Abstract
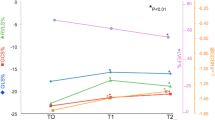
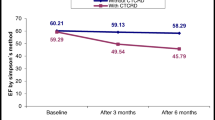
Angiogenesis inhibitor Bevacizumab (BVZ) may lead to the development of adverse effects, including hypertension and cardiac ischemia. Whether assessment of changes in myocardial strain by two-dimensional speckle-tracking echocardiography (2D-STE) can be of value in detecting BVZ-mediated cardiotoxicity at an earlier stage is not known. We investigated whether 2D-STE can non-invasively detect early evidence of cardiotoxicity in metastatic colorectal cancer (mCRC) patients treated with BVZ. Between January and June 2019, 25 consecutive patients (71.8 ± 7.5 year/old, 17 males) with mCRC were prospectively enrolled. Patients underwent physical examination, blood tests, and conventional 2D-transthoracic echocardiography implemented with 2D-STE analysis, at baseline and at 3 and 6 months following treatment with BVZ (15 mg/kg every 15 days) + 5-fluorouracil/folinic acid plus oxaliplatin (FOLFOX i.v.). At 6-month follow-up, we assessed occurrence of global longitudinal strain (GLS) impairment (> 15% decrease in GLS compared with baseline) as primary end-point and a new-onset systemic hypertension (secondary end-point). On average, GLS showed a progressive significant impairment after BVZ, from − 17.4 ± 3.2% at baseline to − 16 ± 2.9% (p = 0.003) at 6-month follow-up; > 15% decrease in GLS (primary end-point) was detected in 9 patients (36%). All other strain parameters remained unchanged. New-onset systemic hypertension (secondary end-point) was diagnosed in five patients (20%). No significant changes were observed in serial high-sensitivity cardiac troponin I measurements. No patient developed significant changes in LV size or LV ejection fraction; no case of clinically symptomatic HF was observed during BVZ-treatment. Measurement of GLS by 2D-STE analysis can effectively detect BVZ-mediated cardiotoxicity at an early stage.


Similar content being viewed by others
Abbreviations
- 2D:
-
Two-dimensional
- AFI:
-
Automated function imaging
- AUC:
-
Area under the curve
- AVC:
-
Aortic valve closure
- BP:
-
Blood pressure
- BSA:
-
Body surface area
- BVZ:
-
Bevacizumab
- CI:
-
Confidence interval
- CRP:
-
C-reactive protein
- CTRCD:
-
Cancer therapeutics-related cardiac dysfunction
- DBP:
-
Diastolic blood pressure
- ECG:
-
Electrocardiogram
- GCS:
-
Global circumferential strain
- GCSR:
-
Global circumferential strain rate
- GLS:
-
Global longitudinal strain
- GLSR:
-
Global longitudinal strain rate
- GRS:
-
Global radial strain
- GRSR:
-
Global radial strain rate
- GSR+ :
-
First positive global strain rate
- GSRE:
-
Global early-diastolic strain rate
- GSRL:
-
Global late-diastolic strain rate
- HF:
-
Heart failure
- HR:
-
Heart rate
- HS-cTnl:
-
High-sensitivity cardiac troponin I
- ICC:
-
Intraclass correlation coefficient
- LA:
-
Left atrial
- LV:
-
Left ventricular
- LVEF:
-
Left ventricular ejection fraction
- LVFP:
-
Left ventricular filling pressures
- mCRC:
-
Metastatic colorectal cancer
- ROI:
-
Region of interest
- SBP:
-
Systolic blood pressure
- SD:
-
Standard deviation
- SR:
-
Strain rate
- STE:
-
Speckle-tracking echocardiography
- TnI:
-
Troponin I
- TnT:
-
Troponin T
- TTE:
-
Transthoracic echocardiography
- VEGF:
-
Vascular endothelial growth factor
- VEGF-i:
-
Vascular endothelial growth factor inhibitors
References
Fernando, N. H., & Hurwitz, H. I. (2003). Inhibition of vascular endothelial growth factor in the treatment of colorectal cancer. Seminars in Oncology, 30(3 Suppl 6), 39–50.
Jain, R. K. (2001). Normalizing tumor vasculature with anti-angiogenic therapy: a new paradigm for combination therapy. Nature Medicine, 7, 987–989.
Folkman, J. (2007). Angiogenesis: An organizing principle for drug discovery? Nature Reviews Drug Discovery, 6, 273–286.
Ferrara, N., Hillan, K. J., & Novotny, W. (2005). Bevacizumab (Avastin), a humanized anti-VEGF monoclonal antibody for cancer therapy. Biochemical and Biophysical Research Communications, 333, 328–335.
Hurwitz, H., Fehrenbacher, L., Novotny, W., Cartwright, T., Hainsworth, J., Heim, W., et al. (2004). Bevacizumab plus irinotecan, fluorouracil, and leucovorin for metastatic colorectal cancer. New England Journal of Medicine, 350, 2335–2342.
Giantonio, B. J., Catalano, P. J., Meropol, N. J., O’Dwyer, P. J., Mitchell, E. P., Alberts, S. R., et al. (2007). Bevacizumab in combination with oxaliplatin, fluorouracil, and leucovorin (FOLFOX4) for previously treated metastatic colorectal cancer: Results from the Eastern Cooperative Oncology Group Study E3200. Journal of Clinical Oncology, 25, 1539–1544.
Hall, P. S., Harshman, L. C., Srinivas, S., & Witteles, R. M. (2013). The frequency and severity of cardiovascular toxicity from targeted therapy in advanced renal cell carcinoma patients. Journal of the American College of Cardiology: Heart Failure, 1, 72–78.
Economopoulou, P., Kotsakis, A., Kapiris, I., & Kentepozidis, N. (2015). Cancer therapy and cardiovascular risk: Focus on bevacizumab. Cancer Management and Research, 7, 133–143.
Abdel-Qadir, H., Ethier, J. L., Lee, D. S., Thavendiranathan, P., & Amir, E. (2017). Cardiovascular toxicity of angiogenesis inhibitors in treatment of malignancy: A systematic review and meta-analysis. Cancer Treatment Reviews, 53, 120–127.
Ewer, M. S., & Lenihan, D. J. (2008). Left ventricular ejection fraction and cardiotoxicity: Is our ear really to the ground? Journal of Clinical Oncology, 26, 1201–1203.
Cardinale, D., Salvatici, M., & Sandri, M. T. (2011). Role of biomarkers in cardioncology. Clinical Chemistry and Laboratory Medicine, 49, 1937–1948.
Ducas, R., Tsang, W., Chong, A. A., Jassal, D. S., Lang, R. M., Leong-Poi, H., et al. (2013). Echocardiography and vascular ultrasound: New developments and future directions. Canadian Journal of Cardiology, 29, 304–316.
Fallah-Rad, N., Walker, J. R., Wassef, A., Lytwyn, M., Bohonis, S., Fang, T., et al. (2011). The utility of cardiac biomarkers, tissue velocity and strain imaging, and cardiac magnetic resonance imaging in predicting early left ventricular dysfunction in patients with human epidermal growth factor receptor ii-positive breast cancer treated with adjuvant trastuzumab therapy. Journal of the American College of Cardiology, 57, 2263–2270.
Di Lisi, D., Bonura, F., Macaione, F., Cuttitta, F., Peritore, A., Meschisi, M., et al. (2011). Novo G, D’Alessandro N, Novo S. Chemotherapy-induced cardiotoxicity: Role of the conventional echocardiography and the tissue Doppler. Minerva Cardioangiologica, 59, 301–308.
Albini, A., Pennesi, G., Donatelli, F., Cammarota, R., De Flora, S., & Noonan, D. M. (2010). Cardiotoxicity of anticancer drugs: The need for cardio-oncology and cardio-oncological prevention. Journal of the National Cancer Institute, 102, 14–25.
Ho, E., Brown, A., Barrett, P., Morgan, R. B., King, G., Kennedy, M. J., et al. (2010). Subclinical anthracycline- and trastuzumab-induced cardiotoxicity in the long-term follow-up of asymptomatic breast cancer survivors: A speckle tracking echocardiographic study. Heart, 96, 701–707.
Sawaya, H., Sebag, I. A., Plana, J. C., Januzzi, J. L., Ky, B., Cohen, V., et al. (2011). Early detection and prediction of cardiotoxicity in chemotherapy-treated patients. American Journal of Cardiology, 107, 1375–1380.
Thavendiranathan, P., Poulin, F., Lim, K. D., Plana, J. C., Woo, A., & Marwick, T. H. (2014). Use of myocardial strain imaging by echocardiography for the early detection of cardiotoxicity in patients during and after cancer chemotherapy: A systematic review. Journal of the American College of Cardiology, 63(25 Pt A), 2751–2768.
Plana, J. C., Galderisi, M., Barac, A., Ewer, M. S., Ky, B., Scherrer-Crosbie, M., et al. (2014). Expert consensus for multimodality imaging evaluation of adult patients during and after cancer therapy: A report from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. Journal of the American Society of Echocardiography, 27, 911–939.
Nhola, L. F., Abdelmoneim, S. S., Villarraga, H. R., Kohli, M., Grothey, A., Bordun, K. A., et al. (2019). Echocardiographic assessment for the detection of cardiotoxicity due to vascular endothelial growth factor inhibitor therapy in metastatic renal cell and colorectal cancers. Journal of the American Society of Echocardiography, 32, 267–276.
Ponikowski, P., Voors, A. A., Anker, S. D., Bueno, H., Cleland, J. G., Coats, A. J., et al. (2016). 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: The Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC). Developed with the special contribution of the Heart Failure Association (HFA) of the ESC. European Journal of Heart Failure, 18, 891–975.
Lang, R. M., Badano, L. P., Mor-Avi, V., Afilalo, J., Armstrong, A., Ernande, L., et al. (2015). Recommendations for cardiac chamber quantification by echocardiography in adults: An update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. Journal of the American Society of Echocardiography, 28, 1–39.
Nagueh, S. F., Smiseth, O. A., Appleton, C. P., Byrd, B. F., 3rd, Dokainish, H., Edvardsen, T., et al. (2016). Recommendations for the evaluation of left ventricular diastolic function by echocardiography: An update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. Journal of the American Society of Echocardiography, 29, 277–314.
Medvedofsky, D., Kebed, K., Laffin, L., Stone, J., Addetia, K., Lang, R. M., et al. (2017). Reproducibility and experience dependence of echocardiographic indices of left ventricular function: Side-by-side comparison of global longitudinal strain and ejection fraction. Echocardiography, 34, 365–370.
Duchateau, N., Loncaric, F., Cikes, M., Doltra, A., Sitges, M., & Bijnens, B. (2020). Variability in the assessment of myocardial strain patterns: Implications for adequate interpretation. Ultrasound in Medicine and Biology, 46, 244–254.
Chobanian, A. V., Bakris, G. L., Black, H. R., Cushman, W. C., Green, L. A., Izzo, J. L., Jr., et al. (2003). Seventh report of the Joint National Committee on prevention, detection, evaluation, and treatment of high blood pressure. Hypertension, 42, 1206–1252.
Nada, A., Gintant, G. A., Kleiman, R., Gutstein, D. E., Gottfridsson, C., Michelson, E. L., et al. (2013). The evaluation and management of drug effects on cardiac conduction (PR and QRS intervals) in clinical development. American Heart Journal, 165, 489–500.
Pathan, F., D’Elia, N., Nolan, M. T., Marwick, T. H., & Negishi, K. (2017). Normal ranges of left atrial strain by speckle-tracking echocardiography: A systematic review and meta-analysis. Journal of the American Society of Echocardiography, 30, 59–70.
Sugimoto, T., Dulgheru, R., Bernard, A., Ilardi, F., Contu, L., Addetia, K., et al. (2017). Echocardiographic reference ranges for normal left ventricular 2D strain: Results from the EACVI NORRE study. European Heart Journal—Cardiovascular Imaging, 18, 833–840.
Scartozzi, M., Galizia, E., Chiorrini, S., Giampieri, R., Berardi, R., Pierantoni, C., et al. (2009). Arterial hypertension correlates with clinical outcome in colorectal cancer patients treated with first-line bevacizumab. Annals of Oncology, 20, 227–230.
Vaklavas, C., Lenihan, D., Kurzrock, R., & Tsimberidou, A. M. (2010). Anti-vascular endothelial growth factor therapies and cardiovascular toxicity: What are the important clinical markers to target? The Oncologist, 15, 130–141.
Tocchetti, C. G., Gallucci, G., Coppola, C., Piscopo, G., Cipresso, C., Maurea, C., et al. (2013). The emerging issue of cardiac dysfunction induced by antineoplastic angiogenesis inhibitors. European Journal of Heart Failure, 15, 482–489.
Groarke, J. D., Choueiri, T. K., Slosky, D., Cheng, S., & Moslehi, J. (2014). Recognizing and managing left ventricular dysfunction associated with therapeutic inhibition of the vascular endothelial growth factor signaling pathway. Current Treatment Options in Cardiovascular Medicine, 16, 335.
Totzeck, M., Mincu, R. I., & Rassaf, T. (2017). Cardiovascular adverse events in patients with cancer treated with bevacizumab: A meta-analysis of more than 20,000 patients. Journal of the American Heart Association. https://doi.org/10.1161/JAHA.117.006278.
Touyz, R. M., & Herrmann, J. (2018). Cardiotoxicity with vascular endothelial growth factor inhibitor therapy. Nature Partner Journals Precision Oncology, 2, 13.
Chen, C. T., Yamaguchi, H., Lee, H. J., Du, Y., Lee, H. H., Xia, W., et al. (2011). Dual targeting of tumor angiogenesis and chemotherapy by endostatincytosine deaminase-uracil phosphoribosyltransferase. Molecular Cancer Therapeutics, 10, 1327–1336.
Chu, T. F., Rupnick, M. A., Kerkela, R., Dallabrida, S. M., Zurakowski, D., Nguyen, L., et al. (2007). Cardiotoxicity associated with tyrosine kinase inhibitor sunitinib. Lancet, 370, 2011–2019.
Hasinoff, B. B., Patel, D., & O’Hara, K. A. (2008). Mechanisms of myocyte cytotoxicity induced by the multiple receptor tyrosine kinase inhibitor sunitinib. Molecular Pharmacology, 74, 1722–1728.
Alexander, J., Dainiak, N., Berger, H. J., Goldman, L., Johnstone, D., Reduto, L., et al. (1979). Serial assessment of doxorubicin cardiotoxicity with quantitative radionuclide angiocardiography. New England Journal of Medicine, 300, 278–283.
Walker, J., Bhullar, N., Fallah-Rad, N., Lytwyn, M., Golian, M., Fang, T., et al. (2010). Role of three-dimensional echocardiography in breast cancer: Comparison with two-dimensional echocardiography, multiple-gated acquisition scans, and cardiac magnetic resonance imaging. Journal of Clinical Oncology, 28, 3429–3436.
Meinardi, M. T., van der Graaf, W. T., van Veldhuisen, D. J., Gietema, J. A., de Vries, E. G., & Sleijfer, D. T. (1999). Detection of anthracycline-induced cardiotoxicity. Cancer Treatment Reviews, 25, 237–247.
Nousiainen, T., Vanninen, E., Jantunen, E., Puustinen, J., Remes, J., Rantala, A., et al. (2001). Comparison of echocardiography and radionuclide ventriculography in the follow-up of left ventricular systolic function in adult lymphoma patients during doxorubicin therapy. Journal of Internal Medicine, 249, 297–303.
Villani, F., Meazza, R., & Materazzo, C. (2006). Non-invasive monitoring of cardiac hemodynamic parameters in doxorubicin-treated patients: Comparison with echocardiography. Anticancer Research, 26, 797–801.
Coiro, S., Huttin, O., Bozec, E., Selton-Suty, C., Lamiral, Z., Carluccio, E., et al. (2019). Reproducibility of echocardiographic assessment of 2D-derived longitudinal strain parameters in a population-based study (the STANISLAS Cohort study). International Journal of Cardiovascular Imaging, 33, 1361–1369.
Mignot, A., Donal, E., Zaroui, A., Reant, P., Salem, A., Hamon, C., et al. (2010). Global longitudinal strain as a major predictor of cardiac events in patients with depressed left ventricular function: A multicenter study. Journal of the American Society of Echocardiography, 23, 1019–1024.
Bertini, M., Ng, A. C. T., Antoni, M. L., Nucifora, G., Ewe, S. H., Auger, D., et al. (2012). Global longitudinal strain predicts long-term survival in patients with chronic ischemic cardiomyopathy. Circulation Cardiovascular Imaging, 5, 383–391.
Koene, R. J., Prizment, A. E., Blaes, A., & Konety, S. H. (2016). Shared risk factors in cardiovascular disease and cancer. Circulation, 133, 1104–1114.
Meijers, W. C., & de Boer, R. A. (2019). Common risk factors for heart failure and cancer. Cardiovascular Research, 115, 844–853.
de Boer, R. A., Meijers, W. C., van der Meer, P., & van Veldhuisen, D. J. (2019). Cancer and heart disease: Associations and relations. European Journal of Heart Failure. https://doi.org/10.1002/ejhf.1539.
Anker, M. S., Ebner, N., Hildebrandt, B., Springer, J., Sinn, M., Riess, H., et al. (2016). Resting heart rate is an independent predictor of death in patients with colorectal, pancreatic, and non-small cell lung cancer: Results of a prospective cardiovascular long-term study. European Journal of Heart Failure, 18, 1524–1534.
Lee, D. H., Park, S., Lim, S. M., Lee, M. K., Giovannucci, E. L., Kim, J. H., et al. (2016). Resting heart rate as a prognostic factor for mortality in patients with breast cancer. Breast Cancer Research and Treatment, 159, 375–384.
Park, J., Kim, J. H., Park, Y., Park, S. J., Cheon, J. H., Kim, W. H., et al. (2018). Resting heart rate is an independent predictor of advanced colorectal adenoma recurrence. PLoS ONE, 13, e0193753.
Curwen, J. O., Musgrove, H. L., Kendrew, J., Richmond, G. H., Ogilvie, D. J., & Wedge, S. R. (2008). Inhibition of vascular endothelial growth factor-a signaling induces hypertension: Examining the effect of cediranib (recentin; AZD2171) treatment on blood pressure in rat and the use of concomitant antihypertensive therapy. Clinical Cancer Research, 14, 3124–3131.
Kappers, M. H., van Esch, J. H., Sluiter, W., Sleijfer, S., Danser, A. H., & van den Meiracker, A. H. (2010). Hypertension induced by the tyrosine kinase inhibitor sunitinib is associated with increased circulating endothelin-1 levels. Hypertension, 56, 675–681.
Ranieri, G., Patruno, R., Ruggieri, E., Montemurro, S., Valerio, P., & Ribatti, D. (2006). Vascular endothelial growth factor (VEGF) as a target of bevacizumab in cancer: From the biology to the clinic. Current Medicinal Chemistry, 13, 1845–1857.
Brinda, B. J., Viganego, F., Vo, T., Dolan, D., & Fradley, M. G. (2016). Anti-VEGF-induced hypertension: A review of pathophysiology and treatment options. Current Treatment Options in Cardiovascular Medicine, 18(5), 33.
Hayman, S. R., Leung, N., Grande, J. P., & Garovic, V. D. (2012). VEGF inhibition, hypertension, and renal toxicity. Current Oncology Reports, 14, 285–294.
Belcik, J. T., Qi, Y., Kaufmann, B. A., Xie, A., Bullens, S., Morgan, T. K., et al. (2012). Cardiovascular and systemic microvascular effects of anti-vascular endothelial grown factor therapy for cancer. Journal of the American College of Cardiology, 60, 618–625.
Coutinho Cruz, M., Moura Branco, L., Portugal, G., Galrinho, A., Timóteo, A. T., Rio, P., et al. (2019). Three-dimensional speckle-tracking echocardiography for the global and regional assessments of left ventricle myocardial deformation in breast cancer patients treated with anthracyclines. Clinical Research in Cardiology. https://doi.org/10.1007/s00392-019-01556-1.
Acknowledgements
This work has been supported by Italian Ministry of Health Ricerca Corrente - IRCCS MultiMedica.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethics Approval and Consent to Participate
All procedures were in accordance with the ethical standards of our Institutional Research Committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. A written informed consent was obtained from all patients, and the protocol was approved by the Independent Ethical Committee IRCCS MultiMedica (Committee’s reference number CE 98.2019).
Consent for Publication
Not applicable.
Additional information
Handling Editor: Vera Costa.
Electronic supplementary material
Below is the link to the electronic supplementary material.

12012_2020_9583_MOESM1_ESM.jpg
Supplementary material 1 (JPG 1418 kb) Supplemental table. Intra- and interobserver variability analysis of the main conventional and functional echocardiographic parameters, measured in a subgroup of ten patients, randomly selected. GCS, global circumferential strain. GLS, global longitudinal strain. GSA+, positive global atrial strain. ICC, intraclass correlation coefficient. LVEF, left ventricular ejection fraction. LVMi, left ventricular mass indexed.
Rights and permissions
About this article
Cite this article
Sonaglioni, A., Albini, A., Fossile, E. et al. Speckle-Tracking Echocardiography for Cardioncological Evaluation in Bevacizumab-Treated Colorectal Cancer Patients. Cardiovasc Toxicol 20, 581–592 (2020). https://doi.org/10.1007/s12012-020-09583-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12012-020-09583-5