Abstract
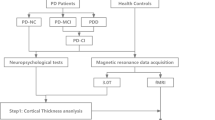
Mild cognitive impairment in Parkinson’s disease (PD-MCI) is associated with consistent structural and functional brain changes. Whether different approaches for diagnosing PD-MCI are equivalent in their neural correlates is presently unknown. We aimed to profile the neuroimaging changes associated with the two endorsed methods of diagnosing PD-MCI. We recruited 53 consecutive non-demented PD patients and classified them as PD-MCI according to comprehensive neuropsychological examination as operationalized by the Movement Disorders Task Force. Voxel-based morphometry, cortical thickness, functional connectivity and graph theoretical measures were obtained on a 3-Tesla MRI scanner. 18 patients (32%) were classified as PD-MCI with Level-II criteria, 19 (33%) with the Parkinson’s disease Cognitive Rating Scale (PD-CRS) and 32 (60%) with the Montreal Cognitive Assessment (MoCA) scale. Though regions of atrophy differed across classifications, reduced gray matter in the precuneus was found using both Level-II and PD-CRS classifications in PD-MCI patients. Patients diagnosed with the PD-CRS also showed extensive changes in cortical thickness, concurring with the MoCA in regions of the cingulate cortex, and again with Level-II regarding cortical thinning in the precuneus. Functional connectivity analysis found higher coherence within salience network regions of interest, and decreased anticorrelations between salience/central executive and default-mode networks in the PD-CRS classification for PD-MCI patients. Graph theoretical metrics showed a widespread decrease in node degree for the three classifications in PD-MCI, whereas betweenness centrality was increased in select nodes of the default mode network (DMN). Clinical and neuroimaging commonalities between the endorsed methods of cognitive assessment suggest a corresponding set of neural correlates in PD-MCI: loss of structural integrity in DMN structures, mainly the precuneus, and a loss of weighted connections in the salience network that might be counterbalanced by increased centrality in the DMN. Furthermore, the similarity of the results between exhaustive Level-II and screening Level-I tools might have practical implications in the search for neuroimaging biomarkers of cognitive impairment in Parkinson’s disease.




Similar content being viewed by others
References
Aarsland, D., & Kurz, M. W. (2010). The epidemiology of dementia associated with Parkinson disease. Journal of the Neurological Sciences, 289(1–2), 18–22
Aracil-Bolaños, I., Sampedro, F., Marín-Lahoz, J., Horta-Barba, A., Martínez-Horta, S., Botí, M., et al. (2019). 40(11), 3233–3242
Ashburner, J. (2007). A fast diffeomorphic image registration algorithm. Neuroimage, 38(1), 95–113
Baggio, H., Sala-llonch, R., Valldeoriola, F., Compta, Y. (2014). Functional brain networks and cognitive deficits in Parkinson’ s disease. Human Brain Mapping, 35(9), 4620–4634
Bastian, M., Heymann, S., Jacomy, M. (2009) Gephi: An Open Source Software for Exploring and Manipulating Networks. In: Proceedings of the Third International ICWSM Conference
Bejr-kasem, H., Pagonabarraga, J., Martínez-Horta, S., Sampedro, F., Marín-Lahoz, J., Horta-Barba, A., et al. (2019). Disruption of the default mode network and its intrinsic functional connectivity underlies minor hallucinations in Parkinson’s disease. Movement Disorders, 34(1), 78–86
Christopher, L., Duff-Canning, S., Koshimori, Y., Segura, B., Boileau, I., Chen, R., et al. (2015). Salience network and parahippocampal dopamine dysfunction in memory-impaired parkinson disease. Annals of Neurology, 77(2), 269–280
Dalrymple-Alford, J. C., MacAskill, M. R., Nakas, C. T., Livingston, L., Graham, C., Crucian, G. P., et al. (2010). The MoCA: Well-suited screen for cognitive impairment in Parkinson disease. Neurology., 75(19), 1717–1725
Darby, R. R., Joutsa, J., & Fox, M. D. (2018). Network localization of heterogeneous neuroimaging findings. Brain, 142(1), 70–79
Emre, M., Aarsland, D., Brown, R., Burn, D.J., Duyckaerts, C., Mizuno, Y., et al. (2007). Clinical diagnostic criteria for dementia associated with Parkinson’s disease. Movement Disorders, 22(12), 1689–1707
Fernández de Bobadilla, R., Pagonabarraga, J., Martínez-Horta, S., Pascual-Sedano, B., Campolongo, A., & Kulisevsky, J. (2013). Parkinson’s disease-cognitive rating scale: Psychometrics for mild cognitive impairment. Movement Disorders, 28(10), 1376–1383
Filippi, M., van den Heuvel, M. P., Fornito, A., He, Y., Hulshoff Pol, H. E., Agosta, F., et al. (2013). Assessment of system dysfunction in the brain through MRI-based connectomics. Lancet Neurology, 12(12), 1189–1199
Fischl, B., &, Dale, A.M. (2000). Measuring the thickness of the human cerebral cortex from magnetic resonance images. Proceedings of the National Academy of Sciences, 97(20), 11050–11055
Garcia-Diaz, A. I., Segura, B., Baggio, H. C., Marti, M. J., Valldeoriola, F., Compta, Y., et al. (2014). Structural MRI correlates of the MMSE and pentagon copying test in Parkinson’s disease. Parkinsonism and Related Disorder., 20(12), 1405–1410
Gasca-Salas, C., Clavero, P., García-García, D., Obeso, J. A., & Rodríguez-Oroz, M. C. (2016). Significance of visual hallucinations and cerebral hypometabolism in the risk of dementia in Parkinson’s disease patients with mild cognitive impairment. Human Brain Mapping, 37(3), 968–977
Gee, M., Dukart, J., Draganski, B., Wayne Martin, W. R., Emery, D., & Camicioli, R. (2017). Regional volumetric change in Parkinson’s disease with cognitive decline. Journal of the Neurological Sciences, 373, 88–94
Goldman, J. G., Stebbins, G. T., Dinh, V., Bernard, B., Merkitch, D., Detoledo-Morrell, L., et al. (2014). Visuoperceptive region atrophy independent of cognitive status in patients with Parkinson’s disease with hallucinations. Brain., 137(3), 849–859
González-Redondo, R., García-García, D., Clavero, P., Gasca-Salas, C., García-Eulate, R., Zubieta, J. L., et al. (2014). Grey matter hypometabolism and atrophy in Parkinson’s disease with cognitive impairment: A two-step process. Brain., 137(8), 2356–2367
Gorges, M., Müller, H., Lulé, D., Consortium, L., Pinkhardt, E. H., Ludolph, A. C., et al. (2015). Neurobiology of aging to rise and to fall : Functional connectivity in cognitively normal and cognitively impaired patients with Parkinson ’ s disease. Neurobiology of Aging, 36(4), 1727–1735
Greicius, M.D., Krasnow, B., Reiss, A.L., Menon, V. (2003). Functional connectivity in the resting brain : A network analysis of the default mode hypothesis. Proceedings of the National Academy of Sciences, 100(1), 253–258
Hoffstaedter, F., Grefkes, C., Caspers, S., Roski, C., Palomero-Gallagher, N., Laird, A. R., et al. (2014). The role of anterior midcingulate cortex in cognitive motor control: Evidence from functional connectivity analyses. Human Brain Mapping, 35(6), 2741–2753
Hoogland, J., Boel, J. A., de Bie, R. M. A., Geskus, R. B., Schmand, B. A., Dalrymple-Alford, J. C., et al. (2017). Mild cognitive impairment as a risk factor for Parkinson’s disease dementia. Movement Disorders, 32(7), 1056–1065
Hoogland, J., van Wanrooij, L. L., Boel, J. A., Goldman, J. G., Stebbins, G. T., Dalrymple-Alford, J. C., et al. (2018). Detecting mild cognitive deficits in Parkinson’s disease: Comparison of neuropsychological tests. Movement Disorders, 33(11), 1750–1759
Hughes, A. J., Daniel, S. E., Kilford, L., & Lees, A. J. (1992). Accuracy of clinical diagnosis of idiopathic Parkinson ’ s disease : A clinico-pathological study of 100 cases. Journal of Neurology, Neurosurgery, and Psychiatry, 55, 181–184
Kehagia, A. A., Barker, R. A., & Robbins, T. W. (2012). Cognitive impairment in Parkinson’s disease: The dual syndrome hypothesis. Neurodegenerative Diseases, 11(2), 79–92
Kruschwitz, J. D., List, D., Waller, L., Rubinov, M., & Walter, H. (2015). GraphVar: A user-friendly toolbox for comprehensive graph analyses of functional brain connectivity. Journal of Neuroscience Methods, 245, 107–115
Litvan, I., Aarsland, D., Adler, C. H., Goldman, J. G., Kulisevsky, J., Mollenhauer, B., et al. (2011). MDS task force on mild cognitive impairment in Parkinson’s disease: Critical review of PD-MCI. Movement Disorders, 26(10), 1814–1824
Litvan, I., Goldman, J. G., Tröster, A. I., Ben, A., Weintraub, D., Petersen, R. C., et al. (2012). Diangostic criteria for mild cognitive impairment in Parkinson’s disease: Movement Disorder Society task force guidelines. Movement Disorders, 27(3), 349–356
Lopes, R., Delmaire, C., Defebvre, L., Moonen, A.J., Duits, A.A., Hofman, P., et al. (2016). Cognitive phenotypes in Parkinson ’ s disease differ in terms of brain-network organization and connectivity. Human Brain Mapping, 38(3), 1604–1621
Lucas-Jiménez, O., Ojeda, N., Peña, J., Díez-Cirarda, M., Cabrera-Zubizarreta, A., Gómez-Esteban, J. C., Gómez-Beldarrain, M. Á., & Ibarretxe-Bilbao, N. (2016). Altered functional connectivity in the default mode network is associated with cognitive impairment and brain anatomical changes in Parkinson ’ s disease. Park Relat Disord, 33, 58–64
Mak, E., Bergsland, N., Dwyer, M. G., Zivadinov, R., & Kandiah, N. (2014). Subcortical atrophy is associated with cognitive impairment in mild Parkinson disease: A combined investigation of volumetric changes, cortical thickness, and vertex-based shape analysis. AJNR. American Journal of Neuroradiology, 35(12), 2257–2264
Mak, E., Su, L., Williams, G. B., Firbank, M. J., Lawson, R. A., Yarnall, A. J., et al. (2015). Baseline and longitudinal grey matter changes in newly diagnosed Parkinson’s disease: ICICLE-PD study. Brain., 138(10), 2974–2986
Martinez-Horta, S., Sampedro, F., Pagonabarraga, J., Fernandez-Bobadilla, R., Marin-Lahoz, J., Riba, J., et al. (2016). Non-demented Parkinson’s disease patients with apathy show decreased grey matter volume in key executive and reward-related nodes. Brain Imaging and Behavior, 11(5), 1334–1342
Pagonabarraga, J., & Kulisevsky, J. (2012). Cognitive impairment and dementia in Parkinson’s disease. Neurobiology of Disease, 46(3), 590–596
Pagonabarraga, J., Pascual-Sedano, B., Campolongo, A., Kulisevsky, J. (2013). Parkinson ’ s disease-cognitive rating scale : Psychometrics for mild cognitive impairment. 28(10), 1376–1383
Pedersen, K. F., Larsen, J. P., Tysnes, O. B., & Alves, G. (2013). Prognosis of mild cognitive impairment in early Parkinson disease: The Norwegian ParkWest study. JAMA Neurology, 70(5), 580–586
Peña-Casanova, J., Blesa, R., Aguilar, M., Gramunt-Fombuena, N., Gómez-Ansón, B., Oliva, R., et al. (2009). Spanish multicenter normative studies (NEURONORMA project): Methods and sample characteristics. Archives of Clinical Neuropsychology, 24(4), 307–319
Pigott, K., Rick, J., Xie, S. X., et al. (2015). Longitudinal study of normal cognition in Parkinson disease. Neurology., 85(15), 1276–1282
Rorden, C., Karnath, H. O., & Bonilha, L. (2007). Improving lesion-symptom mapping. Journal of Cognitive Neuroscience, 19(7), 1081–1088
Seeley, W.W., Menon, V., Schatzberg, A.F., Keller, J., Glover, G.H., Kenna, H., et al. (2007). Dissociable intrinsic connectivity networks for salience processing and executive control. The Journal of Neuroscience, 27(9), 2349–2356
Seeley, W. W., Crawford, R. K., Zhou, J., Miller, B. L., & Greicius, M. D. (2009). Neurodegenerative diseases target large-scale human brain networks. Neuron., 62(1), 42–52
Segura, B., Baggio, H. C., Marti, M. J., Valldeoriola, F., Compta, Y., Garcia-Diaz, A. I., et al. (2014). Cortical thinning associated with mild cognitive impairment in Parkinson’s disease. Movement Disorders, 29(12), 1495–1503
Shirer, W. R., Ryali, S., Rykhlevskaia, E., Menon, V., & Greicius, M. D. (2012). Decoding subject-driven cognitive states with whole-brain connectivity patterns. Cerebral Cortex, 22(1), 158–165
Skorvanek, M., Goldman, J. G., Jahanshahi, M., Marras, C., Rektorova, I., Schmand, B., et al. (2018). Global scales for cognitive screening in Parkinson’s disease: Critique and recommendations. Movement Disorders, 33(2), 208–218
Svenningsson, P., Westman, E., Ballard, C., & Aarsland, D. (2012). Cognitive impairment in patients with Parkinson’s disease: Diagnosis, biomarkers, and treatment. Lancet Neurology, 11(8), 697–707
Tessitore, A., Esposito, F., Vitale, C., Tessitore, A., Santangelo, G., Cirillo, G. (2012). Default-mode network connectivity in cognitively unimpaired patients with Parkinson disease. Neurology, 79(23), 2226–2232
Watanabe, H., Senda, J., Kato, S., Ito, M., Atsuta, N., Hara, K., et al. (2013). Cortical and subcortical brain atrophy in Parkinson’s disease with visual hallucination. Movement Disorders, 28(12), 1732–1736
Whitfield-Gabrieli, S., & Nieto-Castanon, A. (2012). Conn: A functional connectivity toolbox for correlated and Anticorrelated brain networks. Brain Connectivity, 2(3), 125–141
Wood, K.-L., Myall, D. J., Livingston, L., Melzer, T. R., Pitcher, T. L., MacAskill, M. R., et al. (2016). Different PD-MCI criteria and risk of dementia in Parkinson’s disease: 4-year longitudinal study. Parkinsons’s Disease., 2(1), 1–8
Funding
The present work has received funding from
- La Marató de TV3, Expedient number 20142910
- FIS Grant PI14/02058, PI 18/01717.
- CIBERNED (Fundación CIEN, Instituto de Salud Carlos III, Spain)
Author information
Authors and Affiliations
Contributions
Ignacio Aracil-Bolaños contributed to conception, organization and execution of the research project; designed and executed the imaging and statistical analyses and wrote the first draft.
Frederic Sampedro contributed to execution of the research project, assisted in statistical and imaging analyses and provided review and critique of the manuscript.
Juan Marín-Lahoz contributed to execution of the research project, assisted in statistical analysis and provided review and critique of the manuscript.
Andrea Horta-Barba contributed to conception and execution of the research project and provided review and critique of the manuscript.
Saül Martínez-Horta contributed to conception and execution of the research project and provided review and critique of the manuscript.
José María Gónzalez-de-Echávarri contributed to the execution of the research project and assisted in statistical and imaging analyses.
Mariángeles Botí contributed to conception and execution of the research project and provided review and critique of the manuscript.
Jesús Pérez-Pérez contributed to conception and execution of the research project and provided review and critique of the manuscript.
Helena Bejr-Kasem contributed to conception and execution of the research project and provided review and critique of the manuscript.
Berta Pascual-Sedano contributed to conception and execution of the research project and provided review and critique of the manuscript.
Antonia Campolongo contributed to organization and execution of the research project and provided review and critique of the manuscript.
Cristina Izquierdo contributed to organization and execution of the research project and provided review and critique of the manuscript.
Alexandre Gironell contributed to organization and execution of the research project and provided review and critique of the manuscript.
Beatriz Gómez-Ansón contributed to organization and execution of the research project and provided review and critique of the manuscript.
Jaime Kulisevsky contributed to conception, organization and execution of the research project and provided review and critique of the manuscript.
Javier Pagonabarraga contributed to conception, organization and execution of the research project and provided review and critique of the manuscript.
Corresponding authors
Ethics declarations
All patients provided written informed consent according to the Declaration of Helsinki. The study was approved by the Ethics Comitee for Clinical Research at the Hospital de la Santa Creu i Sant Pau, Barcelona.
Conflict of interest
The work of Dr. Aracil is supported by the Spanish Neurological Society via the Movement Disorders Study Group Grant, and is employed by Hospital de la Santa Creu i Sant Pau. The work of Dr. Bejr-Kasem is supported by Instituto de Salud Carlos III, Spain and has served on advisory or speakers’ boards, and received honoraria from Zambon. Dr. Javier Pagonabarraga has served on advisory or speakers’ boards, and received honoraria from UCB, Zambon, AbbVie, Italfarmaco, Allergan, Ipsen and Bial, and received grants from CIBERNED & FIS PI14/02058) (Spanish Government grants) and Fundació La Marató de TV3 20,142,910. Dr. Kulisevsky has received research grants from CIBERNED & FIS PI15/00962 (Spanish Government grants), and Fundació La Marató de TV3 20,142,410, and consulting fees or speaker honoraria from Zambon, Roche, Abbvie, Bial, UCB and Teva. Jesus Perez-Perez is employed as a Joan Rodes researcher (Spanish Government contract) and received grants from FIS (PI17/001885). Saul Martinez-Horta, Mariángeles Boti, Andrea Horta-Barba, Frederic Sampedro, Alexandre Gironell, Antonia Campolongo, Cristina Izquierdo, José María Gónzalez-de-Echávarri and Juan Marín-Lahoz are employed by Hospital de la Santa Creu i Sant Pau and report no other conflict of interest or funding.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOCX 2.27 MB)
Rights and permissions
About this article
Cite this article
Aracil-Bolaños, I., Sampedro, F., Marín-Lahoz, J. et al. Tipping the scales: how clinical assessment shapes the neural correlates of Parkinson’s disease mild cognitive impairment. Brain Imaging and Behavior 16, 761–772 (2022). https://doi.org/10.1007/s11682-021-00543-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11682-021-00543-3