Abstract
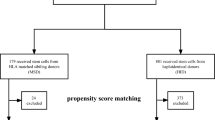
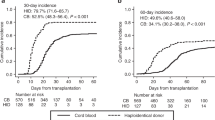
This study evaluated the influence of the degree of donor bone marrow (BM) hyperplasia on patient clinical outcomes after allogeneic hematopoietic stem cell transplantation (allo-HSCT). Twelve patients received allo-HSCT from hypoplastic BM donors between January 2010 and December 2017. Forty-eight patients whose donors demonstrated BM hyperplasia were selected using a propensity score matching method (1:4). Primary graft failure including poor graft function and graft rejection did not occur in two groups. In BM hypoplasia and hyperplasia groups, the cumulative incidence (CI) of neutrophil engraftment at day 28 (91.7% vs. 93.8%, P=0.75), platelet engraftment at day 150 (83.3% vs. 93.8%, P=0.48), the median time to myeloid engraftment (14 days vs. 14 days, P=0.85) and platelet engraftment (14 days vs. 14 days, P=0.85) were comparable. The 3-year progression-free survival, overall survival, CI of non-relapse mortality and relapse were 67.8% vs. 71.7% (P=0.98), 69.8% vs. 77.8% (P=0.69), 18.5% vs. 13.6% (P=0.66), and 10.2% vs. 10.4% (P=0.82), respectively. In multivariate analysis, donor BM hypoplasia did not affect patient clinical outcomes after allo-HSCT. If patients have no other suitable donor, a donor with BM hypoplasia can be used for patients receiving allo-HSCT if the donor Complete Blood Count and other examinations are normal.
Similar content being viewed by others
References
Apperley, J., Niederwieser, D., Huang, X., Nagler, A., Fuchs, E., Szer, J., and Kodera, Y. (2016). Reprint of: haploidentical hematopoietic stem cell transplantation: a global overview comparing Asia, the European Union, and the United States. Biol Blood Marrow Transplant 22, S15–S18.
Aversa, F., Reisner, Y., and Martelli, M.F. (2008). The haploidentical option for high-risk haematological malignancies. Blood Cell Mol Dis 40, 8–12.
Aversa, F., Terenzi, A., Tabilio, A., Falzetti, F., Carotti, A., Ballanti, S., Felicini, R., Falcinelli, F., Velardi, A., Ruggeri, L., et al. (2005). Full haplotype-mismatched hematopoietic stem-cell transplantation: a phase II study in patients with acute leukemia at high risk of relapse. J Clin Oncol 23, 3447–3454.
Baldomero, H., Gratwohl, M., Gratwohl, A., Tichelli, A., Niederwieser, D., Madrigal, A., Frauendorfer, K., and Frauendorfer, K. (2011). The EBMT activity survey 2009: trends over the past 5 years. Bone Marrow Transplant 46, 485–501.
Boo, M., van Walraven, S.M., Chapman, J., Lindberg, B., Schmidt, A.H., Shaw, B.E., Switzer, G.E., Yang, E., Egeland, T., and Egeland, T. (2011). Remuneration of hematopoietic stem cell donors: principles and perspective of the World Marrow Donor Association. Blood 117, 21–25.
Buckner, C.D., Clift, R.A., Sanders, J.E., Stewart, P., Bensinger, W.I., Doney, K.C., Sullivan, K.M., Witherspoon, R.P., Deeg, H.J., and Appelbaum, F.R. (1984). Marrow harvesting from normal donors. Blood 64, 630–634.
Chang, Y.J., and Huang, X.J. (2012). Haploidentical hematopoietic stem cell transplantation with unmanipulated granulocyte colony stimulating factor mobilized marrow and blood grafts. Curr Opin Hematol 19, 454–461.
Chang, Y.J., and Huang, X.J. (2014). Haploidentical SCT: the mechanisms underlying the crossing of HLA barriers. Bone Marrow Transplant 49, 873–879.
Ciceri, F., Labopin, M., Aversa, F., Rowe, J.M., Bunjes, D., Lewalle, P., Nagler, A., Di Bartolomeo, P., Lacerda, J.F., Lupo Stanghellini, M.T., et al. (2008). A survey of fully haploidentical hematopoietic stem cell transplantation in adults with high-risk acute leukemia: a risk factor analysis of outcomes for patients in remission at transplantation. Blood 112, 3574–3581.
Filipovich, A.H., Weisdorf, D., Pavletic, S., Socie, G., Wingard, J.R., Lee, S.J., Martin, P., Chien, J., Przepiorka, D., Couriel, D., et al. (2005). National Institutes of Health consensus development project on criteria for clinical trials in chronic graft-versus-host disease: I. Diagnosis and staging working group report. Biol Blood Marrow Transplant 11, 945–956.
Fu, Q., Xu, L., Zhang, X., Wang, Y., Chang, Y., Liu, K., and Huang, X. (2018). Platelet transfusion refractoriness after T-cell-replete haploidentical transplantation is associated with inferior clinical outcomes. Sci China Life Sci 61, 569–577.
Gratwohl, A., Baldomero, H., Aljurf, M., Pasquini, M.C., Bouzas, L.F., Yoshimi, A., Szer, J., Lipton, J., Schwendener, A., Gratwohl, M., et al. (2010). Hematopoietic stem cell transplantation: a global perspective. JAMA 303, 1617–1624.
Halter, J.P., van Walraven, S.M., Worel, N., Bengtsson, M., Hägglund, H., Nicoloso de Faveri, G., Shaw, B.E., Schmidt, A.H., Fechter, M., Madrigal, A., et al. (2013). Allogeneic hematopoietic stem cell donation—standardized assessment of donor outcome data: A consensus statement from the Worldwide Network for Blood and Marrow Transplantation (WBMT). Bone Marrow Transplant 48, 220–225.
Kiss, T.L., Chang, H., Daly, A., Messner, H.A., Jamal, N., Spaner, D., Rubin, S., and Lipton, J.H. (2004). Bone marrow aspirates as part of routine donor assessment for allogeneic blood and marrow transplantation can reveal presence of occult hematological malignancies in otherwise asymptomatic individuals. Bone Marrow Transplant 33, 855–858.
Lanza, S.T., Moore, J.E., and Butera, N.M. (2013). Drawing causal inferences using propensity scores: a practical guide for community psychologists. Am J Commun Psychol 52, 380–392.
Lown, R.N., Philippe, J., Navarro, W., van Walraven, S.M., Philips-Johnson, L., Fechter, M., Pawson, R., Bengtsson, M., Beksac, M., Field, S., et al. (2014). Unrelated adult stem cell donor medical suitability: recommendations from the World Marrow Donor Association Clinical Working Group Committee. Bone Marrow Transplant 49, 880–886.
Pasquini, M., and Wang, Z. (2010). Current use and outcome of hematopoietic stem cell transplantation: CIBMTR summary slides 2010. Available at: http://www.cibmtr.org.
Przepiorka, D., Weisdorf, D., Martin, P., Klingemann, H.G., Beatty, P., Hows, J., and Thomas, E.D. (1995). 1994 Consensus Conference on Acute GVHD Grading. Bone Marrow Transplant 15, 825–828.
Wang, Y., Chang, Y.J., Xu, L.P., Liu, K.Y., Liu, D.H., Zhang, X.H., Chen, H., Han, W., Chen, Y.H., Wang, F.R., et al. (2014). Who is the best donor for a related HLA haplotype-mismatched transplant? Blood 124, 843–850.
Wang, Y., Liu, D.H., Liu, K.Y., Xu, L.P., Zhang, X.H., Han, W., Chen, H., Chen, Y.H., Wang, F.R., Wang, J.Z., et al. (2013). Long-term follow-up of haploidentical hematopoietic stem cell transplantation without in vitro T cell depletion for the treatment of leukemia. Cancer 119, 978–985.
Wang, Y., Liu, Q.F., Xu, L.P., Liu, K.Y., Zhang, X.H., Ma, X., Fan, Z.P., Wu, D.P., and Huang, X.J. (2015). Haploidentical vs identical-sibling transplant for AML in remission: a multicenter, prospective study. Blood 125, 3956–3962.
Wang, Y., Liu, Q.F., Xu, L.P., Liu, K.Y., Zhang, X.H., Ma, X., Wu, M.Q., Wu, D.P., and Huang, X.J. (2016a). Haploidentical versus matched-sibling transplant in adults with Philadelphia-negative high-risk acute lymphoblastic leukemia: a biologically phase III randomized study. Clin Cancer Res 22, 3467–3476.
Wang, Y., Wang, H.X., Lai, Y.R., Sun, Z.M., Wu, D.P., Jiang, M., Liu, D. H., Xu, K.L., Liu, Q.F., Liu, L., et al. (2016b). Haploidentical transplant for myelodysplastic syndrome: registry-based comparison with identical sibling transplant. Leukemia 30, 2055–2063.
Xu, L., Chen, H., Chen, J., Han, M., Huang, H., Lai, Y., Liu, D., Liu, Q., Liu, T., Jiang, M., et al. (2018). The consensus on indications, conditioning regimen, and donor selection of allogeneic hematopoietic cell transplantation for hematological diseases in China—recommendations from the Chinese Society of Hematology. J Hematol Oncol 11, 33.
Xu, L.P., Wang, S.Q., Wu, D.P., Wang, J.M., Gao, S.J., Jiang, M., Wang, C. B., Zhang, X., Liu, Q.F., Xia, L.H., et al. (2016). Haplo-identical transplantation for acquired severe aplastic anaemia in a multicentre prospective study. Br J Haematol 175, 265–274.
Yu, W., Wang, Y., Wu, D., Liu, Q., Xu, L., Zhang, X., Liu, K., and Huang, X. (2019). Comparison of efficacy between HLA6/6- and HLA3/6-matched haploidentical hematopoietic stem cell transplant in T-cell-replete transplants between parents and children. Sci China Life Sci 62, 104–111.
Yu, X., Xu, L., Chang, Y., Huang, X., and Zhao, X. (2018). Rapid reconstitution of NK1 cells after allogeneic transplantation is associated with a reduced incidence of graft-versus-host disease. Sci China Life Sci 61, 902–911.
Zhang, X.H., Wang, Q.M., Zhang, J.M., Feng, F.E., Wang, F.R., Chen, H., Zhang, Y.Y., Chen, Y.H., Han, W., Xu, L.P., et al. (2015). Desialylation is associated with apoptosis and phagocytosis of platelets in patients with prolonged isolated thrombocytopenia after allo-HSCT. J Hematol Oncol 8, 116.
Acknowledgements
This work was supported by the National Natural Science Foundation of China (81670167), the Foundation for Innovative Research Groups of the National Natural Science Foundation of China (81621001) and sponsored by the Fund for Fostering Young Scholars of Peking University Health Science Center (BMU2017PY010). The authors thank all of the core facilities at the Peking University Institute of Hematology for sample collection.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Compliance and ethics The author(s) declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Tang, F., Mo, X., Zhang, X. et al. Influence of the degree of donor bone marrow hyperplasia on patient clinical outcomes after allogeneic hematopoietic stem cell transplantation. Sci. China Life Sci. 63, 138–147 (2020). https://doi.org/10.1007/s11427-018-9509-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11427-018-9509-y