Abstract
Purpose
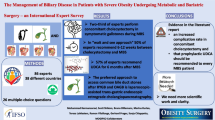
Incidence of non-alcoholic fatty liver disease (NAFLD) is on the rise and is one of the most common causes of chronic liver disease worldwide. Obesity and metabolic syndrome are considered the most significant risk factors. Bariatric surgery is the only treatment modality in morbid obesity which allows long-term weight loss with improvement in associated co-morbid conditions. However, the effects of bariatric surgery on NAFLD are not well established. NAFLD fibrosis score (NFS) is a validated non-invasive scoring system used to assess advanced fibrosis. We used the NFS to analyse the impact of weight loss on NAFLD following sleeve gastrectomy.
Materials and Methods
174 patients who underwent bariatric surgery between 2010 and 2016 were retrospectively reviewed. Multivariate analysis was performed using pre-operative patient characteristics, biochemical markers and TANITA body analysis measurements to determine significant risk factors for NFS > 0.675. Additionally, the NFS was calculated at 6 months, 1 year and 2 years post-operatively to determine correlation with weight loss.
Results
Pre-operatively, 13.8% of our patients had significant fibrosis by NFS. Mean change in NFS was − 0.46 ± 1.02, − 0.55 ± 0.98 and − 0.55 ± 1.12 at 6 months, 1 year and 2 years respectively. This was significantly correlated with percent of total weight loss with R coefficients of 0.253, 0.292 and 0.274 respectively (P < 0.05). 79.2% of patients with NFS > 0.675 achieved resolution by 2 years post-operatively.
Conclusion
Based on our study, we conclude that sleeve gastrectomy may be a viable treatment option for management of NAFLD in the obese.

Similar content being viewed by others
References
Browning JD, Szczepaniak LS, Dobbins R, et al. Prevalence of hepatic steatosis in an urban population in the United States: impact of ethnicity. Hepatology. 2004;40:1387–95.
Bedogni G, Miglioli L, Masutti F, et al. Prevalence of and risk factors for nonalcoholic fatty liver disease: the Dionysos nutrition and liver study. Hepatology. 2005;42:44–52.
Fan JG, Zhu J, Li XJ, et al. Prevalence of and risk factors for fatty liver in a general population of Shanghai, China. J Hepatol. 2005;43:508–14.
Nomura H, Kashiwagi S, Hayashi J, et al. Prevalence of fatty liver in a general population of Okinawa, Japan. Jpn J Med. 1988;27:142–9.
The World at Six Billion. UN Population Division.
Chitturi S, Farrell GC, Hashimoto E, et al. Nonalcoholic fatty liver disease in the Asia-Pacific region: definitions and overview of proposed guidelines. J Gastroenterol Hepatol. 2007;22(6):778–87.
Jafar TH, Hatcher J, Poulter N, et al. Community-based interventions to promote blood pressure control in a developing country: a cluster randomized trial. Ann Intern Med. 2009;151(9):593–601.
Lear SA, Toma M, Birmingham CL, et al. Modification of the relationship between simple anthropometric indices and risk factors by ethnic background. Metabolism. 2003;52(10):1295–301.
Hamaguchi M, Kojima T, Takeda N, et al. The metabolic syndrome as a predictor of nonalcoholic fatty liver disease. Ann Intern Med. 2005;143(10):722–8.
Brunt EM. Nonalcoholic steatohepatitis. Semin Liver Dis. 2004;24(1):3–20.
Cusi K. Role of obesity and lipotoxicity in the development of non-alcoholic steatohepatitis: pathophysiology and clinical implications. Gastroenterology. 2012;142(4):711–25.
Fabbrini E, Sullivan S, Klein S. Obesity and nonalcoholic fatty liver disease: biochemical, metabolic and clinical implications. Hepatology. 2010;51(2):679–89.
McCullough AJ. Pathophysiology of nonalcoholic steatohepatitis. J Clin Gastroenterol. 2006;40(suppl 1):S17–29.
Duvnjak M, Lerotić I, Barsić N, et al. Pathogenesis and management issues for non-alcoholic fatty liver disease. World J Gastroenterol. 2007;13(34):4539–50.
Siebler J, Galle PR, Weber MM. The gut-liver-axis: endotoxemia, inflammation, insulin resistance and NASH. J Hepatol. 2008;48(6):1032–4.
Wong VW, Wong GL, Choi PC, et al. Disease progression of non-alcoholic fatty liver disease: a prospective study with paired liver biopsies at 3 years. Gut. 2010;59(7):969–74.
Pais R, Pascale A, Fedchuck L, et al. Progression from isolated steatosis to steatohepatitis and fibrosis in nonalcoholic fatty liver disease. Clin Res Hepatol Gastroenterol. 2011;35(1):23–8.
Pais R, Charlotte F, Fedchuk L, et al. A systematic review of followup biopsies reveals disease progression in patients with non-alcoholic fatty liver. J Hepatol. 2013;59(3):550–6.
Angulo P, Hui JM, Marchesini G, et al. The NAFLD fibrosis score: a noninvasive system that identifies liver fibrosis in patients with NAFLD. Hepatology. 2007;45(4):846–54.
McPherson S, Stewart SF, Henderson E, et al. Simple non-invasive fibrosis scoring systems can reliably exclude advanced fibrosis in patients with non-alcoholic fatty liver disease. Gut. 2010;59(9):1265–9.
Angulo P. Nonalcoholic fatty liver disease. N Engl J Med. 2002;346(16):1221–31.
Qureshi K, Clements RH, Abrams GA. The utility of the “NAFLD fibrosis score” in morbidly obese subjects with NAFLD. Obes Surg. 2008;18(3):264–70.
Pimentel SK, Strobel R, Gonçalves CG, et al. Evaluation of the nonalcoholic fat liver disease fibrosis score for patients undergoing bariatric surgery. Arq Gastroenterol. 2010;47(2):170–3.
Attar BM, Van Thiel DH. Current concepts and management approaches in nonalcoholic fatty liver disease. ScientificWorldJournal. 2013;2013:481893.
Marra F, Lotersztajin S. Pathophysiology of NASH: perspectives for a targeted treatment. Curr Pharm Des. 2013;19(29):5250–69.
Mi X-X, Wang L, Xun Y-H, et al. Assessment nonalcoholic fatty liver disease fibrosis score for staging and predicting outcome. Int J Clin Exp Med. 2016;9(8):16146–56.
Chalasani N, Younossi Z, Lavine JE, et al. The diagnosis and managements of non-alcoholic fatty liver disease: practice guideline by the American Association for the Study of Liver Diseases, American College of Gastroenterology, and the American Gastroenterological Association. Hepatology. 2012;55(6):2005–23. https://doi.org/10.1002/hep.25762.
Tai CM, Huang CK, Hwang JC, et al. Improvement of nonalcoholic fatty liver disease after bariatric surgery in morbidly obese Chinese patients. Obes Surg. 2012;22:1016–21.
Kakizaki S, Takizawa D, Yamazaki Y, et al. Nonalcoholic fatty liver disease in Japanese patients with severe obesity who received laparoscopic Roux-en-Y gastric bypass surgery (LRYGB) in comparison to non-Japanese patients. J Gastroenterol. 2008;43(1):86–92.
Praveen RP, Gomes RM, Kumar S, et al. The effect of surgically induced weight loss on nonalcoholic fatty liver disease in morbidly obese Indians: NASHOST prospective observational trial. Surg Obes Relat Dis. 2015;11(6):1315–22.
Froylich D, Corcelles R, Daigle C, et al. Effect of Roux-en-Y gastric bypass and sleeve gastrectomy on nonalcoholic fatty liver disease: a comparative study. Surg Obes Relat Dis. 2016;12(1):127–31.
Vargas V, Allende H, Lecube A, et al. Surgically induced weight loss by gastric bypass improves non alcoholic fatty liver disease in morbid obese patients. World J Hepatol. 2012;4(12):382–8.
Cazzo E, Jimenez LS, Pareja JC, et al. Effect of roux-en-y gastric bypass on Nonalcoholic Fatty Liver Disease evaluated through NAFLD fibrosis score: a prospective study. Obes Surg. 2015;25:982–5.
Karcz WK, Krawczykowski D, Kuesters S, et al. Influence of sleeve gastrectomy on NASH and type 2 diabetes mellitus. J Obes. 2011;2011:765473.
Myronovych A et al. Vertical sleeve gastrectomy reduces hepatic steatosis while increasing serum bile acids in a weight-loss-independent manner. Obesity. 2014;22:390–400.
Myronovych A, Salazar-Gonzalez R-M, Ryan KK, et al. The role of small heterodimer partner in nonalcoholic fatty liver disease improvement after sleeve gastrectomy in mice. Obesity. 2014;22:2301–11.
Du J, Tian J, Ding L, et al. Vertical sleeve gastrectomy reverses diet-induced gene-regulatory changes impacting lipid metabolism. Sci Rep. 2017;7:5274.
European Association for Study of Liver. Asociacion Latinoamericana para el Estudio del Higado EASL-ALEH Clinical Practice Guidelines: non-invasive tests for evaluation of liver disease severity and prognosis. J Hepatol. 2015;63:237–64. https://doi.org/10.1016/j.jhep.2015.04.006.
McPherson S, Stewart SF, Henderson E, et al. Simple non-invasive fibrosis scoring systems can reliably exclude advanced fibrosis in patients with non-alcoholic fatty liver disease. Gut. 2010;59:1265–9. https://doi.org/10.1136/gut.2010.216077.
Kim D, Kim WR, Kim HJ, et al. Association between noninvasive fibrosis markers and mortality among adults with nonalcoholic fatty liver disease in the United States. Hepatology. 2013;57:1357–65. https://doi.org/10.1002/hep.26156.
Treeprasertsuk S, Björnsson E, Enders F, et al. NAFLD fibrosis score: a prognostic predictor for mortality and liver complications among NAFLD patients. World J Gastroenterol. 2013;19:1219–29. https://doi.org/10.3748/wjg.v19.i8.1219.
Wong VW, Wong GL, Chim AM, et al. Validation of the NAFLD fibrosis score in a Chinese population with low prevalence of advanced fibrosis. Am J Gastroenterol. 2008;103:1682–8. https://doi.org/10.1111/j.1572-0241.2008.01933.x.
Mummadi RR, Kasturi KS, Chennareddygari S, et al. Effects of bariatric surgery on nonalcoholic fatty liver disease: systematic review and meta- analysis. Clin Gastroenterol Hepatol. 2008;6(12):1396–402.
Chavez-Tapia NC, Tellez-Avila FI, Barrientos-Gutierrez T, et al. Bariatric surgery for non-alcoholic steatohepatitis in obese patients. Cochrane Database Syst Rev. 2010;20(1):CD007340.
Ministry of Health. National health survey 2010. Singapore: Epidemiology and Disease Control Division, Ministry of Health; 2011.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethics Statements
This study has been approved by the institutional research ethics committee. No formal consent was required as this was a retrospective study.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Koh, Z.J., Salgaonkar, H.P., Lee, W.J.J. et al. Improvement in Non-alcoholic Fatty Liver Disease Score Correlates with Weight Loss in Obese Patients Undergoing Laparoscopic Sleeve Gastrectomy: a Two-Centre Study from an Asian Cohort. OBES SURG 29, 862–868 (2019). https://doi.org/10.1007/s11695-018-3581-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-018-3581-5