Abstract
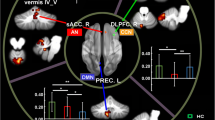
Electroconvulsive therapy (ECT), a rapidly acting and effective treatment for major depressive disorder (MDD), is frequently accompanied by cognitive impairment. Recent studies have documented that ECT reorganizes dysregulated inter/intra- connected cerebral networks, including the affective network, the cognitive control network(CCN) and default mode network (DMN).Moreover, cerebellum is thought to play an important role in emotion regulation and cognitive processing. However, little is known about the relationship between cerebro-cerebellar connectivity alterations following ECT and antidepressant effects or cognitive impairment. We performed seed-based resting-state functional connectivity (RSFC) analyses in 28 MDD patients receiving ECT and 20 healthy controls to identify cerebro-cerebellar connectivity differences related to MDD and changes induced by ECT. Six seed regions (three per hemisphere) in the cerebrum were selected for RSFC, corresponding to the affective network, CCN and DMN, to establish cerebro-cerebellar functional connectivity with cerebellum. MDD patients showed increased RSFC between left sgACC and left cerebellar lobule VI after ECT. Ggranger causality analyses (GCA) identified the causal interaction is from left cerebellar lobule VI to left sgACC. Furthermore, increased effective connectivity from left cerebellar lobule VI to left sgACC exhibited positively correlated with the change in verbal fluency test (VFT) score following ECT (r = 0.433, p = 0.039). Our findings indicate that the enhanced cerebro-cerebellar functional connectivity from left lobule VI to left sgACC may ameliorate cognitive impairment induced by ECT. This study identifies a potential neural pathway for mitigation of cognitive impairment following ECT.



Similar content being viewed by others
References
Allen, M. D., & Fong, A. K. (2008). Clinical application of standardized cognitive assessment using fMRI. II. Verbal fluency. Behavioural Neurology, 20, 141–152. https://doi.org/10.3233/ben-2008-0224.
Bai, T., Wei, Q., Wei, W., Wang, A., Wang, J., Ji, G., et al. (2019a). Hippocampal-subregion functional alterations associated with antidepressant effects and cognitive impairments of electro convulsive therapy. Psychological Medicine, 49, 1357–1364. https://doi.org/10.1017/S0033291718002684.
Bai, T., Wei, Q., Zu, M., Wen, X., Wang, J., Ji, G., et al. (2019b). Functional plasticity of the dorsomedial prefrontal cortex in depression reorganized by electroconvulsive therapy: Validation in two independent samples. Human Brain Mapping, 40, 465–473. https://doi.org/10.1002/hbm.24387.
Berman, M. G., Peltier, S., Nee, D. E., Kross, E., Deldin, P. J., & Jonides, J. (2011). Depression, rumination and the default network. Social Cognitive and Affective Neuroscience, 6, 548–555. https://doi.org/10.1093/scan/nsq080.
Chao-Gan, Y., & Yu-Feng, Z. (2010). DPARSF: A MATLAB toolbox for “Pipeline” data analysis of resting-state fMRI. Frontiers in Systems Neuroscience, 4, 13. https://doi.org/10.3389/fnsys.2010.00013.
Chen, S. A., & Desmond, J. E. (2005). Cerebrocerebellar networks during articulatory rehearsal and verbal working memory tasks. Neuroimage, 24, 332–338. https://doi.org/10.1016/j.neuroimage.2004.08.032.
Connolly, C. G., Wu, J., Ho, T. C., Hoeft, F., Wolkowitz, O., Eisendrath, S., et al. (2013). Resting-state functional connectivity of subgenual anterior cingulate cortex in depressed adolescents. Biological Psychiatry, 74, 898–907. https://doi.org/10.1016/j.biopsych.2013.05.036.
Depping, M. S., Wolf, N. D., Vasic, N., Sambataro, F., Hirjak, D., Thomann, P. A., & Wolf, R. C. (2016). Abnormal cerebellar volume in acute and remitted major depression. Progress in Neuro-Psychopharmacology and Biological Psychiatry, 71, 97–102. https://doi.org/10.1016/j.pnpbp.2016.06.005.
Depping, M. S., Nolte, H. M., Hirjak, D., Palm, E., Hofer, S., Stieltjes, B., et al. (2017). Cerebellar volume change in response to electroconvulsive therapy in patients with major depression. Progress in Neuro-Psychopharmacology & Biological Psychiatry, 73, 31–35. https://doi.org/10.1016/j.pnpbp.2016.09.007
Depping, M. S., Wolf, N. D., Vasic, N., Sosic-Vasic, Z., Schmitgen, M. M., Sambataro, F., & Wolf, R. C. (2018). Aberrant resting-state cerebellar blood flow in major depression. Journal of Affective Disorders, 226, 227–231. https://doi.org/10.1016/j.jad.2017.09.028
Drevets, W. C., Savitz, J., & Trimble, M. (2008). The subgenual anterior cingulate cortex in mood disorders. CNS Spectrums, 13, 663–681. https://doi.org/10.1017/s1092852900013754.
Ferrari, A. J., Charlson, F. J., Norman, R. E., Patten, S. B., Freedman, G., Murray, C. J. L., Vos, T., & Whiteford, H. A. (2013). Burden of depressive disorders by country, sex, age, and year: findings from the global burden of disease study 2010. Plos Medicine, 10, e1001547. https://doi.org/10.1371/journal.pmed.1001547.
Gryglewski, G., Baldinger-Melich, P., Seiger, R., Godbersen, G. M., Michenthaler, P., Kloebl, M., et al. (2019). Structural changes in amygdala nuclei, hippocampal subfields and cortical thickness following electroconvulsive therapy in treatment-resistant depression: longitudinal analysis. British Journal of Psychiatry, 214, 159–167. https://doi.org/10.1192/bjp.2018.224.
Guo, W., Liu, F., Xue, Z., Gao, K., Liu, Z., Xiao, C., et al. (2013). Abnormal resting-state cerebellar-cerebral functional connectivity in treatment-resistant depression and treatment sensitive depression. Progress in Neuro-Psychopharmacology & Biological Psychiatry, 44, 51–57. https://doi.org/10.1016/j.pnpbp.2013.01.010
Habas, C., Kamdar, N., Nguyen, D., Prater, K., Beckmann, C. F., Menon, V., & Greicius, M. D. (2009). Distinct cerebellar contributions to intrinsic connectivity networks. Journal of Neuroscience, 29, 8586–8594. https://doi.org/10.1523/jneurosci.1868-09.2009.
Haq, A., Sitzmann, A., Goldman, M., Maixner, D. & Mickey, B. (2015). Response of depression to electroconvulsive therapy: a meta-analysis of clinical predictors. Journal of Clinical Psychiatry, 76, 1374–84. https://doi.org/10.4088/JCP.14r09528.
Harding, I. H., Corben, L. A., Storey, E., Egan, G. F., Stagnitti, M. R., Poudel, G. R., et al. (2016). Fronto-cerebellar dysfunction and dysconnectivity underlying cognition in friedreich ataxia: The IMAGE-FRDA study. Human Brain Mapping, 37, 338–350. https://doi.org/10.1002/hbm.23034.
He, Y., Wang, Y., Chang, T. -T., Jia, Y., Wang, J., Zhong, S., et al. (2018). Abnormal intrinsic cerebro-cerebellar functional connectivity in un-medicated patients with bipolar disorder and major depressive disorder. Psychopharmacology (Berl), 235, 3187–3200. https://doi.org/10.1007/s00213-018-5021-6.
Lai, C. -H., & Wu, Y. -T. (2015). The gray matter alterations in major depressive disorder and panic disorder: Putative differences in the pathogenesis. Journal of Affective Disorders, 186, 1–6. https://doi.org/10.1016/j.jad.2015.07.022
Luna, B., Marek, S., Larsen, B., Tervo-Clemmens, B., & Chahal, R. (2015). An integrative model of the maturation of cognitive control. Annual Review of Neuroscience, 38, 151–170. https://doi.org/10.1146/annurev-neuro-071714-034054.
Ma, Q., Zeng, L. -L., Shen, H., Liu, L., & Hu, D. (2013). Altered cerebellar-cerebral resting-state functional connectivity reliably identifies major depressive disorder. Brain Research, 1495, 86–94. https://doi.org/10.1016/j.brainres.2012.12.002
Marvel, C. L., & Desmond, J. E. (2010). The contributions of cerebro-cerebellar circuitry to executive verbal working memory. Cortex, 46(7), 880–895. https://doi.org/10.1016/j.cortex.2009.08.017
Menon, V. (2011). Large-scale brain networks and psychopathology: a unifying triple network model. Trends in Cognitive Sciences, 15, 483–506. https://doi.org/10.1016/j.tics.2011.08.003.
Moore, D. M., D’Mello, A. M., McGrath, L. M., & Stoodley, C. J. (2017). The developmental relationship between specific cognitive domains and grey matter in the cerebellum. Developmental Cognitive Neuroscience, 24, 1–11. https://doi.org/10.1016/j.dcn.2016.12.001
Mulders, P. C. R., van Eijndhoven, P. F. P., Pluijmen, J., Schene, A. H., Tendolkar, I., & Beckmann, C. F. (2016). Default mode network coherence in treatment-resistant major depressive disorder during electroconvulsive therapy. Journal of Affective Disorders, 205, 130–137. https://doi.org/10.1016/j.jad.2016.06.059
Nuninga, J. O., Claessens, T. F. I., Somers, M., Mandl, R., Nieuwdorp, W., Boks, M. P., et al. (2018). Immediate and long-term effects of bilateral electroconvulsive therapy on cognitive functioning in patients with a depressive disorder. Journal of Affective Disorders, 238, 659–665. https://doi.org/10.1016/j.jad.2018.06.040
O’Reilly, J. X., Beckmann, C. F., Tomassini, V., Ramnani, N., & Johansen-Berg, H. (2010). Distinct and overlapping functional zones in the cerebellum defined by resting state functional connectivity. Cerebral Cortex, 20, 953–965. https://doi.org/10.1093/cercor/bhp157.
Paasonen, J., Stenroos, P., Salo, R. A., Kiviniemi, V., & Gröhn, O. (2018). Functional connectivity under six anesthesia protocols and the awake condition in rat brain. Neuroimage, 172, 9–20. https://doi.org/10.1016/j.neuroimage.2018.01.014.
Perrin, J. S., Merz, S., Bennett, D. M., Currie, J., Steele, D. J., Reid, I. C., & Schwarzbauer, C. (2012). Electroconvulsive therapy reduces frontal cortical connectivity in severe depressive disorder. Proceedings of the National Academy of Sciences of the United States of America, 109, 5464–5468. https://doi.org/10.1073/pnas.1117206109.
Power, J. D., Barnes, K. A., Snyder, A. Z., Schlaggar, B. L., & Petersen, S. E. (2012). Spurious but systematic correlations in functional connectivity MRI networks arise from subject motion. Neuroimage, 59, 2142–2154. https://doi.org/10.1016/j.neuroimage.2011.10.018.
Qiu, H., Li, X., Luo, Q., Li, Y., Zhou, X., Cao, H., et al. (2019). Alterations in patients with major depressive disorder before and after electroconvulsive therapy measured by fractional amplitude of low-frequency fluctuations (fALFF). Journal of Affective Disorders, 244, 92–99. https://doi.org/10.1016/j.jad.2018.10.099
Ramirez-Mahaluf, J. P., Perramon, J., Otal, B., Villoslada, P., & Compte, A. (2018). Subgenual anterior cingulate cortex controls sadness-induced modulations of cognitive and emotional network hubs. Scientific Reports, 8, 8566. https://doi.org/10.1038/s41598-018-26317-4.
Rodriguez-Cano, E., Sarro, S., Monte, G. C., Maristany, T., Salvador, R., McKenna, P. J., & Pomarol-Clotet, E. (2014). Evidence for structural and functional abnormality in the subgenual anterior cingulate cortex in major depressive disorder. Psychological Medicine, 44, 3263–3273. https://doi.org/10.1017/s0033291714000841.
Salmi, J., Pallesen, K. J., Neuvonen, T., Brattico, E., Korvenoja, A., Salonen, O., & Carlson, S. (2010). Cognitive and motor loops of the human cerebrocerebellar system. Journal of Cognitive Neuroscience, 22, 2663–2676. https://doi.org/10.1162/jocn.2009.21382.
Sang, L., Qin, W., Liu, Y., Han, W., Zhang, Y., Jiang, T., & Yu, C. (2012). Resting-state functional connectivity of the vermal and hemispheric subregions of the cerebellum with both the cerebral cortical networks and subcortical structures. Neuroimage, 61, 1213–1225. https://doi.org/10.1016/j.neuroimage.2012.04.011.
Sartorius, A., Demirakca, T., Böhringer, A., von Hohenberg, C. C., Aksay, S. S., Bumb, J. M., et al. (2018). Electroconvulsive therapy induced gray matter increase is not necessarily correlated with clinical data in depressed patients. Brain Stimulation. https://doi.org/10.1016/j.brs.2018.11.017.
Schmahmann, J. D., Doyon, J., McDonald, D., Holmes, C., Lavoie, K., Hurwitz, A. S., Kabani, N., Toga, A., Evans, A., & Petrides, M. (1999). Three-dimensional MRI atlas of the human cerebellum in proportional stereotaxic space. Neuroimage, 10, 233–260.
Schmahmann, J. D. (2004). Disorders of the cerebellum: Ataxia, dysmetria of thought, and the cerebellar cognitive affective syndrome. Journal of Neuropsychiatry and Clinical Neurosciences, 16, 367–378. https://doi.org/10.1176/appi.neuropsych.16.3.367.
Schraa-Tam, C. K. L., Rietdijk, W. J. R., Verbeke, W. J. M. I., Dietvorst, R. C., van den Berg, W. E., Bagozzi, R. P., & De Zeeuw, C. I. (2012). fMRI activities in the emotional cerebellum: a preference for negative stimuli and goal-directed behavior. Cerebellum, 11, 233–245. https://doi.org/10.1007/s12311-011-0301-2.
Shackman, A. J., Salomons, T. V., Slagter, H. A., Fox, A. S., Winter, J. J., & Davidson, R. J. (2011). The integration of negative affect, pain and cognitive control in the cingulate cortex. Nature Reviews Neuroscience, 12, 154–167. https://doi.org/10.1038/nrn2994.
Song, X.-W., Dong, Z.-Y., Long, X.-Y., Li, S.-F., Zuo, X.-N., Zhu, C.-Z., He, Y., Yan, C.-G., & Zang, Y.-F. (2011). REST: A toolkit for resting-state functional magnetic resonance imaging data processing. Plos One, 6, e25031. https://doi.org/10.1371/journal.pone.0025031.
Stoodley, C. J., Valera, E. M., & Schmahmann, J. D. (2012). Functional topography of the cerebellum for motor and cognitive tasks: An fMRI study. Neuroimage, 59, 1560–1570. https://doi.org/10.1016/j.neuroimage.2011.08.065.
Strikwerda-Brown, C., Davey, C. G., Whittle, S., Allen, N. B., Byrne, M. L., Schwartz, O. S., et al. (2014). Mapping the relationship between subgenual cingulate cortex functional connectivity and depressive symptoms across adolescence. Social Cognitive and Affective Neuroscience, 10, 961–968. https://doi.org/10.1093/scan/nsu143.
Takamiya, A., Chung, J. K., Liang, K. -C., Graff-Guerrero, A., Mimura, M., & Kishimoto, T. (2018). Effect of electroconvulsive therapy on hippocampal and amygdala volumes: systematic review and meta-analysis. British Journal of Psychiatry, 212, 19–26. https://doi.org/10.1192/bjp.2017.11.
Tang, C. Y., Ramani, R., Functional, C., & Anesthesia. (2016). Functional Connectivity and Anesthesia. International Anesthesiology Clinics., 54, 143–155. https://doi.org/10.1097/AIA.0000000000000083.
Wang, J., Wei, Q., Bai, T., Zhou, X., Sun, H., Becker, B., et al. (2017). Electroconvulsive therapy selectively enhanced feedforward connectivity from fusiform face area to amygdala in major depressive disorder. Social Cognitive and Affective Neuroscience, 12, 1983–1992. https://doi.org/10.1093/scan/nsx100.
Wang, H., Li, R., Zhou, Y., Wang, Y., Cui, J., Nguchu, B. A., et al. (2018a). Altered cerebro-cerebellum resting-state functional connectivity in HIV-infected male patients. Journal of Neurovirology, 24, 587–596. https://doi.org/10.1007/s13365-018-0649-x.
Wang, J., Wei, Q., Wang, L., Zhang, H., Bai, T., Cheng, L., et al. (2018b). Functional reorganization of intra- and internetwork connectivity in major depressive disorder after electroconvulsive therapy. Human Brain Mapping, 39, 1403–1411. https://doi.org/10.1002/hbm.23928.
Wang, L., Wei, Q., Wang, C., Xu, J., Wang, K., Tian, Y., & Wang, J. (2019). Altered functional connectivity patterns of insular subregions in major depressive disorder after electroconvulsive therapy. Brain Imaging and Behavior. https://doi.org/10.1007/s11682-018-0013-z.
Wei, Q., Tian, Y., Yu, Y., Zhang, F., Hu, X., Dong, Y., Chen, Y., Hu, P., Hu, X., & Wang, K. (2014). Modulation of interhemispheric functional coordination in electroconvulsive therapy for depression. Translational Psychiatry, 4, e453. https://doi.org/10.1038/tp.2014.101.
Wei, Q., Bai, T., Chen, Y., Ji, G., Hu, X., Xie, W., Xiong, Z., Zhu, D., Wei, L., Hu, P., Yu, Y., Wang, K., & Tian, Y. (2018). The changes of functional connectivity strength in electroconvulsive therapy for depression: A longitudinal study. Frontiers in Neuroscience, 12, 661. https://doi.org/10.3389/fnins.2018.00661.
Wong, J. J., O’Daly, O., Mehta, M. A., Young, A. H., & Stone, J. M. (2016). Ketamine modulates subgenual cingulate connectivity with the memory-related neural circuit—a mechanism of relevance to resistant depression? PeerJ, 4, e1710. https://doi.org/10.7717/peerj.1710.
Wu, H., Sun, H., Xu, J., Wu, Y., Wang, C., Xiao, J., She, S., Huang, J., Zou, W., Peng, H., Lu, X., Huang, G., Jiang, T., Ning, Y., & Wang, J. (2016). Changed hub and corresponding functional connectivity of subgenual anterior cingulate cortex in major depressive disorder. Frontiers in Neuroanatomy, 10, 120. https://doi.org/10.3389/fnana.2016.00120.
Xu, L.-Y., Xu, F.-C., Liu, C., Ji, Y.-F., Wu, J.-M., Wang, Y., Wang, H.-B., & Yu, Y.-Q. (2017). Relationship between cerebellar structure and emotional memory in depression. Brain and Behavior, 7, e00738. https://doi.org/10.1002/brb3.738.
Yan, C.-G., Wang, X.-D., Zuo, X.-N., & Zang, Y.-F. (2016). DPABI: Data Processing & Analysis for (Resting-State) Brain Imaging. Neuroinformatics, 14, 339–351. https://doi.org/10.1007/s12021-016-9299-4.
Zhan, C., Liu, Y., Wu, K., Gao, Y., & Li, X. (2017). Structural and functional abnormalities in children with attention-deficit/hyperactivity disorder: A focus on subgenual anterior cingulate cortex. Brain Connect, 7, 106–114. https://doi.org/10.1089/brain.2016.0444.
Zhou, B., Zhao, Q., Teramukai, S., Ding, D., Guo, Q., Fukushima, M., & Hong, Z. (2010). Executive function predicts survival in Alzheimer disease: a study in Shanghai. Journal of Alzheimer’s Disease, 22, 673–682. https://doi.org/10.3233/JAD-2010-100318.
Acknowledgements
Thanks to all medical workers for their contributions and all participants for their participation in this study.
Funding
This study was funded by the National Natural Science Foundation of China (81601187 and 81671354) and Science fund for outstanding youth of Anhui Province (1808085J23).
Author information
Authors and Affiliations
Contributions
Author contributions included study design and protocol writing(YT and WK), literature search and analysis (TB and QW), data collection (MZ, YG and YM), statistical analysis( GJ ), drafting the manuscript(QW and YJ), approval of final version to be published(All authors).
Corresponding authors
Ethics declarations
All procedures involving human participants were in accordance with the ethical standards of the institutional research committee (the Anhui Medical University Ethics Committee: reference number 20160236), and with the 1964 Helsinki declaration and later amendments or comparable ethical standards. All participants provided written informed consent.
Conflict of interest
The authors declared no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wei, Q., Ji, Y., Bai, T. et al. Enhanced cerebro-cerebellar functional connectivity reverses cognitive impairment following electroconvulsive therapy in major depressive disorder. Brain Imaging and Behavior 15, 798–806 (2021). https://doi.org/10.1007/s11682-020-00290-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11682-020-00290-x