Abstract
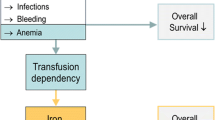
The myelodysplastic syndromes (MDS) are a group of clonal hematopoietic stem cell diseases characterized by ineffective hematopoiesis in one or more cell lines, resulting in insufficient bone marrow function. For most patients with MDS, supportive care by blood transfusions is still the mainstay of treatment. Especially in low-risk patients, anemia represents the major clinical problem, and many of these patients develop transfusional iron overload. This paper reviews the literature on transfusional iron overload in patients with MDS, looking at pathophysiology, evaluation, and treatment of the transfusional iron burden with desferrioxamine and oral chelators.
Similar content being viewed by others
References and Recommended Reading
Bennett JM, Catovsky D, Daniel MT, et al.: Proposals for the classification of the myelodysplastic syndromes. Br J Haematol 1982, 51:189–199.
Germing U, Gattermann N, Strupp C, et al.: Validation of the WHO proposals for a new classification of primary myelodysplastic syndromes: a retrospective analysis of 1600 patients. Leuk Res 2000, 24:983–992.
Cazzola M, Anderson JE, Ganser A, Hellstrom-Lindberg E: A patient-oriented approach to treatment of myelodysplastic syndromes. Haematologica 1998, 83:910–935.
Pootrakul P, Kitcharoen K, Yansukon P, et al.: The effect of erythroid hyperplasia on iron balance. Blood 1988, 71:1124–1129.
Cazzola M, Barosi G, Gobbi PG: Natural history of idiopathic refractory sideroblastic anemia. Blood 1988, 71:305–312.
Hershko C, Rachmilewitz EA: Mechanism of desferrioxamine-induced iron excretion in thalassaemia. Br J Haematol 1979, 42:125–132.
Hershko C, Konijn AM, Link G: Iron chelators for thalassaemia. Br J Haematol 1998, 101:399–406.
Esposito BP, Breuer W, Sirankapracha P, et al.: Labile plasma iron in iron overload: redox activity and susceptibility to chelation. Blood 2003, 102:2670–2677.
Pootrakul P, Breuer W, Sametband M, et al.: Labile plasma iron (LPI) as an indicator of chelatable plasma redox activity in iron-overloaded beta-thalassemia/HbE patients treated with an oral chelator. Blood 2004, 104:1504–1510.
Link G, Pinson A, Hershko C: Heart cells in culture: a model of myocardial iron overload and chelation. J. Lab Clin Med 1985, 106:147–153.
Randell EW, Parkes JG, Olivieri NF, Templeton DM: Uptake of non-transferrin-bound iron by both reductive and nonreductive processes is modulated by intracellular iron. J Biol Chem 1994, 269:16046–16053.
Gutteridge JM, Rowley DA, Griffiths E, Halliwell B: Low-molecular-weight iron complexes and oxygen radical reactions in idiopathic haemochromatosis. Clin Sci (Colch) 1985, 68:463–467.
Hershko C, Link G, Cabantchik I: Pathophysiology of iron overload. Ann N Y Acad Sci 1998, 850:191–201.
Modell B, Berdoukas V: The Clinical Approach to Thalassemia. New York: Grune and Stratton; 1981.
Pippard M: Measurement of iron status. Prog Clin Biol Res 1989, 309:705–713.
Barry M: Liver iron concentration, stainable iron and total body storage iron. Gut 1974, 15:411–415.
Brissot P, Bourel M, Herry D, et al.: Assessment of liver iron content in 271 patients: a reevaluation of direct and indirect methods. Gastroenterology 1981, 80:557–565.
Angelucci E, Brittenham GM, McLaren CE, et al.: Hepatic iron concentration and total body iron stores in thalassemia major. N Engl J Med 2000, 343:327–331.
Angelucci E, Baronciani D, Lucarelli G, et al.: Needle liver biopsy in thalassaemia: analyses of diagnostic accuracy and safety in 1184 consecutive biopsies. Br J Haematol 1995, 89:757–761.
Brittenham GM, Badman DG: Noninvasive measurement of iron: report of an NIDDK workshop. Blood 2003, 101:15–19.
St. Pierre TG, Clark PR, Chua-anusorn W, et al.: Noninvasive measurement and imaging of liver iron concentrations using proton magnetic resonance. Blood 2005, 105:855–861.
Clark PR, Chua-anusorn W, St. Pierre TG: Proton transverse relaxation rate (R2) images of iron-loaded liver tissue; mapping local tissue iron concentrations with MRI. Magn Reson Med 2003, 49:572–575. [Published erratum appears in Magn Reson Med 2003, 49:1201.]
Wood JC, Enriquez C, Ghugre N, et al.: MRI R2 and R2* mapping accurately estimates hepatic iron concentration in transfusion-dependent thalassemia and sickle cell disease patients. Blood 2005, 106:1460–1465.
Jensen PD, Jensen FT, Christensen T, Ellegaard J: Non-invasive assessment of tissue iron overload in the liver by magnetic resonance imaging. Br J Haematol 1994, 87:171–184.
Konijn AM: Iron metabolism in inflammation. Baillieres Clin Haematol 1994, 7:829–849.
Tran TN, Eubanks SK, Schaffer KJ: Secretion of ferritin by rat hepatoma cells and its regulation by inflammatory cytokines and iron. Blood 1997, 90:4979–4986.
Prieto J, Barry M, Sherlock S: Serum ferritin in patients with iron overload and with acute and chronic liver diseases. Gastroenterology 1975, 68:525–533.
Brittenham GM, Cohen AR, McLaren CE, et al.: Hepatic iron stores and plasma ferritin concentration in patients with sickle cell anemia and thalassemia major. Am J Hematol 1993, 42:81–85.
Nielsen P, Fischer R, Engelhardt R, et al.: Liver iron stores in patients with secondary haemosiderosis under iron chelation therapy with deferoxamine or deferiprone. Br J Haematol 1995, 91:827–833.
Jensen PD, Jensen FT, Christensen T, Ellegaard J: Evaluation of transfusional iron overload before and during iron chelation by magnetic resonance imaging of the liver and determination of serum ferritin in adult non-thalassaemic patients. Br J Haematol 1995, 89:880–889.
Jensen PD, Jensen FT, Christensen T, et al.: Relationship between hepatocellular injury and transfusional iron overload prior to and during iron chelation with desferrioxamine: a study in adult patients with acquired anemias. Blood 2003, 101:91–96.
Jensen PD, Jensen FT, Christensen T, et al.: Indirect evidence for the potential ability of magnetic resonance imaging to evaluate the myocardial iron content in patients with transfusional iron overload. Magma 2001, 12:153–166.
Jensen PD, Jensen FT, Christensen T, et al.: Evaluation of myocardial iron by magnetic resonance imaging during iron chelation therapy with deferrioxamine: indication of close relation between myocardial iron content and chelatable iron pool. Blood 2003, 101:4632–4639.
Brittenham GM, Griffith PM, Nienhuis AW, et al.: Efficacy of deferoxamine in preventing complications of iron overload in patients with thalassemia major. N Engl J Med 1994, 331:567–573.
Engle MA, Erlandson M, Smith CH: Late cardiac complications of chronic severe, refractory anaemia with hemochromatosis. Circulation 1964, 30:698–705.
Schafer AI, Cheron RG, Dluhy R, et al.: Clinical consequences of acquired transfusional iron overload in adults. N Engl J Med 1981, 304:319–324.
Jaeger M, Aul C, Sohngen D, et al.: Secondary hemochromatosis in polytransfused patients with myelodysplastic syndromes] [German]. Beitr Infusionsther 1992, 30:464–468.
Cohen A, Martin M, Schwartz E: Depletion of excessive liver iron stores with desferrioxamine. Br J Haematol 1984, 58:369–373.
Freeman AP, Giles RW, Berdoukas VA, et al.: Sustained normalization of cardiac function by chelation therapy in thalassaemia major. Clin Lab Haematol 1989, 11:299–307.
Wolfe L, Olivieri N, Sallan D, et al.: Prevention of cardiac disease by subcutaneous deferoxamine in patients with thalassemia major. N Engl J Med 1985, 312:1600–1603.
De Sanctis V, Zurlo MG, Senesi E, et al.: Insulin dependent diabetes in thalassaemia. Arch Dis Child 1988, 63:58–62.
Bronspiegel-Weintrob N, Olivieri NF, Tyler B, et al.: Effect of age at the start of iron chelation therapy on gonadal function in beta-thalassemia major. N Engl J Med 1990, 323:713–719.
Olivieri NF, Nathan DG, MacMillan JH, et al.: Survival in medically treated patients with homozygous beta-thalassemia. N Engl J Med 1994, 331:574–578.
Olivieri NF, Brittenham GM: Iron-chelation therapy and the treatment of thalassemia. Blood 1997, 89:739–761.
Schafer AI, Rabinowe S, Le Boff MS, et al.: Long-term efficacy of deferoxamine iron chelation therapy in adults with acquired transfusional iron overload. Arch Intern Med 1985, 145:1217–1221.
Di Gregorio F, Romeo MA, Pizzarelli G, et al.: An alternative to continuous subcutaneous infusion of desferrioxamine in thalassaemic patients. Br J Haematol 1997, 98:601–602.
Borgna-Pignatti C, Franchini M, Gandini G, et al.: Subcutaneous bolus injection of deferoxamine in adult patients affected by onco-hematologic diseases and iron overload. Haematologica 1998, 83:788–790.
Franchini M, Gandini G, de Gironcoli M, et al.: Safety and efficacy of subcutaneous bolus injection of deferoxamine in adult patients with iron overload. Blood 2000, 95:2776–2779.
Jensen PD, Heickendorff L, Pedersen B, et al.: The effect of iron chelation on haemopoiesis in MDS patients with transfusional iron overload. Br J Haematol 1996, 94:288–299.
Porter JB, Davis BA: Monitoring chelation therapy to achieve optimal outcome in the treatment of thalassaemia [review]. Best Pract Res Clin Haematol 2002, 15:329–368.
Haines ME, Wainscoat JS: Relapsing sideroblastic anaemia. Br J Haematol 1991, 78:285–286.
Del Rio Garma J, Fernandez Lago C, Batlle Fonrodona FJ: Desferrioxamine in the treatment of myelodysplastic syndromes. Haematologica 1997, 82:639–640.
Cortelezzi A, Cattaneo C, Cristiani S, et al.: Non-transferrin-bound iron in myelodysplastic syndromes: a marker of ineffective erythropoiesis? Hematol J 2000, 1:153–158.
Cohen AR, Galanello R, Piga A, et al: Safety and effectiveness of long-term therapy with the oral iron chelator deferiprone. Blood 2003, 102:1583–1587.
Hoffbrand AV, Cohen A, Hershko C: Role of deferiprone in chelation therapy for transfusional iron overload. Blood 2003, 102:17–24.
Wonke B, Wright C, Hoffbrand AV: Combined therapy with deferiprone and desferrioxamine. Br J Haematol 1998, 103:361–364.
Anderson LJ, Wonke B, Prescott E, et al.: Comparison of effect of oral deferiprone and subcutaneous desferrioxamine on myocardial iron concentrations and ventricular function in beta-thalassaemia. Lancet 2002, 360:516–520.
Borgna-Pignatti C, Cappellini MD, De Stefano P, et al.: Cardiac morbidity and mortality in deferoxamine-or deferiprone-treated patients with thalassemia major. Blood 2006, 107:3733–3737.
Kersten MJ, Lange R, Smeets ME, et al.: Long-term treatment of transfusional iron overload with the oral iron chelator deferiprone (L1): a Dutch multicenter trial. Ann Hematol 1996, 73:247–252.
Nisbet-Brown E, Olivieri NF, Giardina PJ, et al.: Effectiveness and safety of ICL670 in iron-loaded patients with thalassaemia: a randomised, double-blind, placebo-controlled, dose-escalation trial. Lancet 2003, 361:1597–1602.
Nick H, Wong A, Acklin P, et al.: ICL670A: preclinical profile. Adv Exp Med Biol 2002, 509:185–203.
Cappellini MD: Iron-chelating therapy with the new oral agent ICL670 (Exjade). Best Pract Res Clin Haematol 2005, 18:289–298.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Jensen, PD. Iron overload in patients with myelodysplastic syndromes. Curr Hematol Malig Rep 2, 13–21 (2007). https://doi.org/10.1007/s11899-007-0003-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11899-007-0003-5