Abstract
Aim
A review of a single-centre experience of pelvic exenteration as a treatment modality for patients with locally advanced primary and recurrent rectal cancer. The perioperative outcomes, morbidity and long term oncological outcomes are reviewed.
Materials & Methods
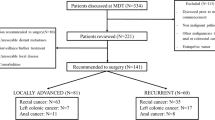
Patients undergoing pelvic exenterations for recurrent and locally advanced rectal cancer between 1 January 2006 and 1 August 2012 were identified from a prospective database. All patients underwent pre-operative staging investigations with computed tomography (CT) scan of chest, abdomen and pelvis and pelvic magnetic resonance imaging (MRI). Patients with locally advanced primary rectal cancer were counselled for pre-operative chemoradiation. Structures such as the urinary bladder and female reproductive organs were resected en bloc where indicated with the lesion. Urological or plastic reconstructions were employed where indicated. The primary outcome measured was overall survival and secondary outcomes measured were time to local recurrence (LR) and systemic recurrence. Disease-free survival was examined by the Kaplan–Meier Method (Fig. 1).
Results
Pelvic exenterations were performed in 13 patients with a median age of 59 (range 26–81). The rate of major post-operative complications was 8 % (n = 1), where the patient had anastomotic leakage. There were no mortalities in the perioperative period. All patients were operated with curative intent and negative circumferential margins were shown in 9 out of 13 patients (70 %). The DFS was 19.4 and the OS was 22.5 months.
Conclusion
An aggressive approach with en bloc resection of organs involved provides survival benefit to patients with locally advanced primary and recurrent rectal cancer with an acceptable morbidity profile.

Similar content being viewed by others
References
Brunschwig A. Complete excision of pelvic viscera for advanced carcinoma: one-stage abdominoperineal operation with end colostomy and bilateral ureteral implantation into colon above colostomy. Cancer. 1948;1:177–83.
Tjandra JJ, Kilkenny JW, Buie WD, et al. Practice parameters for the Management of Rectal Cancer (Revised). Dis Colon Rectum. 2005;48:411–23.
Harris DA, Davies M, Lucas MG, Drew P, Carr ND, Beynon J. Multivisceral resection for primary locally advanced rectal carcinoma. Br J Surg. 2011;98:582–8.
Park J, Guillem J. T4 And recurrent rectal cancer current clinical oncology. Rectal, Cancer. 2013;6:109–21.
Rodriguez-Bigas MA, Petrelli NJ. Pelvic exenteration and its modifications. Am J Surg. 1996;171:293–301.
Gunderson LL, Jessup JM, Sargent DJ, Greene FL, Stewart A. Revised tumor and node categorization for rectal cancer based on surveillance, epidemiology, and End results and rectal pooled analysis outcomes. J Clin Oncol. 2010;28:256–63.
Palmer G, Martling A, Lagergren P, Cedermark B, Holm T. Quality of life after potentially curative treatment for locally advanced rectal cancer. Ann Surg Oncol. 2008;15:3109–17.
Gannon CJ, Zager JS, Chang GJ, et al. Pelvic exenteration affords safe and durable treatment for locally advanced rectal carcinoma. Ann Surg Oncol. 2007;14:1870–7.
Lopez MJ, Monafo WW. Role of extended resection in the initial treatment of locally advanced colorectal carcinoma. Surgery. 1993;113:365–72.
Nielsen MB, Rasmussen PC, Lindegaard JC, Laurberg S. A 10-year experience of total pelvic exenteration for primary advanced and locally recurrent rectal cancer based on a prospective database. Colorectal Dis. 2012;14:1076–83.
Farouk R, Nelson H, Radice E, Mercill S, Gunderson L. Accuracy of computed tomography in determining resectability for locally advanced primary or recurrent colorectal cancers. Am J Surg. 1998;175:283.
Messiou C, Chalmers AG, Boyle K, Wilson D, Sagar P. Pre-operative MR assessment of recurrent rectal cancer. Br J Radiol. 2008;81:468–73.
Petros JG, Augustinos P, Lopez MJ. Pelvic exenteration for carcinoma of the colon and rectum. Semin Surg Oncol. 1999;17:206–12.
Sauer R, Becker H, Hohenberger W, et al. Preoperative versus postoperative chemoradiotherapy for rectal cancer. N Engl J Med. 2004;351:1731–40.
Bosset JF, Collette L, Calais G, et al. Chemotherapy with preoperative radiotherapy in rectal cancer. N Engl J Med. 2006;14:355–7.
Lehnert T, Methner M, Pollok A, Schaible A, Hinz U, Herfarth C. Multivisceral resection for locally advanced primary colon and rectal cancer: an analysis of prognostic factors in 201 patients. Ann Surg. 2002;235:217–25.
Gohl J, Merkel S, Rodel C, Hohenberger W. Can neoadjuvant radiochemotherapy improve the results of multivisceral resections in advanced rectal carcinoma (cT4a). Colorectal Dis. 2003;5:436–41.
Govindarajan A, Coburn NG, Kiss A, Rabeneck L, Smith AJ, Law CH. Population-based assessment of the surgical management of locally advanced colorectal cancer. J Natl Cancer Inst. 2006;98:1474–81.
Lopez MJ. Multivisceral resections for colorectal cancer. J Surg Oncol. 2001;76:1–5.
Law WL, Chu KW, Choi HK. Total pelvic exenteration for locally advanced rectal cancer. J Am Coll Surg. 2000;190:78–83.
Wanebo HJ, Koness RJ, Vezeridis MP, Cohen SI, Wrobleski DE. Pelvic resection of recurrent rectal cancer. Ann Surg. 1994;220:586–9.
Bricker EM, Kraybill WG, Lopez MJ, Johnston WD. The current role of ultraradical surgery in the treatment of pelvic cancer. Curr Probl Surg. 1986;23:869–953.
Chessin DB, Hartley J, Cohen AM, et al. Rectus flap reconstruction decreases perineal wound complications after pelvic chemoradiation and surgery: a cohort study. Ann Surg Oncol. 2005;12:104–10.
Sagar PM. Extended surgery for local recurrence and advanced rectal cancer. Colorectal Dis. 2006;8:43–6.
Pearlman NW, Donohue RE, Stiegmann GV, et al. Pelvic and sacropelvic exenteration for locally advanced or recurrent anorectal cancer. Arch Surg. 1987;122:537–41.
Conflict of Interest
All authors have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Xin, K.Y., Ng, D.W.J., Tan, G.H.C. et al. Role of Pelvic Exenteration in the Management of Locally Advanced Primary and Recurrent Rectal Cancer. J Gastrointest Canc 45, 291–297 (2014). https://doi.org/10.1007/s12029-014-9586-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12029-014-9586-y