Abstract
Background
Reduced-port laparoscopic surgery remains controversial due to technical challenges that can lead to suboptimal outcomes, and data pertaining to operative and clinical outcomes of reduced-port sleeve gastrectomy (RPSG) vs. conventional laparoscopic sleeve gastrectomy (CLSG) are lacking.
Aims
This retrospective case-matched study aimed to compare midterm (2-year) outcomes of RPSG and of CLSG.
Methods
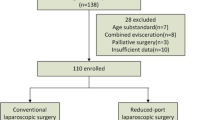
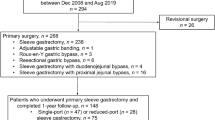
Patients included in the study had undergone laparoscopic bariatric surgery at our center between 2010 and 2017. Thirty-one consecutive female patients who underwent RPSG were compared to a sex-, age-, body mass index–matched group of 31 patients who underwent CLSG. Outcomes were evaluated and compared between groups.
Results
Estimated blood loss volume, incidences of intraoperative and postoperative complications, and length of postoperative hospital stay did not differ significantly between the 2 groups. Operation time was significantly greater in the RPSG group than in the CLSG group (148.7 ± 22.6 vs. 120.2 ± 25.9 min, respectively; p < 0.001). Excess weight loss at 1 year was 105.9% and 109.7%, respectively (p = 0.94) and at 2 years was 101.1% and 105.3%, respectively (p = 0.64). One RPSG patient required placement of additional trocars because of bleeding from short gastric vessels, but conversion to open surgery was not required.
Conclusions
RPSG is feasible in carefully selected bariatric patients and results in midterm outcomes comparable to those observed after CLSG. Good cosmesis is a potential benefit of RPSG.




Similar content being viewed by others
References
Sjöström L, Narbro K, Sjöström CD, et al. Effects of bariatric surgery on mortality in Swedish obese subjects. N Engl J Med. 2007;357:741–52.
Angrisani L, Santonicola A, Iovino P, et al. Bariatric surgery and endoluminal procedures: IFSO worldwide survey 2014. Obes Surg. 2017;27:2279–89.
Ohta M, Seki Y, Wong SK, Wang C, Huang CK, Aly A, et al. Bariatric/metabolic surgery in the Asia-Pacific region: APMBSS 2018 survey. Obes Surg. Springer; 2018;1–8.
Lee WS, Choi ST, Lee JN, et al. Single-port laparoscopic appendectomy versus conventional laparoscopic appendectomy: a prospective randomized controlled study. Ann Surg. 2013;257:214–8.
Curcillo PG, Wu AS, Podolsky ER, et al. Single-port-access (SPA TM) cholecystectomy: a multi-institutional report of the first 297 cases. Surg Endosc. 2010;24:1854–60.
Champagne BJ, Papaconstantinou HT, Parmar SS, et al. Single-incision versus standard multiport laparoscopic colectomy: a multicenter, case-controlled comparison. Ann Surg LWW. 2012;255:66–9.
Raman JD, Bagrodia A, Cadeddu JA. Single-incision, umbilical laparoscopic versus conventional laparoscopic nephrectomy: a comparison of perioperative outcomes and short-term measures of convalescence. Eur Urol. 2009;55:1198–206.
Targarona EM, Balague C, Martinez C, et al. Single-port access: a feasible alternative to conventional laparoscopic splenectomy. Surg Innov. 2009;16:348–52.
Hamzaoglu I, Karahasanoglu T, Aytac E, et al. Transumbilical totally laparoscopic single-port Nissen fundoplication: a new method of liver retraction: the Istanbul technique. J Gastrointest Surg. 2010;14:1035–9.
Saber AA, El-Ghazaly TH, Dewoolkar AV, et al. Single-incision laparoscopic sleeve gastrectomy versus conventional multiport laparoscopic sleeve gastrectomy: technical considerations and strategic modifications. Surg Obes Relat Dis. 2010;6:658–64.
Lakdawala M, Agarwal A, Dhar S, et al. Single-incision sleeve gastrectomy versus laparoscopic sleeve gastrectomy. A 2-year comparative analysis of 600 patients. Obes Surg. 2015;25:607–14.
Delgado S, Ibarzabal A, Adelsdorfer C, et al. Transumbilical single-port sleeve gastrectomy: initial experience and comparative study. Surg Endosc. 2012;26:1247–53.
Sucher R, Resch T, Mohr E, et al. Single-incision laparoscopic sleeve gastrectomy versus multiport laparoscopic sleeve gastrectomy: analysis of 80 cases in a single center. J Laparoendosc Adv Surg Tech. 2014;24:83–8.
Gomberawalla A, Salamat A, Lutfi R. Outcome analysis of single incision vs traditional multiport sleeve gastrectomy: a matched cohort study. Obes Surg Springer;. 2014;24:1870–4.
Porta A, Aiolfi A, Musolino C, et al. Prospective comparison and quality of life for single-incision and conventional laparoscopic sleeve gastrectomy in a series of morbidly obese patients. Obes Surg. Springer;. 2017;27:681–7.
Hosseini SV, Hosseini SA, Al-Hurry AMAH, et al. Comparison of early results and complications between multi-and single-port sleeve gastrectomy: a randomized clinical study. Iran J Med Sci. 2017;42:251.
Himpens J, Dobbeleir J, Peeters G. Long-term results of laparoscopic sleeve gastrectomy for obesity. Ann Surg. 2010;252:319–24.
Guidelines for Clinical Application of Laparoscopic Bariatric Surgery. Society of American Gastrointestinal and Endoscopic Surgeons (SAGES). http://www.sages.org/publications/guidelines/guidelines-for-clinical-application-of-laparoscopic-bariatric-surgery/. Accessed 26 Jan 2019.
Zachariah SK, Tai CM, Chang PC, et al. The “T-suspension tape” for liver and gallbladder retraction in bariatric surgery: feasibility, technique, and initial experience. J Laparoendosc Adv Surg Tech A. 2013;23:311–5.
Mittermair R, Pratschke J, Sucher R. Single-incision laparoscopic sleeve gastrectomy. Am Surg. 2013;79:393–7.
Fernández JI, Ovalle C, Farias C, et al. Transumbilical laparoscopic Roux-en-Y gastric bypass with hand-sewn gastrojejunal anastomosis. Obes Surg. 2013;23:140–4.
Palanivelu P, Patil KP, Parthasarathi R, et al. Review of various liver retraction techniques in single incision laparoscopic surgery for the exposure of hiatus. J Minim Access Surg. 2015;11:198–202.
Shi X, Karmali S, Sharma AM, et al. A review of laparoscopic sleeve gastrectomy for morbid obesity. Obes Surg. 2010;20:1171–7.
Gentileschi P, Camperchioli I, Benavoli D, et al. Laparoscopic single-port sleeve gastrectomy for morbid obesity: preliminary series. Surg Obes Relat Dis. 2010;6:665–9.
Uslu HY, Erkek AB, Cakmak A, et al. Trocar site hernia after laparoscopic cholecystectomy. J Laparoendosc Adv Surg Tech. 2007;17:600–3.
Marks JM, Phillips MS, Tacchino R, et al. Single-incision laparoscopic cholecystectomy is associated with improved cosmesis scoring at the cost of significantly higher hernia rates: 1-year results of a prospective randomized, multicenter, single-blinded trial of traditional multiport laparoscopic. J Am Coll Surg. 2013;216:1037–47.
Julliard O, Hauters P, Possoz J, et al. Incisional hernia after single-incision laparoscopic cholecystectomy: incidence and predictive factors. Surg Endosc. 2016;30:4539–43.
Buckley 3rd FP, Vassaur HE, Jupiter DC, et al. Influencing factors for port-site hernias after single-incision laparoscopy. Hernia. 2016;20:729–33.
Soricelli E, Iossa A, Casella G, et al. Sleeve gastrectomy and crural repair in obese patients with gastroesophageal reflux disease and/or hiatal hernia. Surg Obes Relat Dis. 2013;9:356–61.
Acknowledgments
The authors thank Prof. Tina Tajima for her assistance in presenting our findings in English.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
All procedures performed in our study involving human participants were in accordance with the ethical standards of the institutional and/or Japanese national research committees and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed Consent
Consent to use their anonymized data for research purposes has been obtained from all included in the study.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Amiki, M., Seki, Y., Kasama, K. et al. Reduced-Port Sleeve Gastrectomy for Morbidly Obese Japanese Patients: a Retrospective Case-Matched Study. OBES SURG 29, 3291–3298 (2019). https://doi.org/10.1007/s11695-019-03987-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-019-03987-1