Abstract
Purpose of review
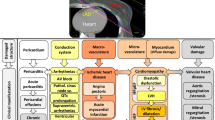
Ionizing radiation is a highly effective treatment for a wide range of malignancies, yet the cardiovascular (CV) toxicity that can result from chest radiotherapy impairs the long-term health of cancer survivors and can be a limiting factor for its use. Despite over 100 years of successful clinical use, the mechanisms by which high-energy photons damage critical components within cells of the heart’s myocardium, pericardium, vasculature, and valves remain unclear.
Recent findings
Recent studies exploring the acute and chronic effects of radiation therapy on cardiac and vascular tissue have provided new insights into the development and progression of heart disease, including the identification and understanding of age- and complication-associated risk factors. However, key questions relating to the connection from upstream signaling to fibrotic changes remain. In addition, advances in the delivery of chest radiotherapy have helped to limit heart exposure and damage, but additional refinements to delivery techniques and cardioprotective therapeutics are absolutely necessary to reduce patient mortality and morbidity.
Summary
Radiation therapy (RT)-driven CV toxicity remains a major issue for cancer survivors and more research is needed to define the precise mechanisms of toxicity. However, recent findings provide meaningful insights that may help improve patient outcomes.

Similar content being viewed by others
References and Recommended Reading
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
De Rose F, Franceschini D, Reggiori G, Stravato A, Navarria P, Ascolese AM, et al. Organs at risk in lung SBRT. Medica: Phys; 2017.
Gujral DM, Lloyd G, Bhattacharyya S. Radiation-induced valvular heart disease. Heart. 2016;102:269–76.
Zheng HC, Onderko L, Francis SA. Cardiovascular risk in survivors of cancer. Curr Cardiol. Rep. 2017.
Gernaat SAM, Ho PJ, Rijnberg N, Emaus MJ, Baak LM, Hartman M, et al. Risk of death from cardiovascular disease following breast cancer: a systematic review. Breast Cancer Res Treat. 2017;164:537–55.
McGale P, Darby SC, Hall P, Adolfsson J, Bengtsson NO, Bennet AM, et al. Incidence of heart disease in 35,000 women treated with radiotherapy for breast cancer in Denmark and Sweden. Radiother Oncol. 2011;100:167–75.
Raghunathan D, Khilji MI, Hassan SA, Yusuf SW. Radiation-induced cardiovascular disease. Curr. Atheroscler. Rep. Current Atherosclerosis Reports; 2017;19.
Hudson MM, Ness KK, Gurney JG, Mulrooney DA, Chemaitilly W, Krull KR, et al. Clinical ascertainment of health outcomes among adults treated for childhood cancer. JAMA. 2013;309:2371.
•• Fidler MM, Reulen RC, Henson K, Kelly J, Cutter D, Levitt GA, et al. Population-based long-term cardiac-specific mortality among 34,489 five-year survivors of childhood cancer in Great Britain. Circulation. 2017. Highlights the importance of monitoring cardiac diseases in survivors of childhood cancer, and suggests that recent initiatives to reduce cardiotoxicity may have a measurable impact.
• Boerma M, Sridharan V, Mao X-W, Nelson GA, Cheema AK, Koturbash I, et al. Effects of ionizing radiation on the heart. Mutat Res. 2016;770:319–27. Describes acute and late radiation-induced cardiovascular toxicities, as well as epidemiology for clinical and non-clinical radiation exposure situations.
Lipshultz SE, Franco VI, Miller TL, Colan SD, Sallan SE. Cardiovascular disease in adult survivors of childhood cancer. Annu Rev Med. 2015;66:161–76.
Lipshultz SE, Cochran TR, Franco VI, Miller TL. Treatment-related cardiotoxicity in survivors of childhood cancer. Nat Rev Clin Oncol Nature Publishing Group. 2013;10:697–710.
Hutchins KK, Siddeek H, Franco VI, Lipshultz SE. Prevention of cardiotoxicity among survivors of childhood cancer. Br J Clin Pharmacol. 2017. p. 455–65.
Bhattacharya S, Asaithamby A. Ionizing radiation and heart risks. Semin Cell Dev Biol. 2016. p. 14–25.
Tapio S. Pathology and biology of radiation-induced cardiac disease. J. Radiat. Res. 2016;57:439–48.
Hughson RL, Helm A, Durante M. Heart in space: effect of the extraterrestrial environment on the cardiovascular system. Nat Rev Cardiol 2017;
Taunk NK, Haffty BG, Kostis JB, Goyal S. Radiation-induced heart disease: pathologic abnormalities and putative mechanisms. Front Oncol 2015;5.
Brosius FC, Waller BF, Roberts WC. Radiation heart disease. Analysis of 16 young (aged 15 to 33 years) necropsy patients who received over 3500 rads to the heart. Am J Med. 1981;70:519–30.
Finet JE. Management of heart failure in cancer patients and cancer survivors. Heart Fail Clin 2017. p. 253–88.
Groarke JD, Tanguturi VK, Hainer J, Klein J, Moslehi JJ, Ng A, et al. Abnormal exercise response in long-term survivors of Hodgkin lymphoma treated with thoracic irradiation: evidence of cardiac autonomic dysfunction and impact on outcomes. J Am Coll Cardiol. 2015;65:573–83.
Nielsen KM, Offersen BV, Nielsen HM, Vaage-Nilsen M, Yusuf SW. Short and long term radiation induced cardiovascular disease in patients with cancer. Clin Cardiol. 2017. p. 255–61.
Eriksson D, Stigbrand T. Radiation-induced cell death mechanisms. Tumor Biol. 2010;31:363–72.
Kaina B. DNA damage-triggered apoptosis: critical role of DNA repair, double-strand breaks, cell proliferation and signaling. Biochem. Pharmacol. 2003;66:1547–54.
Lee C-L, Moding EJ, Cuneo KC, Li Y, Sullivan JM, Mao L, et al. p53 functions in endothelial cells to prevent radiation-induced myocardial injury in mice. Sci Signal. 2012;5:ra52.
Sarosiek KA, Ni Chonghaile T, Letai A. Mitochondria: gatekeepers of response to chemotherapy. Trends Cell Biol. Elsevier Ltd. 2013;23:612–9.
Willers H, Held KD. Introduction to clinical radiation biology. Hematol Oncol Clin North Am. 2006. p. 1–24.
Bergonié J, Tribondeau L. De Quelques Résultats de la Radiotherapie et Essai de Fixation d’une Technique Rationnelle. Comptes Rendus des Séances l’Académie des Sci. 1906;143:983–5.
Jaworski C, Mariani JA, Wheeler G, Kaye DM. Cardiac complications of thoracic irradiation. J Am Coll Cardiol. 2013;61:2319–28.
Bergmann O, Bhardwaj RD, Bernard S, Zdunek S, Barnabé-Heider F, Walsh S, et al. Evidence for cardiomyocyte renewal in humans. Science (80-.). 2009;324:98–102.
Tzahor E, Poss KD. Cardiac regeneration strategies: staying young at heart. Science (80-.). 2017;356:1035 LP–1039.
Yarnold J, Vozenin Brotons MC. Pathogenetic mechanisms in radiation fibrosis. Radiother Oncol. 2010. p. 149–61.
Sherman ML, Datta R, Hallahan DE, Weichselbaum RR, Kufe DW. Ionizing radiation regulates expression of the c-jun protooncogene. Proc Natl Acad Sci U. S. A. 1990;87:5663–6.
Kara M, Özçağlı E, Jannuzzi AT, Alpertunga B. Oxidative stress mediated cardiac apoptosis. J Fac Pharm Istanbul Univ. 2015;45:217–32.
Firsanov D, Vasilishina A, Kropotov A, Mikhailov V. Dynamics of γh2AX formation and elimination in mammalian cells after X-irradiation. Biochimie. 2012;94:2416–22.
Salata C, Ferreira-Machado SC, De Andrade CBV, Mencalha AL, Mandarim-De-Lacerda CA, de Almeida CE. Apoptosis induction of cardiomyocytes and subsequent fibrosis after irradiation and neoadjuvant chemotherapy. Int J Radiat Biol. 2014;90:284–90.
Sarosiek KA, Chi X, Bachman JA, Sims JJ, Montero J, Patel L, et al. BID Preferentially activates BAK while BIM preferentially activates BAX, affecting chemotherapy response. Mol Cell. 2013;51:751–65.
Mitchel REJ, Hasu M, Bugden M, Wyatt H, Hildebrandt G, Chen Y-X, et al. Low-dose radiation exposure and protection against atherosclerosis in ApoE(−/−) mice: the influence of P53 heterozygosity. Radiat Res. 2013;179:190–9.
• Sarosiek KA, Fraser C, Muthalagu N, Bhola PD, Chang W, McBrayer SK, et al. Developmental regulation of mitochondrial apoptosis by c-Myc governs age- and tissue-specific sensitivity to cancer therapeutics. Cancer Cell. Elsevier Inc. 2017;31:142–56. Introduces the concept of developmental regulation of apoptosis as a component of the treatment-associated toxicities observed in pediatric patients.
Darby SC, Ewertz M, McGale P, Bennet AM, Blom-Goldman U, Brønnum D, et al. Risk of ischemic heart disease in women after radiotherapy for breast cancer. N Engl J Med. 2013;368:987–98.
• De Ruysscher D, Faivre-Finn C, Moeller D, Nestle U, Hurkmans CW, Le Péchoux C, et al. European Organization for Research and Treatment of Cancer (EORTC) recommendations for planning and delivery of high-dose, high precision radiotherapy for lung cancer. Radiother Oncol. 2017;124:1–10. Comprehensive guidelines for the planning of lung cancer radiotherapy, in terms of both target volume and organs at risk.
Gagliardi G, Lax I, Ottolenghi A, Rutqvist LE. Long-term cardiac mortality after radiotherapy of breast cancer—application of the relative seriality model. Br J Radiol. 1996;69:839–46.
Pollock S, Keall R, Keall P. Breathing guidance in radiation oncology and radiology: a systematic review of patient and healthy volunteer studies. Med Phys. 2015;42:5490–509.
Lymberis SC, De Wyngaert JK, Parhar P, Chhabra AM, Fenton-Kerimian M, Chang J, et al. Prospective assessment of optimal individual position (prone versus supine) for breast radiotherapy: volumetric and dosimetric correlations in 100 patients. Int J Radiat Oncol Biol Phys. 2012;84:902–9.
Sung KH, Choi YE, Lee KC. Cardiac risk index as a simple geometric indicator to select patients for the heart-sparing radiotherapy of left-sided breast cancer. J Med Imaging Radiat Oncol. 2017;61:410–7.
• Nona Duma M, Herr A-C, Borm KJ, Trott KR, Molls M, Oechsner M, et al. Tangential field radiotherapy for breast cancer—the dose to the heart and heart subvolumes: what structures must be contoured in future clinical trials? Front Oncol. 2017;7:130. Highlights the importance of heart substructure-specific contouring in RT planning, especially considering late toxicities.
Hedin E, Bäck A, Chakarova R. Impact of lung density on the lung dose estimation for radiotherapy of breast cancer. Phys. Imaging Radiat. Oncol. 2017;3:5–10.
Hoppe BS, Flampouri S, Su Z, Latif N, Dang NH, Lynch J, et al. Effective dose reduction to cardiac structures using protons compared with 3DCRT and IMRT in mediastinal Hodgkin lymphoma. Int. J. Radiat. Oncol. Biol. Phys. 2012;84:449–55.
Vogel J, Lin L, Simone CB, Berman AT. Risk of major cardiac events following adjuvant proton versus photon radiation therapy for patients with thymic malignancies. Acta Oncol. (Madr). 2017;56:1060–4.
Amino M, Yoshioka K, Shima M, Okada T, Nakajima M, Furusawa Y, et al. Changes in arrhythmogenic properties and five-year prognosis after carbon-ion radiotherapy in patients with mediastinum cancer. Ann Noninvasive Electrocardiol. 2017;1–13.
Stick LB, Yu J, Maraldo MV, Aznar MC, Pedersen AN, Bentzen SM, et al. Joint estimation of cardiac toxicity and recurrence risks after comprehensive nodal photon versus proton therapy for breast cancer. Int J Radiat Oncol Biol Phys Elsevier Inc. 2017;97:754–61.
Wu S, Tao L, Wang J, Xu Z, Wang J, Xue Y, et al. Amifostine pretreatment attenuates myocardial ischemia/reperfusion injury by inhibiting apoptosis and oxidative stress. Oxid Med Cell Longev. 2017;2017:1–12.
De Freitas RB, Boligon AA, Rovani BT, Piana M, De Brum TF, Da Silva JR, et al. Effect of black grape juice against heart damage from acute gamma TBI in rats. Molecules. 2013;18:12154–67.
Qian L, Cao F, Cui J, Wang Y, Huang Y, Chuai Y, et al. The potential cardioprotective effects of hydrogen in irradiated mice. J Radiat Res. 2010;51:741–7.
Fan Z, Han Y, Ye Y, Liu C, Cai H. L-carnitine preserves cardiac function by activating p38 MAPK/Nrf2 signaling in hearts exposed to irradiation. Eur. J. Pharmacol. 2017;804:7–12.
Zhang W, Li Y, Li R, Wang Y, Zhu M, Wang B, et al. Sodium tanshinone IIA sulfonate prevents radiation-induced toxicity in H9c2 ardiomyocytes. Evidence-based Complement Altern Med 2017;2017.
Zhang ZY, Li Y, Li R, Zhang AA, Shang B, Yu J, et al. Tetrahydrobiopterin protects against radiation-induced growth inhibition in H9c2 cardiomyocytes. Chin. Med. J. (Engl). 2016;129:2733–40.
Galano A, Tan DX, Reiter RJ. Melatonin as a natural ally against oxidative stress: a physicochemical examination. J. Pineal Res. 2011. p. 1–16.
Elitok A, Oz F, Ahmet Y, Kilic L, Ciftci R, Sen F, et al. Effect of carvedilol on silent anthracycline-induced cardiotoxicity assessed by strain imaging: a prospective randomized controlled study with six-month follow-up. Cardiol J. 2014;21:509–15.
Panel M, Ghaleh B, Morin D. Targeting mitochondrial permeability as a pharmacological cardioprotective strategy. Med Res Arch. 2017;5
Frankenreiter S, Bednarczyk P, Kniess A, Bork N, Straubinger J, Koprowski P, et al. cGMP-elevating compounds and ischemic conditioning provide cardioprotection against ischemia and reperfusion injury via cardiomyocyte-specific BK channels. Circulation. 2017;
Guo X, Yin H, Li L, Chen Y, Li J, Doan J, et al. Cardioprotective role of TRAF2 by suppressing apoptosis and necroptosis. Circulation. 2017;
Kura B, Babal P, Slezak J. Implication of microRNAs in the development and potential treatment of radiation-induced heart disease. Can J Physiol Pharmacol. 2017;95:1236–44.
Children’s Oncology Group. Guidelines for Survivors of Childhood, Adolescent, and Young Adult Cancer Long-Term Follow-Up Guidelines, Version 4.0. 2013;1–241.
Spewak MB, Williamson RS, Mertens AC, Border WL, Meacham LR, Wasilewski-Masker KJ. Yield of screening echocardiograms during pediatric follow-up in survivors treated with anthracyclines and cardiotoxic radiation. Pediatr Blood Cancer. 2017;64.
• Sritharan HP, Delaney GP, Lo Q, Batumalai V, Xuan W, Thomas L. Evaluation of traditional and novel echocardiographic methods of cardiac diastolic dysfunction post radiotherapy in breast cancer. Int J Cardiol. 2017;243:204–8. Describes the current status of echocardiographic diagnostics, and the need for novel methods in future guidelines.
Patel AA, Labovitz AJ. Advanced echocardiographic techniques in detection of cardiotoxicity. Curr. Treat. Options Cardiovasc. Med. 2016. p. 1–13.
Lipshultz SE, Adams MJ, Colan SD, Constine LS, Herman EH, Hsu DT, et al. Long-term cardiovascular toxicity in children, adolescents, and young adults who receive cancer therapy: Pathophysiology, course, monitoring, management, prevention, and research directions: a scientific statement from the American Heart Association. Circulation. 2013;128:1927–55.
Yusuf SW, Sami S, Daher IN. Radiation-induced heart disease: a clinical update. Cardiol Res Pract. 2011;2011:1–9.
Wu W, Masri A, Popovic ZB, Smedira NG, Lytle BW, Marwick TH, et al. Long-term survival of patients with radiation heart disease undergoing cardiac surgery: A cohort study. Circulation. 2013;127:1476–84.
•• Nishimura RA, Otto CM, Bonow RO, Carabello BA, Erwin JP, Fleisher LA, et al. AHA/ACC focused update of the 2014 AHA/ACC guideline for the management of patients with valvular heart disease. J Am Coll Cardiol. 2017;70:252–89. Comprehensive clinical guidelines applicable to patients with or at risk of developing valvular heart disease.
Adler Y, Charron P, Imazio M, Badano L, Barón-Esquivias G, Bogaert J, et al. ESC guidelines for the diagnosis and management of pericardial diseases. Eur Heart J. 2015;2015:2921–64.
Johnston DR. Surgical management of pericardial diseases. Prog. Cardiovasc. Dis. 2017. p. 407–16.
Lee Y, Naruse Y, Tanaka K. Effectiveness and long-term outcomes of surgical intervention for constrictive epicardium in constrictive pericarditis. Gen. Thorac. Cardiovasc. Surg. Springer Japan; 2017;0:0.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflicts of interest.
Human and Animal Rights and Informed Consent
All reported studies/experiments with human or animal subjects performed by the authors have been previously published and complied with all applicable ethical standards (including the Helsinki declaration and its amendments, institutional/national research committee standards, and international/national/institutional guidelines).
Additional information
This article is part of the Topical Collection on Cardio-oncology
Rights and permissions
About this article
Cite this article
Spetz, J., Moslehi, J. & Sarosiek, K. Radiation-Induced Cardiovascular Toxicity: Mechanisms, Prevention, and Treatment. Curr Treat Options Cardio Med 20, 31 (2018). https://doi.org/10.1007/s11936-018-0627-x
Published:
DOI: https://doi.org/10.1007/s11936-018-0627-x