Abstract
Surgical treatment is the gold standard for correction of penile deviation in patients with Peyronie’s disease. Generally, plication techniques are applied when deviation is less than 60°, the patient has decreased erectile function, and penile length is satisfactory. Grafting techniques are indicated when deviation exceeds 60°, there is a short penis or an hourglass deformity, and the patient has good erectile capacity. In patients with erectile dysfunction refractory to medical treatment, penile prosthesis implantation with simultaneous correction of deviation is the optimal approach. This article summarizes some of the novel advances for each of these procedures, which have been reported in recent years. Surgical technique and outcomes of these techniques are described, and limitations set. Adequate preoperative counseling, including all options available today, is crucial before planning surgical treatment in Peyronie’s disease. Surgeon experience and careful patient selection for each procedure will remain the most determining factors for success.
Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Hatzichristodoulou G, Lahme S. Peyronie’s disease. In: Merseburger AS, Kuczyk MM, Moul JW, editors. Urology at a Glance. Berlin-Heidelberg: Springer Publishing; 2014. p. 225–36.
Kadioglu A, Kücükdurmaz F, Sanli O. Current status of the surgical management of Peyronie’s disease. Nat Rev Urol. 2011;8:95–106.
Larsen S, Levine LA. Review of non-surgical treatment options for Peyronie’s disease. Int J Impot Res. 2012;24:1–10.
Ralph D, Gonzalez-Cadavid N, Mirone V, et al. The management of Peyronie’s disease: evidence-based 2010 guidelines. J Sex Med. 2010;7:2359–74.
Smith J, Walsh TJ, Lue TF. Peyronie’s disease: a critical appraisal of current diagnosis and treatment. Int J Impot Res. 2008;20:445–59.
Nelson C, Mulhall JP. Psychological impact of Peyronie’s disease: a review. J Sex Med. 2013;10:653–60.
Levine L, Burnett AL. Standard operating procedures for Peyronie’s disease. J Sex Med. 2013;10:230–44.
Mulhall J, Schiff J, Guhring P. An analysis of the natural history of Peyronie’s disease. J Urol. 2006;175:2115–8.
Hatzichristodoulou G. Conservative therapy of Peyronie’ s disease: update 2015. Urologe A. 2015;54:641–7.
Nehra A, Alterowitz R, Culkin DJ, et al. Peyronie’s disease: AUA Guideline. J Urol. 2015;194:745–53.
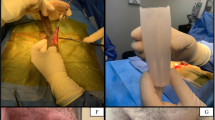
Hatzichristodoulou G, Gschwend JE, Lahme S. Surgical therapy of Peyronie’s disease by partial plaque excision and grafting with collagen fleece: feasibility study of a new technique. Int J Impot Res. 2013;25:183–7. This study reports initial results of a novel technique by partial plaque excision and grafting of the tunical defect with a self-adhesive collagen fleece.
Walsh T, Hotaling JM, Lue TF, et al. How curved is too curved? The severity of penile deformity may predict sexual disability among men with Peyronie’s disease. Int J Impot Res. 2013;25:109–12. This study emphasizes that penile curvature > 60° is the main determing factor for performing sexual intercourse, rather than the type of deformity.
Staerman F, Pierrevelcin J, Ripert T, et al. Medium-term follow-up of plaque incision and porcine small intestinal submucosal grafting for Peyronie’s disease. Int J Impot Res. 2010;22:343–8.
Kueronya V, Miernik A, Stupar S, et al. International multicentre psychometric evaluation of patient-reported outcome data for the treatment of Peyronie’s disease. BJU Int. 2015;115:822–8.
Sansalone S, Garaffa G, Djinovic R, et al. Long-term results of the surgical treatment of Peyronie’s disease with Egydio’s technique: a European multicentre study. Asian J Androl. 2011;13:842–5.
Taylor F, Levine LA. Surgical correction of Peyronie’s disease via tunica albuginea plication or partial plaque excision with pericardial graft: long-term follow up. J Sex Med. 2008;5:2221–8.
Chung E, Clendinning E, Lessard L, et al. Five-year follow-up of Peyronie’s graft surgery: outcomes and patient satisfaction. J Sex Med. 2011;8:594–600.
Nesbit R. Congenital curvature of the phallus: report of three cases with description of corrective operation. J Urol. 1965;93:230–2.
Gur S, Limin M, Hellstrom WJG. Current status and new developments in Peyronie’s disease: medical, minimally invasive and surgical treatment options. Expert Opin Pharmacother. 2011;12:931–44.
Chung P, Tausch TJ, Simhan J, et al. Dorsal plication without degloving is safe and effective for correcting ventral penile deformities. Urology. 2014;84:1228–33. This study shows that dorsal plication without degloving is safe and leads to satifying results in patients with ventral deviation.
Cantoro U, Polito M, Catanzariti F, et al. Penile plication for Peyronie’s disease: our results with mean follow-up of 103 months on 89 patients. Int J Impot Res. 2014;26:156–9. This study shows that plication techniques lead to reliable results for correction of deviation, even in the long-term.
Yafi F, Hatzichristodoulou G, Knoedler CJ, et al. Comparative analysis of tunical plication vs. intralesional injection therapy for ventral Peyronie’s disease. J Sex Med. 2015;12:2492–8.
Cormio L, Zucchi A, Lorusso F, et al. Surgical treatment of Peyronie’s disease by plaque incision and grafting with buccal mucosa. Eur Urol. 2009;55:1469–76.
Hsu GL, Chen HS, Hsieh CH, et al. Long-term results of autologous venous grafts for penile morphological reconstruction. J Androl. 2007;28:186–93.
Imbeault A, Bernard G, Ouellet G, et al. Surgical option for the correction of Peyronie’s disease: an autologous tissue-engineered endothelialized graft. J Sex Med. 2011;8:3227–35.
Kalsi J, Christopher N, Ralph DJ, et al. Plaque incision and fascia lata grafting in the surgical management of Peyronie’s disease. BJU Int. 2006;98:110–5.
Kim D, Lesser TF, Aboseif SR. Subjective patient-reported experiences after surgery for Peyronie’s disease: corporal plication versus plaque incision with vein graft. Urology. 2008;71:698–702.
Knoll L. Use of porcine small intestinal submucosa graft in the surgical management of Peyronie’s disease. Urology. 2001;57:753–7.
Knoll L. Use of small intestinal submucosa graft for the surgical management of Peyronie’s disease. J Urol. 2007;178:2474–8.
Levine L, Estrada CR, Storm DW, et al. Peyronie disease in younger men: characteristics and treatment results. J Androl. 2003;24:27–32.
Otero J, Gómez BG, Polo JM, et al. Use of a lyophilized bovine pericardium graft to repair tunical defect in patients with Peyronie’s disease: experience in a clinical setting. Asian J Androl. 2016. doi:10.4103/1008-682X.171572.
Salehipour M, Izadpanah K, Safaei A, et al. Application of human amniotic membrane in canine penile tunica albuginea defect: first step toward an innovating new method for treatment of Peyronie’s disease. Int Braz J Urol. 2014;40:400–7.
Salem E, Elkady EH, Sakr A, et al. Lingual mucosal graft in treatment of Peyronie disease. Urology. 2014;84:1374–7.
Segal R, Burnett AL. Surgical management for Peyronie’s disease. World J Mens Health. 2013;31:1–11.
Wimpissinger F, Parnham A, Gutjahr G, et al. 10 years’ plaque incision and vein grafting for Peyronie’s disease: does time matter? J Sex Med. 2016;13:120–8. This study shows that reliable and durable long-term results can be achieved with grafting techniques.
Zucchi A, Silvani M, Pastore AL, et al. Corporoplasty using buccal mucosa graft in Peyronie disease: is it a first choice? Urology. 2015;85:679–83.
Hatzichristodoulou G. Partial plaque excision and grafting with collagen fleece in Peyronie disease. J Sex Med. 2016;13:277–81. This article gives a detailed description of the grafting technique with the self-adhesive collagen fleece.
Fabiani A, Fioretti F, Filosa A, et al. Patch bulging after plaque incision and grafting procedure for Peyronie’s disease. Surgical repair with a collagen fleece. Arch Ital Urol Androl. 2015;87:173–4.
Kozacioglu Z, Degirmenci T, Gunlusoy B, et al. Effect of tunical defect size after Peyronie’s plaque excision on postoperative erectile function: do centimeters matter? Urology. 2012;80:1051–5.
Simonato A, Gregori A, Varca V, et al. Penile dermal flap in patients with Peyronie’s disease: long-term results. J Urol. 2010;183:1065–8.
Wilson S, Delk II JR. A new treatment for Peyronie’s disease: modeling the penis over an inflatable penile prosthesis. J Urol. 1994;152:1121–3.
Wilson S, Cleves MA, Delk II JR. Long-term follow-up of treatment for Peyronie’s disease: modeling the penis over an inflatable penile prosthesis. J Urol. 2001;165:825–9.
Berookhim B, Karpman E, Carrion R. Adjuvant maneuvers for residual curvature correction during penile prosthesis implantation in men with Peyronie’s disease. J Sex Med. 2015;12 Suppl 7:449–54.
Segal R, Cabrini MR, Bivalacqua TJ, et al. Penile straightening maneuvers employed during penile prosthesis surgery: technical options and outcomes. Int J Impot Res. 2014;26:182–5.
Chung P, Scott JF, Morey AF. High patient satisfaction of inflatable penile prosthesis insertion with synchronous penile plication for erectile dysfunction and Peyronie’s disease. J Sex Med. 2014;11:1593–8.
Djordjevic M, Kojovic V. Penile prosthesis implantation and tunica albuginea incision without grafting in the treatment of Peyronie’s disease with erectile dysfunction. Asian J Androl. 2013;15:391–4. This study reports results after plaque incision without grafting, to correct penile deviation during penile prosthesis implantation.
Egydio P, Kuehhas FE, Valenzuela RJ. Modified sliding technique (MoST) for penile lengthening with insertion of inflatable penile prosthesis. J Sex Med. 2015;12:1100–4.
Perito P, Wilson SK. The Peyronie’s plaque “scratch”: an adjunct to modeling. J Sex Med. 2013;10:1194–7.
Rolle L, Falcone M, Ceruti C, et al. A prospective multicentric international study on the surgical outcomes and patients’ satisfaction rates of the ‘sliding’ technique for end-stage Peyronie’s disease with severe shortening of the penis and erectile dysfunction. BJU Int. 2015. doi:10.1111/bju.13371. This study reports results of the sliding technique to correct penile deviation and increase penile length, during penile prosthesis implantation.
Weinberg A, Pagano MJ, Diebert CM, et al. Sub-coronal inflatable penile prosthesis placement with modified no-touch technique: a step-by-step approach with outcomes. J Sex Med. 2016;13:270–6.
Zucchi A, Silvani M, Pecoraro S. Corporoplasty with small soft axial prostheses (VIRILIS I®) and bovine pericardial graft (HYDRIX®) in Peyronie’s disease. Asian J Androl. 2013;15:275–9.
Egydio P, Kuehhas FE. Penile lengthening and widening without grafting according to a modified ‘sliding’ technique. BJU Int. 2015;116:965–72.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The author declares that he has no conflict of interest.
Human and Animal Rights and Informed Consent
All reported studies/experiments with human or animal subjects performed by the author have been previously published and complied with all applicable ethical standards (including the Helsinki declaration and its amendments, institutional/ national research committee standards, and international/national/institutional guidelines).
Additional information
This article is part of the Topical Collection on Male Sexual Dysfunction and Disorders
Rights and permissions
About this article
Cite this article
Hatzichristodoulou, G. Advances in the Surgical Treatment of Peyronie’s Disease. Curr Sex Health Rep 8, 186–192 (2016). https://doi.org/10.1007/s11930-016-0083-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11930-016-0083-0