Abstract
Objective
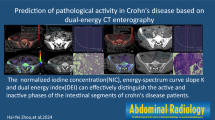
To investigate the value of dual-energy CT (DECT) imaging in the diagnosis of nonspecific terminal ileitis (NTI).
Materials and methods
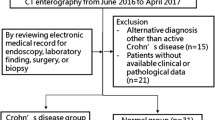
This is a retrospective study, enrolling patients with symptomatic terminal ileitis that underwent conventional multidetector CT (MDCT) enterography or DECT enterography. The sensitivity of the diagnosis of NTI between MDCT images and different kinds of DECT images (40–70 kev virtual monoenergetic images (VMIs) and iodine density images) was compared. The iodine concentrations of lesion bowel wall among NTI, Crohn's disease (CD) and intestinal tuberculosis (ITB) in DECT group and the value of lesion-to-non-lesion contrast ratios of all patients were measured. Receiver operator characteristic (ROC) curves for normalized iodine concentration (NIC) for differentiating among the three kinds of disease were drawn.
Results
The sensitivity for the diagnosis of NTI in DECT group (including 40 kev, 50 keV VMIs, and iodine density images) were all 89.7%, significantly higher than that in MDCT group (65.1%) (P = 0.026). Statistical analysis did not reveal marked differences between 60 kev, 70 kev VMIs (86.2%) and MDCT images (65.1%) (P = 0.059). The NIC of NTI was (0.15 ± 0.04)100 µg/cm3 and (0.45 ± 0.08)100 µg/cm3, significantly lower than that of CD (0.34 ± 0.09) 100 µg/cm3, (0.85 ± 0.06) 100 µg/cm3 and that of ITB (0.29 ± 0.07) 100 µg/cm3, (0.88 ± 0.07) 100 µg/cm3 at the enteric phase (EP) and portal venous phase (PVP) (P < 0.001, wholly). The area under the ROC curves (AUROCs) of NICEP and NICPVP were 0.910 and 0.980, respectively, for differentiating between NTI and CD. The value of lesion-to-non-lesion contrast ratios is maximum on the 40 keV VMI both EP and PVP. The value of lesion-to-non-lesion contrast ratios of NTI was lower than that of CD and ITB on each image. The AUROCs of NICEP and NICPVP were 0.875 and 0.940, respectively, for differentiating between NTI and ITB.
Conclusions
DECT has higher sensitivity in the diagnosis of NTI than MDCT. Low-keV VMI and iodine density images of DECT can clearly show the NTI. DECT imaging can help to differentiate NTI from CD or ITB by comparing the NIC.






Similar content being viewed by others
References
Kim DH, Cheon JH. Intestinal Behçet’s disease: a true inflammatory bowel disease or merely an intestinal complication of systemic vasculitis? Yonsei Med J. 2016. https://doi.org/10.3349/ymj.2016.57.1.22.
Adamek HE, Schantzen W, Rinas U, Goyen M, Ajaj W, Esser C. Ultra-high-field magnetic resonance enterography in the diagnosis of ileitis (Neo-)terminalis: a prospective study. J Clin Gastroenterol. 2012. https://doi.org/10.1097/MCG.0b013e31822fec0c.
Dilauro S, Crum-Cianflone NF. Ileitis: when it is not Crohn’s disease. Curr Gastroenterol Rep. 2010. https://doi.org/10.1007/s11894-010-0112-5.
Balthazar EJ, Megibow AJ, Siegel SE, Birnbaum BA. Appendicitis: prospective evaluation with high-resolution CT. Radiology. 1991. https://doi.org/10.1148/radiology.180.1.2052696.
Günther C, Ruder B, Stolzer I, Dorner H, He GW, Chiriac MT, et al. Interferon lambda promotes paneth cell death via STAT1 signaling in mice and is increased in inflamed ileal tissues of patients with Crohn’s disease. Gastroenterology. 2019. https://doi.org/10.1053/j.gastro.2019.07.031.
Kedia S, Kurrey L, Pratap Mouli V, Dhingra R, Srivastava S, Pradhan R, et al. Frequency, natural course and clinical significance of symptomatic terminal ileitis. J Dig Dis. 2016. https://doi.org/10.1111/1751-2980.12307.
Goulart RA, Barbalho SM, Gasparini RG, de Carvalho AC. Facing terminal ileitis: going beyond Crohn’s disease. Gastroenterol Res. 2016. https://doi.org/10.14740/gr698w.
Erden A, Kuru Öz D, Gürsoy Çoruh A, Erden İ, Özalp Ateş FS, Törüner M. Backwash ileitis in ulcerative colitis: are there MR enterographic features that distinguish it from Crohn disease? Eur J Radiol. 2019. https://doi.org/10.1016/j.ejrad.2018.11.027.
Dane B, O’Donnell T, Ream J, Chang S, Megibow A. Novel dual-energy computed tomography enterography iodine density maps provide unique depiction of Crohn disease activity. J Comput Assist Tomogr. 2020. https://doi.org/10.1097/RCT.0000000000001009.
Parakh A, Lennartz S, An C, Rajiah P, Yeh BM, Simeone FJ, et al. Dual-energy CT images: pearls and pitfalls. Radiographics. 2021. https://doi.org/10.1148/rg.2021200102.
Lin XZ, Miao F, Li JY, Dong HP, Shen Y, Chen KM. High-definition CT Gemstone spectral imaging of the brain: initial results of selecting optimal monochromatic image for beam-hardening artifacts and image noise reduction. J Comput Assist Tomogr. 2011. https://doi.org/10.1097/RCT.0b013e3182058d5c.
Zhao LQ, He W, Li JY, Chen JH, Wang KY, Tan L. Improving image quality in portal venography with spectral CT imaging. Eur J Radiol. 2012. https://doi.org/10.1016/j.ejrad.2011.02.063.
Lv P, Lin XZ, Li J, Li W, Chen K. Differentiation of small hepatic hemangioma from small hepatocellular carcinoma: recently introduced spectral CT method. Radiology. 2011. https://doi.org/10.1148/radiol.11101425.
Shang J, Zhou LP, Wang H, Liu B. Diagnostic performance of dual-energy CT versus ultrasonography in gout: a meta-analysis. Acad Radiol. 2020. https://doi.org/10.1016/j.acra.2020.08.030.
Zhao XS, Wang ZT, Wu ZY, Yin QH, Zhong J, Miao F, et al. Differentiation of Crohn’s disease from intestinal tuberculosis by clinical and CT enterographic models. Inflamm Bowel Dis. 2014. https://doi.org/10.1097/MIB.0000000000000025.
Goyal P, Shah J, Gupta S, Gupta P, Sharma V. Imaging in discriminating intestinal tuberculosis and Crohn’s disease: past, present and the future. Expert Rev Gastroenterol Hepatol. 2019. https://doi.org/10.1080/17474124.2019.1673730.
van der Merwe BS, Ackermann C, Els H. CT enteroclysis in the developing world: how we do it, and the pathology we see. Eur J Radiol. 2013. https://doi.org/10.1016/j.ejrad.2013.03.018.
Zhu C, Yu Y, Wang S, Wang X, Gao Y, et al. A novel clinical radiomics nomogram to identify Crohn’s disease from intestinal tuberculosis. J Inflamm Res. 2021. https://doi.org/10.2147/JIR.S344563.
Jung D, Heiss R, Kramer V, Thoma OM, Regensburger AP, Rascher W, et al. Contrast-enhanced µCT for visualizing and evaluating murine intestinal inflammation. Theranostics. 2018. https://doi.org/10.7150/thno.26013.
Wang L, Liu B, Wu XW, Wang J, Zhou Y, Wang WQ, et al. Correlation between CT attenuation value and iodine concentration in vitro: discrepancy between gemstone spectral imaging on single-source dual-energy CT and traditional polychromatic X-ray imaging. J Med Imaging Radiat Oncol. 2012. https://doi.org/10.1111/j.1754-9485.2012.02379.x.
Park YS, Jun DW, Kim SH, Lee HH, Jo YJ, Song MH, et al. Colonoscopy evaluation after short-term anti-tuberculosis treatment in nonspecific ulcers on the ileocecal area. World J Gastroenterol. 2008. https://doi.org/10.3748/wjg.14.5051.
Dane B, Sarkar S, Nazarian M, Galitzer H, O’Donnell T, Remzi F, Megibow A, et al. Crohn disease active inflammation assessment with iodine density from dual-energy CT enterography: comparison with histopathologic analysis. Radiology. 2021. https://doi.org/10.1148/radiol.2021204405.
Yao J, Jiang Y, Ke J, Lu Y, Hu J, Zhi M. A validated prognostic model and nomogram to predict early-onset complications leading to surgery in patients with Crohn’s disease. Dis Colon Rectum. 2020. https://doi.org/10.1097/DCR.0000000000001881.
Kim YS, Kim SH, Ryu HS, Han JK. Iodine quantification on spectral detector-based dual-energy CT enterography: correlation with Crohn’s disease activity index and external validation. Korean J Radiol. 2018. https://doi.org/10.3348/kjr.2018.19.6.1077.
Tanoue S, Nakaura T, Nagayama Y, Uetani H, Ikeda O, Yamashita Y. Virtual monochromatic image quality from dual-layer dual-energy computed tomography for detecting brain tumors. Korean J Radiol. 2021. https://doi.org/10.3348/kjr.2020.0677.
Dar G, Goldberg SN, Hiller N, Caplan N, Sosna J, Appelbaum L, Lev-Cohain N. CT severity indices derived from low monoenergetic images at dual-energy CT may improve prediction of outcome in acute pancreatitis. Eur Radiol. 2021. https://doi.org/10.1007/s00330-020-07477-2.
Rizzo S, Radice D, Femia M, De Marco P, Origgi D, Preda L, et al. Metastatic and non-metastatic lymph nodes: quantification and different distribution of iodine uptake assessed by dual-energy CT. Eur Radiol. 2018. https://doi.org/10.1007/s00330-017-5015-5.
Goo HW, Goo JM. Dual-energy CT: New horizon in medical imaging. Korean J Radiol. 2017. https://doi.org/10.3348/kjr.2017.18.4.555.
Marin D, Boll DT, Mileto A, Nelson RC. State of the art: dual-energy CT of the abdomen. Radiology. 2014. https://doi.org/10.1148/radiol.14131480.
Siegel MJ, Kaza RK, Bolus DN, Boll DT, Rofsky NM, De Cecco CN, et al. White paper of the society of computed body tomography and magnetic resonance on dual-energy CT, Part 1: technology and terminology. J Comput Assist Tomogr. 2016. https://doi.org/10.1097/RCT.0000000000000531.
Fulwadhva UP, Wortman JR, Sodickson AD. Use of dual-energy CT and iodine maps in evaluation of bowel disease. Radiographics. 2016. https://doi.org/10.1148/rg.2016150151.
Acknowledgements
The authors thank Dr. Xingwang Wu from The First Affiliated Hospital of Anhui Medical University, for the critical reading of the manuscript. The authors also thank Dr. Xia Wang, from the department of radiology of the same hospital, for clinical assistance.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Xu, X., Zhu, J., Wang, X. et al. Diagnostic performance of dual-energy CT in nonspecific terminal ileitis. Jpn J Radiol 40, 1069–1078 (2022). https://doi.org/10.1007/s11604-022-01288-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11604-022-01288-9