Abstract
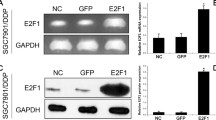
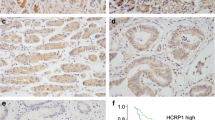
Oxaliplatin-based chemotherapy is the main treatment regimen for gastric cancer (GC), but can fail because of drug resistance. We investigated the role of a recently identified drug-resistance gene, taxol-resistant gene 1 (Txr1), in oxaliplatin resistance. A retrospective study based on banked tissue was carried out. We collected clinical data from 95 patients with stage II–III GC who were treated with radical D2 surgery and standardized first-line chemotherapy with oxaliplatin; paraffin blocks of their tumor specimens were prepared for a tissue microarray in which Txr1 expression was analyzed immunohistochemically and compared with their clinical data and their 3-year disease-free survival (DFS) rate. The human GC cell line, SGC7901, was developed into the oxaliplatin-resistant cell line, SGC7901/L-OHP, using slowly increased oxaliplatin concentrations over 6 months. The relationship between Txr1 expression and drug-resistance of oxaliplatin in GC was studied with drug intervention, gene silencing technology, real-time PCR and Western blot analysis. Of the 95 patients with GC, those with TXR1− GC had longer postoperative 3-year DFS (77.8 %) than those with TXR1+ GC (52.9 %). In oxaliplatin-resistant SGC7901/L-OHP cells, the main expression location of Txr1 shifted from the nucleus to cytoplasm, and both the mRNA and protein expression of Txr1 were higher than that of the parental cells, whereas expression of thrombospondin-1 (TSP1) decreased. When the Txr1 gene was silenced, TSP1 expression increased and the oxaliplatin resistance was significantly reduced in SGC7901/L-OHP cells. Changed Txr1 expression in GC affects the efficacy of oxaliplatin-based chemotherapy. Increased Txr1 expression decreases TSP1 expression and inhibits apoptosis. Txr1 could be a target in reversing oxaliplatin resistance in GC.



Similar content being viewed by others
References
Kwon HC, Roh MS, Oh SY, Kim SH, Kim MC, Kim JS, Kim HJ. Prognostic value of expression of ERCC1, thymidylate synthase, and glutathione S-transferase P1 for 5-fluorouracil/oxaliplatin chemotherapy in advanced gastric cancer. Ann Oncol. 2007;18(3):504–9.
Rivera F, Vega-Villegas ME, Lopez-Brea MF. Chemotherapy of advanced gastric cancer. Cancer Treat Rev. 2007;33(4):315–24.
Martin LP, Hamilton TC, Schilder RJ. Platinum resistance: the role of DNA repair pathways. Clin Cancer Res. 2008;14(5):1291–5.
Yang AD, Fan F, Camp ER, van Buren G, Liu W, Somcio R, Gray MJ, Cheng H, Hoff PM, Ellis LM. Chronic oxaliplatin resistance induces epithelial-to-mesenchymal transition in colorectal cancer cell lines. Clin Cancer Res. 2006;12(14 Pt1):4147–53.
Chen CC, Chen LT, Tsou TC, Pan WY, Kuo CC, Liu JF, Yeh SC, Tsai FY, Hsieh HP, Chang JY. Combined modalities of resistance in an oxaliplatin-resistant human gastric cancer cell line with enhanced sensitivity to 5-fluorouracil. Br J Cancer. 2007;97(3):334–44.
Lih CJ, Wei W, Cohen SN. Txr1: a transcriptional regulator of thrombospondin-1 that modulates cellular sensitivity to Taxanes. Genes Dev. 2006;20(15):2082–95.
Bai ZG, Qu X, Han W, Ma XM, Zhao XM, Zhang ZT. Expression of taxol resistance gene 1 correlates with gastric cancer patient clinical outcome and induces taxol resistance. Mol Med Rep. 2010;3(6):1071–8.
Papadaki C, Mavroudis D, Trypaki M, Koutsopoulos A, Stathopoulos E, Hatzidaki D, Tsakalaki E, Georgoulias V, Souglakos J. Tumoral expression of TXR1 and TSP1 predicts overall survival of patients with lung adenocarcinoma treated with first-line docetaxel-gemcitabine regimen. Clin Cancer Res. 2009;15(11):3827–33.
Peng X, Li W, Tan G. Reversal of taxol resistance by cisplatin in nasopharyngeal carcinoma by upregulating thromspondin-1 expression. Anticancer Drugs. 2010;21(4):381–8.
Bang YJ, Kim YW, Yang HK, Chung HC, Park YK, Lee KH, Lee KW, Kim YH, Noh SI, Cho JY, Mok YJ, Ji J, Yeh TS, Button P, Sirzen F, Noh SH. Adjuvant capecitabine and oxaliplatin for gastric cancer after D2 gastrectomy (CLASSIC): a phase three open-label, randomised controlled trial. Lancet. 2012;379(9813):315–21.
Knauer SK, Kramer OH, Knosel T, Engels K, Rodel F, Kovacs AF, Dietmaier W, Klein-Hitpass L, Habtemichael N, Schweitzer A, Brieger J, Rodel C, Mann W, Petersen I, Heinzel T, Stauber RH. Nuclear export is essential for the tumor-promoting activity of survivin. FASEB J. 2007;21(1):207–16.
Kleinberg L, Florenes VA, Silins I, Haug K, Trope CG, Nesland JM, Davidson B. Nuclear expression of survivin is associated with improved survival in metastatic ovarian carcinoma. Cancer. 2007;109(2):228–38.
Zhang D, Fan D. Multidrug resistance in gastric cancer: recent research advances and ongoing therapeutic challenges. Expert Rev Anticancer Ther. 2007;7(10):1369–78.
Mateo V, Brown EJ, Biron G, Rubio M, Fischer A, Deist FL, Sarfati M. Mechanisms of CD47-induced caspase-independent cell death in normal and leukemic cells: link between phosphatidylserine exposure and cytoskeleton organization. Blood. 2002;100(8):2882–90.
Saumet A, Slimane MB, Lanotte M, Lawler J, Dubernard V. Type 3 repeat/C-terminal domain of thrombospondin-1 triggers caspase-independent cell death through CD47/v3 in promyelocytic leukemia NB4 cells. Blood. 2005;106(2):658–67.
Liu T, Brouha B, Grossman D. Rapid induction of mitochondrial events and caspase independent apoptosis in Survivin targeted melanoma cells. Oncogene. 2004;23(1):39–48.
Pavlyukov Marat S, Antipova Nadezhda V, Balashova Maria V, Vinogradova Tatjana V, Kopantzev Evgenij P, Shakhparonov Mihail I. Survivin monomer plays an essential role in apoptosis regulation. J Biol Chem. 2011;286(26):23296–307.
Acknowledgments
This work was supported by National Natural Science Foundation of China (No. 81172317).
Conflict of interest
We declare no conflict of commercial or associative interest in connection with the work.
Author information
Authors and Affiliations
Corresponding author
Additional information
Jingtao Bi and Zhigang Bai have contributed equally to this work.
Rights and permissions
About this article
Cite this article
Bi, J., Bai, Z., Ma, X. et al. Txr1: an important factor in oxaliplatin resistance in gastric cancer. Med Oncol 31, 807 (2014). https://doi.org/10.1007/s12032-013-0807-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12032-013-0807-1