Abstract
Purpose
Telemedicine care dramatically expanded during the COVID-19 pandemic. We characterized facilitators and barriers to telemedicine implementation among safety-net primary care clinics serving patients with limited English proficiency (LEP).
Methods
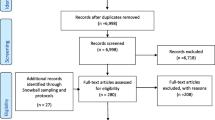
We collected data on telemedicine volume and patient demographics among safety-net clinics participating in a telemedicine learning collaborative. Data on various metrics were reported to the collaborative from February 2019 through August 2021. We conducted semi-structured interviews with clinical and quality leaders, purposively sampling clinics serving high proportions of patients with LEP. We analyzed interviews with a mixed inductive-deductive approach applying the Consolidated Framework for Implementation Research.
Results
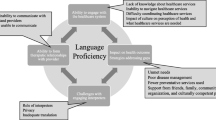
By September 2020, the 23 sites served 121,589 unique patients with in-person and 120,338 with telephone visits; 47% of these patients had LEP. Of 10,897 unique patients served by video visits, 38% had LEP. As a proportion of total visits, telemedicine (telephone and video) visits increased from 0–17% in October 2019–March 2020 to 10–98% in March–August 2020. We conducted 14 interviews at 11 sites. Themes included (1) existing telemedicine platforms and interpreter services were not optimized to support patients with LEP; (2) clinics invested significant labor iterating workflows; (3) sites with technological infrastructure and language-concordant staff were best suited to serve patients; (4) patients speaking less-represented languages or experiencing intersecting literacy barriers were underserved with telemedicine. Interviewees recommended innovations in telemedicine platforms and community-based access.
Conclusions
Safety-net sites relied on existing resources to accommodate patients with LEP, but struggled providing access for the most marginalized. Proactive, data-driven strategies to address patient and community barriers as well as optimize clinical workflows with high-quality, certified medical interpreters are needed to ensure equitable access.



Similar content being viewed by others
References
Selected Social Characteristics in the United States. Published 2019. Accessed May 25, 2022. https://data.census.gov/cedsci/table?q=dp02&tid=ACSDP5Y2019.DP02
Anderson TS, Karliner LS, Lin GA. Association of Primary Language and Hospitalization for Ambulatory Care Sensitive Conditions. Med Care. 2020;58(1):45-51. https://doi.org/10.1097/MLR.0000000000001245
Ponce NA, Hays RD, Cunningham WE. Linguistic Disparities in Health Care Access and Health Status Among Older Adults. Journal of General Internal Medicine. 2006;21(7):786-791. https://doi.org/10.1111/j.1525-1497.2006.00491.x
Rawal S, Srighanthan J, Vasantharoopan A, Hu H, Tomlinson G, Cheung AM. Association Between Limited English Proficiency and Revisits and Readmissions After Hospitalization for Patients With Acute and Chronic Conditions in Toronto, Ontario, Canada. JAMA. 2019;322(16):1605-1607. https://doi.org/10.1001/jama.2019.13066
John-Baptiste A, Naglie G, Tomlinson G, et al. The effect of English language proficiency on length of stay and in-hospital mortality. J GEN INTERN MED. 2004;19(3):221-228. https://doi.org/10.1111/j.1525-1497.2004.21205.x
Nápoles AM, Santoyo-Olsson J, Karliner LS, Gregorich SE, Pérez-Stable EJ. Inaccurate Language Interpretation and its Clinical Significance in the Medical Encounters of Spanish-speaking Latinos. Med Care. 2015;53(11):940-947. https://doi.org/10.1097/MLR.0000000000000422
Flores G. Language Barriers to Health Care in the United States. https://doi.org/10.1056/NEJMp058316. https://doi.org/10.1056/NEJMp058316
Allen MP, Johnson RE, McClave EZ, Alvarado-Little W. Language, Interpretation, and Translation A Clarification and Reference Checklist in Service of Health Literacy and Cultural Respect. NAM Perspectives. Published online February 18, 2020. https://doi.org/10.31478/202002c
Jones CP. Levels of racism: a theoretic framework and a gardener’s tale. Am J Public Health. 2000;90(8):1212-1215. https://doi.org/10.2105/ajph.90.8.1212
Schiaffino MK, Nara A, Mao L. Language Services In Hospitals Vary By Ownership And Location. Health Affairs. 2016;35(8):1399-1403. https://doi.org/10.1377/hlthaff.2015.0955
Fernandez A, Schillinger D, Warton EM, et al. Language Barriers, Physician-Patient Language Concordance, and Glycemic Control Among Insured Latinos with Diabetes: The Diabetes Study of Northern California (DISTANCE). J Gen Intern Med. 2011;26(2):170-176. https://doi.org/10.1007/s11606-010-1507-6
Saadi A, Sanchez Molina U, Franco-Vasquez A, Inkelas M, Ryan GW. Barriers and Facilitators to Implementation of Health System Interventions Aiming to Welcome and Protect Immigrant Patients: a Qualitative Study. J Gen Intern Med. 2021;36(10):3071-3079. https://doi.org/10.1007/s11606-021-06788-4
Saadi A, Sanchez Molina U, Franco-Vasquez A, Inkelas M, Ryan GW. Assessment of Perspectives on Health Care System Efforts to Mitigate Perceived Risks Among Immigrants in the United States: A Qualitative Study. JAMA Network Open. 2020;3(4):e203028. https://doi.org/10.1001/jamanetworkopen.2020.3028
Title VI of the Civil Rights Act of 1964; Policy Guidance on the Prohibition Against National Origin Discrimination As It Affects Persons With Limited English Proficiency. Federal Register. Published August 30, 2000. Accessed November 14, 2021. https://www.federalregister.gov/documents/2000/08/30/00-22140/title-vi-of-the-civil-rights-act-of-1964-policy-guidance-on-the-prohibition-against-national-origin
Volk J, Palanker D, O’Brien M, Goe C. States’ Actions to Expand Telemedicine Access During COVID-19 and Future Policy Considerations. The Commonwealth Fund. https://doi.org/10.26099/r95z-bs17
Jun 22 EHP, 2020. State Efforts to Expand Medicaid Coverage & Access to Telehealth in Response to COVID-19. KFF. Published June 22, 2020. Accessed December 17, 2021. https://www.kff.org/coronavirus-covid-19/issue-brief/state-efforts-to-expand-medicaid-coverage-access-to-telehealth-in-response-to-covid-19/
Cantor JH, McBain RK, Pera MF, Bravata DM, Whaley CM. Who Is (and Is Not) Receiving Telemedicine Care During the COVID-19 Pandemic. Am J Prev Med. 2021;61(3):434-438. https://doi.org/10.1016/j.amepre.2021.01.030
Uscher-Pines L, Sousa J, Jones M, et al. Telehealth Use Among Safety-Net Organizations in California During the COVID-19 Pandemic. JAMA. 2021;325(11):1106-1107. https://doi.org/10.1001/jama.2021.0282
López L, Green AR, Tan-McGrory A, King RS, Betancourt JR. Bridging the Digital Divide in Health Care: The Role of Health Information Technology in Addressing Racial and Ethnic Disparities. The Joint Commission Journal on Quality and Patient Safety. 2011;37(10):437-445. https://doi.org/10.1016/S1553-7250(11)37055-9
David E. Velasquez BS, Adam L. Beckman BS, Jorge A. Rodriguez MD. The Missing Strategy in Addressing Language Barriers. The American Journal of Managed Care. 2020;27(3). Accessed June 22, 2022. https://www.ajmc.com/view/the-missing-strategy-in-addressing-language-barriers
Gilson SF, Umscheid CA, Laiteerapong N, Ossey G, Nunes KJ, Shah SD. Growth of Ambulatory Virtual Visits and Differential Use by Patient Sociodemographics at One Urban Academic Medical Center During the COVID-19 Pandemic: Retrospective Analysis. JMIR Medical Informatics. 2020;8(12):e24544. https://doi.org/10.2196/24544
Rodriguez JA, Betancourt JR, Sequist TD, Ganguli I. Differences in the use of telephone and video telemedicine visits during the COVID-19 pandemic. Am J Manag Care. 2021;27(1):21-26. https://doi.org/10.37765/ajmc.2021.88573
Park J, Erikson C, Han X, Iyer P. Are State Telehealth Policies Associated With The Use Of Telehealth Services Among Underserved Populations? Health Affairs. 2018;37(12):2060-2068. https://doi.org/10.1377/hlthaff.2018.05101
Chang JE, Lindenfeld Z, Albert SL, et al. Telephone vs. Video Visits During COVID-19: Safety-Net Provider Perspectives. J Am Board Fam Med. 2021;34(6):1103-1114. https://doi.org/10.3122/jabfm.2021.06.210186
Benjenk I, Franzini L, Roby D, Chen J. Disparities in Audio-only Telemedicine Use Among Medicare Beneficiaries During the Coronavirus Disease 2019 Pandemic. Medical Care. 2021;59(11):1014-1022. https://doi.org/10.1097/MLR.0000000000001631
Reed ME, Huang J, Graetz I, et al. Patient Characteristics Associated With Choosing a Telemedicine Visit vs Office Visit With the Same Primary Care Clinicians. JAMA Netw Open. 2020;3(6):e205873. https://doi.org/10.1001/jamanetworkopen.2020.5873
Nouri S, Khoong EC, Lyles CR, Karliner L. Addressing Equity in Telemedicine for Chronic Disease Management During the Covid-19 Pandemic. NEJM Catalyst Innovations in Care Delivery. Published online May 4, 2020. Accessed November 13, 2021. https://catalyst.nejm.org/doi/full/10.1056/CAT.20.0123
Eberly LA, Khatana SAM, Nathan AS, et al. Telemedicine Outpatient Cardiovascular Care During the COVID-19 Pandemic. Circulation. 2020;142(5):510-512. https://doi.org/10.1161/CIRCULATIONAHA.120.048185
Hsueh L, Huang J, Millman AK, et al. Disparities in Use of Video Telemedicine Among Patients With Limited English Proficiency During the COVID-19 Pandemic. JAMA Network Open. 2021;4(11):e2133129. https://doi.org/10.1001/jamanetworkopen.2021.33129
Rodriguez JA, Saadi A, Schwamm LH, Bates DW, Samal L. Disparities In Telehealth Use Among California Patients With Limited English Proficiency. Health Affairs. 2021;40(3):487-495. https://doi.org/10.1377/hlthaff.2020.00823
Merid B, Robles MC, Nallamothu BK. Digital Redlining and Cardiovascular Innovation. Circulation. 2021;144(12):913-915. https://doi.org/10.1161/CIRCULATIONAHA.121.056532
Skinner B, Levy H, Burtch T. Digital redlining: the relevance of 20th century housing policy to 21st century broadband access and education. EdWorking Paper, Retrieved from Annenberg Institute at Brown University. 2021;21(471). 10.26300/Q9AV-9C93
Vogels E a. Digital divide persists even as Americans with lower incomes make gains in tech adoption. Pew Research Center. Accessed November 13, 2021. https://www.pewresearch.org/fact-tank/2021/06/22/digital-divide-persists-even-as-americans-with-lower-incomes-make-gains-in-tech-adoption/
Atske S, Perrin R. Home broadband adoption, computer ownership vary by race, ethnicity in the U.S. Pew Research Center. Accessed November 14, 2021. https://www.pewresearch.org/fact-tank/2021/07/16/home-broadband-adoption-computer-ownership-vary-by-race-ethnicity-in-the-u-s/
Connected Care Accelerator. Center for Care Innovations. Accessed January 12, 2021. https://www.careinnovations.org/programs/connected-care-accelerator/
Uniform Data System Reporting Requirements for 2022 Health Center Data. Bureau of Primary Health Care; 2022. https://bphc.hrsa.gov/sites/default/files/bphc/data-reporting/2022-uds-manual.pdf
Walker D, Myrick F. Grounded theory: an exploration of process and procedure. Qual Health Res. 2006;16(4):547-559. https://doi.org/10.1177/1049732305285972
Damschroder LJ, Lowery JC. Evaluation of a large-scale weight management program using the consolidated framework for implementation research (CFIR). Implement Sci. 2013;8(1):51. https://doi.org/10.1186/1748-5908-8-51
Damschroder L, Aron D, Keith R, Kirsh S, Alexander J, Lowery J. Fostering implementation of health services research findings into practice: a consolidated framework for advancing implementation science. Implementation science : IS. 2009;4. https://doi.org/10.1186/1748-5908-4-50
Tong A, Sainsbury P, Craig J. Consolidated criteria for reporting qualitative research (COREQ): a 32-item checklist for interviews and focus groups. International Journal for Quality in Health Care. 2007;19(6):349-357. https://doi.org/10.1093/intqhc/mzm042
Community Health Centers: 2021 State Profile. California Primary Care Association; 2021. https://www.dropbox.com/s/fk25l6guc1prqv0/2021_CPCA_CAstateprofile.pdf?dl=0
Serving Patients with Limited English Proficiency: Results of a Community Health Center Survey. National Association of Community Health Centers; 2008. http://nachc.org/wp-content/uploads/2015/06/LEPReport.pdf
Eberly LA, Kallan MJ, Julien HM, et al. Patient Characteristics Associated With Telemedicine Access for Primary and Specialty Ambulatory Care During the COVID-19 Pandemic. JAMA Netw Open. 2020;3(12):e2031640. https://doi.org/10.1001/jamanetworkopen.2020.31640
Pagán VM, McClung KS, Peden CJ. An Observational Study of Disparities in Telemedicine Utilization in Primary Care Patients Before and During the COVID-19 Pandemic. Telemed J E Health. Published online December 20, 2021. https://doi.org/10.1089/tmj.2021.0412
Sachs JW, Graven P, Gold JA, Kassakian SZ. Disparities in telephone and video telehealth engagement during the COVID-19 pandemic. JAMIA Open. 2021;4(3):ooab056. https://doi.org/10.1093/jamiaopen/ooab056
El-Toukhy S, Méndez A, Collins S, Pérez-Stable EJ. Barriers to Patient Portal Access and Use: Evidence from the Health Information National Trends Survey. J Am Board Fam Med. 2020;33(6):953-968. https://doi.org/10.3122/jabfm.2020.06.190402
Payán DD, Frehn JL, Garcia L, Tierney AA, Rodriguez HP. Telemedicine implementation and use in community health centers during COVID-19: Clinic personnel and patient perspectives. SSM - Qualitative Research in Health. 2022;2:100054. https://doi.org/10.1016/j.ssmqr.2022.100054
Nguyen MLT, Garcia F, Juarez J, et al. Satisfaction can co-exist with hesitation: qualitative analysis of acceptability of telemedicine among multi-lingual patients in a safety-net healthcare system during the COVID-19 pandemic. BMC Health Serv Res. 2022;22(1):195. https://doi.org/10.1186/s12913-022-07547-9
Rodriguez JA, Clark CR, Bates DW. Digital Health Equity as a Necessity in the 21st Century Cures Act Era. JAMA. 2020;323(23):2381-2382. https://doi.org/10.1001/jama.2020.7858
Khoong EC. Policy Considerations To Ensure Telemedicine Equity. Health Aff (Millwood). 2022;41(5):643-646. https://doi.org/10.1377/hlthaff.2022.00300
Lyles C, Sharma A, Fields J, Getachew Y, Sarkar U, Zephyrin L. Centering Health Equity in Telemedicine. Annals of Family Medicine. Accepted, In Press;20(4).
Moreno MR, Otero-Sabogal R, Newman J. Assessing Dual-Role Staff-Interpreter Linguistic Competency in an Integrated Healthcare System. J GEN INTERN MED. 2007;22(S2):331-335. https://doi.org/10.1007/s11606-007-0344-8
Engstrom DW, Piedra LM, Min JW. Bilingual Social Workers: Language and Service Complexities. Administration in Social Work. 2009;33(2):167-185. https://doi.org/10.1080/03643100902768832
Crenshaw. Demarginalizing the Intersection of Race and Sex: A Black Feminist Critique of Antidiscrimination Doctrine, Feminist Theory and Antiracist Politics. University of Chicago Legal Forum. 1989(1). Accessed April 12, 2022. https://chicagounbound.uchicago.edu/uclf/vol1989/iss1/8
Goodman R, Lacktman N, Ferrante T. Medicare Telehealth Services for 2023 – CMS Proposes Substantial Changes | Foley & Lardner LLP. Health Care Law Today. Published July 14, 2022. Accessed July 28, 2022. https://www.foley.com/en/insights/publications/2022/07/medicare-telehealth-services-2023-cms-changes
Alkureishi MA, Choo ZY, Rahman A, et al. Digitally Disconnected: Qualitative Study of Patient Perspectives on the Digital Divide and Potential Solutions. JMIR Hum Factors. 2021;8(4):e33364. https://doi.org/10.2196/33364
Anaya YBM, Mota AB, Hernandez GD, Osorio A, Hayes-Bautista DE. Post-Pandemic Telehealth Policy for Primary Care: An Equity Perspective. J Am Board Fam Med. 2022;35(3):588-592. https://doi.org/10.3122/jabfm.2022.03.210509
Basu G, Costa VP, Jain P. Clinicians’ obligations to use qualified medical interpreters when caring for patients with limited English proficiency. AMA journal of ethics. 2017 Mar 1;19(3):245-52.
Lion KC, Gritton J, Scannell J, et al. Patterns and Predictors of Professional Interpreter Use in the Pediatric Emergency Department. Pediatrics. 2021;147(2):e20193312. https://doi.org/10.1542/peds.2019-3312
Schulson LB, Anderson TS. National Estimates of Professional Interpreter Use in the Ambulatory Setting. J GEN INTERN MED. 2022;37(2):472-474. https://doi.org/10.1007/s11606-020-06336-6
Karliner LS, Jacobs EA, Chen AH, Mutha S. Do professional interpreters improve clinical care for patients with limited English proficiency? A systematic review of the literature. Health Serv Res. 2007;42(2):727-754. https://doi.org/10.1111/j.1475-6773.2006.00629.x
Charting a Course for an Equity-Centered Data System. Robert Wood Johnson Foundation | National Commission to Transform Public Health Data Systems; 2021. Accessed October 5, 2022. https://www.rwjf.org/en/library/research/2021/10/charting-a-course-for-an-equity-centered-data-system.html
Acknowledgements
The authors would like to thank all participants in the Connected Care Accelerator, and all the interviewees, Erica Shin, BA, Elaine Khoong, MD, MAS, Sofi Bergkvist, MS, MBA, and Jeanette Wong, BS.
Funding
This work was supported by The Commonwealth Fund, a national, private foundation based in New York City that supports independent research on healthcare issues and makes grants to improve healthcare practice and policy (Grant No. 20202842). The views presented here are those of the author and not necessarily those of The Commonwealth Fund, its directors, officers, or staff. The Connected Care Accelerator was supported by the California Health Care Foundation (Grant No. G-31003). Dr. Sharma was supported by K08 HS028477-01 (Agency for Healthcare Research and Quality) and KL2 TR001870 (National Center for Advancing Translational Sciences of the National Institutes of Health). Dr. Sarkar was supported by K24 CA212294 (National Cancer Institute).This paper’s contents are solely the responsibility of the authors and do not necessarily represent the official views of AHRQ nor the NIH.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest:
Dr Sarkar received contract funding from InquisitHealth, AppliedVR, and SomnologyMD; is supported by a gift from The Doctors Company Foundation; serves as a scientific/expert advisor for nonprofit organizations HealthTech 4 Medicaid and HopeLab (no compensation); is a member of the American Medical Association’s Equity and Innovation Advisory Group (for which she receives honoraria); and previously served as a clinical advisor for Omada Health and as an advisory board member for Doximity (for which she received honoraria). Dr. Lyles received contract funding from InquisitHealth, AppliedVR, and SomnologyMD. She is currently a Visiting Researcher at Google.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOCX 89 kb)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sharma, A.E., Lisker, S., Fields, J.D. et al. Language-Specific Challenges and Solutions for Equitable Telemedicine Implementation in the Primary Care Safety Net During COVID-19. J GEN INTERN MED 38, 3123–3133 (2023). https://doi.org/10.1007/s11606-023-08304-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-023-08304-2