Abstract
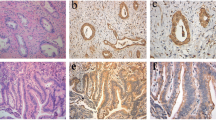
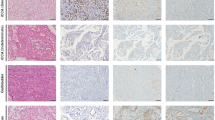
Multidrug resistance-associated protein 2 (MRP2) is a multi-specific organic anion transporter predominantly expressed in the canalicular membrane of hepatocytes, epithelial cells from gallbladder and apical membranes of proximal tubular kidney epithelium whereas multidrug resistance-associated protein 3 (MRP3) is present in the basolateral membrane of hepatocytes and cholangiocytes. This study aims to detect the expression of these transporters in hepatocellular carcinoma (HCC) and in cholangiocarcinoma (CC), searching for evidences for future studies on differential diagnosis and on clinical essays. The immunohistochemical reactivity (IHC) of these transporters was assessed in tissue microarrays of 80 HCC and 56 CC cases using monoclonal antibodies and compared with anatomopathological (AP) variables. The positivity of MRP2 was observed in 92.3% of HCC and in 96.3% of CC. The detection of high MRP2 expression in HCC was not significantly different (p > 0.05) according to the size, number of nodules architectural pattern and growth pattern of HCC and CC. Regarding histological grades, 22/22 well moderately differentiated HCC versus 50/56 poorly differentiated HCC were positive for MRP2. A trend for lower expression in poor differentiation HCC was found. And 50/50 well/moderately differentiated CC versus 2/4 poorly/undifferentiated CC were positive for MRP2. This result showed a reduced expression (p = 0,0004) in poorly differentiated CC. MRP3 positivity was observed in 18.8% of HCC and was not significantly different according to AP parameters. MRP3 was expressed in 44.5% CC, with a trend for lower expression in less differentiated CC and significantly lower rates in the ductular histological subtype (p = 0.023). The high expression of MRP2 in HCC and in CC is conserved regardless most of the anatomopathological parameters, except for a trend of lower expression in less differentiated HCC and CC. The observation of lower MRP3 expression in less differentiated CC and, especially, in the histological subtype with expression of hepatic progenitor cell phenotypes leads to future opportunities to evaluate the expression of this marker in cholangiocarcinomas.


Similar content being viewed by others
References
Vasiliou V, Vasiliou K, Nebert DW (2009) Human ATP-binding cassette (ABC) transporter family. Hum Genomics 3:281–290. https://doi.org/10.1186/1479-7364-3-3-281
Stefková J, Poledne R, Hubácek JA (2004) ATP-binding cassette (ABC) transporters in human metabolism and diseases. Physiol Res 53(3):235–243
Tarling EJ, de Aguiar Vallim TQ, Edwards PA (2013) Role of ABC transporters in lipid transport and human disease. Trends Endocrinol Metab 24(7):342–350. https://doi.org/10.1016/j.tem.2013.01.006
Lagana SM, Salomao M, Remotti HE, Knisely AS, Moreira RK (2015) Bile salt export pump: a sensitive and specific immunohistochemical marker of hepatocellular carcinoma. Histopathology 66(4):598–602. https://doi.org/10.1111/his.12601
Nguyen T, Phillips D, Jain D, Torbenson M, Wu T-T, Yeh MM et al (2015) Comparison of 5 immunohistochemical markers of hepatocellular differentiation for the diagnosis of hepatocellular carcinoma. Arch Pathol Lab Med 139(8):1028–1034. https://doi.org/10.5858/arpa.2014-0479-OA
Fujikura K, Yamasaki T, Otani K, Kanzawa M, Fukumoto T, Ku Y et al (2016) BSEP and MDR3 – useful immunohistochemical markers to discriminate hepatocellular carcinomas from intrahepatic cholangiocarcinomas and hepatoid carcinomas. Am J Surg Pathol 40(5):689–696. https://doi.org/10.1097/PAS.0000000000000585
Trauner M, Boyer JL (2003) Bile salt transporters: molecular characterization, function, and regulation. Physiol Rev 83(2):633–671. https://doi.org/10.1152/physrev.00027.2002
ABCC2: ATP-binding cassette, sub-family C (CFTR/MRP), member 2. [Internet]. The Human Protein Atlas. 2017. http://www.proteinatlas.org/ENSG00000023839-ABCC2/tissue. Accessed 31 Jan 2017
Taniguchi K, Wada M, Kohno K, Nakamura T, Kawabe T, Kawakami M et al (1996) A human canalicular multispecific organic anion transporter (cMOAT) gene is overexpressed in cisplatin-resistant human cancer cell lines with decreased drug accumulation. Cancer Res 56(18):4124–4129
Chen Z, Shi T, Zhang L, Zhu P, Deng M, Huang C et al (2016) Mammalian drug efflux transporters of the ATP binding cassette (ABC) family in multidrug resistance: a review of the past decade. Cancer Lett 370(1):153–164. https://doi.org/10.1016/j.canlet.2015.10.010
Nies AT, Konig J, Cui Y, Brom M, Spring H, Keppler D (2002) Structural requirements for the apical sorting of human multidrug resistance protein 2 (ABCC2). Eur J Biochem 269(7):1866–1876. https://doi.org/10.1007/s00424-006-0109-y
Jedlitschky G, Hoffmann U, Kroemer HK (2006) Structure and function of the MRP2 (ABCC2) protein and its role in drug disposition. Expert Opin Drug Metab Toxicol 2(3):351–366
Alrefai WA, Gill RK (2007) Bile acid transporters: structure, function, regulation and pathophysiological implications. Pharm Res 10:1803–1823. https://doi.org/10.1517/17425255.2.3.351
Erlinger S, Arias IM, Dhumeaux D (2014) Inherited disorders of bilirubin transport and conjugation: new insights into molecular mechanisms and consequences. Gastroenterology 146(7):1625–1638. https://doi.org/10.1053/j.gastro.2014.03.047
Keppler D (2014) The roles of MRP2, MRP3, OATP1B1, and OATP1B3 in conjugated hyperbilirubinemia. Drug Metab Dispos 42(4):561–565. https://doi.org/10.1124/dmd.113.055772
Kool M, van der Linden M, de Haas M, Scheffer GL, de Vree JM, Smith AJ et al (1999) MRP3, an organic anion transporter able to transport anti-cancer drugs. Proc Natl Acad Sci U S A 96(12):6914–6919. https://doi.org/10.1073/pnas.96.12.6914
Scheffer GL, Kool M, Heijn M, de Haas M, Pijnenborg AC, Wijnholds J et al (2000) Specific detection of multidrug resistance proteins MRP1, MRP2, MRP3, MRP5, and MDR3 P-glycoprotein with a panel of monoclonal antibodies. Cancer Res 60(18):5269–5277
Klaassen CD, Aleksunes LM (2010) Xenobiotic, bile acid, and cholesterol transporters: function and regulation. Pharmacol Rev 62(1):1–96. https://doi.org/10.1124/pr.109.002014
ABCC3: ATP-binding cassette, sub-family C (CFTR/MRP), member 3 [Internet]. The Human Protein Atlas. 2017. http://www.proteinatlas.org/ENSG00000108846-ABCC3/tissue. Accessed 31 Jan 2017
ABCC3: ATP-binding cassette, sub-family C (CFTR/MRP), member 3 [Internet]. GenAtlas - Universite Paris Descartes. 2017. http://genatlas.medecine.univ-paris5.fr/fiche.php?symbol=ABCC3. Accessed 31 Jan 2017
König J, Rost D, Cui Y, Keppler D (1999) Characterization of the human multidrug resistance protein isoform MRP3 localized to the basolateral hepatocyte membrane. Hepatology 29(4):1156–1163. https://doi.org/10.1002/hep.510290404
Ballatori N, Hammond CL, Cunningham JB, Krance SM, Marchan R (2005) Molecular mechanisms of reduced glutathione transport: role of the MRP/CFTR/ABCC and OATP/SLC21A families of membrane proteins. Toxicol Appl Pharmacol 204(3):238–255. https://doi.org/10.1016/j.taap.2004.09.008
Belinsky MG, Dawson PA, Shchaveleva I, Bain LJ, Wang R, Ling V et al (2005) Analysis of the in vivo functions of Mrp3. Mol Pharmacol 68(1):160–168. https://doi.org/10.1124/mol.104.010587
Halilbasic E, Claudel T, Trauner M (2013) Bile acid transporters and regulatory nuclear receptors in the liver and beyond. J Hepatol 58(1):155–168. https://doi.org/10.1016/j.jhep.2012.08.002
Sodani K, Patel A, Kathawala RJ, Chen Z-S (2012) Multidrug resistance associated proteins in multidrug resistance. Chin J Cancer 31(2):58–72. https://doi.org/10.5732/cjc.011.10329
Rau S, Autschbach F, Riedel HD, Konig J, Kulaksiz H, Stiehl A et al (2008) Expression of the multidrug resistance proteins MRP2 and MRP3 in human cholangiocellular carcinomas. Eur J Clin Investig 38(2):134–142. https://doi.org/10.1111/j.1365-2362.2007.01916.x
Tomonari T, Takeishi S, Taniguchi T, Tanaka T, Tanaka H, Fujimoto S et al (2016) MRP3 as a novel resistance factor for sorafenib in hepatocellular carcinoma. Oncotarget 7(6):7207–7215. https://doi.org/10.18632/oncotarget.6889
Zollner G, Wagner M, Fickert P, Silbert D, Fuchsbichler A, Zatloukal K et al (2005) Hepatobiliary transporter expression in human hepatocellular carcinoma. Liver Int (2):367–379. https://doi.org/10.1111/j.1478-3231.2005.01033.x
Nies AT, König J, Pfannschmidt M, Klar E, Hofmann WJ, Keppler D (2001) Expression of the multidrug resistance proteins MRP2 and MRP3 in human hepatocellular carcinoma. Int J Cancer 94(4):492–499. https://doi.org/10.1111/j.1478-3231.2005.01033.x
Borght VS, Libbrecht L, Blokzijl H, Faber NK, Moshage H, Aerts R et al (2005) Diagnostic and pathogenetic implications of the expression of hepatic transporters in focal lesions occurring in normal liver. J Pathol 207(4):471–482. https://doi.org/10.1002/path.1852
Apte U, Krisnamurthy P (2010) Molecular pathology of liver diseases. In: Monga SPS (ed) Molecular pathology of liver diseases 1st edn. Springer, Boston, pp 147–164
Korita PV, Wakai T, Shirai Y, Matsuda Y, Sakata J, Takamura M et al (2010) Multidrug resistance-associated protein 2 determines the efficacy of cisplatin in patients with hepatocellular carcinoma. Oncol Rep 4:965–972. https://doi.org/10.3892/ijmm.2012.1173
Atilano-Roque A, Roda G, Fogueri U, Kiser JJ, Joy MS (2016) Effect of disease pathologies on transporter expression and function. J Clin Pharmacol 56(Suppl7):S205–S221. https://doi.org/10.1002/jcph.768
Buettner S, van Vugt JLA, IJzermans J, Groot Koerkamp B (2017) Intrahepatic cholangiocarcinoma: current perspectives. Onco Targets Ther 10:1131–1142. https://doi.org/10.2147/OTT.S93629
Nakanuma Y, Kakuda Y (2015) Pathologic classification of cholangiocarcinoma: new concepts. Best Pract Res Clin Gastroenterol 29(2):277–293. https://doi.org/10.1016/j.bpg.2015.02.006
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest with respect to this article.
Rights and permissions
About this article
Cite this article
Cirqueira, C.S., Felipe-Silva, A.S., Wakamatsu, A. et al. Immunohistochemical Assessment of the Expression of Biliary Transportation Proteins MRP2 and MRP3 in Hepatocellular Carcinoma and in Cholangiocarcinoma. Pathol. Oncol. Res. 25, 1363–1371 (2019). https://doi.org/10.1007/s12253-018-0386-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12253-018-0386-8