Abstract
Prostate-specific membrane antigen (PSMA) is a transmembrane glycoprotein highly expressed by prostate cancer cells. PSMA-based radioligand therapy (RLT) emerged as a promising therapeutic option for prostate cancer in the early 2000s, and has been clinically validated with great enthusiasm during these past two decades. Last year, the European Association of Nuclear Medicine (EANM) published the procedure guidelines for the safe clinical practice of Lutetium-177 (177Lu)-labelled PSMA RLT. In addition, PSMA RLT with alpha-ray-emitting radioisotopes has been also developed recently. Following the clinical use of 177Lu-PSMA RLT, PSMA-targeted positron-emission tomography (PET) with Gallium-68 (68Ga) has been performed inevitably for “theranostics” for the last decade; prostate cancer is going to be treated with PSMA-RLT based on the diagnosis by PSMA-PET. Furthermore, the diagnostic usefulness of 68Ga-PSMA PET has been documented in various diseases beyond prostate cancer more recently. Regrettably, Japan is behind European countries and the United States in this field, and has just made a belated start of their clinical trials. In this review article, we briefly overviewed the current status of PSMA RLT and PSMA PET. We hope that this topic will be a particular focus of attention for most ANM readers in Japan, and that our efforts will help to facilitate the early approval of PSMA RLT and PSMA PET by the Japanese government even if only slightly.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Prostate-specific membrane antigen (PSMA) is a transmembrane glycoprotein highly expressed by prostate cancer cells. PSMA-based radioligand therapy (RLT) emerged as a promising therapeutic option for prostate cancer in the early 2000s [1], and has been clinically validated with great enthusiasm during these past these two decades. Last year, the European Association of Nuclear Medicine (EANM) published the procedure guidelines for the safe clinical practice of Lutetium-177 (177Lu)-labelled PSMA RLT [2]. In addition, PSMA RLT with alpha-ray-emitting radioisotopes has also been developed recently.
Following the clinical use of 177Lu-PSMA RLT, PSMA-targeted positron-emission tomography (PET) with Gallium-68 (68 Ga) has been performed inevitably for “theranostics” for the last decade [3]; prostate cancer is going to be treated with PSMA RLT based on the diagnosis by PSMA PET. Dr. Jadvar, one of pioneers in the field of PSMA RLT, once said: “Theranostics is currently experiencing a renaissance since the early days of radioiodine use in thyroid diseases” [4]. Furthermore, the diagnostic usefulness of 68Ga-PSMA PET has been clarified in various diseases beyond prostate cancer more recently.
Regrettably, Japan is behind European countries and the United States in this field, and has just made a belated start of their clinical trials. In this review article, we briefly overview the current status of PSMA RLT and PSMA PET.
Safety of 177Lu-PSMA radioligand therapy: EANM Procedure Guidelines and literature review
Last year, the EANM published procedure guidelines for 177Lu-PSMA RLT to assist nuclear medicine specialists in delivering PSMA-RLT as an “unproven intervention in clinical practice”, in accordance with the best currently available knowledge [2]. Presented in these safety guidelines are the results of recent phase II trials in which the most common toxic effects possibly related to 177Lu-PSMA-617 were grade 3 lymphocytopenia in 37% of patients, grade 3 anemia in 13%, and grade 3 or 4 thrombocytopenia in 13%. In addition, grade 1 dry mouth was reported in 87% of patients, grade 1 or 2 transient nausea in 50%, and grade 1 or 2 fatigue in 50%. The authors considered that these data indicated a favorable safety profile for 177Lu-PSMA RLT [2].
Banerjee et al. synthesized 14 new PSMA-targeted, 177Lu-labeled radioligands (177Lu-L1–177Lu-L14) [5] and investigated their pharmacokinetics, capacity to kill cells in vitro, and tumor control in vivo. In addition, they evaluated the cell uptake, internalization, biodistribution, efficacy, toxicity, tumor regression, and survival rate of these radioligands in mice. They optimized aspects of the radiosynthesis and assessed the short- and long-term toxicity of 177Lu-L1. Their self-blocking study showed that 177Lu-L1, which already demonstrates relatively low renal uptake as a type-II agent, caused no significant change in tumor uptake but yielded a ten-fold kidney blockade. They concluded that the scaffold on which 177Lu-L1 is based may also provide guidance for the corresponding alpha-ray emitters, which although potentially more efficacious, have the disadvantage of more severe adverse reactions [5]. This paper presents various important topics for discussion.
In their study of 16 prostate cancer patients undergoing initial 177Lu-PSMA RLT, Schumann et al. examined DNA damage in blood samples taken before and at seven time points (between 1 and 96 h) after radionuclide administration [6]. This study was the first to report the induction and persistence of double-strand break (DSB) DNA damage combined with internal dosimetry after therapy with 177Lu-PSMA. The minimal, maximal, and average total absorbed doses to the blood were 76, 164, and 109 ± 28 mGy, respectively. The average number of radiation-induced foci (RIF) per cell increased within the first 4 h after administration, followed by a decrease indicating DNA repair. The number of RIF during the first 2.6 h correlated linearly with the absorbed dose to the blood, which was in good agreement with previously published in-vitro data [7]. DNA DSBs were repaired effectively in many patients; however, RIF did not disappear completely in some patients, even 96 h after administration. Parameters of kidney function did not correlate with the absorbed dose rate or with the average number of RIF. The authors recognized the necessity to conduct further clinical research in a larger number of patients.
There are few data regarding the feasibility of rechallenge 177Lu-PSMA-617 RLT. Yordanova et al. performed a retrospective review of survival, response, and adverse events in patients who underwent rechallenge PSMA RLT [8], and found no cases of life-threatening (i.e., Common Toxicity Criteria [CTC] grade 4) adverse events after retreatment. However, 23% of patients experienced serious impairment of bone marrow function, one patient developed serious renal impairment, and 70% of patients developed irreversible adverse events (of which 90% were low-grade and 10% were grade 3 toxicity). The difference in overall survival between patients who underwent rechallenge PSMA-RLT compared with those who received only baseline PSMA RLT was significant: 25 vs. 9 months, respectively. The authors concluded that retreatment with PSMA-RLT appears to be safe and effective, resulting in benefits for most patients who had previously responded to PSMA-RLT [8]. The findings of this paper are important when considering the indications for PSMA-RLT.
PSMA-targeted radioligand therapy with new beta-ray and alpha-ray emitting radioisotopes other than 177Lu-PSMA monotherapy
In Europe single-agent 177Lu-PSMA RLT has been studied in clinical trials, but there is also great interest in alpha-ray-emitting radioisotopes with significant therapeutic effects and easy outpatient treatment management, as well as beta-ray-emitting radioisotopes and with Auger electrons emitting radioisotopes with a short range [9]. PSMA RLT labeled with alpha-ray-emitting radioisotopes is being used clinically in some countries, and has been reported increasingly. In Japan, where government regulations are strict and obtaining some therapeutic radioisotopes produced by the nuclear reactor is difficult, the introduction of alpha-ray-emitting radioisotopes other than Radium-223 (223Ra) is still insufficient. Thus, there are no reports of the use of PSMA RLT with alpha-ray-emitting radioisotopes thus far. Although delayed in some countries, manufacturing alpha-ray-emitting radioisotopes by cyclotrons is possible, with several results emerging despite its being still in the research stage [10, 11].
The most advanced clinical PSMA RLT study of alpha-ray-emitting radioisotopes involves Actinium-225 (225Ac)-PSMA-617, although in a report of 17 patients with advanced prostate cancer treated with chemotherapy, more than 91% showed a decrease in PSA levels of more than 50%, with 41% saying that it had dropped below the measurement limit. Even in patients who discontinued it during the treatment course due to bone marrow suppression and renal dysfunction, relief of bone metastasis pain was observed [12, 13]. It should be noted that a rare case of prostate cancer brain metastasis with 225Ac-PSMA-617 has been reported, and in small multiple brain metastasis cases, this treatment may be a useful option to consider [14].
177Lu-PSMA RLT is known to have only around a 30% effect, whereas PSMA RLT with alpha-ray-emitting radioisotopes has produced surprising results. Treatment with 225Ac-PRLT has been reported to result in dry mouth [9]. In an attempt to reduce this side effect, a study combined tandem PSMA RLT with low-dose administration of 225Ac-PSMA after 177Lu-PSMA, with improved therapeutic effects and reduction in side effects observed in 20 cases [15].
A study calculated the absorption dose based on the distribution of Bismuth-213 (213Bi)-PSMA RLT on 68Ga-PSMA PET, which is expected to be another alpha-ray-emitting radioisotope. Unfortunately, although it had greater off-target perfusion radioactivity than 225Ac-PSMA RLT, its therapeutic window was shown to be narrower than that of 225Ac-PSMA RLT [16]. After theoretical dose calculation, 213Bi seems to be the choice after 225Ac according to their report. Given its physical half-life, 8 h to 10 days is considered desirable in practical clinical practice, while for 225Ac and Lead-212 (212Pb), 9.9 days and 10.6 h, respectively, are promising [17]. According to the study, the dynamics of 212Pb-PSMA can be confirmed based on 203Pb-PSMA, although slightly inferior to the computational 225Ac-PSMA RLT, 212Pb has the possibility of being available using the 224Ra generator.
Among the therapeutic beta-ray-emitting radioisotopes, 177Lu is at the core of PSMA RLT. However, it has been reported that Terbium-161 (161Tb) has better characteristics than 177Lu from theoretical dose calculation (T1/2 = 6.89 days; Eβav = 154 keV) [18]. According to the report, because of the effect of Auger electrons in addition to beta rays in 161Tb-PSMA-617, it is possible to deliver higher absorption doses to tumor cells than if 177Lu was used. Further, low-energy gamma rays suitable for SPECT (Eγ = 49 keV, I = 17.0%; Eγ = 75 keV, I = 10.2%) are also emitted. Therefore, imaging and dosimetry are also possible at the same time. In general, targeted radioligand therapy is effective for the treatment of small metastatic cells. Since the effect of 161 Tb is high and its range of radiation is short, it seems to be preferable as can be seen from the current situation where it is being replaced by 177Lu rather than Iodine-131 (131I) or yttrium-90 (90Y).
Diagnostic performance of 68 Ga-PSMA PET
68Ga-PSMA is one of the promising PET tracers for detecting prostate cancer in various clinical scenarios. Recently, there are many articles published in patients with very low PSA to predict the diagnostic ability of 68Ga-PSMA PET. Farolfi et al. reported the diagnostic performance of 68Ga-PSMA PET/CT in 119 prostate cancer patients with biochemical recurrence retrospectively, whose PSA levels are the range 0.2–0.5 ng/ml at the time of PET. 68Ga-PSMA PET/CT was positive in 34.4%, and clinical physicians changed their treatment strategy in 30.2% [19]. Ceci et al. demonstrated the diagnostic usefulness of 68Ga-PSMA PET/CT prospectively in 332 patients with biological recurrence (PSA 0.2–2.0) [20]. The detection rate in this study was 53.6% and was different depending on the clinical stage of biological recurrence. These results reveal that 68Ga-PSMA PET/CT can detect very early recurrence in at least 30% of patients.
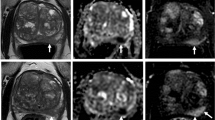
Magnetic resonance imaging (MRI) is one of the common imaging modalities to diagnose prostate cancer, and recently several studies compared the diagnostic performance of multi-parametric MRI (mpMRI) with 68 Ga-PSMA PET/CT. A retrospective study showed 43 patients with recurrent prostate cancer who underwent MRI with 68 Ga-PSMA PET/CT within 2 months. 68 Ga-PSMA PET/CT detected more pelvic lesions characteristic for recurrent prostate cancer (75 lesions) when compared to MRI (53 lesions) [21]. Another retrospective study revealed 58 patients who underwent MRI with 68 Ga-PSMA PET/CT followed by radical prostatectomy. 68 Ga-PSMA PET/CT correctly detected more foci (78%, AUC 0.817) than mpMRI (69%, AUC 0.729) [22]. 68 Ga-PSMA PET/CT may better reflect the histopathology of radical prostatectomy compared to mpMRI when considering multifocal and bilateral disease. The notable points of these articles are not only the high diagnostic performance of 68 Ga-PSMA PET/CT but also possibly include 68 Ga-PSMA PET/CT for the initial staging of recurrent prostate cancer in the clinical algorithms.
From the viewpoint of clinical impact, 68 Ga-PSMA PET/CT led to a change in management in 60% with recurrent prostate cancer [23]. The proportion of patients in whom systemic therapy was selected decreased from 60 to 34% based on the information provided by the 68 Ga-PSMA PET/CT scan. In another cohort of the early biochemical relapse setting following radical prostatectomy, 68 Ga-PSMA PET/CT led to a management change in 42.8% [24]. These articles suggested that some clinical impact of 68 Ga-PSMA may be seen in about half of prostate cancer patients. In summary, 68 Ga-PSMA is a tracer outgrowth that has the potential to significantly change treatment strategies for prostate cancer.
68Ga-PSMA PET/CT beyond prostate cancer
The role of 68 Ga-PSMA PET/CT in the staging of prostate cancer has been widely reported. As PSMA is also overexpressed in the neovasculature of other tumours [25], it has a great potential for the diagnosis of cancer beyond prostate cancer [26].
Raveenthiran et al. evaluated the value of 68 Ga-PSMA PET/CT in the investigation and management decisions of renal cell carcinoma. 68 Ga-PSMA-avid primary lesions were identified in 75% of cases, the majority of which were clear cell subtype. The 68 Ga-PSMA PET/CT findings altered the clinical management in 43.8% of the primary staging patients and in 40.9% of those undergoing restaging, and directly changed the management in 42.1% of patients following the identification of new sites of suspected metastases and the detection of synchronous primaries [27].
Metastasis to organs can also be identified by 68 Ga-PSMA PET/CT. Sathekge et al. reported highly positive 68 Ga-PSMA PET/CT in cerebral metastases and widespread skeletal metastases. Identified 68 Ga-PSMA-positive lesions can be treated using recently introduced 177Lu-PSMA-617 RLT and 225Ac-PSMA RLT. Sathekge et al. described a patient with brain metastasis from prostate cancer who was treated with 225Ac-PSMA ligand. The patient was treated with one cycle of 225Ac-PSMA-617 with activity of 8 MBq. After one cycle of 225Ac-PSMA-617 therapy, 68 Ga-PSMA PET/CT demonstrated marked functional and biochemical responses [14]. This case highlights the potential of 225Ac-PSMA-617 for treatment of brain metastases from metastatic castration-resistant prostate cancer with limited treatment options. Therefore, the potential of PSMA for identification of metastasis and cancer beyond prostate cancer appears to be substantial in terms of patient management and subsequent alpha and beta radiation therapy.
Pfob et al. reported parathyroid adenoma as an incidental finding on 68 Ga PSMA PET/CT [28]. It is important to understand the physiological uptake of PSMA ligand in PSMA-avid benign lesions to avoid misdiagnosis and the possible side effects of subsequent alpha and beta radiation therapy. As the number of studies reporting incidental findings on 68 Ga PSMA PET/CT has increased recently, we need to regularly update our understanding of the behavior 68 Ga PSMA PET/CT [26].
In surveying for organ-specific disease, the most precise imaging modality will greatly increase the diagnostic sensitivity. Morsing et al. reported the results of a hybrid PET/MRI study of major cancers [29]. They considered that PSMA PET can be most effectively employed in PET/MRI because of the superior image quality of MRI imaging of the pelvis compared with PET/CT, which will in turn improve accuracy in the assessment of disease extent and the discrimination of benign lesions from physiological uptake.
Understanding the potential of 68 Ga PSMA PET/CT as an emerging imaging modality will enable the further application of PSMA ligand.
Conclusions
In this review article, we briefly overviewed the current status of PSMA RLT and PSMA PET. We hope that this topic will be a particular focus of attention for most ANM readers in Japan, and that our efforts will facilitate the early approval of PSMA RLT and PSMA PET by the Japanese government even if only slightly.
References
Bander NH, Nanus DM, Milowsky MI, Kostakoglu L, Vallabahajosula S, Goldsmith SJ. Targeted systemic therapy of prostate cancer with a monoclonal antibody to prostate-specific membrane antigen. Semin Oncol. 2003;30:667–76.
Kratochwil C, Fendler WP, Eiber M, Baum R, Bozkurt MF, Czernin J, et al. EANM procedure guidelines for radionuclide therapy with 177Lu-labelled PSMA-ligands (177Lu-PSMA-RLT). Eur J Nucl Med Mol Imaging. 2019;46:2536–44.
Afshar-Oromieh A, Malcher A, Eder M, Eisenhut M, Linhart HG, Hadaschik BA, et al. PET imaging with a [68Ga]gallium-labelled PSMA ligand for the diagnosis of prostate cancer: biodistribution in humans and first evaluation of tumour lesions. Eur J Nucl Med Mol Imaging. 2013;40:486–95.
Jadvar H. Value proposition of PSMA-targeted alpha-particle radioligand therapy in metastatic prostate cancer. Eur J Nucl Med Mol Imaging. 2019;46:8–10.
Banerjee SR, Kumar V, Lisok A, Chen J, Brummet MM, Boinapally S, et al. 177Lu-labeled low-molecular-weight agents for PSMA-targeted radiopharmaceutical therapy. Eur J Nucl Med Mol Imaging. 2019;46:2545–57.
Schumann S, Scherthan H, Lapa C, Serfling S, Muhtadi R, Lassmann M, et al. DNA damage in blood leucocytes of prostate cancer patients during therapy with 177Lu-PSMA. Eur J Nucl Med Mol Imaging. 2019;46:1723–54.
Eberlein U, Nowak C, Bluemel C, Buck AK, Werner RA, Scherthan H, et al. DNA damage in blood lymphocytes in patients after 177Lu peptide receptor radionuclide therapy. Eur J Nucl Med Mol Imaging. 2015;42:1739–49.
Yordanova A, Linden P, Hauser S, Kürpig S, Feldmann G, Gaertner FC, et al. Outcome and safety of rechallenge [177Lu]Lu-PSMA-617 in patients with metastatic prostate cancer. Eur J Nucl Med Mol Imaging. 2019;46:1073–80.
Rathke H, Kratochwil C, Hohenberger R, Giesel FL, Bruchertseifer F, Flechsig P, et al. Initial clinical experience performing sialendoscopy for salivary gland protection in patients undergoing 225Ac-PSMA-617 RLT. Eur J Nucl Med Mol Imaging. 2019;46:139–47.
Watabe T, Liu Y, Kaneda-Nakashima K, Shirakami Y, Lindner T, Ooe K, et al. Theranostics targeting fibroblast activation protein in the tumor stroma: 64Cu- and 225Ac-labeled FAPI-04 in pancreatic cancer xenograft mouse models. J Nucl Med. 2020;61:563–9.
Watabe T, Kaneda-Nakashima K, Liu Y, Shirakami Y, Ooe K, Toyoshima A, et al. Enhancement of 211At uptake via the sodium iodide symporter by the addition of ascorbic acid in targeted alpha-therapy of thyroid cancer. J Nucl Med. 2019;60:1301–7.
Sathekge M, Bruchertseifer F, Knoesen O, Reyneke F, Lawal I, Lengana T, et al. 225Ac-PSMA-617 in chemotherapy-naive patients with advanced prostate cancer: a pilot study. Eur J Nucl Med Mol Imaging. 2019a;46:129–38.
Sathekge M, Bruchertseifer F, Knoesen O, Reyneke F, Lawal I, Lengana T, et al. Correction to: 225Ac-PSMA-617 in chemotherapy-naive patients with advanced prostate cancer: a pilot study. Eur J Nucl Med Mol Imaging. 2019b;46:1988.
Sathekge MM, Bruchertseifer F, Lawal IO, Vorster M, Knoesen O, Lengana T, et al. Treatment of brain metastases of castration-resistant prostate cancer with 225Ac-PSMA-617. Eur J Nucl Med Mol Imaging. 2019;46:1756–7.
Khreish F, Ebert N, Ries M, Maus S, Rosar F, Bohnenberger H, et al. 225Ac-PSMA-617/177Lu-PSMA-617 tandem therapy of metastatic castration-resistant prostate cancer: pilot experience. Eur J Nucl Med Mol Imaging. 2020;47:721–8.
Kratochwil C, Schmidt K, Afshar-Oromieh A, Bruchertseifer F, Rathke H, Morgenstern A, et al. Targeted alpha therapy of mCRPC: dosimetry estimate of 213Bismuth-PSMA-617. Eur J Nucl Med Mol Imaging. 2018;45:31–7.
Dos Santos JC, Schafer M, Bauder-Wust U, Lehnert W, Leotta K, Morgenstern A, et al. Development and dosimetry of 203Pb/212Pb-labelled PSMA ligands: bringing “the lead” into PSMA-targeted alpha therapy? Eur J Nucl Med Mol Imaging. 2019;46:1081–91.
Muller C, Umbricht CA, Gracheva N, Tschan VJ, Pellegrini G, Bernhardt P, et al. Terbium-161 for PSMA-targeted radionuclide therapy of prostate cancer. Eur J Nucl Med Mol Imaging. 2019;46:1919–30.
Farolfi A, Ceci F. (68)Ga-PSMA-11 PET/CT in prostate cancer patients with biochemical recurrence after radical prostatectomy and PSA < 0.5 ng/ml. Efficacy and impact on treatment strategy. Eur J Nucl Med Mol Imaging. 2019;46:11–9.
Ceci F, Castellucci P, Graziani T, Farolfi A, Fonti C, Lodi F, et al. (68)Ga-PSMA-11 PET/CT in recurrent prostate cancer: efficacy in different clinical stages of PSA failure after radical therapy. Eur J Nucl Med Mol Imaging. 2019;46:31–9.
Afshar-Oromieh A, Vollnberg B, Alberts I, Bähler A, Sachpekidis C, Dijkstra L, et al. Comparison of PSMA-ligand PET/CT and multiparametric MRI for the detection of recurrent prostate cancer in the pelvis. Eur J Nucl Med Mol Imaging. 2019;46:2289–97.
Donato P, Roberts MJ. Improved specificity with (68)Ga PSMA PET/CT to detect clinically significant lesions “invisible” on multiparametric MRI of the prostate: a single institution comparative analysis with radical prostatectomy histology. Eur J Nucl Med Mol Imaging. 2019;46:20–30.
Müller J, Ferraro DA, Muehlematter UJ, Garcia Schüler HI, Kedzia S, Eberli D, et al. Clinical impact of (68)Ga-PSMA-11 PET on patient management and outcome, including all patients referred for an increase in PSA level during the first year after its clinical introduction. Eur J Nucl Med Mol Imaging. 2019;46:889–900.
Bashir U, Tree A, Mayer E, Levine D, Parker C, Dearnaley D, et al. Impact of Ga-68-PSMA PET/CT on management in prostate cancer patients with very early biochemical recurrence after radical prostatectomy. Eur J Nucl Med Mol Imaging. 2019;46:901–7.
Chang SS, O’Keefe DS, Bacich DJ, Reuter VE, Heston WD, Gaudin PB. Prostate-specific membrane antigen is produced in tumor-associated neovasculature. Clin Cancer Res. 1999;5:2674–81.
Backhaus P, Noto B, Avramovic N, et al. Targeting PSMA by radioligands in non-prostate disease-current status and future perspectives. Eur J Nucl Med Mol Imaging. 2018;45:860–77.
Raveenthiran S, Esler R, Yaxley J, Kyle S. The use of (68)Ga-PET/CT PSMA in the staging of primary and suspected recurrent renal cell carcinoma. Eur J Nucl Med Mol Imaging. 2019;46:2280–8.
Pfob CH, Karimov I, Jesinghaus M, Novotny A, Weber WA, Eiber M, et al. Pitfalls in Ga-68-PSMA-PET/CT: incidental finding of parathyroid adenoma. Eur J Nucl Med Mol Imaging. 2019;46:1041.
Morsing A, Hildebrandt MG, Vilstrup MH, Wallenius SE, Gerke O, Petersen H, et al. Hybrid PET/MRI in major cancers: a scoping review. Eur J Nucl Med Mol Imaging. 2019;46:2138–51.
Acknowledgements
This work was not supported financially.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Inubushi, M., Miura, H., Kuji, I. et al. Current status of radioligand therapy and positron-emission tomography with prostate-specific membrane antigen. Ann Nucl Med 34, 879–883 (2020). https://doi.org/10.1007/s12149-020-01549-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12149-020-01549-5