Summary
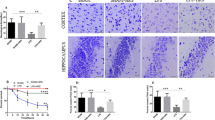
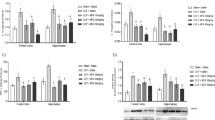
To investigate the interaction and involvement of sodium hydrosulfide (NaHS), a H2S donor, on hippocampus of rats suffering from sepsis-associated encephalopathy, rats were subjected to cecal ligation and puncture (CLP)-induced sepsis. Adult male Sprague-Dawley rats were randomly divided into four groups: Sham group, CLP group, CLP+NaHS group and CLP+aminooxyacetic acid (AOAA, an inhibitor of H2S formation) group. The four groups were observed at 3, 6, 9, 12 h after treatment. We examined hippocampal H2S synthesis and the expression of cystathionine-β-synthetase (CBS), a major enzyme involved in the H2S synthesis in hippocampus. CBS expression was detected by reverse transcription polymerase chain reaction (RT-PCR). The concentrations of inflammatory cytokines (TNF-α, IL-1β) were determined in hippocampus by using enzyme-linked immunosorbent assay (ELISA). Neuronal damage was studied by histological examination of hippocampus. In CLP group, H2S synthesis was significantly increased in hippocampus compared with sham group and it peaked 3 h after CLP (P<0.05). Sepsis also resulted in a significantly upregulated CBS mRNA in hippocampus. The levels of TNF-α and IL-1β in the hippocampus were substantially elevated at each time point of measurement (P<0.05), and they also reached a peak value at about 3 h. Administration of NaHS significantly aggravated sepsis-associated hippocampus inflammation, as evidenced by TNF-α and IL-1β activity and histological changes in hippocampus. In septic rats pretreated with AOAA, sepsis-associated hippocampus inflammation was reduced. It is concluded that the rats subjected to sepsis may suffer from brain injury and elevated pro-inflammatory cytokines are responsible for the process. Furthermore, administration of H2S can increase injurious effects and treatment with AOAA can protect the brain from injury.
Similar content being viewed by others
References
Zhang H, Zhi L, Moochhala SM, et al. Endogenous hydrogen sulfide regulates leukocyte trafficking in cecal ligation and puncture-induced sepsis. J Leukoc Biol, 2007,82(4):894–905
Augus DC, Linde-Zwirble WT, Lidicker J, et al. Epidemiology of severe sepsis in the United States: analysis of incidence, outcome, and associated costs of care. Crit Care Med, 2001,29(7):1303–1310
Dellinger RP, Levy MM, Carlet J M, et al. Surviving sepsis campaign: international guidelines for management of severe sepsis and septic shock. Crit Care Med, 2008,36(1):296–327
Ebersoldt M, Sharshar T, Annane D. Sepsis-associated delirium. Intensive Care Med, 2007,33(6):941–950
Pytel P, Alexander JJ. Pathogenesis of septic encephalopathy. Curr Opin Neurol, 2009,22(3):283–287
Tamizhselvi R, Moore P K, Bhatia M. Hydrogen sulfide acts as a mediator of inflammation in acute pancreatitis: in vitro studies using isolated mouse pancreatic acinar cells. J Cell Mol Med, 2007,11(2):315–326
Hu LF, Wong PT, Moore PK, et al. Hydrogen sulfide attenuates lipopolysaccharide-induced inflammation by inhibition of p38 mitogen-activated protein kinase in microglia. J Neurochem, 2007,100(4):1121–1128
Collin M, Anuar FB, Murch O, et al. Inhibition of endogenous hydrogen sulfide formation reduces the organ injury caused by endotoxemia. Br J Pharmacol, 2005, 146(4):498–505
Zhang H, Zhi L, Moore PK, et al. Role of hydrogen sulfide in cecal ligation and puncture-induced sepsis in the mouse. Am J Physiol Lung Cell Mol Physiol, 2006,290(6): L1193–L1201
Abe K, Kimura H. The possible role of hydrogen sulfide as an endogenous neuromodulator. J Neuroscience, 1996, 16(3):1066–1071
Daniel R, Markus S, Michael A, et al. Immunodesign of experimental sepsis by cecal ligation and puncture. Nature Protocols, 2009,4(1):31–36
Szabo C. Hydrogen sulphide and its therapeutic potential. Nat Rev Drug Discov, 2007,6(11):917–935
Minamishima S, Bougaki M, Sips PY, et al. Hydrogen sulfide improves survival after cardiac arrest and cardiopulmonary resuscitation via a nitric oxide synthase 3-dependent mechanism in mice. Circulation, 2009,120(10):888–896
Li L, Bhatia M, Zhu YZ, et al. Hydrogen sulfide is a novel mediator of lopopolysaccharide-induced inflammation in the mouse. FASEB J, 2005,19(9),1196-1198
Kafa IM, Uysal M, Bakirci S, et al. Sepsis induces apoptotic cell death in different regions of the brain in a rat model of sepsis. Acta Neurobiol Exp, 2010,70(3): 246–260
Papadopoulos MC, Davies DC, Moss RF, et al. Pathophysiology of septic encephalopathy: a review. Crit Care Med, 2000,28(8):3019–3024
Green R, Scott LK, Minagar A, et al. Sepsis associated encephalopathy (SAE): a review. Front Biosci, 2004,9(5): 1637–1641
Annane D. Hippocampus: a future target for sepsis treatment. Intensive Care Med, 2009,35(4):585–586
Kim P K, Deutschman C S. Inflammatory responses and mediators. Surg Clin North Am, 2000,80(3):885–894
Bucova M. Role of cytokines in the development of local and systemic inflammation and septic shock. Vnitr Lek, 2002,48(8):755–762
Alexander JJ, Jacob A, Cunningham P, et al. TNF is a key mediator of septic encephalopathy acting through its receptor, TNF receptor-1. Neurochem Int, 2008,52(3): 447–456
Lynch AM, Walsh C, Delaney A, et al. Lipopolysa-ccharide-induced increase in signaling in hippocampus is abrogated by IL-10—a role for IL-1 beta? J Neurochem, 2004,88(3):635–646
Sharshar T, Annane D, de la Grandmaison G L et al. The neuropathology of septic shock. Brain Pathol, 2004,14(1): 21–33
Lacobone E, Bailly-Salin J, Polito A et al. Sepsisassociated encephalopathy and its differential diagnosis. Crit Care Med, 2009,37(10):S331–S336
Siami S, Annane D, Sharshar T. The encephalopathy in sepsis. Crit Care Clin, 2008,24(1):67–82
Wang J, Yang GT. Role of nuclear transcription factor-κB in endotoxin-induced shock in rats. J Huazhong Univ Sci Technol [Med Sci], 2005,25(2):174–177
Author information
Authors and Affiliations
Corresponding author
Additional information
This project was supported by a grant from the National Natural Sciences Foundation of China (No. 81071526).
Rights and permissions
About this article
Cite this article
Chen, D., Pan, H., Li, C. et al. Effects of hydrogen sulfide on a rat model of sepsis-associated encephalopathy. J. Huazhong Univ. Sci. Technol. [Med. Sci.] 31, 632–636 (2011). https://doi.org/10.1007/s11596-011-0573-2
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11596-011-0573-2