Abstract
Purpose
To examine mental health outcomes of unaccompanied refugee minors during global policy shift. Additionally, to consider mental health service delivery and placement type for this group.
Methods
A rapid systematic search of research published since 2018 which related to mental health outcomes of unaccompanied refugee minors. Data extracted, risk of bias assessed and outcomes reviewed qualitatively.
Research Findings
We found 181 papers, of which 14 met inclusion criteria. This review found consistently high levels of PTSD and PTSS among URMs in various contexts. Exposure to trauma, being unaccompanied (compared to accompanied), being female and being older are associated with poor outcomes. Depression and anxiety were consistently high among URMs and associated with discrimination, limited language attainment and daily hassles.
Summary
High rates of mental illness and symptoms among unaccompanied refugee minors were consistent across national and settlement contexts but the quality of the evidence is variable with significant heterogeneity of assessment. We relate persistence of poor mental health outcomes with problems accessing mental health services and discuss the role of key post-migration factors influencing outcomes—in particular placement type and the use of detention centres.
Similar content being viewed by others
Introduction
Unaccompanied refugee minors are among the rising numbers of forcibly displaced people [1] [2]. In 2019 across Europe, 676,300 asylum seekers applied for international protection up over 10% compared to 2018 [3]. According to Eurostat, of those applying for asylum to Europe recently, most are from Syria, Afghanistan and Venezuela. Europe, Germany, followed by France and then Spain have the greatest numbers of refugees [4]. In the USA over the last few years, due to policy changes by the Trump administration, there has been significant reduction in numbers of refugees entering the USA. For the fiscal year 2020, there was a cap of 18,000 refugees, most from the Democratic Republic of Congo, followed by Myanmar and then the Ukraine [5]. At the time of writing, the Biden administration is faced with increasing numbers of unaccompanied minors arriving from Central America.
It is well documented that refugees are at an increased risk of various mental illnesses [6] [7,8,9]. While the World Health Organization has encouraged the implementation of the Strategy and Action Plan for refugee health [10], addressing the health needs of refugees remains a significant challenge at the global, national and local levels.
Refugee children have often experienced a range of traumatic events, such as death/persecution of family members, war, forced recruitment and personal persecution and then must manage the dual stressors of traumatic past with resettlement [11, 12]. Beyond those risk factors related to the initial process of fleeing one’s native country, there are significant risk factors for poor mental health outcomes associated with resettlement processes and reception. In 2019, 27% of refugee children entering Europe were unaccompanied or separated [13]. An unaccompanied minor is a person less than 18 years old who arrives in another country not accompanied by an adult responsible for the minor or a minor who is left unaccompanied after having entered a country [3] [10]. A separated minor is a child separated from both parents, their legal guardian or primary care giver, but may have travelled with other relatives, and so may have been accompanied by other adult family members [14].
As a major contextual dimension to this paper, we have noted an increasingly punitive response to refugees and migrants in many Western countries, likely to have worsened the health outcomes for refugees; for example in the USA, the increase in use of detention centres and separation of children from families for Mexican migrants has been attributed to increased vulnerability for poor mental health outcomes [15]. In Australia, stringent policy initiatives have created detention in off-shore islands and camps, the inability to apply for permanent residency, removal of free legal assistance and the indefinite inability to reunite with immediate family members [16]. In Europe, there was politicizing concepts of humanitarianism, security, diversity, protectionism—all employed in public discourse to legitimize restrictions in migration, in conjunction with increased hostility to asylum seekers [17]. According to a recent World Bank migration brief (2017), the number of potential returnees from European Union countries, people denied asylum or undocumented migrants more than tripled within 4 years to over 5 million in 2016 [18]. In the USA, potential returnees doubled to 3 million over the same period.
In this review, we have identified and examined recent literature on the prevalence and associated factors for mental health disorders in unaccompanied refugee minors. We also discuss the recent evidence base and service delivery for this group and consider post-migration predictors of mental health outcomes and the key issues of placement type and use of detention centres.
Method: Rapid Systematic Literature Review
Search Strategy and Selection Characteristics
For this rapid review, we searched for potential articles that could be included on PubMed, Medline and socINDEX databases on the 13/03/2021. We used principles recommended by the WHO, and PRISMA reporting guidelines were adhered to [19, 20]. We used the following combination of terms: “refugee”, “displaced”, “asylum seeker”, “unaccompanied”, “child”, “minor”, “adolescent”, “mental illness”, “mental health”, “mental health outcomes”, “depression”, “anxiety”, “PTSD” and “post-traumatic stress”. A copy of the full search strategy is available in the Appendix. The following inclusion criteria were used in assessing articles:
-
1.
Peer reviewed material
-
2.
Review only material published since 2018
-
3.
Published in English language journals
-
4.
Provide data on mental health outcomes of unaccompanied refugee minors
-
5.
Primary research, quantitative, otherwise not design restricted
Exclusion criteria:
-
1.
Qualitative studies
-
2.
If mean age of sample was over 18
-
3.
If article focussed on intervention
-
4.
If no specific outcomes for URMs provided
Duplicates were removed. In the first stage, two independent researchers (JB and MF) screened titles and abstracts for papers identified. In the second stage, the same researchers screened the full texts of all remaining studies to assess eligibility for data extraction and analysis. At either stage, any queries or disagreement on eligibility were remedied via discussion with GL.
Data Extraction and Quality
The authors then extracted data about the following from eligible articles: publication year, country of study, URMs characteristics (country they fled from, number of URMs included in the study), design, assessment method, time period and main results on mental health outcomes in keeping with review processes [21]. We assessed risk of bias via the Joanna Briggs critical appraisal checklist, commonly used in rapid reviews [22]. We then undertook a qualitative synthesis of findings. We begin by describing study characteristics. Following this, we grouped broad health outcomes together to describe mental health outcomes of unaccompanied refugee minors.
Results
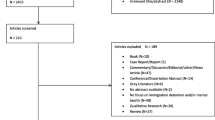
Database search identified 181 articles in total, of which an eventual 14 met inclusion criteria, further details are provided in Fig. 1. The main reason for exclusion commonly was related to the population group not being unaccompanied refugee minors.
Table 1 shows study characteristics. Studies were mainly from Germany, followed by Norway and Sweden. Most studies were cross-sectional, with some prospective cohort studies, and one retrospective cohort study. No RCTs identified.
Most studies solely had only URMs as participants, some had a heterogeneous group of accompanied and unaccompanied youth, often comparing outcomes between the two. As seen in Table 1, a range of assessment tools were utilized across studies, ranging from questionnaires to clinical assessment. Table 2 shows a summary of studies by mental health outcomes. Most assess PTSD, anxiety and/or depression. Some studies focussed on aggregate measures of “psychological distress”, i.e. those individuals at high risk of poor mental health outcomes. A minority of studies examined somatic symptoms and sleeping disturbance.
Quality Assessment/Risk of Bias
Following assessment for risk bias, we concluded that most of the 14 studies were of moderate quality. A small number were of high quality, and a small minority were of low quality. Low quality often related to poor consideration of confounding variables and inadequately described samples.
PTSD and PTSS
Estimates of post-traumatic stress disorder (PTSD) and post-traumatic stress symptoms (PTSS) were generally higher among URMs compared to those of accompanied minors. Some studies measured PTSD, often via a cumulative measure of PTSD-related symptoms and a defined cut-off for caseness or via clinical interview by a trained practitioner. Other studies measured the symptoms associated with post-traumatic events, namely avoidance, hyper vigilance and mistrust. Studies referred to the development of these symptoms as PTSS. There is significant overlap in the symptoms defining PTSD and PTSS [24, 29, 32, 37, 38]. All measures of both PTSD and PTSS in the studies included were symptom driven. PTSD rates were as high as 53.7% among a group of 324 URMs in Sweden, compared to just 37.1% of accompanied refugees [24]. Among another sample in Sweden, of 265 URMs assessed by a medical professional, 21.8% had post-traumatic stress symptoms to such a degree where it was affecting wellbeing on a daily basis, compared to just 5.8% of accompanied refugee minors [28]. Considering PTSS, in Germany, 64.7% of URMs had PTSS, compared to 36.7% of accompanied refugee minors in one study [32]. Among another group of URMs in Germany, 32% were found to have PTSD [33]. This rate differs significantly when compared to that of a German study which reported a PTSD prevalence of 4.6% among 246 URMs from Syria, assessed through a clinical interview [31]. In Ethiopia, among a group of 384 Eritrean URMs in a refugee camp, 38% had probable PTSD [27].
In a prospective cohort study in Germany, PTSS among URMs remained high at follow-up, with 37.5% still experiencing symptoms while other psychopathology tended to improve at follow-up [29]. Moreover, those URMs in Germany who had their asylum status rejected at follow-up were more at risk of poor mental health outcomes. These groups have no legal protection to stay in their host country and can be deported. Similarly, a prospective cohort study in Norway revealed that URMs showed no improvement in PTSS after 5 years, with worse outcomes for females, older refugees and those with severe trauma exposure [30]. Importantly, exposure to daily hassles in their resident country was a predictor of PTSS. This finding related strongly with Arega’s (2020) findings among Eritean URMs, where females and those in the oldest age group (15–17) had the worst outcomes. Among this group of URMs placed in a refugee camp, the most robust predictor of PTSD was previous exposure to trauma. Unaccompanied status was also an important predictor of PTSD and PTSS [24, 28, 32]. PTSD was predicted by number of traumatic experiences, lower individual resources and social support, and language acquisition [32] [33]. In the UK, refugees under the age of 18 have access to specific support and services. One study in the UK followed URMs who had been detained due to dispute regarding their age. This occurs where refugees are thought to not be under the age of 18, and a process is carried out to verify age. Among this group, post-detention, 89% had high PTSD symptoms [35]. Klonig et al.’s assessment of unaccompanied minors within paediatric clinics in Germany found 25% may be at risk of a mental disorder such as PTSD. Casesness was based on clinicians’ assessment of medical records [34].
Depression and Anxiety
A comparison of rates of depression and anxiety between accompanied and unaccompanied minors show fairly consistent findings across studies. A Norwegian study [23] using the Centre for Epidemiologic Studies Depression Scale for adolescents CES-D [39] among a sample of 895 URMs from 31 different countries (51% from Afghanistan) found that 40% met the cut-off for depression. In Germany, a study of minors primarily from Afghanistan, Syria and Eritrea reported 42.6% of URMs had depression compared to just 30% of accompanied refugee minors [32]. The same study reported 38.2% of URMs had anxiety compared to 23.3% of accompanied minors [32]. Another German study of URMs from Syria and Afghanistan aged 14–19 years, living in group homes of the Child Protection Services, reported rates of depression at around 40% [33]. However, another study of 346 Syrian URMs living in Germany, using clinical assessment of symptoms, observed that 2.9% had depression [31].
The study by Hanewald et al. [26] used a screening instrument (RHS-15) to determine the presence of distress. The RHS-15 was derived from the most commonly cited complaints of refugees. The tool avoids seeking details of specific traumatic experiences. Among a sample of 561 URMs, 43.6% were found to be highly likely to experience a mental disorder [26]. Farsi and Somali speakers, older refugees and males were all more likely to have worse outcomes. A prospective cohort study in Denmark found that URMs were at higher risk of any psychiatric disorder and neurotic disorders compared to accompanied minors [36]. Norredam et al. found that URMs from Afghanistan were more vulnerable to any psychiatric disorder and neurotic disorders, while those from Iraq were at risk of any psychiatric disorder, affective disorders and neurotic disorders. Finally, Hjern and Kling [28] found that 32.8% of URMs had significant sleeping disturbance compared to just 21.8% of accompanied refugees.
In Odepal et al.’s Norwegian study, longer length of residence in Norway, and greater heritage and cultural identity among URMs were protective for depression [23, 25]. Symptoms of both depression and anxiety were more prevalent among those URMs who experienced high levels of discrimination in their host countries [25]. The same study [25] noted that post-migration factors rather than pre-migration traumatic events were associated with social anxiety. Additionally, while males were at higher risk of depression, no gender differences were found for risk of anxiety. In Muller et al.’s [29] prospective cohort study, most URMs showed clinical improvement in anxiety and depression symptoms at follow-up, despite baseline psychopathology predicting long-term outcomes. However, in another prospective cohort study among URMs in Norway, symptoms of depression improved at follow-up, but anxiety did not. This study also found that females, those more exposed to trauma, older refugees and those experiencing daily hassles experienced worst outcomes [30]. Sierau et al. [33] found that poor family contact and lower mentor support predicted depression and anxiety symptoms.
Discussion
While young refugees experience high levels of mental health problems and symptoms, predominantly PTSD, PTSS, depression, anxiety and behavioural problems [40, 41], these disorders and symptoms are consistently higher among the more vulnerable unaccompanied minors, such as females and older refugees [42]. While the findings of these studies consistently point to high rates of psychiatric disorders and symptomatology among unaccompanied refugee minors compared to their accompanied counterparts, the quality of the evidence is variable. We noted that rates of PTSD, PTSS and depression were higher when using validated instruments compared to studies that used clinical interviews and interpreters. PTSD was predicted robustly by number of traumatic experiences, in keeping with previous research on refugee children, more generally [43]. Interestingly, social support, ongoing family contact, social connections, language proficiency and experiences of daily hassles were all significant predictors of PTSD and PTSS; follow-up studies reinforced this. Perhaps unsurprisingly, some evidence suggests that detention centres are associated with extremely poor outcomes for PTSD.
Again, some caution is needed in assessing the evidence. As with other reviews on refugee mental health, we found considerable heterogeneity across studies [44]. Many of the findings emerge from relatively small samples and/or samples that comprised young people from a wide range of countries of origin and exposures; differences in host country circumstances and provision (e.g. reception, dispersion, accommodation, healthcare and educational opportunities) which might mitigate psychological distress, are also unknown and, thus, impossible to control for. Heterogenous methods and measures of diagnostic ascertainment make any definitive appraisal about prevalence difficult. While most have relied on diagnostic instruments to assess psychopathology, others have used clinical judgement. However, the variation and inconsistency noted in URMs studies have been noted in the wider refugee literature [45]. Thus, a review by Kien and colleagues [44] found that the point prevalence of psychiatric disorders varied widely among studies (presenting interquartile ranges): for post-traumatic stress disorder between 19.0 and 52.7% and for depression, between 10.3 and 32.8%.
While high rates of mental health problems have been consistently observed, the evidence on long-term psychiatric outcomes is limited. Other longitudinal studies indicate that poor mental health may persist over years [46]. However, it is acknowledged that upon entry to a country, unaccompanied minors have difficulties in accessing health services, due to various structural, legal and practical barriers. Mental health of UMRs represents a complex task for receiving countries, as the needs are often disproportionately high in this group and thus quick access is desirable. However, access to necessary services has been seen to be delayed on both sides of the Atlantic in the Netherlands, Belgium and Canada, with lengthy asylum-seeking procedures, coupled with cultural differences, especially surrounding belief systems and language resulting in deterioration in mental health over time and further increasing the need for services among this group [47].
Furthermore, in recent research conducted among UMRs in the Netherlands, among the sample, 61% had made use of healthcare services; however, when asked about mental healthcare services, this dropped to 17%. Although most attendees understood the importance of mental health support and felt they received good care, poor therapist understanding of their situation was cited as the main reason for dissatisfaction with care [48].
Another key determinant of poor mental health outcomes for URMs may relate to children’s own perceptions of mental health and healthcare systems and the implications of a psychiatric diagnosis. Their perceptions may deter engagement with mental health services [49]. This is illustrated by the explanatory models of mental illness noted among Somalian refugees in Norway and Kurdish refugees in the UK, and how their beliefs in spirit possession and use of traditional healers deterred engagement with the host healthcare systems [50, 51]. Such beliefs could contribute to the view that western mental health services would not understand or be able to adequately address health needs. However, URMs may also lack knowledge of western healthcare systems. These both act as barriers to accessing care and addressing mental health care needs.
The current review found evidence that post-migration factors are important determinants of mental health outcomes for URMs, as opposed to simply pre-flight exposure to trauma. Studies found that poor social support, poor language proficiency of resident country, reduced resources, experience of discrimination, asylum status and increased daily hassles were all key predictors of outcomes [25, 29, 32, 33]. Two key longitudinal studies by Muller et al. [33] and Jensen et al. [31] highlighted the persistence of poor mental health in this population and the importance of maintaining social support and providing language training to develop self-efficacy and mitigate against daily hassles. These findings resonate with a growing body of literature advocating for strong rearing environments in the host country (often foster placements) for the promotion of better mental health outcomes for URMs [52, 53]. We found some evidence of poor outcomes related to detention centres which attract high levels of concern about poor facilities and the denial of human rights [54]. URMs in detention centres may experience family separation which damages key attachment relationships and causes stress, significantly increasing risk of poor mental health outcomes [55]. The process of forced separation causes significant emotional distress and is associated with a range of emotional problems in children and often compounds poor mental health and educational outcomes [56, 57].
Conclusions
There is growing novel evidence of increased burden of psychiatric disorders and symptoms among URMs; however, the studies are heterogeneous in design and population. This review shows that recent studies indicate that post-migration factors are important predictors of mental health outcomes. Namely we found that poor social support, poor language proficiency of resident country, experience of discrimination and experience of daily hassles influence outcomes for URMs. We found some evidence that the process of detention is extremely damaging for URMs’ mental health outcomes, and that strong rearing environments in host countries are protective for mental wellbeing. Future studies should employ a longitudinal design to follow up URMs and their outcomes, and explore how best to address post-migration determinants of well-being such as addressing social support, language proficiency and discrimination.
Data Availability
Not applicable.
References
Moussalli M. Handbook on procedures and criteria for determining refugee status under the 1951 convention and the 1967 protocol relating to the status of refugees. Geneva: Office of the United Nations High Commissioner for Refugees; 1992.
UNHCR. Refugee Data Finder. 2021 [cited 2021 12/02]; Available from: https://www.unhcr.org/refugee-statistics/
Eurostat. Asylum Statistics. 2019 [cited 2021 10/02/2021]; Available from: https://ec.europa.eu/eurostat/statistics-explained/index.php/Asylum_statistics - Number_of_asylum_applicants:_increase_in_2019
Eurostat. Asylum and first time asylum applicants by citizenship, age and sex - annual aggregated data (rounded). 2021 [cited 2021 10/02]; Available from: https://ec.europa.eu/eurostat/databrowser/view/migr_asyappctza/default/table?lang=en
Pew Research Centre. Key facts about refugees in the U.S. 2019 [cited 2021 13/02]; Available from: https://www.pewresearch.org/fact-tank/2019/10/07/key-facts-about-refugees-to-the-u-s/
Lebano A, et al. Migrants’ and refugees’ health status and healthcare in Europe: a scoping literature review. BMC Public Health. 2020;20(1):1–22.
Lustig SL, Kia-Keating M, Knight WG, Geltman P, Ellis H, Kinzie JD, et al. Review of child and adolescent refugee mental health. J Am Acad Child Adolesc Psychiatry. 2004;43(1):24–36.
Hodes M, Vostanis P. Practitioner review: mental health problems of refugee children and adolescents and their management. J Child Psychol Psychiatry. 2019;60(7):716–31.
Bronstein I, Montgomery P. Psychological distress in refugee children: a systematic review. Clin Child Fam Psychol Rev. 2011;14(1):44–56.
World Health Organization, Report on the health of refugees and migrants in the WHO European Region: no public health without refugees and migrant health. 2018
Musliu E, et al. School nurses’ experiences working with unaccompanied refugee children and adolescents: a qualitative study. SAGE Open Nursing. 2019;5:2377960819843713.
Hopkins PE, Hill M. Pre-flight experiences and migration stories: the accounts of unaccompanied asylum-seeking children. Children's geographies. 2008;6(3):257–68.
UNICEF. Latest statistics and graphics on refugee and migrant children 2021 [cited 2021 11/02]; Available from: https://www.unicef.org/eca/emergencies/latest-statistics-and-graphics-refugee-and-migrant-children
International Committeeof The Red Cross, Inter-agency guiding principles on unaccompanied and separated children. 2004: Geneva, Switzerland.
Grace BL, Bais R, Roth BJ. The violence of uncertainty—undermining immigrant and refugee health. N Engl J Med. 2018;379(10):904–5.
UNHCR. Monitoring Asylum in Australia. 2021 [cited 2021 12/02]; Available from: https://www.unhcr.org/uk/asylum-in-australia.html
Krzyżanowski, M., A. Triandafyllidou, and R. Wodak, The mediatization and the politicization of the “refugee crisis” in Europe. 2018, Taylor & Francis
Group, W.B. Migration and remittances. 2017 [cited 2021 30/03/2021]; Available from: http://documents1.worldbank.org/curated/en/719531507124177735/pdf/120240-WP-PUBLIC-3-10-2017-22-22-41-MigrationandDevelopmentBrief.pdf
Tricco AC, et al., Rapid reviews to strengthen health policy and systems: a practical guide. 2017: World Health Organization
Moher D, Liberati A, Tetzlaff J, Altman DG, PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Int J Surg. 2010;8(5):336–41.
Popay J, et al. Guidance on the conduct of narrative synthesis in systematic reviews. A product from the ESRC methods programme Version. 2006;1:b92.
Aromataris E, et al. Summarizing systematic reviews: methodological development, conduct and reporting of an umbrella review approach. JBI Evidence Implementation. 2015;13(3):132–40.
Oppedal B, Ramberg V, Røysamb E. The asylum-process, bicultural identity and depression among unaccompanied young refugees. J Adolesc. 2020;85:59–69.
Solberg Ø, et al. Children at risk: a nation-wide, cross-sectional study examining post-traumatic stress symptoms in refugee minors from Syria, Iraq and Afghanistan resettled in Sweden between 2014 and 2018. Confl Heal. 2020;14(1):1–12.
Jore T, Oppedal B, Biele G. Social anxiety among unaccompanied minor refugees in Norway. The association with pre-migration trauma and post-migration acculturation related factors. J Psychosom Res. 2020;136:110175.
Hanewald B, Knipper M, Fleck W, Pons-Kühnemann J, Hahn E, Ta TMT, et al. Different patterns of mental health problems in unaccompanied refugee minors (URM): a sequential mixed method study. Frontiers in psychiatry. 2020;11:324.
Arega NT, Posttraumatic stress among Eritrean unaccompanied refugee minors in Ethiopia. International Journal of Migration, Health and Social Care, 2020.
Hjern A, Kling S. Health care needs in school-age refugee children. Int J Environ Res Public Health. 2019;16(21):4255.
Müller LRF, et al. 1-year follow-up of the mental health and stress factors in asylum-seeking children and adolescents resettled in Germany. BMC Public Health. 2019;19(1):1–11.
Jensen TK, Skar AMS, Andersson ES, Birkeland MS. Long-term mental health in unaccompanied refugee minors: pre-and post-flight predictors. Eur Child Adolesc Psychiatry. 2019;28(12):1671–82.
Laukamp A, et al. Health of Syrian unaccompanied asylum seeking adolescents (UASA) at first medical examination in Germany in comparison to UASA from other world regions. BMC Int Health Hum Rights. 2019;19(1):1–8.
Müller LRF, et al. Mental health and associated stress factors in accompanied and unaccompanied refugee minors resettled in Germany: a cross-sectional study. Child Adolesc Psychiatry Ment Health. 2019;13(1):1–13.
Sierau S, Schneider E, Nesterko Y, Glaesmer H. Alone, but protected? Effects of social support on mental health of unaccompanied refugee minors. Eur Child Adolesc Psychiatry. 2019;28(6):769–80.
Kloning T, et al. Morbidity profile and sociodemographic characteristics of unaccompanied refugee minors seen by paediatric practices between October 2014 and February 2016 in Bavaria, Germany. BMC Public Health. 2018;18(1):1–9.
Ehntholt KA, Trickey D, Harris Hendriks J, Chambers H, Scott M, Yule W. Mental health of unaccompanied asylum-seeking adolescents previously held in British detention centres. Clinical child psychology and psychiatry. 2018;23(2):238–57.
Norredam M, Nellums L, Nielsen RS, Byberg S, Petersen JH. Incidence of psychiatric disorders among accompanied and unaccompanied asylum-seeking children in Denmark: a nation-wide register-based cohort study. Eur Child Adolesc Psychiatry. 2018;27(4):439–46.
Sachser C, Berliner L, Holt T, Jensen TK, Jungbluth N, Risch E, et al. International development and psychometric properties of the Child and Adolescent Trauma Screen (CATS). J Affect Disord. 2017;210:189–95.
Perrin S, Meiser-Stedman R, Smith P. The Children’s Revised Impact of Event Scale (CRIES): validity as a screening instrument for PTSD. Behav Cogn Psychother. 2005;33(4):487–98.
Radloff LS. The CES-D scale:a self-report depression scale for research in the general population. Appl Psychol Meas. 1977;1(3):385–401.
Jensen TK, Fjermestad KW, Granly L, Wilhelmsen NH. Stressful life experiences and mental health problems among unaccompanied asylum-seeking children. Clin Child Psychol Psychiatry. 2015;20(1):106–16.
Leavey G, King M, Barnes J, Hollins K, Papadopoulos C, Grayson K. Psychological disorder amongst refugee and migrant children in London. Soc Psychiatry Psychiatr Epidemiol. 2004;39:191–5.
Huemer J, Karnik NS, Voelkl-Kernstock S, Granditsch E, Dervic K, Friedrich MH, et al. Mental health issues in unaccompanied refugee minors. Child Adolesc Psychiatry Ment Health. 2009;3(1):13.
Fazel M, Reed RV, Panter-Brick C, Stein A. Mental health of displaced and refugee children resettled in high-income countries: risk and protective factors. Lancet. 2012;379(9812):266–82.
Kien C, Sommer I, Faustmann A, Gibson L, Schneider M, Krczal E, et al. Prevalence of mental disorders in young refugees and asylum seekers in European countries: a systematic review. Eur Child Adolesc Psychiatry. 2019;28(10):1295–310.
Blackmore R, Boyle JA, Fazel M, Ranasinha S, Gray KM, Fitzgerald G, et al. The prevalence of mental illness in refugees and asylum seekers: a systematic review and meta-analysis. PLoS Med. 2020;17(9):e1003337.
Vervliet M, Lammertyn J, Broekaert E, Derluyn I. Longitudinal follow-up of the mental health of unaccompanied refugee minors. Eur Child Adolesc Psychiatry. 2014;23(5):337–46.
Arakelyan , S. And a. Ager Annual Research Review: A multilevel bioecological analysis of factors influencing the mental health and psychosocial well-being of refugee children. Journal of Child Psychology and Psychiatry, 2020
Zijlstra AE, Menninga MC, van Os ECC, Rip JA, Knorth EJ, Kalverboer ME. ‘There is no mother to take care of you’. Views of unaccompanied children on healthcare, their mental health and rearing environment. Resid Treat Child Youth. 2019;36(2):118–36.
Majumder P. Exploring stigma and its effect on access to mental health services in unaccompanied refugee children. BJPsych Bulletin. 2019;43(6):275–81.
Satinsky E, Fuhr DC, Woodward A, Sondorp E, Roberts B. Mental health care utilisation and access among refugees and asylum seekers in Europe: a systematic review. Health Policy. 2019;123(9):851–63.
Leavey G, Guvenir T, Haase-Casanovas S, Dein S. Finding help: Turkish speaking refugees and migrants with a history of psychosis. Transcultural Psychiatry. 2007;44(2):258–74.
Mitra R, Hodes M. Prevention of psychological distress and promotion of resilience amongst unaccompanied refugee minors in resettlement countries. Child Care Health Dev. 2019;45(2):198–215.
Höhne E, van der Meer A.S., Kamp-Becker I., Christiansen H., A systematic review of risk and protective factors of mental health in unaccompanied minor refugees. European Child & Adolescent Psychiatry, 2020
von Werthern M, Robjant K, Chui Z, Schon R, Ottisova L, Mason C, et al. The impact of immigration detention on mental health: a systematic review. BMC Psychiatry. 2018;18(1):382.
Wood LC. Impact of punitive immigration policies, parent-child separation and child detention on the mental health and development of children. BMJ paediatrics open. 2018;2:1.
MacLean SA, Agyeman PO, Walther J, Singer EK, Baranowski KA, Katz CL. Characterization of the mental health of immigrant children separated from their mothers at the US–Mexico border. Psychiatry Res. 2020;286:112555.
Hanes G, Chee J, Mutch R, Cherian S. Paediatric asylum seekers in Western Australia: identification of adversity and complex needs through comprehensive refugee health assessment. J Paediatr Child Health. 2019;55(11):1367–73.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by Jordan Bamford and Mark Fletcher. The first draft of the manuscript was written by Jordan Bamford and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript. Gerard Leavey involved in all processes and edited the final version.
Corresponding author
Ethics declarations
Ethics Approval
Not needed.
Consent to Participate
Not applicable.
Consent for Publication
Not applicable.
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical collection on Disaster Psychiatry: Trauma, PTSD, and Related Disorder
Appendix
Appendix
Search strategy for PubMed, Medline and socINDEX
Search 1
“refugee”, “displaced”, “asylum seeker”
= COMBINE WITH OR
Search 2
“unaccompanied”, “alone”
Search 3
“child”, “minor”, “adolescent” “youth” “teen”
= COMBINE WITH OR
Search 4
“mental illness”, “mental health”, “mental health outcomes”, “depression”, “anxiety”, “PTSD” and “post-traumatic stress” “psychological distress”
= COMBINE WITH OR
Combine search 1 AND search 2 AND search 3 AND search 4
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Bamford, J., Fletcher, M. & Leavey, G. Mental Health Outcomes of Unaccompanied Refugee Minors: a Rapid Review of Recent Research. Curr Psychiatry Rep 23, 46 (2021). https://doi.org/10.1007/s11920-021-01262-8
Accepted:
Published:
DOI: https://doi.org/10.1007/s11920-021-01262-8