Opinion statement
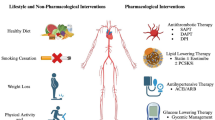
The choice of conduit is the most important factor influencing long-term patency of coronary artery bypass grafts (CABGs); arterial grafts are far superior to saphenous vein bypass grafts (SVGs) in this regard. Aspirin therapy should be started early in the perioperative period and continued indefinitely. Warfarin (Coumadin; Dupont, Wilmington, DE) and other platelet inhibitors offer no added value to aspirin, but may be used with benefit in aspirin-intolerant patients. Every effort should be made to reduce low-density lipoprotein cholesterol (LDL-C) to a value well below 100 mg/ dL. In most instances, this will require the use of an 3-hydroxy-3-methyglutaryl coenzyme A (HMG CoA) reductase inhibitor. Avoidance of cigarette smoking is imperative. Achieving a normal blood pressure, ideal body weight, and a regular exercise program are helpful. Those patients who have important obstruction in a SVG or arterial graft and who are symptomatic, or who have important myocardial ischemia with orjwithout symptoms should be treated with a procedure to improve perfusion to the myocardium supplied by the occluded bypass graft. Successful percutaneous transluminal coronary angioplasty (PTCA) and stenting of the obstructed graft usually will lead to improved myocardial perfusion, although in other clinical circumstances repeat CABG surgery will be required. On occasion, reperfusion of the myocardium can be achieved by PTCA of the native coronary artery with or without stenting while the degenerated graft is abandoned. When planning therapy for myocardial ischemia, the higher rate of PTCA related restenosis and the increased risks from repeat CABG must be carefully considered.
Similar content being viewed by others
References and Recommended Reading
Turina M: Coronary artery surgical technique. Curr Opin Cardiol 1993, 8:919–926.
The Post Coronary Artery Bypass Graft Trial Investigators: The effect of aggressive lowering of low-density lipoprotein cholesterol levels and low-dose anticoagulation on obstructive changes in saphenous-vein coronary bypass graft. N Engl J Med 1997, 336:153–162. This is the first published report indicating that aggressive lipid-lowering (to a level less than 100 mg/dL) is more effective than a moderate approach (a goal of less than 130 mg/dL) in patients with SVGs.
Morwani JG, Topol EJ: Aortocoronary saphenous vein graft disease: pathogenesis, predisposition, and prevention. Circulation 1998, 97:918–931.
Campeau L, Enjalbert M, Lespérance J, et al.: The relation of risk factors to the development of atherosclerosis in saphenous-vein bypass grafts and the progression of disease in the native circulation: a study 10 years after aortocoronary bypass surgery. N Engl J Med 1984, 311:1329–1332.
Knatterud GL, White CW, Geller NL, et al.: Angiographic changes in saphenous vein grafts are predictors of clinical outcomes. Circulation 2000, In press.
Knatterud GL, Rosenberg Y, Campeau L, et al.: The longterm effects on clinical outcomes of aggressive lowering of low-density lipoprotein cholesterol levels and low dose anticoagulation in Post Coronary Artery Bypass Graft Trial. Post CABG Investigators. Circulation 2000, 102:157–165.
Bryan AJ, Angelini GD: The biology of saphenous vein graft occlusion: etiology and strategies for prevention. Curr Opin Cardiol 1994, 9:641–649.
Loop FD: Internal-thoracic-artery grafts—biologically better coronary arteries. N Engl J Med 1996, 334:263–265. This article details the evidence for using autologous arteries for CABG.
Ferro M, Conti M, Novero D, et al.: The thin intima of the internal mammary artery as the possible reason for freedom from atherosclerosis and success in coronary bypass. Am Heart J 1991, 122:1192–1195.
Loop FD, Lytle DW, Cosgrove DM, et al.: Reoperation for coronary atherosclerosis: changing practice in 2509 patients. Ann Surg 1990, 212:378–385.
Loop FD, Lytle BW, Cosgrove DM, et al.: Influence of the internal mammary artery graft on 10-year survival and other cardiac events. N Engl J Med 1986, 314:1–6.
Boylan MJ, Lytle BW, Loop FS, et al.: Surgical treatment of isolated left anterior descending coronary stenosis: comparison of left internal mammary artery and venous autograft at 18–20 years of follow-up. J Thorac Cardiovasc Surg 1994, 107:657–662.
Henderson WG, Goldman S, Copeland JG, et al.: Antiplatelet or anticoagulant therapy after coronary artery bypass surgery: a meta-analysis of clinical trials. Ann Intern Med 1989, 111:743–750.
Goldman S, Copeland J, Moritz T, et al.: Improvement in early saphenous vein graft patency after coronary artery bypass surgery with antiplatelet therapy: results of a Veterans Administration cooperative study. Circulation 1988, 77:1324–1332.
Chesebro JH, Clements IP, Fuster V, et al.: A plateletinhibitor drug trial in coronary artery bypass operations: Benefit of perioperative dipyridamole and aspirin therapy on early post-operative vein-graft patency. N Engl J Med 1982, 307:73–78.
Chesebro JH, Fuster V, Elveback LR, et al.: Effect of dipyridamole and aspirin on late vein-graft patency after coronary bypass operations. N Engl J Med 1984, 310:209–214.
Fremes SE, Levinton C, Naylor CD, et al.: Optimal antithrombotic therapy following aortocoronary bypass: a meta-analysis. Eur J Cardiothorac Surg 1993, 7:169–180.
Goldman S, Copeland J, Moritz T, et al.: Long-term graft patency (3 years) after coronary artery surgery. Effects of aspirin: results of a VA cooperative study. Circulation 1994, 89:1138–1143.
The Medical Research Council’s General Practice Research Framework: Thrombosis prevention trail: randomized trial of low-intensity oral anti-coagulation with warfarin and low-dose aspirin in the primary prevention of ischemic heart disease in men at increased risk. Lancet 1998, 351:233–241.
Waters DD, Azar RR: Postscripts from the post coronary artery bypass graft trial. Circulation 2000, 102:144–146.
Blankenhorn DH, Nessim SA, Johnson RL, et al.: Beneficial effects of combined colestipol-niacin therapy on coronary atherosclerosis and coronary venous bypass grafts. JAMA 1987, 257:3233–3240.
Azen SP, Mack WJ, Cashin-Hemphill L, et al.: Progression of coronary artery disease predicts clinical coronary events: long-term follow-up from the Cholesterol Lowering Atherosclerosis Study. Circulation. 1996, 93:34–41.
Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults: Second report of the Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel II). Circulation 1994, 89:1329–1445.
Bourassa MG, Lespérance J, Corbara F, et al.: Progression of obstructive coronary artery disease 5 to 7 years after aortocoronary bypass surgery. Circulation 1978, 58:100–106.
Rigotti NA, McKool KN, Shiffman S: Predictors of smoking cessation after coronary artery bypass graft surgery: Results of the randomized trial with 5-year follow-up. Ann Intern Med 1994, 120:287–293.
Solymoss BC, Nadeau P, Nillette D, Campeau L: Late thrombosis of saphenous vein coronary bypass grafts related to risk factors. Circulation 1988, 78(suppl I):140–43.
Savage MP, Douglas JS, Fischman DL, et al.: Stent placement compared with balloon angioplasty for obstructed coronary bypass grafts. N Engl J Med 1997, 337:740–747.
Cameron A, Kemp HG Jr., Green GE: Reoperation for coronary artery disease: 10 years of clinical follow-up. Circulation 1988, 78(suppl I):158–162.
Rosengart TK: Risk analysis of primary versus reoperative coronary artery bypass grafting. Ann Thorac Surg 1993, 56(suppl):S-74.
Yusuf S, Zucker D, Peduzzi P, et al.: Effect of coronary artery bypass graft surgery on survival: overview of 10 year results from randomized trials by the Coronary Artery Bypass Graft Surgery Trialists Collaboration. Lancet 1994, 344:563–570.
Gobel FL, Stewart WJ, Campeau L, et al.: Safety of coronary arteriography in clinically stable patients following coronary bypass surgery. Cathet Cardiovasc Diagn 1998, 45:376–381.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Gobel, F.L., Mooney, M.R. & Graham, K.J. Coronary artery bypass graft degenerative disease. Curr Treat Options Cardio Med 3, 47–54 (2001). https://doi.org/10.1007/s11936-001-0084-8
Issue Date:
DOI: https://doi.org/10.1007/s11936-001-0084-8