Abstract
Summary
Osteoporosis in elderly men is an under-recognized problem. In the current study, we intend to look at the performance of two risk assessment tools [OSTA and MORES] for the diagnosis of osteoporosis. Osteoporosis was seen in 1/4th of elderly men at spine and 1/6th of them at femoral neck. Both risk assessment tools were found to have good sensitivity in predicting osteoporosis at spine and femoral neck with good area under curve (AUC).
Purpose
This study attempts to look at the performance of osteoporosis self-assessment tool for Asians (OSTA) and male osteoporosis risk estimation score (MORES) for predicting osteoporosis in south Indian rural elderly men.
Methods
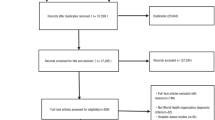
Five hundred and twelve men above 65 years of age from a south Indian rural community were recruited by cluster random sampling. All subjects underwent detailed clinical, anthropometric, and bone mineral density measurement at lumbar spine and femoral neck using dual-energy X-ray absorptiometry scan. A T score ≤ − 2.5 was diagnostic of osteoporosis. Scores for OSTA and MORES were calculated at various cut offs, and their sensitivities and specificities for predicting osteoporosis were derived.
Results
The prevalence of osteoporosis was found to be 16% at femoral neck and 23% at spine. OSTA with a cut-off value of ≤2 predicted osteoporosis with a sensitivity and specificity at lumbar spine of 94 and 17% and at femoral neck of 99 and 18%. The area under ROC curve for OSTA index for spine was 0.716 and for femoral neck was 0.778. MORES with a cut-off value of ≥6 predicted osteoporosis at spine with a sensitivity of 98% and specificity of 15%, and at femoral neck, they were 98 and 13%, respectively. The area under ROC curve for MORES for spine was 0.855 and for femoral neck was 0.760.
Conclusion
OSTA and MORES were found to be useful screening tools for predicting osteoporosis in Indian elderly men. These tools are simple, easy to perform, and cost effective in the context of rural Indian setting.


Similar content being viewed by others
References
Kanis JA, Johnell O, Oden A, Laet CD, Mellstrom D (2004) Epidemiology of osteoporosis and fracture in men. Calcif Tissue Int 75(2):90–99
Haentjens P, Magaziner J, Colón-Emeric CS, Vanderschueren D, Milisen K, Velkeniers B et al (2010) Meta-analysis: excess mortality after hip fracture among older women and men. Ann Intern Med 152(6):380–390
Mithal A, Bansal B, Kyer CS, Ebeling P (2014) The Asia-Pacific regional audit-epidemiology, costs and burden of osteoporosis in India 2013: a report of international osteoporosis foundation. Indian J Endocrinol Metab 18(4):449–454
Marwaha RK, Tandon N, Garg MK, Kanwar R, Narang A, Sastry A et al (2011) Bone health in healthy Indian population aged 50 years and above. Osteoporos Int 22(11):2829–2836
Shetty S, Kapoor N, Naik D, Asha HS, Prabu S, Thomas N, et al. Osteoporosis in healthy South Indian males and the influence of life style factors and vitamin d status on bone mineral density. J Osteoporos. 10.1155/2014/723238
Agrawal NK, Sharma B (2013) Prevalence of osteoporosis in otherwise healthy Indian males aged 50 years and above. Arch Osteoporos 8:116
U.S. Preventive Services Task Force (2002) Screening for osteoporosis in postmenopausal women: recommendations and rationale. Ann Intern Med 137(6):526–528
Genant HK, Cooper C, Poor G, Reid I, Ehrlich G, Kanis J et al (1999) Interim report and recommendations of the World Health Organization task-force for osteoporosis. Osteoporos Int 10(4):259–264
Chen S-J, Chen Y-J, Cheng C-H, Hwang H-F, Chen C-Y, Lin M-R (2016) Comparisons of different screening tools for identifying fracture/osteoporosis risk among community-dwelling older people. Medicine (Baltimore) 95(20):e3415
Cass AR, Shepherd AJ, Asirot R, Mahajan M, Nizami M (2016) Comparison of the male osteoporosis risk estimation score (MORES) with FRAX in identifying men at risk for osteoporosis. Ann Fam Med 14(4):365–369
Bhat KA, Kakaji M, Awasthi A, Kumar K, Mishra K, Shukla M et al (2016) Utility of osteoporosis self-assessment tool as a screening tool for predicting osteoporosis in Indian men. J Clin Densitom. doi:10.1016/j.jocd.2016.04.005
Assessment of fracture risk and its application to screening for postmenopausal osteoporosis. Report of a WHO Study Group. World Health Organ Tech Rep Ser. 1994;843:1–129
Cass AR, Shepherd AJ (2013) Validation of the male osteoporosis risk estimation score (MORES) in a primary care setting. J Am Board Fam Med 26(4):436–444
Koh LK, Sedrine WB, Torralba TP, Kung A, Fujiwara S, Chan SP et al (2001) A simple tool to identify asian women at increased risk of osteoporosis. Osteoporos Int 12(8):699–705
Yang Y, Wang B, Fei Q, Meng Q, Li D, Tang H et al (2013) Validation of an osteoporosis self-assessment tool to identify primary osteoporosis and new osteoporotic vertebral fractures in postmenopausal Chinese women in Beijing. BMC Musculoskelet Disord 14:271
Richy F, Gourlay M, Ross PD, Sen SS, Radican L, De Ceulaer F et al (2004) Validation and comparative evaluation of the osteoporosis self-assessment tool (OST) in a Caucasian population from Belgium. QJM 97(1):39–46
Steuart Richards J, Lazzari AA, Teves Qualler DA, Desale S, Howard R, Kerr GS (2014) Validation of the osteoporosis self-assessment tool in US male veterans. J Clin Densitom 17(1):32–37
Zha X-Y, Hu Y, Pang X-N, Chang G-L, Li L (2015) Diagnostic value of osteoporosis self-assessment tool for Asians (OSTA) and quantitative bone ultrasound (QUS) in detecting high-risk populations for osteoporosis among elderly Chinese men. J Bone Miner Metab 33(2):230–238
Nayak S, Edwards DL, Saleh AA, Greenspan SL (2015) Systematic review and meta-analysis of the performance of clinical risk assessment instruments for screening for osteoporosis or low bone density. Osteoporos Int 26(5):1543–1554
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Rights and permissions
About this article
Cite this article
Satyaraddi, A., Shetty, S., Kapoor, N. et al. Performance of risk assessment tools for predicting osteoporosis in south Indian rural elderly men. Arch Osteoporos 12, 35 (2017). https://doi.org/10.1007/s11657-017-0332-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11657-017-0332-5