Abstract
Purpose
Low bone mineral density (BMD) including low bone mass and osteoporosis is a bone state that carries the risk of fractures and the consequent burden. Since Iran has an aging population and is considered a high-risk country regarding fracture, the objective of this study was to report the low BMD attributable burden in Iran from 1990 to 2019 at national and subnational levels.
Materials and methods
In this study, the Global Burden of Disease (GBD) study 2019 estimates of exposure value and attributable burden were used. For each risk-outcome pair, following the estimation of relative risk, exposure level, and the Theoretical Minimum Risk Exposure Level (TMREL), the Population Attributable Fractions (PAFs) and attributable burden were computed. The Summary Exposure Value (SEV) index was also computed.
Results
Although the age-standardized DALYs and deaths decreased (− 41.0 [95% uncertainty interval: − 45.7 to − 33.2] and − 43.3 [− 48.9 to − 32.5]), attributable all age numbers in Iran increased from 1990 to 2019 (64.3 [50.6 to 89.1] and 66.8 [49.7 to 102.0]). The male gender had a higher low BMD attributed burden in Iran at national and subnational levels except for Tehran. Among low BMD-associated outcomes, motor vehicle road injuries and falls accounted for most of the low BMD-attributed burden in Iran. The SEV for low BMD remained constant from 1990 to 2019 in the country and females had higher SEVs.
Conclusion
Low BMD and the associated outcomes has to gain attention in Iran’s health system due to an aging population. Hence, timely interventions by health systems and the population at stake might assist in reducing the burden attributed to low BMD.






Similar content being viewed by others
Abbreviations
- LBMD:
-
Low Bone Mineral Density
- GBD:
-
Global Burden of Disease
- TMREL:
-
Theoretical Minimum-Risk Exposure Level
- PAFs:
-
Population Attributable Fractions
- SEV:
-
Summary Exposure Value
- SDI:
-
Socio-Demographic Index
References
Shen Y, Huang X, Wu J et al (2022) The global burden of osteoporosis, low bone mass, and its related fracture in 204 countries and territories, 1990–2019. Front Endocrinol (Lausanne) 13:882241. https://doi.org/10.3389/FENDO.2022.882241
Abbafati C, Machado DB, Cislaghi B et al (2020) Global burden of 87 risk factors in 204 countries and territories, 1990–2019: a systematic analysis for the Global Burden of Disease Study 2019. Lancet 396:1223–1249. https://doi.org/10.1016/S0140-6736(20)30752-2
Dong Y, Kang H, Peng R et al (2022) Global, regional, and national burden of low bone mineral density from 1990 to 2019: results from the global burden of disease study 2019. Front Endocrinol (Lausanne) 13:870905. https://doi.org/10.3389/FENDO.2022.870905
Zhang J, Morgan SL, Saag KG (2013) Osteopenia: debates and dilemmas. Curr Rheumatol Rep 15(12):384. https://doi.org/10.1007/s11926-013-0384-5
Aghamohamadi S, Hajinabi K, Jahangiri K et al (2018) Population and mortality profile in the Islamic Republic of Iran, 2006–2035. East Mediterr Heal J 24:469–476. https://doi.org/10.1007/s11926-013-0384-5
Curtis EM, Moon RJ, Harvey NC, Cooper C (2017) The impact of fragility fracture and approaches to osteoporosis risk assessment worldwide. Bone 104:29–38. https://doi.org/10.1016/j.bone.2017.01.024
Abbafati C, Abbas KM, Abbasi-Kangevari M et al (2020) Global burden of 369 diseases and injuries in 204 countries and territories, 1990–2019: a systematic analysis for the Global Burden of Disease Study 2019. Lancet 396:1204–1222. https://doi.org/10.1016/S0140-6736(20)30925-9
Stanaway JD, Afshin A, Gakidou E et al (2018) Global, regional, and national comparative risk assessment of 84 behavioural, environmental and occupational, and metabolic risks or clusters of risks for 195 countries and territories, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet 392:1923–1994. https://doi.org/10.1016/S0140-6736(18)32225-6
Bonjour JP, Theintz G, Law F et al (1994) Peak bone mass. Osteoporos Int 4 (Suppl 1):7–13. https://doi.org/10.1007/BF01623429
Carlson BB, Salzmann SN, Shirahata T et al (2020) Prevalence of osteoporosis and osteopenia diagnosed using quantitative CT in 296 consecutive lumbar fusion patients. Neurosurg Focus 49:1–7. https://doi.org/10.3171/2020.5.FOCUS20241
Qiao D, Liu X, Tu R et al (2020) Gender-specific prevalence and influencing factors of osteopenia and osteoporosis in Chinese rural population: the henan rural cohort Study. BMJ Open 10(1):e028593. https://doi.org/10.1136/bmjopen-2018-028593
Fahimfar N, Noorali S, Yousefi S et al (2021) Prevalence of osteoporosis among the elderly population of Iran. Arch Osteoporos 16(1):16. https://doi.org/10.1007/s11657-020-00872-8
Gambacciani M, Levancini M (2014) Hormone replacement therapy and the prevention of postmenopausal osteoporosis. Przegla̜d Menopauzalny = Menopause Rev 13:213. https://doi.org/10.5114/PM.2014.44996
Rasoul S, Seyed Abbas M, Mashyaneh H et al (2018) Epidemiological study of hospitalized road traffic injuries in Iran 2011. Med J Islam Repub Iran 32:50. https://doi.org/10.14196/mjiri.32.50
Foroutaghe MD, Moghaddam AM, Fakoor V (2019) Time trends in gender-specific incidence rates of road traffic injuries in Iran. PLoS One 14(5):e0216462. https://doi.org/10.1371/journal.pone.0216462
Maharlouei N, Jafarzadeh F, Rezaianzadeh A et al (2020) Survival analysis of patients with hip fracture, Shiraz, Iran. Arch Osteoporos 15(1):33. https://doi.org/10.1007/s11657-020-00714-7
Ghodsi Z, Amanat M, Saeedi Moghaddam S et al (2020) The trend of fall-related mortality at national and provincial levels in Iran from 1990 to 2015. Int J Inj Contr Saf Promot 27:403–411. https://doi.org/10.1080/17457300.2020.1790614
Saadat S, Hafezi-Nejad N, Ekhtiari YS et al (2016) Incidence of fall-related injuries in Iran: A population-based nationwide study. Injury 47:1404–1409. https://doi.org/10.1016/j.injury.2016.05.001
Chang W, Lv H, Feng C et al (2018) Preventable risk factors of mortality after hip fracture surgery: Systematic review and meta-analysis. Int J Surg 52:320–328. https://doi.org/10.1016/j.ijsu.2018.02.061
Panula J, Pihlajamäki H, Mattila VM et al (2011) Mortality and cause of death in hip fracture patients aged 65 or older - A population-based study. BMC Musculoskelet Disord 12:105. https://doi.org/10.1186/1471-2474-12-105
GBD 2016 Healthcare Access and Quality Collaborators (2018) Measuring performance on the healthcare access and quality index for 195 countries and territories and selected subnational locations: a systematic analysis from the global burden of disease study 2016. Lancet (London, England) 391:2236–2271. https://doi.org/10.1016/S0140-6736(18)30994-2
Becker DJ, Kilgore ML, Morrisey MA (2010) The societal burden of osteoporosis. Curr Rheumatol Rep 12:186–191. https://doi.org/10.1007/s11926-010-0097-y
Colón-Emeric CS, Saag KG (2006) Osteoporotic fractures in older adults. Best Pract Res Clin Rheumatol 20:695–706. https://doi.org/10.1016/j.berh.2006.04.004
Ahmadi-Abhari S, Moayyeri A, Abolhassani F (2007) Burden of hip fracture in Iran. Calcif Tissue Int 80:147–153. https://doi.org/10.1007/s00223-006-0242-9
Farzadfar F, Naghavi M, Sepanlou SG et al (2022) Health system performance in Iran: a systematic analysis for the Global Burden of Disease Study 2019. Lancet (London England) 399:1625–1645. https://doi.org/10.1016/S0140-6736(21)02751-3
Pasco JA, Seeman E, Henry MJ et al (2006) The population burden of fractures originates in women with osteopenia, not osteoporosis. Osteoporos Int 17:1404–1409. https://doi.org/10.1007/s00198-006-0135-9
Rajabi M, Ostovar A, Sari AA et al (2021) Direct costs of common osteoporotic fractures (Hip, Vertebral and Forearm) in Iran. BMC Musculoskelet Disord 22:651. https://doi.org/10.1186/s12891-021-04535-8
Chen L, Liu XP, Zhou B et al (2022) Relationship between Change in Bone Mineral Density of Lumbar Spine and Risk of New Vertebral and Nonvertebral Fractures: A Meta-Analysis. Orthop Surg 14:199–206. https://doi.org/10.1111/OS.13184
Watson SL, Weeks BK, Weis LJ et al (2018) High-intensity resistance and impact training improves bone mineral density and physical function in postmenopausal women with osteopenia and osteoporosis: the LIFTMOR randomized controlled trial. J Bone Miner Res 33:211–220. https://doi.org/10.1002/jbmr.3284
Eliakim A, Litmanovitz I, Nemet D (2017) The role of exercise in prevention and treatment of osteopenia of prematurity: An update. Pediatr Exerc Sci 29:450–455. https://doi.org/10.1123/pes.2017-0017
Muñoz-garach A, García-fontana B, Muñoz-torres M (2020) Nutrients and dietary patterns related to osteoporosis. Nutrients 12:1–15. https://doi.org/10.3390/nu12071986
Reid IR, Bolland MJ, Grey A (2014) Effects of vitamin D supplements on bone mineral density: a systematic review and meta-Analysis. Lancet 383:146–155. https://doi.org/10.1016/S0140-6736(13)61647-5
Vatandost S, Jahani M, Afshari A et al (2018) Prevalence of vitamin D deficiency in Iran: a systematic review and meta-analysis. Nutr Health 24:269–278. https://doi.org/10.1177/0260106018802968
Mansouri S, Safabakhsh M, Forooshani A, Shab-Bidar S (2021) The prevalence of vitamin D and calcium supplement use and association with serum 25-Hydroxy-vitamin D (25(OH)D) and demographic and socioeconomic variables in Iranian elderly. Int J Prev Med 12:36. https://doi.org/10.4103/IJPVM.IJPVM_379_18
Esmaily H, Saffaei A (2019) Vitamin D usage among iranian population: a toxicity crisis is on the way. Oman Med J 34:174–175. https://doi.org/10.5001/OMJ.2019.33
Koul PA, Ahmad SH, Ahmad F et al (2011) Vitamin d toxicity in adults: a case series from an area with endemic hypovitaminosis d. Oman Med J 26:201–204. https://doi.org/10.5001/OMJ.2011.49
Acknowledgements
The authors thank the Institute for Health Metrics and Evaluation (IHME) for data provision. Also, the authors sincerely thank all the collaborators who contributed to this study at the Non-Communicable Diseases Research Center (NCDRC) of Endocrinology and Metabolism Research Institute (EMRI) at Tehran University of Medical Sciences.
Funding
None. This study had no funding support and received no grants.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval and consent to participate
This study was approved by the institutional review board of Endocrinology and Metabolism Research Institute at Tehran University of Medical Sciences (IR.TUMS.EMRI.REC.1400.026).
Conflict of interest
Mohammadreza Azangou-Khyavy, Sahar Saeedi Moghaddam, Esmaeil Mohammadi, Parnian Shobeiri, Mohammad-Mahdi Rashidi, Naser Ahmadi, Saba Shahsavan, Zeinab Shirzad Moghaddam, Hanye Sohrabi, Fateme Pourghasem, Reyhaneh Kalantar, Aydin Ghaffari, Seyedeh Melika Hashemi, Negar Rezaei, and Bagher Larijani declare that the research was conducted in the absence of any commercial or financial relationships and declare that they have no conflict of interest.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Below is the link to the electronic supplementary material.
11657_2022_1180_MOESM1_ESM.pdf
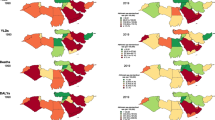
Supplementary file1 Low BMD attributed burden at subnational level among males, females, and both in 1990 and 2019 with percent change. (PDF 455 KB)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Azangou-Khyavy, M., Saeedi Moghaddam, S., Mohammadi, E. et al. Attributable disease burden related to low bone mineral density in Iran from 1990 to 2019: results from the Global Burden of Disease 2019. Arch Osteoporos 17, 140 (2022). https://doi.org/10.1007/s11657-022-01180-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11657-022-01180-z