Abstract
Purpose
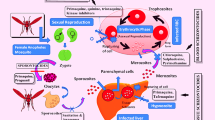
The resistance of parasite to readily affordable antimalarial drugs, the high cost of currently potent drugs, and the resistance of vector mosquitoes to insecticides threaten the possibility of malaria eradication in malaria endemic areas. Due to the fact that quinine and artemisinin were isolated from plants sources, researchers have been encouraged to search for new antimalarials from medicinal plants. This is especially the case in Africa where a large percentage of the population depends on medicinal plant to treat malaria and other ailments.
Method
In this study, we evaluated previously characterized Plasmodium-cidal compounds obtained from the African flora to identify their likely biochemical targets, for an insight into their possible antimalarial chemotherapy. Molecular docking study was first conducted, after which remarkable compounds were submitted for molecular dynamic (MD) simulations studies.
Results
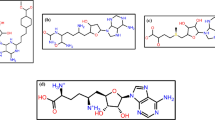
From a total of 38 Plasmodium-cidal compounds docked with confirmed Plasmodium falciparum protein drug targets [plasmepsin II (PMII), histo-aspartic protein (HAP) and falcipain-2 (FP)], two pentacyclic triterpene, cucurbitacin B and 3 beta-O-acetyl oleanolic acid showed high binding affinity relative to artesunate. This implies their capacity to inhibit the three selected P. falciparum target proteins, and consequently, antimalarial potential. From the MD simulations studies and binding free energy outcomes, results confirmed that the two compounds are stable in complex with the selected antimalarial targets; they also showed excellent binding affinities during the 100 ns simulation.
Conclusion
These results showed that cucurbitacin B and 3 beta-O-acetyl oleanolic acid are potent antimalarials and should be considered for further studies.








Similar content being viewed by others
Data availability
The authors confirm that the data supporting the findings of this study are available within the article.
References
Wilairatana P, Chanmol W, Rattaprasert P et al (2021) Prevalence and characteristics of malaria co-infection among individuals with visceral leishmaniasis in Africa and Asia: a systematic review and meta-analysis. Parasit Vectors 14:1–18. https://doi.org/10.1186/s13071-021-05045-1
World Health Organization (2022) World malaria report 2022. World Health Organization. https://www.who.int/teams/global-malaria-programme/reports/world-malaria-report-2022. (ISBN 978-92-4-006489-8). Accessed 20 July 2023
Greenwood D (1995) Conflicts of interest: the genesis of synthetic antimalarial agents in peace and war. J Antimicrob Chemother 36:857–872. https://doi.org/10.1093/jac/36.5.857
Wiesner J, Ortmann R, Jomaa H, Schlitzer M (2003) New antimalarial drugs. Angew Chemie Int Ed 42:5274–5293. https://doi.org/10.1002/anie.200200569
Saxena S, Pant N, Jain DC, Bhakuni RS (2003) Antimalarial agents from plant sources. Curr Sci 85:1314–1329. https://www.jstor.org/stable/24108135
Kaur K, Jain M, Kaur T, Jain R (2009) Antimalarials from nature. Bioorganic Med Chem 17:3229–3256. https://doi.org/10.1016/j.bmc.2009.02.050
Klayman DL (1985) Qinghaosu (artemisinin): an antimalarial drug from China. Science 228:1049–1055. https://doi.org/10.1126/science.3887571
Adebayo JO, Krettli AU (2011) Potential antimalarials from Nigerian plants: a review. J Ethnopharmacol 133:289–302. https://doi.org/10.1016/j.jep.2010.11.024
Hostettmann K, Marston A, Ndjoko K, Wolfender J-L (2000) The potential of African plants as a source of drugs. Curr Org Chem 4:973–1010. https://doi.org/10.2174/1385272003375923
Ersmark K, Samuelsson B, Hallberg A (2006) Plasmepsins as potential targets for new antimalarial therapy. Med Res Rev 26:626–666. https://doi.org/10.1002/med.20082
Werbovetz KA (2000) Target-based drug discovery for malaria, leishmaniasis, and trypanosomiasis. Curr Med Chem 7:835–860. https://doi.org/10.2174/0929867003374615
Woster PM (2003) New therapies for malaria. Annu Rep Med Chem 38:203–211. https://doi.org/10.1016/S0065-7743(03)38022-4
Olliaro PL, Yuthavong Y (1999) An overview of chemotherapeutic targets for antimalarial drug discovery. Pharmacol Ther 81:91–110. https://doi.org/10.1016/s0163-7258(98)00036-9
Doerig C (2004) Protein kinases as targets for anti-parasitic chemotherapy. Biochim Biophys Acta (BBA) Proteins Proteom 1697:155–168. https://doi.org/10.1016/j.bbapap.2003.11.021
Onguéné AP, Ntie-Kang F, Lifongo LL et al (2013) The potential of anti-malarial compounds derived from African medicinal plants, part I: a pharmacological evaluation of alkaloids and terpenoids. Malar J 12:4–25. https://doi.org/10.1186/1475-2875-12-449
Zofou D, Kuete V, Titanji VPK (2013) Antimalarial and other antiprotozoal products from African medicinal plants. Elsevier Inc., London. https://doi.org/10.1016/B978-0-12-405927-6.00017-5
Chinsembu KC (2015) Plants as antimalarial agents in Sub-Saharan Africa. Acta Trop 152:32–48. https://doi.org/10.1016/j.actatropica.2015.08.009
O’Boyle NM, Banck M, James CA et al (2011) Open Babel: an open chemical toolbox. J Cheminform 3:33. https://doi.org/10.1186/1758-2946-3-33
Trott O, Olson AJ (2010) AutoDock Vina: improving the speed and accuracy of docking with a new scoring function, efficient optimization, and multithreading. J Comput Chem 31:455–461. https://doi.org/10.1002/jcc.21334
Lindahl, Abraham, Hess, Spoel van der (2021) GROMACS 2020.5 source code. https://doi.org/10.5281/ZENODO.4420785
Hanwell MD, Curtis DE, Lonie DC et al (2012) Avogadro: an advanced semantic chemical editor, visualization, and analysis platform. J Cheminform 4:1–17. https://doi.org/10.1186/1758-2946-4-17
Vanommeslaeghe K, Hatcher E, Acharya C et al (2009) CHARMM general force field: a force field for drug-like molecules compatible with the CHARMM all-atom additive biological force fields. J Comput Chem 31:671–690. https://doi.org/10.1002/jcc.21367
Kumari R, Kumar R, Consortium OSDD, Lynn A (2014) g_mmpbsa—a GROMACS tool for MM-PBSA and its optimization for high-throughput binding energy calculations. J Chem Inf Model 54:1951–1962. https://doi.org/10.1021/ci500020m
Bhaumik P, Xiao H, Parr CL et al (2009) Crystal structures of the histo-aspartic protease (HAP) from Plasmodium falciparum. J Mol Biol 388:520–540. https://doi.org/10.1016/j.jmb.2009.03.011
Liu P (2017) Plasmepsin: function, characterization and targeted antimalarial drug development. Natural remedies in the fight against parasites. Intech Open, London, pp 183–218. https://doi.org/10.5772/66716
Sherman IW (1977) Amino acid metabolism and protein synthesis in malarial parasites. Bull World Health Organ 55:265. (PMID: 338183; PMCID: PMC2366754)
Musyoka TM, Kanzi AM, Lobb KA, Bishop ÖT (2016) Structure based docking and molecular dynamic studies of plasmodial cysteine proteases against a South African natural compound and its analogs. Sci Rep 6:1–12. https://doi.org/10.1038/srep23690
Goldberg DE (1992) Plasmodial hemoglobin degradation: an ordered pathway in a specialized organelle. Infect Agents Dis 1:207–211. (PMID: 1365547)
Qidwai T (2015) Hemoglobin degrading proteases of Plasmodium falciparum as antimalarial drug targets. Curr Drug Targets 16:1133–1141. https://doi.org/10.2174/138945011666615030410412
Wu Y, Wang X, Liu X, Wang Y (2003) Data-mining approaches reveal hidden families of proteases in the genome of malaria parasite. Genome Res 13:601–616. https://doi.org/10.1101/gr.913403
Pandey KC, Dixit R (2012) Structure-function of falcipains: malarial cysteine proteases. J Trop Med. https://doi.org/10.1155/2012/345195
Abdulai SI, Ishola AA, Bewaji CO (2023) Antimalarial activities of a therapeutic combination of Azadirachta indica, Mangifera indica and Morinda lucida leaves: a molecular view of its activity on Plasmodium falciparum proteins. Acta Parasitol. https://doi.org/10.1007/s11686-023-00698-7
Nwonuma CO, Balogun EA, Gyebi GA (2023) Evaluation of antimalarial activity of ethanolic extract of Annona muricata L.: an in vivo and an in silico approach. J Evid Based Integr Med. https://doi.org/10.1177/2515690X231165104
Gabriel HB, Sussmann RAC, Kimura EA et al (2018) Terpenes as potential antimalarial drugs. Terpenes Terpenoids 1:39–57. https://doi.org/10.5772/intechopen.75108
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors report that there is no conflict of interest.
Ethical approval
Not applicable—the article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ishola, A.A., Adewole, K.E., Adebayo, J.O. et al. Potentials of Terpenoids as Inhibitors of Multiple Plasmodium falciparum Protein Drug Targets. Acta Parasit. 68, 793–806 (2023). https://doi.org/10.1007/s11686-023-00711-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11686-023-00711-z