Abstract
Background
Radical prostatectomy for prostate cancer is associated with significant complications, such as urinary incontinence and erectile dysfunction. Debate remains regarding the influence of surgical technique on these important functional outcomes.
Aim
The aim of this study was to compare the early functional outcomes following robotic-assisted (RARP), laparoscopic (LRP), and open radical prostatectomy (ORP) in a rapid access cohort.
Methods
A retrospective review of a prospectively maintained database was performed between 2011 and 2014. Functional status was objectively assessed using the International Prostate Symptom Score (IPSS), International Index of Erectile Function (IIEF-5), and a self-reported continence score.
Results
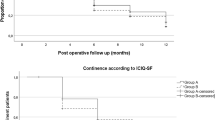
Two hundred and ninety-two patients underwent RP (85 RARP, 100 LRP, 107 ORP). The mean age was 61.3 years with a mean initial PSA was 6.2 ng/ml. There was no difference noted in urinary function between ORP, LRP, and RARP at 3 months (p = 0.894), 6 months (p = 0.244), 9 months (p = 0.068) or 12 months (p = 0.154). All men noted a deterioration in erectile function; however, there was no difference at 3 months (p = 0.922), 6 months (p = 0.723), 9 months (p = 0.101) or 12 months (p = 0.395),
Conclusion
Equivalent good early functional outcomes are being achieved in patients undergoing RP irrespective of surgical approach. Longer follow-up in a prospective randomized fashion is required to fully assess the most appropriate surgical technique.
Similar content being viewed by others
References
Siegel R, Naishadham D, Jemal A (2012) Cancer statistics, 2012. CA Cancer J Clin 62:10–29
Heidenreich A, Bastian PJ, Bellmunt J et al (2014) EAU guidelines on prostate cancer. part 1: screening, diagnosis, and local treatment with curative intent-update 2013. Eur Urol 65(1):124–137
Raina R, Pahlajani G, Agarwal A et al (2010) Long term potency after early use of a vacuum erection device following radical prostatectomy. BJU Int 106:1719–1722
Defade BP, Carson CC 3rd, Kennelly MJ (2011) Postprostatectomy erectile dysfunction: the role of penile rehabilitation. Rev Urol. 13(1):6–13
Kim PH, Pinheiro LC, Atoria CL et al (2013) Trends in the use of incontinence procedures after radical prostatectomy: a population based analysis. J Urol 189(2):602–608
Schuessler WW, Schulam PG, Clayman RV et al (1997) Laparoscopic radical prostatectomy: initial short-term experience. Urology. 50(6):854–857
Pasticier G, Rietbergen JB, Guillonneau B et al (2001) Robotically assisted laparoscopic radical prostatectomy: feasibility study in men. Eur Urol 40(1):70–74
Akand M, Celik O, Avci E et al (2015) Open, laparoscopic and robot-assisted laparoscopic radical prostatectomy: comparative analysis of operative and pathologic outcomes for three techniques with a single surgeon’s experience. Eur Rev Med Pharmacol Sci. 19(4):525–531
Hakimi AA, Feder M, Ghavamian R (2007) Minimally invasive approaches to prostate cancer: a review of the current literature. Urol J. 4(3):130–137
Yaxley JW, Coughlin GD, Chambers SK et al (2016) Robot-assisted laparoscopic prostatectomy versus open radical retropubic prostatectomy: early outcomes from a randomised controlled phase 3 study. Lancet 388(10049):1057–1066
Guillonneau B, Vallancien G (2000) Laparoscopic radical prostatectomy: the Montsouris experience. J Urol 163(2):418–422
Ramirez D, Zargar H, Caputo P et al (2015) Robotic-assisted laparoscopic prostatectomy: An update on functional and oncologic outcomes, techniques, and advancements in technology. J Surg Oncol 112(7):746–752
Ahlering TE, Woo D, Eichel L et al (2004) Robot-assisted versus open radical prostatectomy: a comparison of one surgeon’s outcomes. Urology. 63(5):819–822
Touijer K, Kuroiwa K, Eastham JA et al (2007) Risk-adjusted analysis of positive surgical margins following laparoscopic and retropubic radical prostatectomy. Eur Urol 52:1090
Barocas DA, Salem S, Kordan Y et al (2010) Robotic assisted laparoscopic prostatectomy versus radical retropubic prostatectomy for clinically localized prostate cancer: comparison of short-term biochemical recurrence-free survival. J Urol 183:990
Haglind E, Carlsson S, Stranne J et al (2015) Urinary incontinence and erectile dysfunction after robotic versus open radical prostatectomy: a prospective, controlled, nonrandomised trial. Eur Urol. 68(2):216–225
Barry MJ, Gallagher PM, Skinner JS et al (2012) Adverse effects of robotic-assisted laparoscopic versus open retropubic radical prostatectomy among a nationwide random sample of medicare-age men. J Clin Oncol 30(5):513–518
Ficarra V, Novara G, Fracalanza S et al (2009) A prospective, non-randomized trial comparing robot-assisted laparoscopic and retropubic radical prostatectomy in one European institution. BJU Int 104(4):534–539
O’Neil B, Koyama T, Alvarez J et al (2016) The comparative harms of open and robotic prostatectomy in population-based samples. J Urol 195(2):321–329
Lee JK, Assel M, Thong AE et al (2015) Unexpected long-term improvements in urinary and erectile function in a large cohort of men with self-reported outcomes following radical prostatectomy. Eur Urol 68(5):899–905
Herrell SD, Smith JA (2005) Robotic-assisted laparoscopic prostatectomy: what is the learning curve? J Urol 66:105–107
Thompson JE, Egger S, Bohm M et al (2014) Superior quality of life and improved surgical margins are achievable with robotic radical prostatectomy after a long learning curve: a prospective single-surgeon study of 1552 consecutive cases. Eur Urol 65:521–531
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Ethical approval
The proposed study received ethical approval from the departmental research meeting of the university teaching hospital. All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Rights and permissions
About this article
Cite this article
Nason, G.J., O’Kelly, F., White, S. et al. Patient reported functional outcomes following robotic-assisted (RARP), laparoscopic (LRP), and open radical prostatectomies (ORP). Ir J Med Sci 186, 835–840 (2017). https://doi.org/10.1007/s11845-016-1522-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11845-016-1522-7