Abstract
Objective
To present the clinical, lab profile and outcome of a series of six children who had features of meningoencephalitis (median age of 10.5 y) diagnosed as confirmed scrub typhus (ST) by using a lgM ELISA commercial kit (InBiOS International Inc. USA).
Methods
This was a prospective observational study conducted at a tertiary care hospital, over a period of 7 mo through April 2014. All the patients with undifferentiated febrile illness (aged 1–18 y) with fever of 5–21 d duration were evaluated. After thorough physical examination they were subjected to blood investigations such as complete blood count (CBC), blood culture, hepatic and kidney function tests, serum electrolytes, cerebrospinal fluid (CSF) analysis and IgM ELISA for scrub typhus, coagulogram and chest radiograph, wherever indicated.
Results
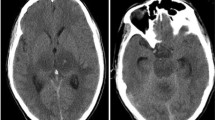
During this period, of the total 81 confirmed cases based on a positive scrub IgM ELISA and/or eschar, 6 (7.4 %), had neurological involvement in the form of presence of neck stiffness, altered sensorium and/or seizures and the CSF findings were suggestive of meningoencephalitis and all had evidence of multiple organ dysfunction syndrome (MODS) needing intensive care. The CECT could be performed in four patients only showing evidence of effacement of sulci and evidence of brain edema.
Conclusions
This communication highlights that variable central nervous system (CNS) involvement is not uncommon in patients with scrub typhus with high mortality. CSF and neuro-radiology findings are nonspecific as these are also observed in patients with aseptic meningitis or encephalitis. Early suspection and institution of appropriate therapy without delay will lead to substantial reduction in the morbidity and mortality.

Similar content being viewed by others
References
Saah AJ. Orientia tsutsugamushi (scrub typhus). In: Mandell GL, Bennett JE, Dolin R, editors. Principles and practice of infectious disease. 5th ed. Philadelphia: Churchill Livingstone; 2000. p. 2056–7.
Settle EB, Pinkerton H, Corbett AJ. A pathologic study of tsutsugamushi disease (scrub typhus) with notes on clinicopathologic correlation. J Lab Clin Med. 1945;30:639–61.
Levine HD. Pathologic study of thirty-one cases of scrub typhus fever with especial reference to the cardiovascular system. Am Heart J. 1946;31:314–28.
Tay ST, Rohani MY, Ho TM, Devi S. Antigenic types of Orientia tsutsugamushi in Malaysia. Southeast Asian J Trop Med Public Health. 2002;33:557–64.
Isaac R, Varghese GM, Mathai E, Manjula J, Joseph I. Scrub typhus: prevalence and diagnostic issues in rural southern India. Clin Infect Dis. 2004;39:1395–6.
Watt G, Parola P. Scrub typhus and tropical rickettsioses. Curr Opin Infect Dis. 2003;16:429–36.
Lee MS, Lee JH, Lee HS, et al. Scrub typhus as a possible aetiology of Guillain-Barre syndrome: two cases. Ir J Med Sci. 2009;178:347–50.
Lee KL, Lee JK, Yim YM, Lim OK, Bae KH. Acute transverse myelitis associated with scrub typhus: case report and a review of literatures. Diagn Microbiol Infect Dis. 2008;60:237–9.
Lin WR, Chen TC, Lin CY, Lu PL, Chen YH. Bilateral simultaneous facial palsy following scrub typhus meningitis. Kaohsiung J Med Sci. 2011;27:573–6.
Viswanathan S, Muthu V, Iqbal N, Remalayam B, George T. Scrub typhus meningitis in South India — a retrospective study. PLoS ONE. 2013;8:e66595.
Lee CS, Hwang JH, Lee HB, Kwon KS. Risk factors leading to fatal outcome in scrub typhus patients. Am J Trop Med Hyg. 2009;81:484–8.
Silpapojakul K, Ukkachoke C, Krisanapan S. Rickettsial meningitis and encephalitis. Arch Intern Med. 1991;151:1753–7.
Wie SH, Chang UI, Kim HW, et al. Clinical features of 212 cases of scrub typhus in southern region of Gyeonggido and the significance of initial simple chest x-ray. Infect Chemother. 2008;40:40–5.
Varghese GM, Mathew A, Kumar S, Abraham OC, Trowbridge P, Mathai E. Differential diagnosis of scrub typhus meningitis from bacterial meningitis using clinical and laboratory features. Neurol India. 2013;61:17–20.
Pai H, Sohn S, Seong Y, Kee S, Chang WH, Choe KW. Central nervous system involvement in patients with scrub typhus. Clin Infect Dis. 1997;24:436–40.
Thakur JS, Mohindroo NK, Sharma DR, Soni K, Kaushal SS. Evoked response audiometry in scrub typhus: prospective, randomised, case–control study. J Laryngol Otol. 2011;125:567–71.
Drevets DA, Leenen PJ, Greenfield RA. Invasion of the central nervous system by intracellular bacteria. Clin Microbiol Rev. 2004;17:323–47.
Kim DE, Lee SH, Park KI, Chang KH, Roh JK. Scrub typhus encephalomyelitis with prominent focal neurologic signs. Arch Neurol. 2000;57:1770–2.
Chrispal A, Boorugu H, Gopinath KG, et al. Scrub typhus: an unrecognized threat in South India – clinical profile and predictors of mortality. Trop Dr. 2010;40:129–33.
Kim DM, Kim YS, Cho HY, Lee YB. Scrub typhus meningoencephalitis occurring during doxycycline therapy for Orientia tsutsugamushi. Diagn Microbiol Infect Dis. 2011;69:271–4.
Jeong YJ, Kim S, Wook YD, et al. Scrub typhus: clinical, pathologic, and imaging findings. Radiographics. 2007;27:161–72.
Allen AC, Spitz S. A comparative study of the pathology of scrub typhus (Tsutsugamushi disease) and other rickettsial diseases. Am J Pathol. 1945;21:603–81.
Kularatne SA, Weerakoon KG, Rajapakse RP, et al. A case series of spotted fever rickettsiosis with neurological manifestations in Sri Lanka. Int J Infect Dis. 2012;16:e514–7.
Papez JW, Bateman JF. Destruction of nerve cells by rickettsial organisms of tsutsugamushi fever. Arch Neurol Psychiatr. 1949;61:545–7.
Varghese GM, Abraham OC, Mathai D, et al. Scrub typhus among hospitalised patients with febrile illness in South India: magnitude and clinical predictors. J Infect. 2006;52:56–60.
Koh GC, Maude RJ, Paris DH, Newton PN, Blacksell SD. Diagnosis of scrub typhus. Am J Trop Med Hyg. 2010;82:368–70.
Kim DM, Kim SW, Choi SH, et al. Clinical and laboratory findings associated with severe scrub typhus. BMC Infect Dis. 2010;10:108.
Varghese GM, Trowbridge P, Janardhanan J, et al. Clinical profile and improving mortality trend of scrub typhus in South India. Int J Infect Dis. 2014;23:39–43.
Vivekanandan M, Mani A, Priya YS, Singh AP, Jayakumar S, Purty S. Outbreak of scrub typhus in Pondicherry. J Assoc Physicians India. 2010;58:24–8.
Boorugu H, Chrispal A, Gopinath KG, et al. CNS involvement in Scrub typhus. Trop Dr. 2014;44:36–7.
Nigwekar P, Kavar Y, Shrikhande DY, Ashok Kumar C. Clinico-pathological profile of Rickettsial Fever in a rural area of western Maharashtra, India. Pravara Med Rev. 2013;5:5–9.
Saifudheen K, Kumar KG, Jose J, Veena V, Gafoor VA. First case of scrub typhus with meningoencephalitis from Kerala: an emerging infectious threat. Ann Indian Acad Neurol. 2012;15:141–4.
Kumar V, Kumar V, Yadav AK, et al. Scrub typhus is an under-recognized cause of acute febrile illness with acute kidney injury in India. PLoS Negl Trop Dis. 2014;8:e2605.
Jeong YJ, Kim S, Wook YD, Lee JW, Kim KI, Lee SH. Scrub typhus: clinical, pathologic and imaging findings. Radiographics. 2007;27:161–72.
Yum KS, Na SJ, Lee KO, Ko JH. Scrub typhus meningo-encephalitis with focal neurologic signs and associated brain MRI abnormal findings: literature review. Clin Neurol Neurosurg. 2011;113:250–3.
Kar A, Dhanaraj M, Dedeepiya D, Harikrishna K. Acute encephalitis syndrome following scrub typhus infection. Indian J Crit Care Med. 2014;18:453–5.
Dotevall L, Hagberg L. Penetration of doxycycline into cerebrospinal fluid in patients treated for suspected Lyme neuroborreliosis. Antimicrob Agents Chemother. 1989;33:1078–80.
Raoult D, Drancourt M. Antimicrobial therapy of rickettsial iseases. Antimicrob Agents Chemother. 1991;35:2457–62.
Yim CW, Flynn NM, Fitzgerald FT. Penetration of oral doxycycline into the cerebrospinal fluid of patients with latent or neurosyphilis. Antimicrob Agents Chemother. 1985;28:347–8.
Mindermann T, Zimmerli W, Gratzl O. Rifampin concentrations in various compartments of the human brain: a novel method for determining drug levels in the cerebral extracellular space. Antimicrob Agents Chemother. 1998;42:2626–9.
Jaruratanasirikul S, Hortiwakul R, Tantisarasart T, Phuenpathom N, Tussanasunthornwong S. Distribution of azithromycin into brain tissue, cerebrospinal fluid, and aqueous humor of the eye. Antimicrob Agents Chemother. 1996;40:825–6.
Jang MO, Jang HC, Kim UJ, et al. Outcome of intravenous azithromycin therapy in patients with complicated scrub typhus compared with that of doxycycline therapy using propensity-matched analysis. Antimicrob Agents Chemother. 2014;58:1488–93.
Cho BA, Ko Y, Kim YS, et al. Phenotypic characterization of peripheral T cells and their dynamics in scrub typhus patients. PLoS Negl Trop Dis. 2012;6:e1789.
Raoult D, Drancourt M. Antimicrobial therapy of rickettsial diseases. Antimicrob Agent Chemother. 1991;35:2457–62.
Acknowledgments
The authors acknowledge the support of the parents of the children and the residents and consultants and paramedics of the associated departments.
Contributions
AKS: Planning, conceptualization, editing, final analysis and submission of the manuscript; LC and HG: Enrollment, collection and analysis of data and follow-up. AKS will act as guarantor for the paper.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
None.
Source of Funding
None.
Rights and permissions
About this article
Cite this article
Sood, A.K., Chauhan, L. & Gupta, H. CNS Manifestations in Orientia tsutsugamushi Disease (Scrub Typhus) in North India. Indian J Pediatr 83, 634–639 (2016). https://doi.org/10.1007/s12098-015-2001-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12098-015-2001-2