Abstract
Background
Dietary advice is a standard component of treatment for pregnant women with impaired glucose tolerance (IGT) and gestational diabetes (GDM), yet few studies report glycemic profiles in response to dietary therapies and the optimal dietary approach remains uncertain.
Aim
To assess changes in maternal glycemic profile and pregnancy outcomes among women with diet-controlled IGT and GDM.
Methods
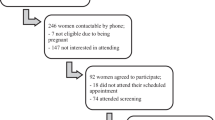
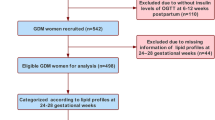
Pregnant women who had one or more elevated values on a 3-h oral glucose tolerance test were enrolled. All participants received dietary advice and glucose monitoring as part of routine clinical care. Fasting and 1-h post-prandial blood samples, collected prior to initiation of clinical treatment and repeated 4–6 weeks later, were analyzed for glucose, insulin, and C-peptide. Homeostasis model assessment of insulin resistance (HOMA-IR) was calculated. Women who required pharmacological therapy for glucose control were excluded from analyses.
Results
Participants (N = 93) were of moderately older age (mean 33 years), with a high rate of overweight/obesity (mean body mass index (BMI) = 28.65 kg/m2), and were diagnosed late in gestation (mean 29 weeks). Fasting (mean ± SD 4.82 ± 0.53 to 4.60 ± 0.42 mmol/l; p < 0.001) and post-prandial glucose (7.01 ± 1.19 to 6.47 ± 1.10; p = 0.004) decreased significantly following the intervention. Baseline HOMA-IR was elevated (3.12 ± 1.03) but did not significantly decrease (2.78 ± 1.52; p = 0.066). There were high rates of macrosomia (24.7%) and cesarean delivery (32.3%).
Conclusions
Although improvements in blood glucose levels were observed among women with diet-controlled IGT and GDM, this was insufficient to significantly affect insulin resistance or perinatal outcome. Late diagnosis and treatment of IGT/GDM may have contributed to such outcomes.
Similar content being viewed by others
References
Bulletin ACOGP (2013) No. 137: gestational diabetes mellitus. Obstet Gynecol 122:406–416
Kim C (2010) Gestational diabetes: risks, management, and treatment options. Int J Womens Health 2:339–351. https://doi.org/10.2147/IJWH.S13333
Alwan N, Tuffnell DJ, West J (2009) Treatments for gestational diabetes. Cochrane Database Syst Rev :Cd003395, DOI: https://doi.org/10.1002/14651858.CD003395.pub2
Landon MB, Spong CY, Thom E, Carpenter MW, Ramin SM, Casey B, Wapner RJ, Varner MW, Rouse DJ, Thorp JM Jr, Sciscione A, Catalano P, Harper M, Saade G, Lain KY, Sorokin Y, Peaceman AM, Tolosa JE, Anderson GB, Eunice Kennedy Shriver National Institute of Child Health and Human Development Maternal-Fetal Medicine Units Network (2009) A multicenter, randomized trial of treatment for mild gestational diabetes. N Engl J Med 361(14):1339–1348. https://doi.org/10.1056/NEJMoa0902430
Kim C, Newton KM, Knopp RH (2002) Gestational diabetes and the incidence of type 2 diabetes: a systematic review. Diabetes Care 25(10):1862–1868. https://doi.org/10.2337/diacare.25.10.1862
Perkins JM, Dunn JP, Jagasia SM (2007) Perspectives in gestational diabetes mellitus: a review of screening, diagnosis, and treatment. Clinical Diabetes 25(2):57–62. https://doi.org/10.2337/diaclin.25.2.57
Han S, Crowther CA, Middleton P, Heatley E (2013) Different types of dietary advice for women with gestational diabetes mellitus. Cochrane Database Syst Rev 3:Cd009275. https://doi.org/10.1002/14651858.CD009275.pub2
Lapolla A, Dalfra MG, Fedele D (2009) Management of gestational diabetes mellitus. Diabetes Metab Syndr Obes 2:73–82. https://doi.org/10.2147/DMSO.S3407
Poolsup N, Suksomboon N, Amin M (2014) Effect of treatment of gestational diabetes mellitus: a systematic review and meta-analysis. PLoS One 9(3):e92485. https://doi.org/10.1371/journal.pone.0092485
Viana LV, Gross JL, Azevedo MJ (2014) Dietary intervention in patients with gestational diabetes mellitus: a systematic review and meta-analysis of randomized clinical trials on maternal and newborn outcomes. Diabetes Care 37(12):3345–3355. https://doi.org/10.2337/dc14-1530
Health Service Executive (2010) Guidelines for the management of pre-gestational and gestational diabetes mellitus from pre-conception to the postnatal period. Health Service Executive: Dublin
National Collaborating Centre for Women’s and Children’s Health (2015) Diabetes in pregnancy: management of diabetes and its complications from pre-conception to the postnatal period, Version 2.1. National Institute of Clinical Excellence: London
American Diabetes Association (2015) Management of diabetes in pregnancy. Diabetes Care 38(Supplement_1):S77–S79. https://doi.org/10.2337/dc15-S015
Crowther CA, Hiller JE, Moss JR, McPhee AJ, Jeffries WS, Robinson JS, Australian Carbohydrate Intolerance Study in Pregnant Women (ACHOIS) Trial Group (2005) Effect of treatment of gestational diabetes mellitus on pregnancy outcomes. N Engl J Med 352(24):2477–2486. https://doi.org/10.1056/NEJMoa042973
Hernandez TL, Anderson MA, Chartier-Logan C, Friedman JE, Barbour LA (2013) Strategies in the nutritional management of gestational diabetes. Clin Obstet Gynecol 56(4):803–815. https://doi.org/10.1097/GRF.0b013e3182a8e0e5
Lindsay KL, Brennan L, Kennelly MA, Maguire OC, Smith T, Curran S et al (2015) Impact of probiotics in women with gestational diabetes mellitus on metabolic health: a randomized controlled trial. Am J Obstet Gynecol 212:496.e1–496.11
Carpenter MW, Coustan DR (1982) Criteria for screening tests for gestational diabetes. Am J Obstet Gynecol 144(7):768–773. https://doi.org/10.1016/0002-9378(82)90349-0
Matthews DR, Hosker JP, Rudenski AS, Naylor BA, Treacher DF, Turner RC (1985) Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 28(7):412–419. https://doi.org/10.1007/BF00280883
Laopaiboon M, Lumbiganon P, Intarut N, Mori R, Ganchimeg T, Vogel JP, Souza JP, Gülmezoglu AM, WHO Multicountry Survey on Maternal Newborn Health Research Network (2014) Advanced maternal age and pregnancy outcomes: a multicountry assessment. BJOG 121 Suppl 1:49–56. https://doi.org/10.1111/1471-0528.12659
International Association of Diabetes in Pregnancy Study Groups Consensus Panel, Metzger BE, Gabbe SG, Persson B, Buchanan TA et al (2010) International association of diabetes and pregnancy study groups recommendations on the diagnosis and classification of hyperglycemia in pregnancy. Diabetes Care 33:676–682
Grant SM, Wolever TM, O'Connor DL, Nisenbaum R, Josse RG (2011) Effect of a low glycaemic index diet on blood glucose in women with gestational hyperglycaemia. Diabetes Res Clin Pract 91(1):15–22. https://doi.org/10.1016/j.diabres.2010.09.002
Carolan M, Davey MA, Biro MA, Kealy M (2012) Maternal age, ethnicity and gestational diabetes mellitus. Midwifery 28(6):778–783. https://doi.org/10.1016/j.midw.2011.08.014
Shah A, Stotland NE, Cheng YW, Ramos GA, Caughey AB (2011) The association between body mass index and gestational diabetes mellitus varies by race/ethnicity. Am J Perinatol 28(07):515–520. https://doi.org/10.1055/s-0031-1272968
Catalano PM (2010) Obesity, insulin resistance, and pregnancy outcome. Reproduction 140(3):365–371. https://doi.org/10.1530/REP-10-0088
Butte NF (2000) Carbohydrate and lipid metabolism in pregnancy: normal compared with gestational diabetes mellitus. Am J Clin Nutr 71(5 Suppl):1256S–1261S
Herrera E (2000) Metabolic adaptations in pregnancy and their implications for the availability of substrates to the fetus. Eur J Clin Nutr 54(Suppl 1):S47–S51. https://doi.org/10.1038/sj.ejcn.1600984
Catalano PM, Tyzbir ED, Wolfe RR, Calles J, Roman NM, Amini SB et al (1993) Carbohydrate metabolism during pregnancy in control subjects and women with gestational diabetes. Am J Phys 264:E60–E67
Nelson SM, Matthews P, Poston L (2010) Maternal metabolism and obesity: modifiable determinants of pregnancy outcome. Hum Reprod Update 16(3):255–275. https://doi.org/10.1093/humupd/dmp050
McFarland MB, Trylovich CG, Langer O (1998) Anthropometric differences in macrosomic infants of diabetic and nondiabetic mothers. J Matern Fetal Med 7(6):292–295. https://doi.org/10.1002/(SICI)1520-6661(199811/12)7:6<292::AID-MFM7>3.0.CO;2-A
Schaefer-Graf UM, Graf K, Kulbacka I, Kjos SL, Dudenhausen J, Vetter K (2008) Maternal lipids as strong determinants of fetal environment and growth in pregnancies with gestational diabetes mellitus. Diabetes Care 31(9):1858–1863. https://doi.org/10.2337/dc08-0039
Friedman JE (2015) Obesity and gestational diabetes mellitus pathways for programming in mouse, monkey, and man—where do we go next? The 2014 Norbert Freinkel Award Lecture. Diabetes Care 38(8):1402–1411. https://doi.org/10.2337/dc15-0628
Catalano PM, McIntyre HD, Cruickshank JK, McCance DR, Dyer AR, Metzger BE, Lowe LP, Trimble ER, Coustan DR, Hadden DR, Persson B, Hod M, Oats JJN, for the HAPO Study Cooperative Research Group (2012) The hyperglycemia and adverse pregnancy outcome study: associations of GDM and obesity with pregnancy outcomes. Diabetes Care 35(4):780–786. https://doi.org/10.2337/dc11-1790
Weissmann-Brenner A, Simchen MJ, Zilberberg E, Kalter A, Weisz B, Achiron R, Dulitzky M (2012) Maternal and neonatal outcomes of macrosomic pregnancies. Med Sci Monit 18(9):Ph77–Ph81
Das S, Irigoyen M, Patterson MB, Salvador A, Schutzman DL (2009) Neonatal outcomes of macrosomic births in diabetic and non-diabetic women. Arch Dis Child Fetal Neonatal Ed 94(6):F419–F422. https://doi.org/10.1136/adc.2008.156026
Boney CM, Verma A, Tucker R, Vohr BR (2005) Metabolic syndrome in childhood: association with birth weight, maternal obesity, and gestational diabetes mellitus. Pediatrics 115(3):e290–e296. https://doi.org/10.1542/peds.2004-1808
Ornoy A (2011) Prenatal origin of obesity and their complications: gestational diabetes, maternal overweight and the paradoxical effects of fetal growth restriction and macrosomia. Reprod Toxicol 32(2):205–212. https://doi.org/10.1016/j.reprotox.2011.05.002
Ali S, Dornhorst A (2011) Diabetes in pregnancy: health risks and management. Postgrad Med J 87(1028):417–427. https://doi.org/10.1136/pgmj.2010.109157
Sinnott S-J, Brick A, Layte R, Cunningham N, Turner MJ (2016) National variation in caesarean section rates: a cross sectional study in Ireland. PLoS One 11(6):e0156172. https://doi.org/10.1371/journal.pone.0156172
Kgosidialwa O, Egan AM, Carmody L, Kirwan B, Gunning P, Dunne FP (2015) Treatment with diet and exercise for women with gestational diabetes mellitus diagnosed using IADPSG criteria. J Clin Endocrinol Metab 100(12):4629–4636. https://doi.org/10.1210/jc.2015-3259
Funding
This research was funded by the National Maternity Hospital Medical Fund with support from the Ivo Drury Award and The European Union’s Seventh Framework Programme (FP7/2007–2013), project EarlyNutrition under grant agreement no. 289346. The funding sources had no role in the study design, data collection, interpretation or analysis, writing of the manuscript, or decision to submit for publication.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The study received full institutional ethical approval and written informed consent was obtained from all individual participants included in the study
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Lindsay, K.L., Brennan, L., Kennelly, M.A. et al. Maternal metabolic response to dietary treatment for impaired glucose tolerance and gestational diabetes mellitus. Ir J Med Sci 187, 701–708 (2018). https://doi.org/10.1007/s11845-018-1744-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11845-018-1744-y