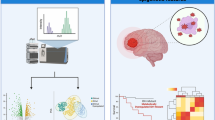
Abstract
Background
Cerebral edema and intracranial hypertension are major contributors to unfavorable prognosis in traumatic brain injury (TBI). Local epigenetic changes, particularly in DNA methylation, may influence gene expression and thus host response/secondary injury after TBI. It remains unknown whether DNA methylation in the central nervous system is associated with cerebral edema severity or intracranial hypertension post TBI. We sought to identify epigenome-wide DNA methylation patterns associated with these forms of secondary injury after TBI.
Methods
We obtained genome-wide DNA methylation profiles of DNA extracted from ventricular cerebrospinal fluid samples at three different postinjury time points from a prospective cohort of patients with severe TBI (n = 89 patients, 254 samples). Cerebral edema and intracranial pressure (ICP) measures were clustered to generate composite end points of cerebral edema and ICP severity. We performed an unbiased epigenome-wide association study (EWAS) to test associations between DNA methylation at 419,895 cytosine–phosphate–guanine (CpG) sites and cerebral edema/ICP severity categories. Given inflated p values, we conducted permutation tests for top CpG sites to filter out potential false discoveries.
Results
Our data-driven hierarchical clustering across six cerebral edema and ICP measures identified two groups differing significantly in ICP based on the EWAS-identified CpG site cg22111818 in RGMA (Repulsive guidance molecule A, permutation p = 4.20 × 10−8). At 3–4 days post TBI, patients with severe intracranial hypertension had significantly lower levels of methylation at cg22111818.
Conclusions
We report a novel potential relationship between intracranial hypertension after TBI and an acute, nonsustained reduction in DNA methylation at cg22111818 in the RGMA gene. To our knowledge, this is the largest EWAS in severe TBI. Our findings are further strengthened by previous findings that RGMA modulates axonal repair in other central nervous system disorders, but a role in intracranial hypertension or TBI has not been previously identified. Additional work is warranted to validate and extend these findings, including assessment of its possible role in risk stratification, identification of novel druggable targets, and ultimately our ability to personalize therapy in TBI.



Similar content being viewed by others
References
Georges A, Booker JG. Traumatic brain injury. StatPearls Publishing; 2020.
Stocchetti N, Maas AIR. Traumatic intracranial hypertension. N Engl J Med. 2014;370:2121–30.
Jha RM, Kochanek PM, Simard JM. Pathophysiology and treatment of cerebral edema in traumatic brain injury. Neuropharmacology. 2019;145:230–46.
Jha RM, Koleck TA, Puccio AM, Okonkwo DO, Park S-Y, Zusman BE, et al. Regionally clustered ABCC8 polymorphisms in a prospective cohort predict cerebral oedema and outcome in severe traumatic brain injury. J Neurol Neurosurg Psychiatry. 2018;89:1152–62.
Jha RM, Puccio AM, Okonkwo DO, Zusman BE, Park S-Y, Wallisch J, et al. ABCC8 single nucleotide polymorphisms are associated with cerebral edema in severe TBI. Neurocrit Care. 2017;26:213–24.
Dardiotis E, Paterakis K, Tsivgoulis G, Tsintou M, Hadjigeorgiou GF, Dardioti M, et al. AQP4 tag single nucleotide polymorphisms in patients with traumatic brain injury. J Neurotrauma. 2014;31:1920–6.
Dardiotis E, Fountas KN, Dardioti M, Xiromerisiou G, Kapsalaki E, Tasiou A, et al. Genetic association studies in patients with traumatic brain injury. Neurosurg Focus. 2010;28:E9.
Jha RM, Desai SM, Zusman BE, Koleck TA, Puccio AM, Okonkwo DO, et al. Downstream TRPM4 polymorphisms are associated with intracranial hypertension and statistically interact with ABCC8 polymorphisms in a prospective cohort of severe traumatic brain injury. J Neurotrauma. 2019;36:1804–17.
Law P-P, Holland ML. DNA methylation at the crossroads of gene and environment interactions. Essays Biochem. 2019;63:717–26.
Haghighi F, Ge Y, Chen S, Xin Y, Umali MU, De Gasperi R, et al. Neuronal DNA methylation profiling of blast-related traumatic brain injury. J Neurotrauma. 2015;32:1200–9.
Zhang Z-Y, Zhang Z, Fauser U, Schluesener HJ. Global hypomethylation defines a sub-population of reactive microglia/macrophages in experimental traumatic brain injury. Neurosci Lett. 2007;429:1–6.
Gao W-M, Chadha MS, Kline AE, Clark RSB, Kochanek PM, Dixon CE, et al. Immunohistochemical analysis of histone H3 acetylation and methylation–evidence for altered epigenetic signaling following traumatic brain injury in immature rats. Brain Res. 2006;1070:31–4.
Chatterton Z, Mendelev N, Chen S, Raj T, Walker R, Carr W, et al. Brain-derived circulating cell-free DNA defines the brain region and cell specific origins associated with neuronal atrophy. bioRxiv. 2019;538827.
Lehmann-Werman R, Neiman D, Zemmour H, Moss J, Magenheim J, Vaknin-Dembinsky A, et al. Identification of tissue-specific cell death using methylation patterns of circulating DNA. Proc Natl Acad Sci USA Natl Acad Sci. 2016;113:E1826–34.
Abu Hamdeh S, Ciuculete D-M, Sarkisyan D, Bakalkin G, Ingelsson M, Schiöth HB, et al. Differential DNA methylation of the genes for amyloid precursor protein, tau, and neurofilaments in human traumatic brain injury. J Neurotrauma. 2021;38:1679–88.
Nagalakshmi B, Sagarkar S, Sakharkar AJ. Epigenetic mechanisms of traumatic brain injuries. Prog Mol Biol Transl Sci. 2018;157:263–98.
Mateen BA, Hill CS, Biddie SC, Menon DK. DNA methylation: basic biology and application to traumatic brain injury. J Neurotrauma. 2017;34:2379–88.
Wong VS, Langley B. Epigenetic changes following traumatic brain injury and their implications for outcome, recovery and therapy. Neurosci Lett. 2016;625:26–33.
Oros Klein K, Grinek S, Bernatsky S, Bouchard L, Ciampi A, Colmegna I, et al. funtooNorm: an R package for normalization of DNA methylation data when there are multiple cell or tissue types. Bioinformatics. 2016;32:593–5.
Aryee MJ, Jaffe AE, Corrada-Bravo H, Ladd-Acosta C, Feinberg AP, Hansen KD, et al. Minfi: a flexible and comprehensive Bioconductor package for the analysis of Infinium DNA methylation microarrays. Bioinformatics. 2014;30:1363–9.
Xu Z, Niu L, Li L, Taylor JA. ENmix: a novel background correction method for Illumina HumanMethylation450 BeadChip. Nucleic Acids Res. 2016;44:e20.
Team RC. R: a language and environment for statistical computing [Internet]. 2018 [cited 2021 Jan 7]. Available from: https://www.R-project.org.
Ritchie ME, Phipson B, Wu D, Hu Y, Law CW, Shi W, et al. limma powers differential expression analyses for RNA-sequencing and microarray studies. Nucleic Acids Res. 2015;43:e47–57.
Leek JT, Johnson WE, Parker HS, Jaffe AE, Storey JD. The sva package for removing batch effects and other unwanted variation in high-throughput experiments. Bioinformatics. 2012;28:882–3.
Saffari A, Silver MJ, Zavattari P, Moi L, Columbano A, Meaburn EL, et al. Estimation of a significance threshold for epigenome-wide association studies. Genet Epidemiol. 2018;42:20–33.
Good P. Permutation tests. New York: Springer; 2000.
Houseman EA, Kile ML, Christiani DC, Ince TA, Kelsey KT, Marsit CJ. Reference-free deconvolution of DNA methylation data and mediation by cell composition effects. BMC Bioinform BioMed Central. 2016;17:259–315.
Oldekamp J, Krämer N, Alvarez-Bolado G, Skutella T. Expression pattern of the repulsive guidance molecules RGM A, B and C during mouse development. Gene Expr Patterns. 2004;4:283–8.
Monnier PP, Sierra A, Macchi P, Deitinghoff L, Andersen JS, Mann M, et al. RGM is a repulsive guidance molecule for retinal axons. Nature. 2002;419:392–5.
O’Leary C, Cole SJ, Langford M, Hewage J, White A, Cooper HM. RGMa regulates cortical interneuron migration and differentiation. Chédotal A, editor. PLoS ONE. 2013;8:e81711.
Matsunaga E, Nakamura H, Chédotal A. Repulsive guidance molecule plays multiple roles in neuronal differentiation and axon guidance. J Neurosci Soc Neurosci. 2006;26:6082–8.
Matsunaga E, Tauszig-Delamasure S, Monnier PP, Mueller BK, Strittmatter SM, Mehlen P, et al. RGM and its receptor neogenin regulate neuronal survival. Nat Cell Biol. 2004;6:749–55.
Fujita Y, Yamashita T. The roles of RGMa-neogenin signaling in inflammation and angiogenesis. Inflamm Regen BioMed Central. 2017;37:4–6.
Schwab JM, Monnier PP, Schluesener HJ, Conrad S, Beschorner R, Chen L, et al. Central nervous system injury-induced repulsive guidance molecule expression in the adult human brain. Arch Neurol Am Med Assoc. 2005;62:1561–8.
Chen L, Gao B, Fang M, Li J, Mi X, Xu X, et al. Lentiviral vector-induced overexpression of RGMa in the hippocampus suppresses seizures and mossy fiber sprouting. Mol Neurobiol. 2017;54:1379–91.
Kong Y, Rogers MR, Qin X. Effective neuroprotection by ischemic postconditioning is associated with a decreased expression of RGMa and inflammation mediators in ischemic rats. Neurochem Res. 2013;38:815–25.
Satoh J, Tabunoki H, Ishida T, Saito Y, Arima K. Accumulation of a repulsive axonal guidance molecule RGMa in amyloid plaques: a possible hallmark of regenerative failure in Alzheimer’s disease brains. Neuropathol Appl Neurobiol. 2013;39:109–20.
Muramatsu R, Kubo T, Mori M, Nakamura Y, Fujita Y, Akutsu T, et al. RGMa modulates T cell responses and is involved in autoimmune encephalomyelitis. Nat Med. 2011;17:488–94.
Nohra R, Beyeen AD, Guo JP, Khademi M, Sundqvist E, Hedreul MT, et al. RGMA and IL21R show association with experimental inflammation and multiple sclerosis. Genes Immun. 2010;11:279–93.
Mothe AJ, Tassew NG, Shabanzadeh AP, Penheiro R, Vigouroux RJ, Huang L, et al. RGMa inhibition with human monoclonal antibodies promotes regeneration, plasticity and repair, and attenuates neuropathic pain after spinal cord injury. Sci Rep. 2017;7:10529–618.
Hata K, Fujitani M, Yasuda Y, Doya H, Saito T, Yamagishi S, et al. RGMa inhibition promotes axonal growth and recovery after spinal cord injury. J Cell Biol. 2006;173:47–58.
Wilson M-M, Henshall DC, Byrne SM, Brennan GP. CHD2-related CNS pathologies. IJMS. 2021;22:588.
Jha RM, Kochanek PM. A precision medicine approach to cerebral edema and intracranial hypertension after severe traumatic brain injury: Quo Vadis? Curr Neurol Neurosci Rep. 2018;18:105–19.
Acknowledgements
We thank the participants of this study for making this work possible.
Funding
The authors are grateful to funding from the following grants: National Institutes of Health (NIH)/National Institute of Neurological Disorders and Stroke (NINDS) Grant K23NS101036 (RMJ), NIH/NINDS Grant R01NS115815 (RMJ), NIH Grant R21NR015142 (YPC), NIH/National Institute of Nursing Research (NINR) Grant R00 NR013176 (AMP), NIH Grant P50 NS30318 (DOO), NIH/NINDS Grant 1R01NS087978-01 (PMK), NIH/NINR Grant R01NR013342 (YPC), the Chuck Noll Foundation (PMK and RMJ), and the Barrow Neurological Foundation (RMJ).
Author information
Authors and Affiliations
Contributions
RMJ and YPC are the principal investigators of the cerebral edema and epigenome-wide association studies of TBI, respectively. RMJ, YPC, DEW, JRS, and DL conceived and designed the study. BEZ, SMD, AMP, and DOO collected the phenotype data. DL, YL, AIA, and SL performed the statistical analysis and contributed to the initial writing of the manuscript. All authors reviewed, edited, and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflicts of Interest
RMJ is a paid consultant and is on advisory boards for Biogen and ASTRAL (Antagonizing SUR1-TRPM4 to Reduce the Progression of Intracerebral Hematoma and Edema Surrounding Lesions clinical trial). The other authors declare no conflicts of interest.
Ethical approval/informed consent
The University of Pittsburgh Institutional Review Board approved this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Liu, D., Zusman, B.E., Shaffer, J.R. et al. Decreased DNA Methylation of RGMA is Associated with Intracranial Hypertension After Severe Traumatic Brain Injury: An Exploratory Epigenome-Wide Association Study. Neurocrit Care 37, 26–37 (2022). https://doi.org/10.1007/s12028-021-01424-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-021-01424-9