Abstract
Background
The various uses of biological valves for either aortic or mitral valve replacement have recently increased because of the growing proportion of elderly patients requiring surgery.
Results
The durability of recent xenografts has been reported to be over 90 % at 10 years after aortic or mitral valve replacement for elderly patients more than 65 years of age, and therefore the guidelines now recommend the use of bioprostheses for patients over 65 years of age. Bioprostheses are also recommended for valve replacement of the right side of the heart by several authors; however, no clear guidelines are available. Trans-catheter aortic valve replacement and percutaneous pulmonary valve implantation are promising procedures for high-risk patients, although evaluation of the long-term durability of these valves is mandatory.
Conclusions
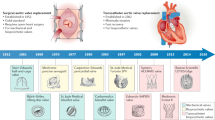
This article will review the development of the tissue valve for valve surgery.
Similar content being viewed by others
References
Bonow RO, Carabello BA, Chatterjee K, De Leon AC Jr, Faxon DP, Freed MD, et al. Focused update incorporated into the ACC/AHA 2006 guidelines for the management of patients with valvular heart disease: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to Revise the 1998 Guidelines for the Management of Patients With Valvular Heart Disease): endorsed by the Society of Cardiovascular Anesthesiologists, Society for Cardiovascular Angiography and Interventions, and Society of Thoracic Surgeons. Circulation 2008;118:e523–661.
Kuwano H, Amano J, Yokomise H. Thoracic and cardiovascular surgery in Japan during 2010: annual report by The Japanese Association for Thoracic Surgery. Gen Thorac Cardiovasc Surg. 2012;60:680–708.
Yasui H, Osada H, Ando N, Koyanagi H. Thoracic and cardiovascular surgery in Japan during 1996: annual report by the Japanese Association for Thoracic Surgery. Committee of science. Jpn J Thorac Cardiovasc Surg. 1998;46:406–20.
Revuelta JM, Alonso C, Cagigas JC, Lequerica MA, Gaite L, Herrera S, et al. Long-term evaluation of the Ionescu-Shiley pericardial xenograft bioprosthesis in the aortic position. J Card Surg. 1988;3:391–6.
Cohn LH, Collins JJ Jr, DiSesa VJ, Couper GS, Peigh PS, Kowalker W, et al. Fifteen-year experience with 1678 Hancock porcine bioprosthetic heart valve replacements. Ann Surg. 1989;210:435–42. (discussion 42–3).
Kirali K, Guler M, Tuncer A, Daglar B, Ipek G, Isik O, et al. Fifteen-year clinical experience with the biocor porcine bioprostheses in the mitral position. Ann Thorac Surg. 2001;71:811–5.
Jamieson WR, Burr LH, Miyagishima RT, Germann E, Macnab JS, Stanford E, et al. Carpentier-Edwards supra-annular aortic porcine bioprosthesis: clinical performance over 20 years. J Thorac Cardiovasc Surg. 2005;130:994–1000.
Borger MA, Ivanov J, Armstrong S, Christie-Hrybinsky D, Feindel CM, David TE. Twenty-year results of the Hancock II bioprosthesis. J Heart Valve Dis. 2006;15:49–55. (discussion-6).
Rizzoli G, Mirone S, Ius P, Polesel E, Bottio T, Salvador L, et al. Fifteen-year results with the Hancock II valve: a multicenter experience. J Thorac Cardiovasc Surg. 2006;132:602–9. 9 e1-4.
Eichinger WB, Hettich IM, Ruzicka DJ, Holper K, Schricker C, Bleiziffer S, et al. Twenty-year experience with the St. Jude medical Biocor bioprosthesis in the aortic position. Ann Thorac Surg. 2008;86:1204–10.
Jamieson WR, Gudas VM, Burr LH, Janusz MT, Fradet GJ, Ling H, et al. Mitral valve disease: if the mitral valve is not reparable/failed repair, is bioprosthesis suitable for replacement? Eur J Cardiothorac Surg. 2009;35:104–10.
Myken PS, Bech-Hansen O. A 20-year experience of 1712 patients with the Biocor porcine bioprosthesis. J Thorac Cardiovasc Surg. 2009;137:76–81.
Chan V, Kulik A, Tran A, Hendry P, Masters R, Mesana TG, et al. Long-term clinical and hemodynamic performance of the Hancock II versus the Perimount aortic bioprostheses. Circ. 2010;122:S10–6.
Riess FC, Cramer E, Hansen L, Schiffelers S, Wahl G, Wallrath J, et al. Clinical results of the Medtronic Mosaic porcine bioprosthesis up to 13 years. Eur J Cardiothorac Surg. 2010;37:145–53.
Jamieson WR, Lewis CT, Sakwa MP, Cooley DA, Kshettry VR, Jones KW, et al. St. Jude Medical Epic porcine bioprosthesis: results of the regulatory evaluation. J Thorac Cardiovasc Surg. 2011;141:1449–54. e2.
Jamieson WR, Riess FC, Raudkivi PJ, Metras J, Busse EF, Goldstein J, et al. Medtronic Mosaic porcine bioprosthesis: assessment of 12-year performance. J Thorac Cardiovasc Surg. 2011;142:302–7. e2.
Celiento M, Ravenni G, Milano AD, Pratali S, Scioti G, Nardi C, et al. Aortic valve replacement with the Medtronic Mosaic bioprosthesis: a 13-year follow-up. Ann Thorac Surg. 2012;93:510–5.
Ruggieri VG, Flecher E, Anselmi A, Lelong B, Corbineau H, Verhoye JP, et al. Long-Term Results of the Carpentier-Edwards Supraannular Aortic Valve Prosthesis. Ann Thorac Surg. 2012;94:1191–7.
Ayegnon KG, Aupart M, Bourguignon T, Mirza A, May MA, Marchand M. A 25-year experience with Carpentier-Edwards Perimount in the mitral position. Asian Cardiovasc Thorac Ann. 2011;19:14–9.
Dellgren G, David TE, Raanani E, Armstrong S, Ivanov J, Rakowski H. Late hemodynamic and clinical outcomes of aortic valve replacement with the Carpentier-Edwards Perimount pericardial bioprosthesis. J Thorac Cardiovasc Surg. 2002;124:146–54.
Jamieson WR, Germann E, Aupart MR, Neville PH, Marchand MA, Fradet GJ. 15-year comparison of supra-annular porcine and PERIMOUNT aortic bioprostheses. Asian Cardiovasc Thorac Ann. 2006;14:200–5.
Marchand MA, Aupart MR, Norton R, Goldsmith IR, Pelletier LC, Pellerin M, et al. Fifteen-year experience with the mitral Carpentier-Edwards PERIMOUNT pericardial bioprosthesis. Ann Thorac Surg. 2001;71:S236–9.
Minami K, Zittermann A, Schulte-Eistrup S, Koertke H, Korfer R. Mitroflow synergy prostheses for aortic valve replacement: 19 years experience with 1,516 patients. Ann Thorac Surg. 2005;80:1699–705.
Yankah CA, Pasic M, Musci M, Stein J, Detschades C, Siniawski H, et al. Aortic valve replacement with the Mitroflow pericardial bioprosthesis: durability results up to 21 years. J Thorac Cardiovasc Surg. 2008;136:688–96.
Wheatley DJ, Fisher J, Reece IJ, Spyt T, Breeze P. Primary tissue failure in pericardial heart valves. J Thorac Cardiovasc Surg. 1987;94:367–74.
Bortolotti U, Milano A, Mazzucco A, Guerra F, Valente M, Thiene G, et al. The Hancock pericardial xenograft: incidence of early mechanical failures at a medium-term follow-up. Eur J Cardiothorac Surg. 1988;2:458–64.
Bortolotti U, Milano A, Guerra F, Mazzucco A, Mossuto E, Thiene G, et al. Failure of Hancock pericardial xenografts: is prophylactic bioprosthetic replacement justified? Ann Thorac Surg. 1991;51:430–7.
Gabbay S, Bortolotti U, Wasserman F, Tindel N, Factor SM, Frater RW. Long-term follow-up of the Ionescu-Shiley mitral pericardial xenograft. J Thorac Cardiovasc Surg. 1984;88:758–63.
Ionescu MI, Tandon AP, Chidambaram M, Yakirevich VS, Silverton NP. Durability of the pericardial valve. Eur Heart J. 1984;5 Suppl D:101–6.
Gallo I, Nistal F, Revuelta JM, Garcia-Satue E, Artinano E, Duran CG. Incidence of primary tissue valve failure with the Ionescu-Shiley pericardial valve. Preliminary results. J Thorac Cardiovasc Surg. 1985;90:278–80.
Jamieson WR, Janusz MT, MacNab J, Henderson C. Hemodynamic comparison of second- and third-generation stented bioprostheses in aortic valve replacement. Ann Thorac Surg. 2001;71:S282–4.
David TE, Pollick C, Bos J. Aortic valve replacement with stentless porcine aortic bioprosthesis. J Thorac Cardiovasc Surg. 1990;99:113–8.
Elkins RC, Thompson DM, Lane MM, Elkins CC, Peyton MD. Ross operation: 16-year experience. J Thorac Cardiovasc Surg. 2008;136(623–30):e5.
de Kerchove L, Rubay J, Pasquet A, Poncelet A, Ovaert C, Pirotte M, et al. Ross operation in the adult: long-term outcomes after root replacement and inclusion techniques. Ann Thorac Surg. 2009;87:95–102.
David TE, Omran A, Ivanov J, Armstrong S, de Sa MP, Sonnenberg B, et al. Dilation of the pulmonary autograft after the Ross procedure. J Thorac Cardiovasc Surg. 2000;119:210–20.
Brown JW, Fehrenbacher JW, Ruzmetov M, Shahriari A, Miller J, Turrentine MW. Ross root dilation in adult patients: is preoperative aortic insufficiency associated with increased late autograft reoperation? Ann Thorac Surg. 2011;92:74–81 (discussion).
Ross DN. Homograft replacement of the aortic valve. Lancet. 1962;2:487.
Ali A, Abu-Omar Y, Patel A, Sheikh AY, Ali Z, Saeed A, et al. Propensity analysis of survival after subcoronary or root replacement techniques for homograft aortic valve replacement. J Thorac Cardiovasc Surg. 2009;137:334–41.
Vogt F, Kowert A, Beiras-Fernandez A, Oberhoffer M, Kaczmarek I, Reichart B, et al. Pulmonary homografts for aortic valve replacement: long-term comparison with aortic grafts. Heart Surg Forum. 2011;14:E237–41.
Bortolotti U, Milano A, Thiene G, Guerra F, Mazzucco A, Valente M, et al. Early mechanical failures of the Hancock pericardial xenograft. J Thorac Cardiovasc Surg. 1987;94:200–7.
Thiene G, Bortolotti U, Valente M, Milano A, Calabrese F, Talenti E, et al. Mode of failure of the Hancock pericardial valve xenograft. Am J Cardiol. 1989;63:129–33.
Gabbay S, Bortolotti U, Wasserman F, Factor S, Strom J, Frater RW. Fatigue-induced failure of the Ionescu-Shiley pericardial xenograft in the mitral position. In vivo and in vitro correlation and a proposed classification. J Thorac Cardiovasc Surg. 1984;87:836–44.
Goldman B, Scully H, Tong C, Mandell R, Butany J, Azuma J, et al. Clinical results of pericardial xenograft valves: the Ionescu-Shiley and Hancock valves. Can J Cardiol. 1988;4:328–32.
Wells SM, Sacks MS. Effects of fixation pressure on the biaxial mechanical behavior of porcine bioprosthetic heart valves with long-term cyclic loading. Biomaterials. 2002;23:2389–99.
Vesely I. Analysis of the medtronic intact bioprosthetic valve. Effects of “zero-pressure” fixation. J Thorac Cardiovasc Surg. 1991;101:90–9.
Cohn LH, Collins JJ Jr, Rizzo RJ, Adams DH, Couper GS, Aranki SF. Twenty-year follow-up of the Hancock modified orifice porcine aortic valve. Ann Thorac Surg. 1998;66:S30–4.
Said SM, Ashikhmina E, Greason KL, Suri RM, Park SJ, Daly RC, et al. Do pericardial bioprostheses improve outcome of elderly patients undergoing aortic valve replacement? Ann Thorac Surg. 2012;93:1868–74. (discussion 74–5).
David TE, Bos J, Rakowski H. Aortic valve replacement with the Toronto SPV bioprosthesis. J Heart Valve Dis. 1992;1:244–8.
David TE, Puschmann R, Ivanov J, Bos J, Armstrong S, Feindel CM, et al. Aortic valve replacement with stentless and stented porcine valves: a case-match study. J Thorac Cardiovasc Surg. 1998;116:236–41.
El-Hamamsy I, Clark L, Stevens LM, Sarang Z, Melina G, Takkenberg JJ, et al. Late outcomes following freestyle versus homograft aortic root replacement: results from a prospective randomized trial. J Am Coll Cardiol. 2010;55:368–76.
Ennker JA, Ennker IC, Albert AA, Rosendahl UP, Bauer S, Florath I. The Freestyle stentless bioprosthesis in more than 1000 patients: a single-center experience over 10 years. J Card Surg. 2009;24:41–8.
Oosterlinck W, Meuris B, Herregods MC, Vandeplas A, Daenen W, Flameng W, et al. Long-term results with a stentless porcine aortic valve: the Edwards PRIMA model 2500. J Heart Valve Dis. 2009;18:198–206.
Auriemma S, D’Onofrio A, Brunelli M, Magagna P, Paccanaro M, Rulfo F, et al. Long-term results of aortic valve replacement with Edwards Prima Plus stentless bioprosthesis: eleven years’ follow up. J Heart Valve Dis. 2006;15:691–5 (discussion 5).
O’Brien MF, Gardner MA, Garlick B, Jalali H, Gordon JA, Whitehouse SL, et al. CryoLife-O’Brien stentless valve: 10-year results of 402 implants. Ann Thorac Surg. 2005;79:757–66.
Desai ND, McCarthy F, Moser W, Szeto WY, Zeeshan A, Brown D, et al. Durability of porcine bioroots in younger patients with aortic root pathology: a propensity-matched comparison with composite mechanical roots. Ann Thorac Surg. 2011;92:2054–60 (discussion 60-1).
Cohen G, Zagorski B, Christakis GT, Joyner CD, Vincent J, Sever J, et al. Are stentless valves hemodynamically superior to stented valves? Long-term follow-up of a randomized trial comparing Carpentier-Edwards pericardial valve with the Toronto stentless porcine valve. J Thorac Cardiovasc Surg. 2010;139:848–59.
Ali A, Halstead JC, Cafferty F, Sharples L, Rose F, Lee E, et al. Early clinical and hemodynamic outcomes after stented and stentless aortic valve replacement: results from a randomized controlled trial. Ann Thorac Surg. 2007;83:2162–8.
Ali A, Halstead JC, Cafferty F, Sharples L, Rose F, Coulden R, et al. Are stentless valves superior to modern stented valves? A prospective randomized trial. Circulation. 2006;114:I535–40.
Cribier A, Eltchaninoff H, Bash A, Borenstein N, Tron C, Bauer F, et al. Percutaneous transcatheter implantation of an aortic valve prosthesis for calcific aortic stenosis: first human case description. Circulation. 2002;106:3006–8.
Vassiliades TA Jr, Block PC, Cohn LH, Adams DH, Borer JS, Feldman T, et al. The clinical development of percutaneous heart valve technology. J Thorac Cardiovasc Surg. 2005;129:970–6.
Vassiliades TA Jr, Block PC, Cohn LH, Adams DH, Borer JS, Feldman T, et al. The clinical development of percutaneous heart valve technology: a position statement of the Society of Thoracic Surgeons (STS), the American Association for Thoracic Surgery (AATS), and the Society for Cardiovascular Angiography and Interventions (SCAI). Ann Thorac Surg. 2005;79:1812–8.
Walther T, Kasimir MT, Doss M, Schuler G, Simon P, Schachinger V, et al. One-year interim follow-up results of the TRAVERCE trial: the initial feasibility study for trans-apical aortic-valve implantation. Eur J Cardiothorac Surg. 2011;39:532–7.
Chan KM, Rahman-Haley S, Mittal TK, Gavino JA, Dreyfus GD. Truly stentless autologous pericardial aortic valve replacement: an alternative to standard aortic valve replacement. J Thorac Cardiovasc Surg. 2011;141:276–83.
Ozaki S, Kawase I, Yamashita H, Uchida S, Nozawa Y, Matsuyama T, et al. Aortic valve reconstruction using self-developed aortic valve plasty system in aortic valve disease. Interact Cardiovasc Thorac Surg. 2011;12:550–3.
Duran CM, Gometza B, Kumar N, Gallo R, Martin-Duran R. Aortic valve replacement with freehand autologous pericardium. J Thorac Cardiovasc Surg. 1995;110:511–6.
Alsoufi B, Al-Shahid M, Manlhiot C, Al-Amri M, McCrindle BW, Fadel B, et al. Mitral valve replacement with the Quattro stentless pericardial bioprosthesis: mid-term clinical and echocardiographic follow up. J Heart Valve Dis. 2010;19:304–11.
Mohr FW, Lehmann S, Falk V, Metz S, Walther C, Doll N, et al. Clinical experience with stentless mitral valve replacement. Ann Thorac Surg. 2005;79:772–5.
Kawachi Y, Masuda M, Tominaga R, Tokunaga K. Comparative study between St. Jude Medical and bioprosthetic valves in the right side of the heart. Jpn Circ J. 1991;55:553–62.
Van Nooten GJ, Caes FL, Francois KJ, Taeymans Y, Primo G, Wellens F, et al. The valve choice in tricuspid valve replacement: 25 years of experience. Eur J Cardiothorac Surg. 1995;9:441–6. (discussion 6–7).
Dalrymple-Hay MJ, Leung Y, Ohri SK, Haw MP, Ross JK, Livesey SA, et al. Tricuspid valve replacement: bioprostheses are preferable. J Heart Valve Dis. 1999;8:644–8.
Hwang HY, Kim KH, Kim KB, Ahn H. Mechanical tricuspid valve replacement is not superior in patients younger than 65 years who need long-term anticoagulation. Ann Thorac Surg. 2012;93:1154–60.
Ratnatunga CP, Edwards MB, Dore CJ, Taylor KM. Tricuspid valve replacement: UK Heart Valve Registry mid-term results comparing mechanical and biological prostheses. Ann Thorac Surg. 1998;66:1940–7.
Chang BC, Lim SH, Yi G, Hong YS, Lee S, Yoo KJ, et al. Long-term clinical results of tricuspid valve replacement. Ann Thorac Surg. 2006;81:1317–23. (discussion 23–4).
Garatti A, Nano G, Bruschi G, Canziani A, Colombo T, Frigiola A, et al. Twenty-five year outcomes of tricuspid valve replacement comparing mechanical and biologic prostheses. Ann Thorac Surg. 2012;93:1146–53.
Kawachi Y, Tominaga R, Hisahara M, Nakashima A, Yasui H, Tokunaga K. Excellent durability of the Hancock porcine bioprosthesis in the tricuspid position. A sixteen-year follow-up study. J Thorac Cardiovasc Surg. 1992;104:1561–6.
Kuwaki K, Komatsu K, Morishita K, Tsukamoto M, Abe T. Long-term results of porcine bioprostheses in the tricuspid position. Surg Today. 1998;28:599–603.
Nakano K, Ishibashi-Ueda H, Kobayashi J, Sasako Y, Yagihara T. Tricuspid valve replacement with bioprostheses: long-term results and causes of valve dysfunction. Ann Thorac Surg. 2001;71:105–9.
Stulak JM, Dearani JA, Burkhart HM, Connolly HM, Warnes CA, Suri RM, et al. The increasing use of mechanical pulmonary valve replacement over a 40-year period. Ann Thorac Surg. 2010;90:2009–14. (discussion 14–5).
Balaguer JM, Byrne JG, Cohn LH. Orthotopic pulmonic valve replacement with a pulmonary homograft as an interposition graft. J Card Surg. 1996;11:417–20.
Eyskens B, Reybrouck T, Bogaert J, Dymarkowsky S, Daenen W, Dumoulin M, et al. Homograft insertion for pulmonary regurgitation after repair of tetralogy of fallot improves cardiorespiratory exercise performance. Am J Cardiol. 2000;85:221–5.
Oosterhof T, Meijboom FJ, Vliegen HW, Hazekamp MG, Zwinderman AH, Bouma BJ, et al. Long-term follow-up of homograft function after pulmonary valve replacement in patients with tetralogy of Fallot. Eur Heart J. 2006;27:1478–84.
Vohra HA, Whistance RN, Baliulis G, Janusauskas V, Kaarne M, Veldtman GR, et al. Midterm evaluation of biological prosthetic valves in the pulmonary position of grown-up patients. Thorac Cardiovasc Surg. 2012;60:205–9.
Shiokawa Y, Sonoda H, Tanoue Y, Nishida T, Nakashima A, Tominaga R. Pulmonary valve replacement long after repair of tetralogy of Fallot. Gen Thorac Cardiovasc Surg. 2012;60:341–4.
Lee C, Park CS, Lee CH, Kwak JG, Kim SJ, Shim WS, et al. Durability of bioprosthetic valves in the pulmonary position: long-term follow-up of 181 implants in patients with congenital heart disease. J Thorac Cardiovasc Surg. 2011;142:351–8.
Miyazaki A, Yamamoto M, Sakaguchi H, Tsukano S, Kagisaki K, Suyama K, et al. Pulmonary valve replacement in adult patients with a severely dilated right ventricle and refractory arrhythmias after repair of tetralogy of fallot. Circ J. 2009;73:2135–42.
George I, Shah JN, Bacchetta M, Stewart A. Stentless bioprosthesis in a valved conduit: implications for pulmonary reconstruction. Ann Thorac Surg. 2009;88:2022–4.
Hawkins JA, Sower CT, Lambert LM, Kouretas PC, Burch PT, Kaza AK, et al. Stentless porcine valves in the right ventricular outflow tract: improved durability? Eur J Cardiothorac Surg. 2009;35:600–4. (discussion 4–5).
Guccione P, Milanesi O, Hijazi ZM, Pongiglione G. Transcatheter pulmonary valve implantation in native pulmonary outflow tract using the Edwards SAPIEN transcatheter heart valve. Eur J Cardiothorac Surg. 2012;41:1192–4.
Eicken A, Ewert P, Hager A, Peters B, Fratz S, Kuehne T, et al. Percutaneous pulmonary valve implantation: two-centre experience with more than 100 patients. Eur Heart J. 2011;32:1260–5.
Khambadkone S, Coats L, Taylor A, Boudjemline Y, Derrick G, Tsang V, et al. Percutaneous pulmonary valve implantation in humans: results in 59 consecutive patients. Circulation 2005;112:1189–97.
Chen PC, Sager MS, Zurakowski D, Pigula FA, Baird CW, Mayer JE Jr, et al. Younger age and valve oversizing are predictors of structural valve deterioration after pulmonary valve replacement in patients with tetralogy of Fallot. J Thorac Cardiovasc Surg. 2012;143:352–60.
Batlivala SP, Emani S, Mayer JE, McElhinney DB. Pulmonary valve replacement function in adolescents: a comparison of bioprosthetic valves and homograft conduits. Ann Thorac Surg. 2012;93:2007–16.
Zubairi R, Malik S, Jaquiss RD, Imamura M, Gossett J, Morrow WR. Risk factors for prosthesis failure in pulmonary valve replacement. Ann Thorac Surg. 2011;91:561–5.
Acknowledgments
We would like to thank Mr. Brian Quinn for reviewing this manuscript.
Author information
Authors and Affiliations
Corresponding author
Additional information
The review was submitted at the invitation of the editorial committee.
Rights and permissions
About this article
Cite this article
Nishida, T., Tominaga, R. A look at recent improvements in the durability of tissue valves. Gen Thorac Cardiovasc Surg 61, 182–190 (2013). https://doi.org/10.1007/s11748-013-0202-z
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11748-013-0202-z