Abstract
Purpose
Solid dispersions (SDs) of a poorly water-soluble drug were prepared, and their physicochemical properties were compared to those of control physical mixtures (PMs). Among the multiple techniques used to characterize the solid state of preparations, confocal micro Raman spectroscopy (CMRS) was used as a non-destructive tool to qualitatively probe content uniformity and distribution of drug and carrier.
Methods
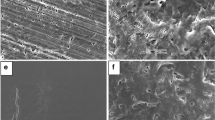
SDs and PMs of drug (fenbendazole, FBZ) were prepared containing two different carriers (poloxamer P188 or P407) with different drug polymer ratios. The preparations were characterized by powder X-ray diffractometry, Fourier transform infrared spectroscopy, thermal analysis, scanning electron microscopy, and in vitro dissolution assay. In addition, CMRS technique and principal component analysis (PCA) were used in order to statistically define the content uniformity and distribution of the drug within the polymeric matrix.
Results
In vitro dissolution results exhibited a marked improvement when the drug was formulated as SD compared to control PM and to pure drug. The solid state of these preparations characterized by X-ray powder diffraction and Fourier transform infrared spectroscopy showed no changes in the crystalline state of the drug and no chemical interactions between the components. Raman studies showed a better content uniformity of the drug within the polymeric matrix when subjected to SD process, correlating with the improved dissolution profile.
Conclusion
This study provides evidence of the potential of the confocal Raman imaging technique, providing a fast and powerful method to characterize solid dispersions which could be incorporated towards the use of quality by design (QbD) approaches in pharmaceutical development.









Similar content being viewed by others
References
Loftsson T, Brewster ME. Pharmaceutical applications of cyclodextrins: basic science and product development. J Pharm Pharmacol. 2010;62(11):1607–21. https://doi.org/10.1111/j.2042-7158.2010.01030.x.
Leuner C, Dressman J. Improving drug solubility for oral delivery using solid dispersions. Eur J Pharm Biopharm. 2000;50(1):47–60. https://doi.org/10.1016/S0939-6411(00)00076-X.
Vasconcelos T, Sarmento B, Costa P. Solid dispersions as strategy to improve oral bioavailability of poor water soluble drugs. Drug Discov Today. 2007;12(23):1068–75. https://doi.org/10.1016/j.drudis.2007.09.005.
Brough C, Williams RO. Amorphous solid dispersions and nano-crystal technologies for poorly water-soluble drug delivery. Int J Pharm. 2013;453(1):157–66. https://doi.org/10.1016/j.ijpharm.2013.05.061.
Vo CL-N, Park C, Lee B-J. Current trends and future perspectives of solid dispersions containing poorly water-soluble drugs. Eur J Pharm Biopharm. 2013;85(3):799–813. https://doi.org/10.1016/j.ejpb.2013.09.007.
Mehanna MM, Motawaa AM, Samaha MW. In sight into tadalafil–block copolymer binary solid dispersion: mechanistic investigation of dissolution enhancement. Int J Pharm. 2010;402(1):78–88. https://doi.org/10.1016/j.ijpharm.2010.09.024.
Bhandari KH, Newa M, Kim JA, Yoo BK, Woo JS, Lyoo WS, et al. Preparation, characterization and evaluation of coenzyme Q10 binary solid dispersions for enhanced solubility and dissolution. Biol Pharm Bull. 2007;30(6):1171–6. https://doi.org/10.1248/bpb.30.1171.
U.S. Food and Drug Administration, Center for Drugs Evaluation Research (CDER), Center for Veterinary Medicine (CVM) and Office of Regulatory Affairs (ORA). Guidance for Industry: PAT - A Framework for Innovative Pharmaceutical Development. 2004.https://www.fda.gov/downloads/Drugs/GuidanceComplianceRegulatoryInformation/Guidances/UCM070305.pdf. Accessed 11 Dec 2017.
Vasanthavada M, Tong W-Q, Serajuddin A. Development of solid dispersions for poorly water-soluble drugs. In: Liu R, editor. Water insoluble-drug formulation. 2nd ed. Boca Raton: CRC Press; 2008. p. 499–529.
Karavas E, Georgarakis M, Docoslis A, Bikiaris D. Combining SEM, TEM, and micro-Raman techniques to differentiate between the amorphous molecular level dispersions and nanodispersions of a poorly water-soluble drug within a polymer matrix. Int J Pharm. 2007;340(1):76–83. https://doi.org/10.1016/j.ijpharm.2007.03.037.
Furuyama N, Hasegawa S, Hamaura T, Yada S, Nakagami H, Yonemochi E, et al. Evaluation of solid dispersions on a molecular level by the Raman mapping technique. Int J Pharm. 2008;361(1):12–8. https://doi.org/10.1016/j.ijpharm.2008.05.009.
Punčochová K, Vukosavljevic B, Hanuš J, Beránek J, Windbergs M, Štěpánek F. Non-invasive insight into the release mechanisms of a poorly soluble drug from amorphous solid dispersions by confocal Raman microscopy. Eur J Pharm Biopharm. 2016;101:119–25. https://doi.org/10.1016/j.ejpb.2016.02.001.
Schoenherr C, Haefele T, Paulus K, Francese G. Confocal Raman microscopy to probe content uniformity of a lipid based powder for inhalation: a quality by design approach. Eur J Pharm Sci. 2009;38(1):47–54. https://doi.org/10.1016/j.ejps.2009.05.011.
Haefele T, Paulus K. Confocal raman microscopy in pharmaceutical development. In: Dieing T, Hollricher O, Toporski J, editors. Confocal raman microscopy. Springer series in optical sciences. Heidelberg: Springer; 2010. p. 165–202.
Choi DS, Zhang Y-E, Tian H, Shah N, Chokshi HP. Evaluation on the drug–polymer mixing status in amorphous solid dispersions at the early stage formulation and process development. J Pharm Innov. 2013;8(3):163–74.
Campbell WC. Benzimidazoles: veterinary uses. Parasitol Today. 1990;6(4):130–3. https://doi.org/10.1016/0169-4758(90)90231-R.
Saunders GI, Wasmuth JD, Beech R, Laing R, Hunt M, Naghra H, et al. Characterization and comparative analysis of the complete Haemonchus contortus β-tubulin gene family and implications for benzimidazole resistance in strongylid nematodes. Int J Parasitol. 2013;43(6):465–75. https://doi.org/10.1016/j.ijpara.2012.12.011.
Longo M, Zanoncelli S, Messina M, Scandale I, Mackenzie C, Geary T, et al. In vivo preliminary investigations of the effects of the benzimidazole anthelmintic drug flubendazole on rat embryos and fetuses. Reprod Toxicol. 2014;49:33–42. https://doi.org/10.1016/j.reprotox.2014.06.009.
Munguía B, Michelena M, Melian E, Saldaña J, Ures X, Manta E, et al. Development of novel valerolactam-benzimidazole hybrids anthelmintic derivatives: diffusion and biotransformation studies in helminth parasites. Exp Parasitol. 2015;153:75–80. https://doi.org/10.1016/j.exppara.2015.03.013.
Munguía B, Mendina P, Espinosa R, Lanz A, Saldaña J, Andina MJ, et al. Synthesis and anthelmintic evaluation of novel valerolactam-benzimidazole hybrids. Lett Drug Des Discovery. 2013;10(10):1007–14. https://doi.org/10.2174/15701808113109990028.
Hennessy DR. Modifying the formulation or delivery mechanism to increase the activity of anthelmintic compounds. Vet Parasitol. 1997;72(3):367–90. https://doi.org/10.1016/S0304-4017(97)00106-4.
Vilhelmsen T, Eliasen H, Schæfer T. Effect of a melt agglomeration process on agglomerates containing solid dispersions. Int J Pharm. 2005;303(1):132–42. https://doi.org/10.1016/j.ijpharm.2005.07.012.
Zhai H, Li S, Andrews G, Jones D, Bell S, Walker G. Nucleation and growth in fluidised hot melt granulation. Powder Technol. 2009;189(2):230–7. https://doi.org/10.1016/j.powtec.2008.04.021.
Kibbe AH, American Pharmaceutical A. Handbook of pharmaceutical excipients. Washington, D.C.: American Pharmaceutical Association; 2000.
Xie F, Ji S, Cheng Z. In vitro dissolution similarity factor (f2) and in vivo bioequivalence criteria, how and when do they match? Using a BCS class II drug as a simulation example. Eur J Pharm Sci. 2015;66:163–72. https://doi.org/10.1016/j.ejps.2014.10.002.
Pharmacopeia U. USP 29–NF 24. Rockville: USP; 2005.
Castro SG, Bruni SS, Lanusse CE, Allemandi DA, Palma SD. Improved albendazole dissolution rate in Pluronic 188 solid dispersions. AAPS PharmSciTech. 2010;11(4):1518–25. https://doi.org/10.1208/s12249-010-9517-6.
Horvat AJ, Babić S, Pavlović D, Ašperger D, Pelko S, Kaštelan-Macan M, et al. Analysis, occurrence and fate of anthelmintics and their transformation products in the environment. TrAC Trends Anal Chem. 2012;31:61–84. https://doi.org/10.1016/j.trac.2011.06.023.
Craig DQM. The mechanisms of drug release from solid dispersions in water-soluble polymers. Int J Pharm. 2002;231(2):131–44. https://doi.org/10.1016/S0378-5173(01)00891-2.
Eaton JW, Bateman D, Hauberg S, Wehbring R. A high-level interactive language for numerical computations. In GNU Octave version 4.2.1. Free Software Foundation. 2017. https://www.gnu.org/software/octave/octave.pdf. Accessed 11 Dec 2017.
Acknowledgments
The authors especially thank Dario O. Weitmann, Business Coordinator BCS in BASF Argentina S.A for the Poloxamer samples, Q.F. Antonio Malanga (BIOTEFA—Instituto Polo Tecnológico de Pando, Facultad de Química, UdelaR, Uruguay) for kindly providing access to the necessary equipment, and Lourdes Martino, who edited this paper. The authors acknowledge Prof. Dr. Alejandro Ayala (Universidade Federal do Ceará, UFC, Brazil) for providing DSC and TG measurement, and Fernando Pignanelli (Facultad de Química, UdelaR, Uruguay) for the help in the implementation of PCA and the peak-to-peak computational scripts for the data analysis.
Funding
This work was supported by grants from the Programa de Desarrollo de Ciencias Básicas (PEDECIBA, Uruguay), ANII (Agencia Nacional de Investigación e Innovación, Uruguay), Project ANII-EQC-X-2012-1-14 IPTP, AUGM (Asociación de Universidades del Grupo Montevideo), SECyT-UNC, CONICET, ANPCyT (Argentina).
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Melian, M.E., Munguía, A.B., Faccio, R. et al. The Impact of Solid Dispersion on Formulation, Using Confocal Micro Raman Spectroscopy as Tool to Probe Distribution of Components. J Pharm Innov 13, 58–68 (2018). https://doi.org/10.1007/s12247-017-9306-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12247-017-9306-9