfler JM, Allen JE, Schnizler M, Ziemann AE, et al. Acid-sensing ion channel-1a in the amygdala, a novel therapeutic target in depression-related behavior. J Neurosci 2009, 29: 5381–5388.
Fedoriuk MP, Cherninskyi AO, Maximyuk OP, Isaev DS, Bogovyk RI, Venhreniuk AV, et al. Inhibition of brain asics affects hippocampal theta-rhythm and openfield behavior in rats. Fiziol Zh 2019, 65: 15–19.
Yellepeddi V, Sayre C, Burrows A, Watt K, Davies S, Strauss J, et al. Stability of extemporaneously compounded amiloride nasal spray. PLoS One 2020, 15: e0232435.
Leibold NK, van den Hove D, Viechtbauer W, Kenis G, Goossens L, Lange I, et al. Amiloride-sensitive cation channel 2 genotype affects the response to a carbon dioxide panic challenge. J Psychopharmacol 2017, 31: 1294–1301.
Gugliandolo A, Gangemi C, Caccamo D, Currò M, Pandolfo G, Quattrone D, et al. The RS685012 polymorphism of ACCN2, the human ortholog of murine acid-sensing ion channel (ASIC1) gene, is highly represented in patients with panic disorder. Neuromolecular Med 2016, 18: 91–98.
Dietrich CJ, Morad M. Synaptic acidification enhances GABAA signaling. J Neurosci 2010, 30: 16044–16052.
Palmer MJ, Hull C, Vigh J, von Gersdorff H. Synaptic cleft acidification and modulation of short-term depression by exocytosed protons in retinal bipolar cells. J Neurosci 2003, 23: 11332–11341.
Stawarski M, Hernandez RX, Feghhi T, Borycz JA, Lu Z, Agarwal AB, et al. Neuronal glutamatergic synaptic clefts alkalinize rather than acidify during neurotransmission. J Neurosci 2020, 40: 1611–1624.
Rash LD. Acid-sensing ion channel pharmacology, past, present, and future …. Adv Pharmacol 2017, 79: 35–66.
Tikhonov DB, Magazanik LG, Nagaeva EI. Ligands of acid-sensing ion channel 1a: Mechanisms of action and binding sites. Acta Naturae 2019, 11: 4–13.
Allen NJ, Attwell D. Modulation of ASIC channels in rat cerebellar Purkinje neurons by ischaemia-related signals. J Physiol 2002, 543: 521–529.
Nagaeva EI, Tikhonova TB, Magazanik LG, Tikhonov DB. Histamine selectively potentiates acid-sensing ion channel 1a. Neurosci Lett 2016, 632: 136–140.
Park JH, Kim YC. P2X7 receptor antagonists: A patent review (2010–2015). Expert Opin Ther Pat 2017, 27: 257–267.
Pevarello P, Bovolenta S, Tarroni P, Za L, Severi E, Torino D, et al. P2X7 antagonists for CNS indications: Recent patent disclosures. Pharm Pat Anal 2017, 6: 61–76.
Andrejew R, Oliveira-Giacomelli Á, Ribeiro DE, Glaser T, Arnaud-Sampaio VF, Lameu C, et al. The P2X7 receptor: Central hub of brain diseases. Front Mol Neurosci 2020, 13: 124.
Pelegrin P. P2X7 receptor and the NLRP3 inflammasome: Partners in crime. Biochem Pharmacol 2021, 187: 114385.
Adinolfi E, Giuliani AL, de Marchi E, Pegoraro A, Orioli E, di Virgilio F. The P2X7 receptor: A main player in inflammation. Biochem Pharmacol 2018, 151: 234–244.
Guo J, Fu X, Cui X, Fan M. Contributions of purinergic P2X3 receptors within the midbrain periaqueductal gray to diabetes-induced neuropathic pain. J Physiol Sci 2015, 65: 99–104.
Kuan YH, Shih HC, Tang SC, Jeng JS, Shyu BC. Targeting P2X7 receptor for the treatment of central post-stroke pain in a rodent model. Neurobiol Dis 2015, 78: 134–145.
Falzoni S, Donvito G, Di Virgilio F. Detecting adenosine triphosphate in the pericellular space. Interface Focus 2013, 3: 20120101.
He Y, Taylor N, Fourgeaud L, Bhattacharya A. The role of microglial P2X7: Modulation of cell death and cytokine release. J Neuroinflammation 2017, 14: 1–13.
Lord B, Ameriks MK, Wang Q, Fourgeaud L, Vliegen M, Verluyten W, et al. A novel radioligand for the ATP-gated ion channel P2X7: [3H]JNJ-54232334. Eur J Pharmacol 2015, 765: 551–559.
Bhattacharya A, Lord B, Grigoleit JS, He Y, Fraser I, Campbell SN, et al. Neuropsychopharmacology of JNJ-55308942: Evaluation of a clinical candidate targeting P2X7 ion channels in animal models of neuroinflammation and anhedonia. Neuropsychopharmacology 2018, 43: 2586–2596.
Cheng RD, Ren JJ, Zhang YY, Ye XM. P2X4 receptors expressed on microglial cells in post-ischemic inflammation of brain ischemic injury. Neurochem Int 2014, 67: 9–13.
Li F, Wang L, Li JW, Gong M, He L, Feng R, et al. Hypoxia induced amoeboid microglial cell activation in postnatal rat brain is mediated by ATP receptor P2X4. BMC Neurosci 2011, 12: 111.
Verma R, Cronin CG, Hudobenko J, Venna VR, McCullough LD, Liang BT. Deletion of the P2X4 receptor is neuroprotective acutely, but induces a depressive phenotype during recovery from ischemic stroke. Brain Behav Immun 2017, 66: 302–312.
Wixey JA, Reinebrant HE, Carty ML, Buller KM. Delayed P2X4R expression after hypoxia-ischemia is associated with microglia in the immature rat brain. J Neuroimmunol 2009, 212: 35–43.
Ozaki T, Muramatsu R, Sasai M, Yamamoto M, Kubota Y, Fujinaka T, et al. The P2X4 receptor is required for neuroprotection via ischemic preconditioning. Sci Rep 2016, 6: 25893.
Xiao J, Huang Y, Li X, Li L, Yang T, Huang L, et al. TNP-ATP is beneficial for treatment of neonatal hypoxia-induced hypomyelination and cognitive decline. Neurosci Bull 2016, 32: 99–107.
Beamer E, Conte G, Engel T. ATP release during seizures - A critical evaluation of the evidence. Brain Res Bull 2019, 151: 65–73.
Ulmann L, Levavasseur F, Avignone E, Peyroutou R, Hirbec H, Audinat E, et al. Involvement of P2X4 receptors in hippocampal microglial activation after status epilepticus. Glia 2013, 61: 1306–1319.
Engel T, Gomez-Villafuertes R, Tanaka K, Mesuret G, Sanz-Rodriguez A, Garcia-Huerta P, et al. Seizure suppression and neuroprotection by targeting the purinergic P2X7 receptor during status epilepticus in mice. FASEB J 2012, 26: 1616–1628.
Huang C, Chi XS, Li R, Hu X, Xu HX, Li JM, et al. Inhibition of P2X7 receptor ameliorates nuclear factor-kappa B mediated neuroinflammation induced by status epilepticus in rat hippocampus. J Mol Neurosci 2017, 63: 173–184.
Jimenez-Pacheco A, Mesuret G, Sanz-Rodriguez A, Tanaka K, Mooney C, Conroy R, et al. Increased neocortical expression of the P2X7 receptor after status epilepticus and anticonvulsant effect of P2X7 receptor antagonist A-438079. Epilepsia 2013, 54: 1551–1561.
Mesuret G, Engel T, Hessel EV, Sanz-Rodriguez A, Jimenez-Pacheco A, Miras-Portugal MT, et al. P2X7 receptor inhibition interrupts the progression of seizures in immature rats and reduces hippocampal damage. CNS Neurosci Ther 2014, 20: 556–564.
Rodriguez-Alvarez N, Jimenez-Mateos EM, Engel T, Quinlan S, Reschke CR, Conroy RM, et al. Effects of P2X7 receptor antagonists on hypoxia-induced neonatal seizures in mice. Neuropharmacology 2017, 116: 351–363.
Avignone E, Ulmann L, Levavasseur F, Rassendren F, Audinat E. Status epilepticus induces a particular microglial activation state characterized by enhanced purinergic signaling. J Neurosci 2008, 28: 9133–9144.
Zhou X, Ma LM, Xiong Y, Huang H, Yuan JX, Li RH, et al. Upregulated P2X3 receptor expression in patients with intractable temporal lobe epilepsy and in a rat model of epilepsy. Neurochem Res 2016, 41: 1263–1273.
Xia J, Wang H, Zhang Q, Han Z. Modulation of P2X purinoceptor 3 (P2X3) in pentylenetetrazole-induced kindling epilepsy in rats. Med Sci Monit 2018, 24: 6165–6177.
Edwards C, Klekot O, Halugan L, Korchev Y. Follow your nose: A key clue to understanding and treating COVID-19. Front Endocrinol (Lausanne) 2021, 12: 747744.
Ceban F, Ling S, Lui LMW, Lee Y, Gill H, Teopiz KM, et al. Fatigue and cognitive impairment in Post-COVID-19 Syndrome: A systematic review and meta-analysis. Brain Behav Immun 2022, 101: 93–135.
Wan D, Du T, Hong W, Chen L, Que H, Lu S, et al. Neurological complications and infection mechanism of SARS-CoV-2. Signal Transduct Target Ther 2021, 6: 406.
Lukiw WJ, Pogue A, Hill JM. SARS-CoV-2 infectivity and neurological targets in the brain. Cell Mol Neurobiol 2022, 42: 217–224.
Hamming I, Timens W, Bulthuis MLC, Lely AT, Navis GJ, van Goor H. Tissue distribution of ACE2 protein, the functional receptor for SARS coronavirus. A first step in understanding SARS pathogenesis. J Pathol 2004, 203: 631–637.
Cui H, Su S, Cao Y, Ma C, Qiu W. The altered anatomical distribution of ACE2 in the brain with Alzheimer’s disease pathology. Front Cell Dev Biol 2021, 9: 684874.
Di Virgilio F, Tang Y, Sarti AC, Rossato M. A rationale for targeting the P2X7 receptor in Coronavirus disease 19. Br J Pharmacol 2020, 177: 4990–4994.
Heppner FL, Ransohoff RM, Becher B. Immune attack: The role of inflammation in Alzheimer disease. Nat Rev Neurosci 2015, 16: 358–372.
McGeer PL, Rogers J, McGeer EG. Inflammation, antiinflammatory agents, and Alzheimer’s disease: The last 22 years. J Alzheimers Dis 2016, 54: 853–857.
Sáez-Orellana F, Fuentes-Fuentes MC, Godoy PA, Silva-Grecchi T, Panes JD, Guzmán L, et al. P2X receptor overexpression induced by soluble oligomers of amyloid beta peptide potentiates synaptic failure and neuronal dyshomeostasis in cellular models of Alzheimer’s disease. Neuropharmacology 2018, 128: 366–378.
Sáez-Orellana F, Godoy PA, Bastidas CY, Silva-Grecchi T, Guzmán L, Aguayo LG, et al. ATP leakage induces P2XR activation and contributes to acute synaptic excitotoxicity induced by soluble oligomers of β-amyloid peptide in hippocampal neurons. Neuropharmacology 2016, 100: 116–123.
Rampe D, Wang L, Ringheim GE. P2X7 receptor modulation of β-amyloid- and LPS-induced cytokine secretion from human macrophages and microglia. J Neuroimmunol 2004, 147: 56–61.
Sanz JM, Chiozzi P, Ferrari D, Colaianna M, Idzko M, Falzoni S, et al. Activation of microglia by amyloid{beta}requires P2X7 receptor expression. J Immunol 2009, 182: 4378–4385.
Skaper SD, Facci L, Culbert AA, Evans NA, Chessell I, Davis JB, et al. P2X(7) receptors on microglial cells mediate injury to cortical neurons in vitro. Glia 2006, 54: 234–242.
Kim SY, Moon JH, Lee HG, Kim SU, Lee YB. ATP released from beta-amyloid-stimulated microglia induces reactive oxygen species production in an autocrine fashion. Exp Mol Med 2007, 39: 820–827.
Lee HG, Won SM, Gwag BJ, Lee YB. Microglial P2X7 receptor expression is accompanied by neuronal damage in the cerebral cortex of the APPswe/PS1dE9 mouse model of Alzheimer’s disease. Exp Mol Med 2011, 43: 7–14.
Diaz-Hernandez JI, Gomez-Villafuertes R, León-Otegui M, Hontecillas-Prieto L, del Puerto A, Trejo JL, et al. In vivo P2X7 inhibition reduces amyloid plaques in Alzheimer’s disease through GSK3β and secretases. Neurobiol Aging 2012, 33: 1816–1828.
León-Otegui M, Gómez-Villafuertes R, Díaz-Hernández JI, Díaz-Hernández M, Miras-Portugal MT, Gualix J. Opposite effects of P2X7 and P2Y2 nucleotide receptors on α-secretase-dependent APP processing in Neuro-2a cells. FEBS Lett 2011, 585: 2255–2262.
Delarasse C, Auger R, Gonnord P, Fontaine B, Kanellopoulos JM. The purinergic receptor P2X7 triggers alpha-secretase-dependent processing of the amyloid precursor protein. J Biol Chem 2011, 286: 2596–2606.
Chen X, Hu J, Jiang L, Xu S, Zheng B, Wang C, et al. Brilliant Blue G improves cognition in an animal model of Alzheimer’s disease and inhibits amyloid-β-induced loss of filopodia and dendrite spines in hippocampal neurons. Neuroscience 2014, 279: 94–101.
Varma R, Chai Y, Troncoso J, Gu J, Xing H, Stojilkovic SS, et al. Amyloid-β induces a caspase-mediated cleavage of P2X4 to promote purinotoxicity. Neuromol Med 2009, 11: 63–75.
Godoy PA, Mennickent D, Cuchillo-Ibáñez I, Ramírez-Molina O, Silva-Grecchi T, Panes-Fernández J, et al. Increased P2X2 receptors induced by amyloid-β peptide participates in the neurotoxicity in Alzheimer’s disease. Biomed Pharmacother 2021, 142: 111968.
Carmo M, Gonçalves FQ, Canas PM, Oses JP, Fernandes FD, Duarte FV, et al. Enhanced ATP release and CD73-mediated adenosine formation sustain adenosine A2A receptor over-activation in a rat model of Parkinson’s disease. Br J Pharmacol 2019, 176: 3666–3680.
Ferrazoli EG, de Souza HDN, Nascimento IC, Oliveira-Giacomelli Á, Schwindt TT, Britto LR, et al. Brilliant blue G, but not fenofibrate, treatment reverts hemiparkinsonian behavior and restores dopamine levels in an animal model of Parkinson’s disease. Cell Transplant 2017, 26: 669–677.
Jiang T, Hoekstra J, Heng X, Kang W, Ding J, Liu J, et al. P2X7 receptor is critical in α-synuclein—mediated microglial NADPH oxidase activation. Neurobiol Aging 2015, 36: 2304–2318.
Kumar S, Mishra A, Krishnamurthy S. Purinergic antagonism prevents mitochondrial dysfunction and behavioral deficits associated with dopaminergic toxicity induced by 6-OHDA in rats. Neurochem Res 2017, 42: 3414–3430.
Oliveira-Giacomelli Á, Albino CM, de Souza HDN, Corrêa-Velloso J, de Jesus Santos AP, Baranova J, et al. P2Y6 and P2X7 receptor antagonism exerts neuroprotective/neuroregenerative effects in an animal model of Parkinson’s disease. Front Cell Neurosci 2019, 13: 476.
Ma J, Gao J, Niu M, Zhang X, Wang J, Xie A. P2X4R overexpression upregulates interleukin-6 and exacerbates 6-OHDA-induced dopaminergic degeneration in a rat model of PD. Front Aging Neurosci 2020, 12: 580068.
Zhang X, Wang J, Gao JZ, Zhang XN, Dou KX, Shi WD, et al. P2X4 receptor participates in autophagy regulation in Parkinson’s disease. Neural Regen Res 2021, 16: 2505–2511.
Gan M, Moussaud S, Jiang P, McLean PJ. Extracellular ATP induces intracellular alpha-synuclein accumulation via P2X1 receptor-mediated lysosomal dysfunction. Neurobiol Aging 2015, 36: 1209–1220.
Navarro G, Borroto-Escuela DO, Fuxe K, Franco R. Purinergic signaling in Parkinson’s disease. Relevance for treatment. Neuropharmacology 2016, 104: 161–168.
Díaz-Hernández M, Díez-Zaera M, Sánchez-Nogueiro J, Gómez-Villafuertes R, Canals JM, Alberch J, et al. Altered P2X7-receptor level and function in mouse models of Huntington’s disease and therapeutic efficacy of antagonist administration. FASEB J 2009, 23: 1893–1906.
Ollà I, Santos-Galindo M, Elorza A, Lucas JJ. P2X7 receptor upregulation in Huntington’s disease brains. Front Mol Neurosci 2020, 13: 567430.
Yiangou Y, Facer P, Durrenberger P, Chessell IP, Naylor A, Bountra C, et al. COX-2, CB2 and P2X7-immunoreactivities are increased in activated microglial cells/macrophages of multiple sclerosis and amyotrophic lateral sclerosis spinal cord. BMC Neurol 2006, 6: 12.
D’Ambrosi N, Finocchi P, Apolloni S, Cozzolino M, Ferri A, Padovano V, et al. The proinflammatory action of microglial P2 receptors is enhanced in SOD1 models for amyotrophic lateral sclerosis. J Immunol 2009, 183: 4648–4656.
Casanovas A, Hernández S, Tarabal O, Rosselló J, Esquerda JE. Strong P2X4 purinergic receptor-like immunoreactivity is selectively associated with degenerating neurons in transgenic rodent models of amyotrophic lateral sclerosis. J Comp Neurol 2008, 506: 75–92.
Andries M, van Damme P, Robberecht W, van den Bosch L. Ivermectin inhibits AMPA receptor-mediated excitotoxicity in cultured motor neurons and extends the life span of a transgenic mouse model of amyotrophic lateral sclerosis. Neurobiol Dis 2007, 25: 8–16.
Volonté C, Amadio S, Liguori F, Fabbrizio P. Duality of P2X7 receptor in amyotrophic lateral sclerosis. Front Pharmacol 2020, 11: 1148.
Apolloni S, Amadio S, Montilli C, Volonté C, D’Ambrosi N. Ablation of P2X7 receptor exacerbates gliosis and motoneuron death in the SOD1-G93A mouse model of amyotrophic lateral sclerosis. Hum Mol Genet 2013, 22: 4102–4116.
Fabbrizio P, Amadio S, Apolloni S, Volonté C. P2X7 receptor activation modulates autophagy in SOD1-G93A mouse microglia. Front Cell Neurosci 2017, 11: 249.
Vázquez-Villoldo N, Domercq M, Martín A, Llop J, Gómez-Vallejo V, Matute C. P2X4 receptors control the fate and survival of activated microglia. Glia 2014, 62: 171–184.
Amadio S, Parisi C, Piras E, Fabbrizio P, Apolloni S, Montilli C, et al. Modulation of P2X7 receptor during inflammation in multiple sclerosis. Front Immunol 2017, 8: 1529.
Gu BJ, Field J, Dutertre S, Ou A, Kilpatrick TJ, Lechner-Scott J, et al. A rare P2X7 variant Arg307Gln with absent pore formation function protects against neuroinflammation in multiple sclerosis. Hum Mol Genet 2015, 24: 5644–5654.
Sadovnick AD, Gu BJ, Traboulsee AL, Bernales CQ, Encarnacion M, Yee IM, et al. Purinergic receptors P2RX4 and P2RX7 in familial multiple sclerosis. Hum Mutat 2017, 38: 736–744.
Zabala A, Vazquez-Villoldo N, Rissiek B, Gejo J, Martin A, Palomino A, et al. P2X4 receptor controls microglia activation and favors remyelination in autoimmune encephalitis. EMBO Mol Med 2018, 10: e8743.
Lang PA, Merkler D, Funkner P, Shaabani N, Meryk A, Krings C, et al. Oxidized ATP inhibits T-cell-mediated autoimmunity. Eur J Immunol 2010, 40: 2401–2408.
Matute C, Torre I, Pérez-Cerdá F, Pérez-Samartín A, Alberdi E, Etxebarria E, et al. P2X(7) receptor blockade prevents ATP excitotoxicity in oligodendrocytes and ameliorates experimental autoimmune encephalomyelitis. J Neurosci 2007, 27: 9525–9533.
Sharp AJ, Polak PE, Simonini V, Lin SX, Richardson JC, Bongarzone ER, et al. P2x7 deficiency suppresses development of experimental autoimmune encephalomyelitis. J Neuroinflammation 2008, 5: 33.
Cheffer A, Castillo ARG, Corrêa-Velloso J, Gonçalves MCB, Naaldijk Y, Nascimento IC, et al. Purinergic system in psychiatric diseases. Mol Psychiatry 2018, 23: 94–106.
Krügel U. Purinergic receptors in psychiatric disorders. Neuropharmacology 2016, 104: 212–225.
Gubert C, Fries GR, Pfaffenseller B, Ferrari P, Coutinho-Silva R, Morrone FB, et al. Role of P2X7 receptor in an animal model of Mania induced by D-amphetamine. Mol Neurobiol 2016, 53: 611–620.
Mingam R, Smedt VD, Amédée T, Bluthé RM, Kelley KW, Dantzer R, et al. In vitro and in vivo evidence for a role of the P2X7 receptor in the release of IL-1β in the murine brain. Brain Behav Immun 2008, 22: 234–244.
Stokes L, Spencer SJ, Jenkins TA. Understanding the role of P2X7 in affective disorders-are glial cells the major players? Front Cell Neurosci 2015, 9: 258.
Cao X, Li LP, Wang Q, Wu Q, Hu HH, Zhang M, et al. Astrocyte-derived ATP modulates depressive-like behaviors. Nat Med 2013, 19: 773–777.
Basso AM, Bratcher NA, Harris RR, Jarvis MF, Decker MW, Rueter LE. Behavioral profile of P2X7 receptor knockout mice in animal models of depression and anxiety: Relevance for neuropsychiatric disorders. Behav Brain Res 2009, 198: 83–90.
Csölle C, Andó RD, Kittel Á, Gölöncsér F, Baranyi M, Soproni K, et al. The absence of P2X7 receptors (P2rx7) on non-haematopoietic cells leads to selective alteration in mood-related behaviour with dysregulated gene expression and stress reactivity in mice. Int J Neuropsychopharmacol 2013, 16: 213–233.
Csölle C, Baranyi M, Zsilla G, Kittel A, Gölöncsér F, Illes P, et al. Neurochemical changes in the mouse Hippocampus underlying the antidepressant effect of genetic deletion of P2X7 receptors. PLoS One 2013, 8: e66547.
Hempel C, Nörenberg W, Sobottka H, Urban N, Nicke A, Fischer W, et al. The phenothiazine-class antipsychotic drugs prochlorperazine and trifluoperazine are potent allosteric modulators of the human P2X7 receptor. Neuropharmacology 2013, 75: 365–379.
Söderlund J, Schröder J, Nordin C, Samuelsson M, Walther-Jallow L, Karlsson H, et al. Activation of brain interleukin-1β in schizophrenia. Mol Psychiatry 2009, 14: 1069–1071.
Zhang PA, Sun Q, Li YC, Weng RX, Wu R, Zhang HH, et al. Overexpression of purinergic P2X4 receptors in Hippocampus rescues memory impairment in rats with type 2 diabetes. Neurosci Bull 2020, 36: 719–732.
Wyatt LR, Godar SC, Khoja S, Jakowec MW, Alkana RL, Bortolato M, et al. Sociocommunicative and sensorimotor impairments in male P2X4-deficient mice. Neuropsychopharmacology 2013, 38: 1993–2002.
Naviaux RK, Zolkipli Z, Wang L, Nakayama T, Naviaux JC, Le TP, et al. Antipurinergic therapy corrects the autism-like features in the poly(IC) mouse model. PLoS One 2013, 8: e57380.
Cheung KK, Chan WY, Burnstock G. Expression of P2X purinoceptors during rat brain development and their inhibitory role on motor axon outgrowth in neural tube explant cultures. Neuroscience 2005, 133: 937–945.
Huang L, Otrokocsi L, Sperlágh B. Role of P2 receptors in normal brain development and in neurodevelopmental psychiatric disorders. Brain Res Bull 2019, 151: 55–64.
Song XL, Liu DS, Qiang M, Li Q, Liu MG, Li WG, et al. Postsynaptic targeting and mobility of membrane surface-localized hASIC1a. Neurosci Bull 2021, 37: 145–165.
Acknowledgments
This review was supported by the National Research Foundation of Ukraine (https://nrfu.org.ua/en/, 2020.02/0263) and Die Deutsche Forschungsgemeinschaft (https://www.dfg.de/, 441694049).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Cherninskyi, A., Storozhuk, M., Maximyuk, O. et al. Triggering of Major Brain Disorders by Protons and ATP: The Role of ASICs and P2X Receptors. Neurosci. Bull. 39, 845–862 (2023). https://doi.org/10.1007/s12264-022-00986-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12264-022-00986-8