Abstract
Mesenchymal Stem Cells (MSCs), as an adult stem cell type, are used to treat various disorders in clinics. However, derivation of homogenous and adequate amount of MSCs limits the regenerative treatment potential. Although mesoderm is the main source of mesenchymal progenitors during embryonic development, neuromesodermal progenitors (NMPs), reside in the primitive streak during development, is known to differentiate into paraxial mesoderm. In the current study, we generated NMPs from human embryonic stem cells (hESC), subsequently derived MSCs and characterized this cell population in vitro and in vivo. Using a bFGF and CHIR induced NMP formation protocol followed by serum containing culture conditions; here we show that MSCs can be generated from NMPs identified by not only the expression of T/Bra and Sox 2 but also FLK-1/PDGFRα in our study. NMP-derived MSCs were plastic adherent fibroblast like cells with colony forming capacity and trilineage (osteo-, chondro- and adipo-genic) differentiation potential. In the present study, we demonstrate that NMP-derived MSCs have an endothelial tendency which might be related to their FLK-1+/PDGFRα + NMP origin. NMP-derived MSCs displayed a protein expression profile of characterized MSCs. Growth factor and angiogenesis related pathway proteins were similarly expressed in NMP-derived MSCs and characterized MSCs. NMP-derived MSCs keep characteristics after short-term and long-term freeze-thaw cycles and localized into bone marrow followed by tail vein injection into NOD/SCID mice. Together, these data showed that hESC-derived NMPs might be used as a precursor cell population for MSC derivation and could be used for in vitro and in vivo research.
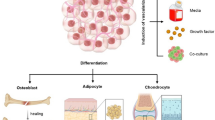
Graphical abstract







Similar content being viewed by others
Data Availability
Data is available upon request.
Code Availability
Not applicable.
References
Abdal Dayem, A., Lee, S. B., Kim, K., Lim, K. M., Jeon, T., Seok, J., & Cho, S. G. (2019). Production of mesenchymal stem cells through stem cell reprogramming. International journal of molecular sciences, 20(8), 1922
Ardeshirylajimi, A., Soleimani, M., Hosseinkhani, S., Parivar, K., & Yaghmaei, P. (2014). A comparative study of osteogenic differentiation human induced pluripotent stem cells and adipose tissue derived mesenchymal stem cells. Cell Journal (Yakhteh), 16(3), 235
Attardi, A., Fulton, T., Florescu, M., Shah, G., Muresan, L., Lenz, M. O., Lancaster, C., Huisken, J., van Oudenaarden, A., & Steventon, B. (2018). Neuromesodermal progenitors are a conserved source of spinal cord with divergent growth dynamics. Development, 145(21).
Augustin, M. (2012). Preconditioning methods in cell therapy of the heart, Doctoral dissertation, [online] Available at: https://helda.helsinki.fi/handle/10138/36906. Accessed 15 Oct 2021.
Bernitz, J. M., & Moore, K. A. (2014). Haematopoietic Stem Cells: Uncovering the origins of a niche. eLife, 3, e05041
Bremer, S., & Hartung, T. (2004). The use of embryonic stem cells for regulatory developmental toxicity testing in vitro-the current status of test development. Current Pharmaceutical Design, 10(22), 2733–2747
Chen, K. G., Mallon, B. S., McKay, R. D., & Robey, P. G. (2014). Human pluripotent stem cell culture: considerations for maintenance, expansion, and therapeutics. Cell Stem Cell, 14(1), 13–26
ATCC Animal Cell Culture Guide. [online] Available at: https://www.atcc.org/resources/culture-guides/animal-cell-culture-guide. Accessed 15 Oct 2021.
Demirci, S., Doğan, A., Apdik, H., Tuysuz, E. C., Gulluoglu, S., Bayrak, O. F., & Şahin, F. (2018). Cytoglobin inhibits migration through PI3K/AKT/mTOR pathway in fibroblast cells. Molecular and Cellular Biochemistry, 437(1), 133–142
Demirci, S., Doğan, A., Karakuş, E., Halıcı, Z., Topçu, A., Demirci, E., & Sahin, F. (2015). Boron and poloxamer (F68 and F127) containing hydrogel formulation for burn wound healing. Biological Trace Element Research, 168(1), 169–180
Demirci, S., Doğan, A., Şişli, B., & Sahin, F. (2014). Boron increases the cell viability of mesenchymal stem cells after long-term cryopreservation. Cryobiology, 68(1), 139–146
Demirci, S., Kaya, M. S., Doğan, A., Kalay, Å, ALTIN, N. Ã, & Şahin, Y. A. R. A. T. A. (2015). Antibacterial and cytotoxic properties of boron-containing dental composite. Turkish Journal of Biology, 39(3), 417–426
Ding, G., Tanaka, Y., Hayashi, M., Nishikawa, S. I., & Kataoka, H. (2013). PDGF receptor alpha+ mesoderm contributes to endothelial and hematopoietic cells in mice. Developmental Dynamics, 242(3), 254–268
Doğan, A. (2018). Embryonic stem cells in development and regenerative medicine. Cell Biology and Translational Medicine, 1, 1–15
Doğan, A., Demirci, S., Apdik, H., Apdik, E. A., & Şahin, F. (2017). Dental pulp stem cells (DPSCs) increase prostate cancer cell proliferation and migration under in vitro conditions. Tissue and Cell, 49(6), 711–718
Doğan, A., Yalvaç, M. E., Şahin, F., Kabanov, A. V., Palotás, A., & Rizvanov, A. A. (2012). Differentiation of human stem cells is promoted by amphiphilic pluronic block copolymers. International Journal of Nanomedicine, 7, 4849
Dou, Z., Ghosh, K., Vizioli, M. G., Zhu, J., Sen, P., Wangensteen, K. J., & Zhou, Z. (2017). Cytoplasmic chromatin triggers inflammation in senescence and cancer. Nature, 550(7676), 402–406
Doyle, E. C., Wragg, N. M., & Wilson, S. L. (2020). Intraarticular injection of bone marrow-derived mesenchymal stem cells enhances regeneration in knee osteoarthritis. Knee Surgery, Sports Traumatology, Arthroscopy, 28, 3827–3842
Du, Z. W., Hu, B. Y., Ayala, M., Sauer, B., & Zhang, S. C. (2009). Cre recombination-mediated cassette exchange for building versatile transgenic human embryonic stem cells lines. Stem Cells, 27(5), 1032–1041
Eirin, A., & Lerman, L. O. (2014). Mesenchymal stem cell treatment for chronic renal failure. Stem Cell Research & Therapy, 5(4), 1–8
Farahani, R. M., & Xaymardan, M. (2015). Platelet-derived growth factor receptor alpha as a marker of mesenchymal stem cells in development and stem cell biology. Stem Cells International, 2015, 1–8
Fujiki, Y., Tao, K., Bianchi, D. W., Giel-Moloney, M., Leiter, A. B., & Johnson, K. L. (2008). Quantification of green fluorescent protein by in vivo imaging, PCR, and flow cytometry: comparison of transgenic strains and relevance for fetal cell microchimerism. Cytometry Part A: The Journal of the International Society for Analytical Cytology, 73(2), 11–118
Galipeau, J. (2013). The mesenchymal stromal cells dilemma—does a negative phase III trial of random donor mesenchymal stromal cells in steroid-resistant graft-versus-host disease represent a death knell or a bump in the road? Cytotherapy, 15(1), 2–8
Gouti, M., Tsakiridis, A., Wymeersch, F. J., Huang, Y., Kleinjung, J., Wilson, V., & Briscoe, J. (2014). In vitro generation of neuromesodermal progenitors reveals distinct roles for wnt signalling in the specification of spinal cord and paraxial mesoderm identity. PLoS Biology, 12(8), e1001937
Henrique, D., Abranches, E., Verrier, L., & Storey, K. G. (2015). Neuromesodermal progenitors and the making of the spinal cord. Development, 142(17), 2864–2875
Herberts, C. A., Kwa, M. S., & Hermsen, H. P. (2011). Risk factors in the development of stem cell therapy. Journal of Translational Medicine, 9(1), 1–14
Hirvonen, T. (2014). Glycan binding proteins in therapeutic mesenchymal stem cell research. Doctoral dissertation, [online] Available at: https://helda.helsinki.fi/handle/10138/135978. Accessed 15 Oct 2021.
Hwang, J. H., Shim, S. S., Seok, O. S., Lee, H. Y., Woo, S. K., Kim, B. H., & Park, Y. K. (2009). Comparison of cytokine expression in mesenchymal stem cells from human placenta, cord blood, and bone marrow. Journal of Korean Medical Science, 24(4), 547
Kiani, A. A., Kazemi, A., Halabian, R., Mohammadipour, M., Jahanian-Najafabadi, A., & Roudkenar, M. H. (2013). HIF-1α confers resistance to induced stress in bone marrow-derived mesenchymal stem cells. Archives of Medical Research, 44(3), 185–193
Kyurkchiev, D., Bochev, I., Ivanova-Todorova, E., Mourdjeva, M., Oreshkova, T., Belemezova, K., & Kyurkchiev, S. (2014). Secretion of immunoregulatory cytokines by mesenchymal stem cells. World Journal of Stem Cells, 6(5), 552
Ludwig, T. E., Bergendahl, V., Levenstein, M. E., Yu, J., Probasco, M. D., & Thomson, J. A. (2006). Feeder-independent culture of human embryonic stem cells. Nature Methods, 3(8), 637–646. https://doi.org/10.1038/nmeth902
Lukomska, B., Stanaszek, L., Zuba-Surma, E., Legosz, P., Sarzynska, S., & Drela, K. (2019). Challenges and controversies in human mesenchymal stem cell therapy. Stem Cells International, 2019, 1–10.
Metsalu, T., & Vilo, J. (2015). ClustVis: a web tool for visualizing clustering of multivariate data using Principal Component Analysis and heatmap. Nucleic Acids Research, 43(W1), W566–W570
Peng, K. Y., Lee, Y. W., Hsu, P. J., Wang, H. H., Wang, Y., Liou, J. Y., & Yen, B. L. (2016). Human pluripotent stem cell (PSC)-derived mesenchymal stem cells (MSCs) show potent neurogenic capacity which is enhanced with cytoskeletal rearrangement. Oncotarget, 7(28), 43949
Phinney, D. G. (2012). Functional heterogeneity of mesenchymal stem cells: implications for cell therapy. Journal of Cellular Biochemistry, 113(9), 2806–2812
Pittenger, M. F., Discher, D. E., Péault, B. M., Phinney, D. G., Hare, J. M., & Caplan, A. I. (2019). Mesenchymal stem cell perspective: cell biology to clinical progress. NPJ Regenerative Medicine, 4(1), 1–15
Pourquié, O. (2001). Vertebrate somitogenesis. Annual Review of Cell and Developmental Biology, 17(1), 311–350
Ripoll, C. B. (2010). Adult stem cell therapy in the twitcher mouse model of Krabbe’s disease utilizing mesenchymal lineage stem cells. Tulane University
Rolletschek, A., Blyszczuk, P., & Wobus, A. M. (2004). Embryonic stem cell-derived cardiac, neuronal and pancreatic cells as model systems to study toxicological effects. Toxicology Letters, 149(1–3), 361–369
Saldaña, L., Bensiamar, F., Vallés, G., Mancebo, F. J., García-Rey, E., & Vilaboa, N. (2019). Immunoregulatory potential of mesenchymal stem cells following activation by macrophage-derived soluble factors. Stem Cell Research & Therapy, 10(1), 1–15
Sarugaser, R., Hanoun, L., Keating, A., Stanford, W. L., & Davies, J. E. (2009). Human mesenchymal stem cells self-renew and differentiate according to a deterministic hierarchy. PloS One, 4(8), e6498
Sheng, G. (2015). The developmental basis of mesenchymal stem/stromal cells (MSCs). BMC Developmental Biology, 15(1), 1–8
Şişli, H. B., Hayal, T. B., Seçkin, S., Şenkal, S., Kıratlı, B., Şahin, F., & Doğan, A. (2019). Gene editing in human pluripotent stem cells: recent advances for clinical therapies. Cell Biology and Translational Medicine, 7, 17–28
Steinemann, D., Göhring, G., & Schlegelberger, B. (2013). Genetic instability of modified stem cells-a first step towards malignant transformation? American Journal of Stem Cells, 2(1), 39
Steventon, B., & Arias, A. M. (2017). Evo-engineering and the cellular and molecular origins of the vertebrate spinal cord. Developmental Biology, 432(1), 3–13
Su, W., Zhou, M., Zheng, Y., Fan, Y., Wang, L., Han, Z., & Xiang, R. (2011). Bioluminescence reporter gene imaging characterize human embryonic stem cell-derived teratoma formation. Journal of Cellular Biochemistry, 112(3), 840–848
Sweetman, D., Wagstaff, L., Cooper, O., Weijer, C., & Münsterberg, A. (2008). The migration of paraxial and lateral plate mesoderm cells emerging from the late primitive streak is controlled by different Wnt signals. BMC Developmental Biology, 8(1), 1–15
Taşlı, P. N., Doğan, A., Demirci, S., & Şahin, F. (2016). Myogenic and neurogenic differentiation of human tooth germ stem cells (hTGSCs) are regulated by pluronic block copolymers. Cytotechnology, 68(2), 319–329
Truong, M. D., Choi, B., Kim, Y., Kim, M., & Min, B. H. (2017). Granulocyte macrophage–colony stimulating factor (GM-CSF) significantly enhances articular cartilage repair potential by microfracture. Osteoarthritis and Cartilage, 25(8), 1345–1352
van Poll, D., Parekkadan, B., Rinkes, I. B., Tilles, A. W., & Yarmush, M. L. (2008). Mesenchymal stem cell therapy for protection and repair of injured vital organs. Cellular and Molecular Bioengineering, 1(1), 42–50
Vanderlaan, R. D., Oudit, G. Y., & Backx, P. H. (2003). Electrophysiological profiling of cardiomyocytes in embryonic bodies derived from human embryonic stem cells: Therapeutic implications. American Heart Association
Vodyanik, M. A., Yu, J., Zhang, X., Tian, S., Stewart, R., Thomson, J. A., & Slukvin, I. I. (2010). A mesoderm-derived precursor for mesenchymal stem and endothelial cells. Cell Stem Cell, 7(6), 718–729
Wang, H., Li, D., Zhai, Z., Zhang, X., Huang, W., Chen, X., & Zou, Z. (2019). Characterization and therapeutic application of mesenchymal stem cells with neuromesodermal origin from human pluripotent stem cells. Theranostics, 9(6), 1683
Wei, X., Yang, X., Han, Z., Qu, F., Shao, L., & Shi, Y. (2013). Mesenchymal stem cells: a new trend for cell therapy. Acta Pharmacologica Sinica, 34(6), 747–754
Xu, M., Shaw, G., Murphy, M., & Barry, F. (2019). Induced pluripotent stem cell-derived mesenchymal stromal cells are functionally and genetically different from bone marrow‐derived mesenchymal stromal cells. Stem cells, 37(6), 754–765
Yamaguchi, T. P., Dumont, D. J., Conlon, R. A., Breitman, M. L., & Rossant, J. (1993). flk-1, an flt-related receptor tyrosine kinase is an early marker for endothelial cell precursors. Development, 118(2), 489–498
Yuan, Z., Lourenco, S. D. S., Sage, E. K., Kolluri, K. K., Lowdell, M. W., & Janes, S. M. (2016). Cryopreservation of human mesenchymal stromal cells expressing TRAIL for human anti-cancer therapy. Cytotherapy, 18(7), 860–869
Zhu, Y., Zhang, P., Gu, R. L., Liu, Y. S., & Zhou, Y. S. (2018). Origin and clinical applications of neural crest-derived dental stem cells. The Chinese Journal of Dental Research, 21(2), 89–100
Acknowledgements
This study was supported by Yeditepe University and Turkish Academy of Sciences Outstanding Young Scientists Award (TÜBA-GEBİP 2020). Albert A Rizvanov was supported by KFU state assignment 0671-2020-0058.
Funding
This study was supported by Yeditepe University and Outstanding Young Scientists Award (TÜBA-GEBİP 2020). Albert A Rizvanov was supported by KFU state assignment 0671-2020-0058.
Author information
Authors and Affiliations
Contributions
Ayşegül Doğan, Fikrettin Şahin, Albert A. Rizvanov and Selinay Şenkal contributed to the study conception and design. Material preparation, data collection and analysis were performed by Taha Bartu Hayal and Selinay Şenkal. In vitro experiments were conducted by Ayşegül Doğan, Taha Bartu Hayal, Selinay Şenkal and Derya Sağraç. In vivo experiments were conducted by Hatice Burcu Şişli, Engin Sümer and Fikrettin Şahin. Flow cytometry analysis and Immunocytochemistry experiments were performed by Ayla Burçin Asutay and Binnur Kıratlı. The first draft of the manuscript was written by Ayşegül Doğan, revised by Albert A. Rizvanov and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflicts of Interest/Competing Interests
The authors have no conflicts of interest to declare that are relevant to the content of this article.
Ethics Approval
Not applicable.
Consent to Participate
Not applicable.
Consent for Publication
Not applicable.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOCX 22 kb)

Supplementary Figure 1
Characterization of NMPs. (a) T/Bra and Sox2 staining of cells at different time points (D3, D5, D8, D10 and D24). (b) T/Bra, Sox2, Wnt3, Nkx1-2 gene expression at different time points (D3, D5, D8, D10 and D24) of differentiation protocol. (c) OCT3/4, Nanog, c-MYC gene expression at different time points. *P<0.05. (PNG 5829 kb)

Supplementary Figure 2
Characterization of NMP-derived MSC population. (a) CD73 and CD45 immunostaining of cells during differentiation (b) Heat map representation of CD73 and CD45 immunostaining during MSC derivation (c) CD73, CD90 and CD105 gene expression analysis during differentiation protocol. *P<0.05. (PNG 6445 kb)

Supplementary Figure 3
Three lineage differentiation analyses of NMP-derived MSCs. Osteo-, chondro- and adipo-genic differentiation of (a) MSC-II, (b) MSC-I, (c) ASC telo s and (d) DPSCs. (PNG 15537 kb)

Supplementary Figure 4
Gene expression analyses after three lineage differentiation of NMP-derived MSCs. Osteo-, chondro- and adipo-genic differentiation related gene expression analyses of MSC II, MSC I, ASC telo and DPSCs. Osteocalcin, Aggrecan and Adiponectin gene expression were calculated. *P<0.05. (PNG 138 kb)

Supplementary Figure 5
Repeated short-term freeze-thaw cycles of MSC II cell population. (a) Experimental design of four repeated short-term freeze-thaw cycles. (b) Morphological images of selected MSC II colonies after each freeze-thaw. (c) CD73 and CD45 immunostaining of cells short-term freeze-thaw cycles (d) Viable cell number of MSC II cells after four repeated short-term freeze-thaw cycles. (e) Three lineage differentiation analyses of NMP-derived MSCs (MSC II) after short-term freeze-thaw cycles. (PNG 1153 kb)

Supplementary Figure 6
Gene expression analyses after three lineage differentiation of cryopreserved MSC II cells. Osteo-, chondro- and adipo-genic differentiation related gene expression analyses of MSC II followed by short-term and long-term cryopreservation analyses. Osteocalcin, Aggrecan and Adiponectin gene expression were calculated. *P<0.05. (PNG 141 kb)

Supplementary Figure 7
Characterization of MSC II cells after long-term cryopreservation. (a) Crystal violet staining and morphological analyses. (b) Diameter and (c) Number of MSC II cell colonies after long-term cryopreservation. (d) Viable cell number of MSC II cells after long-term cryopreservation (e) CD73 and CD45 immunostaining of cells after long-term cryopreservation (f) Three lineage differentiation analyses of NMP-derived MSCs (MSC II) after long-term cryopreservation. (PNG 22023 kb)

Supplementary Figure 8
Immunocytochemistry analyses of (a) FLK-1 and (b) PDGFRα during differentiation protocol. (PNG 1714 kb)

Supplementary Figure 9
Heat map representation of (a) FLK-1 and PDGFRα, (b) PECAM1, VE-Cadherin, VCAM-1 and VEGF immunostaining during NMP-derived MSC derivation. (PNG 59 kb)

Supplementary Figure. 10
Immunocytochemistry analyses of VE-Cadherin and VCAM-1 during NMP-derived MSC derivation. (PNG 6186 kb)

Supplementary Figure 11
Immunocytochemistry analyses of PECAM1 (CD31) and VEGF immunostaining during MSC derivation. (PNG 5033 kb)

Supplementary Figure 12
Protein membrane array analysis of differentiated cells (a) Cytokine, Growth Factor and Angiogenesis arrays of cells at different time points of the differentiation protocol. (b) Selected differentially expressed proteins Cytokine, Growth Factor and Angiogenesis arrays. (PNG 3566 kb)

Supplementary Figure 13
Flow cytometry analyses of GFP+ differentiated cells in various tissues and percentage of tissue distribution during differentiation. (PNG 2558 kb)
Rights and permissions
About this article
Cite this article
Şenkal, S., Hayal, T.B., Sağraç, D. et al. Human ESC-derived Neuromesodermal Progenitors (NMPs) Successfully Differentiate into Mesenchymal Stem Cells (MSCs). Stem Cell Rev and Rep 18, 278–293 (2022). https://doi.org/10.1007/s12015-021-10281-0
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12015-021-10281-0