Abstract
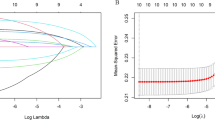
Through multiple different pathways, the environmental multiple metals make their ways to the human bodies, where they induce different levels of the oxidative stress response. This study further investigated the impact of multiple-metal exposure on the risk of developing proliferative diabetic retinopathy (PDR). We designed a case–control study with type 2 diabetic patients (T2D), in which the case group was the proliferative diabetic retinopathy group (PDR group), while the control group was the non-diabetic retinopathy group (NDR group). Graphite furnace atomic absorption spectrometry (GFAAS) and inductively coupled plasma optical emission spectrometry (ICP-OES) were used to detect the metal levels in our participants’ urine samples. The least absolute shrinkage and selection operator (LASSO) regression approach was used to include these representative trace elements in a multiple exposure model. Following that, logistic regression models and Bayesian kernel machine regression (BKMR) models were used to describe the effect of different elements and also analyze their combined effect. In the single-element model, we discovered that lithium (Li), cadmium (Cd), and strontium (Sr) were all positively related to PDR. The multiple-exposure model revealed a positive relationship between Li and PDR risk, with a maximum quartile OR of 2.80 (95% CI: 1.10–7.16). The BKMR model also revealed that selenium (Se) might act as a protective agent, whereas magnesium (Mg), Li, and Cd may raise the risk of PDR. In conclusion, our study not only revealed an association between exposure to multiple metals and PDR risk but it also implied that urine samples might be a useful tool to assess PDR risk.




Similar content being viewed by others
Data availability
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Afridi HI, Kazi TG, Brabazon D, Naher S, Talpur FN (2013) Comparative metal distribution in scalp hair of Pakistani and Irish referents and diabetes mellitus patients. Clin Chim Acta: Int J Clin Chem 415:207–214. https://doi.org/10.1016/j.cca.2012.10.029
Alhamzawi R, Ali HTM (2018) The Bayesian adaptive lasso regression. Math Biosci 303:75–82. https://doi.org/10.1016/j.mbs.2018.06.004
Aline BM, Caprara JF, de Franceschi ID, Feksa LR (2019) Effects of chronic exposure to hexavalent chromium in water on oxidative stress parameters in Wistar rats. Acta Sci: Biol Sci (1). https://doi.org/10.4025/actascibiolsci.v41i1.43771
Al-Shabrawey M, Smith S (2010) Prediction of diabetic retinopathy: role of oxidative stress and relevance of apoptotic biomarkers. EPMA J 1(1):56–72. https://doi.org/10.1007/s13167-010-0002-9
American Diabetes Association (2020) 2. Classification and diagnosis of diabetes: standards of medical care in diabetes-2020. Diabetes Care 43(Suppl 1):S14–S31. https://doi.org/10.2337/dc20-S002
Aouiss A, Anka Idrissi D, Kabine M, Zaid Y (2019) Update of inflammatory proliferative retinopathy: Ischemia, hypoxia and angiogenesis. Curr Res Transl Med 67(2):62–71. https://doi.org/10.1016/j.retram.2019.01.005
Bede-Ojimadu O, Orish CN, Bocca B, Ruggieri F, Frazzoli C, Orisakwe OE (2021) Trace elements exposure and risk in age-related eye diseases: a systematic review of epidemiological evidence. J Environ Sci Health Part C, Toxicol Carcinogenesis 39(3):293–339. https://doi.org/10.1080/26896583.2021.1916331
Bobb JF, Valeri L, Claus Henn B, Christiani DC, Wright RO, Mazumdar M, Godleski JJ, Coull BA (2015) Bayesian kernel machine regression for estimating the health effects of multi-pollutant mixtures. Biostatistics (oxford, England) 16(3):493–508. https://doi.org/10.1093/biostatistics/kxu058
Bobb JF, Claus Henn B, Valeri L, Coull BA (2018) Statistical software for analyzing the health effects of multiple concurrent exposures via Bayesian kernel machine regression. Environ Health : a Global Access Science Source 17(1):67. https://doi.org/10.1186/s12940-018-0413-y
Chakraborty R, Renu K, Eladl MA, El-Sherbiny M, Elsherbini DMA, Mirza AK, Vellingiri B, Iyer M, Dey A, Valsala Gopalakrishnan A (2022) Mechanism of chromium-induced toxicity in lungs, liver, and kidney and their ameliorative agents. Biomed Pharmacother 151:113119. https://doi.org/10.1016/j.biopha.2022.113119
Chen J, Wan Y, Su J, Zhu Z, Pan E, Shen C, Wen J, Wang K, Yu H, Qin Y, Cui L, Zhou J, Wu M (2022) Association of generalized and abdominal obesity with diabetic retinopathy in Chinese type 2 diabetic patients. Acta Diabetol 59(3):359–367. https://doi.org/10.1007/s00592-021-01806-7
de González Vega R, García M, Fernández-Sánchez ML, González-Iglesias H, Sanz-Medel A (2018) Protective effect of selenium supplementation following oxidative stress mediated by glucose on retinal pigment epithelium. Metallomics : integrated biometal science 10(1):83–92. https://doi.org/10.1039/c7mt00209b
Dubey P, Thakur V, Chattopadhyay M (2020) Role of minerals and trace elements in diabetes and insulin resistance. Nutrients 12(6):1864. https://doi.org/10.3390/nu12061864
Ebrahimi Mousavi S, Ghoreishy SM, Hemmati A, Mohammadi H (2021) Association between magnesium concentrations and prediabetes: a systematic review and meta-analysis. Sci Rep 11(1):24388. https://doi.org/10.1038/s41598-021-03915-3
Escobar J, Varela-Nallar L, Coddou C, Nelson P, Maisey K, Valdés D, Aspee A, Espinosa V, Rozas C, Montoya M, Mandiola C, Rodríguez FE, Acuña-Castillo C, Escobar A, Fernández R, Diaz H, Sandoval M, Imarai M, Rios M (2010) Oxidative damage in lymphocytes of copper smelter workers correlated to higher levels of excreted arsenic. Mediators Inflamm 2010:403830. https://doi.org/10.1155/2010/403830
Feng W, Cui X, Liu B, Liu C, Xiao Y, Lu W, Guo H, He M, Zhang X, Yuan J, Chen W, Wu T (2015) Association of urinary metal profiles with altered glucose levels and diabetes risk: a population-based study in China. PLoS One 10(4):e0123742. https://doi.org/10.1371/journal.pone.0123742
Flaxel CJ, Adelman RA, Bailey ST, Fawzi A, Lim JI, Vemulakonda GA, Ying GS (2020) Diabetic Retinopathy Preferred Practice Pattern®. Ophthalmology 127(1):P66–P145. https://doi.org/10.1016/j.ophtha.2019.09.025
Garoma D, Merga H, Hiko D (2020) Determinants of diabetic retinopathy in Southwest Ethiopia: a facility-based case-control study. BMC Public Health 20(1):503. https://doi.org/10.1186/s12889-020-08652-2
Graniel-Amador MA, Torres-Rodríguez HF, Martínez-Mendoza RE, Vargas-Muñoz VM, Acosta-González RI, Castañeda-Corral G, Muñoz-Islas E, Jiménez-Andrade JM (2022) Effect of chronic lithium on mechanical sensitivity and trabecular bone loss induced by type-1 diabetes mellitus in mice. Biometals : an International Journal on the Role of Metal Ions in Biology, Biochemistry, and Medicine 35(5):1033–1042. https://doi.org/10.1007/s10534-022-00421-5
Hermida OG, Fontela T, Ghiglione M, Uttenthal LO (1994) Effect of lithium on plasma glucose, insulin and glucagon in normal and streptozotocin-diabetic rats: role of glucagon in the hyperglycaemic response. Br J Pharmacol 111(3):861–865. https://doi.org/10.1111/j.1476-5381.1994.tb14817.x
Kar I, Patra AK (2021) Tissue bioaccumulation and toxicopathological effects of cadmium and its dietary amelioration in poultry-a review. Biol Trace Elem Res 199(10):3846–3868. https://doi.org/10.1007/s12011-020-02503-2
Khairova R, Pawar R, Salvadore G, Juruena MF, de Sousa RT, Soeiro-de-Souza MG, Salvador M, Zarate CA, Gattaz WF, Machado-Vieira R (2012) Effects of lithium on oxidative stress parameters in healthy subjects. Mol Med Rep 5(3):680–682. https://doi.org/10.3892/mmr.2011.732
Kiełczykowska M, Kocot J, Kurzepa J, Lewandowska A, Żelazowska R, Musik I (2014) Could selenium administration alleviate the disturbances of blood parameters caused by lithium administration in rats? Biol Trace Elem Res 158(3):359–364. https://doi.org/10.1007/s12011-014-9952-4
Koedrith P, Seo YR (2011) Advances in carcinogenic metal toxicity and potential molecular markers. Int J Mol Sci 12(12):9576–9595. https://doi.org/10.3390/ijms12129576
Li G, Yao T, Wu XW, Cao Z, Tu YC, Ma Y, Li BN, Peng QY, Wu B, Hou J (2020) Novel and traditional anthropometric indices for identifying arterial stiffness in overweight and obese adults. Clinical Nutrition (edinburgh, Scotland) 39(3):893–900. https://doi.org/10.1016/j.clnu.2019.03.029
Little BB, Reilly R, Walsh B, Vu GT (2020) Cadmium is associated with type 2 diabetes in a superfund site lead smelter community in Dallas, Texas. Int J Environ Res Public Health 17(12):4558. https://doi.org/10.3390/ijerph17124558
Liu Z, Shao M, Ren J, Qiu Y, Li S, Cao W (2022) Association between increased lipid profiles and risk of diabetic retinopathy in a population-based case-control study. J Inflamm Res 15:3433–3446. https://doi.org/10.2147/JIR.S361613
Madsen-Bouterse SA, Kowluru RA (2008) Oxidative stress and diabetic retinopathy: pathophysiological mechanisms and treatment perspectives. Rev Endocr Metab Disord 9(4):315–327. https://doi.org/10.1007/s11154-008-9090-4
Malhotra A, Dhawan DK (2008) Zinc improves antioxidative enzymes in red blood cells and hematology in lithium-treated rats. Nutr Res (New York, N.Y.) 28(1):43–50. https://doi.org/10.1016/j.nutres.2007.11.002
Man RE, Sabanayagam C, Chiang PP, Li LJ, Noonan JE, Wang JJ, Wong TY, Cheung GC, Tan GS, Lamoureux EL (2016) Differential association of generalized and abdominal obesity with diabetic retinopathy in Asian patients with type 2 diabetes. JAMA Ophthalmol 134(3):251–257. https://doi.org/10.1001/jamaophthalmol.2015.5103
McEligot AJ, Poynor V, Sharma R, Panangadan A (2020) Logistic LASSO regression for dietary intakes and breast cancer. Nutrients 12(9):2652. https://doi.org/10.3390/nu12092652
Miller DJ, Cascio MA, Rosca MG (2020) Diabetic retinopathy: the role of mitochondria in the neural retina and microvascular disease. Antioxidants (basel, Switzerland) 9(10):905. https://doi.org/10.3390/antiox9100905
Nguyen J, Patel A, Gensburg A, Bokhari R, Lamar P, Edwards J (2022) Diabetogenic and obesogenic effects of cadmium in Db/Db mice and rats at a clinically relevant level of exposure. Toxics 10(3):107. https://doi.org/10.3390/toxics10030107
Pamphlett R, Cherepanoff S, Too LK, Kum Jew S, Doble PA, Bishop DP (2020) The distribution of toxic metals in the human retina and optic nerve head: Implications for age-related macular degeneration. PLoS One 15(10):e0241054. https://doi.org/10.1371/journal.pone.0241054
Pedersen EB, Jørgensen ME, Pedersen MB, Siggaard C, Sørensen TB, Mulvad G, Hansen JC, Asmund G, Skjoldborg H (2005) Relationship between mercury in blood and 24-h ambulatory blood pressure in Greenlanders and Danes. Am J Hypertens 18(5 Pt 1):612–618. https://doi.org/10.1016/j.amjhyper.2004.11.022
Reddy RK, Pieramici DJ, Gune S, Ghanekar A, Lu N, Quezada-Ruiz C, Baumal CR (2018) Efficacy of ranibizumab in eyes with diabetic macular edema and macular nonperfusion in RIDE and RISE. Ophthalmology 125(10):1568–1574. https://doi.org/10.1016/j.ophtha.2018.04.002
Sales CH, Pedrosa LF, Lima JG, Lemos TM, Colli C (2011) Influence of magnesium status and magnesium intake on the blood glucose control in patients with type 2 diabetes. Clin Nutr (edinburgh, Scotland) 30(3):359–364. https://doi.org/10.1016/j.clnu.2010.12.011
Schwartz GG, Il’yasova D, Ivanova A (2003) Urinary cadmium, impaired fasting glucose, and diabetes in the NHANES III. Diabetes Care 26(2):468–470. https://doi.org/10.2337/diacare.26.2.468
Sinclair SH, Schwartz SS (2019) Diabetic retinopathy-an underdiagnosed and undertreated inflammatory, neuro-vascular complication of diabetes. Front Endocrinol 10:843. https://doi.org/10.3389/fendo.2019.00843
Tellez-Plaza M, Guallar E, Howard BV, Umans JG, Francesconi KA, Goessler W, Silbergeld EK, Devereux RB, Navas-Acien A (2013) Cadmium exposure and incident cardiovascular disease. Epidemiology (Cambridge, Mass.) 24(3):421–429. https://doi.org/10.1097/EDE.0b013e31828b0631
Valeri L, Mazumdar MM, Bobb JF, Claus Henn B, Rodrigues E, Sharif OIA, Kile ML, Quamruzzaman Q, Afroz S, Golam M, Amarasiriwardena C, Bellinger DC, Christiani DC, Coull BA, Wright RO (2017) The joint effect of prenatal exposure to metal mixtures on neurodevelopmental outcomes at 20–40 months of age: evidence from rural Bangladesh. Environ Health Perspect 125(6):067015. https://doi.org/10.1289/EHP614
Wang W, Schaumberg DA, Park SK (2016) Cadmium and lead exposure and risk of cataract surgery in U.S. adults. Int J Hygiene Environ Health 219(8):850–856. https://doi.org/10.1016/j.ijheh.2016.07.012
World report on vision. Geneva: World Health Organization (2019) Licence: CC BY-NC-SA 3.0 IGO. Available online: https://www.who.int/publications/i/item/9789241516570
Zhong Q, Wu HB, Niu QS, Jia PP, Qin QR, Wang XD, He JL, Yang WJ, Huang F (2021) Exposure to multiple metals and the risk of hypertension in adults: a prospective cohort study in a local area on the Yangtze River, China. Environ Int 153:106538. https://doi.org/10.1016/j.envint.2021.106538
Zhou Q, Guo W, Jia Y, Xu J (2019) Serum and urinary selenium status in patients with the pre-diabetes and diabetes in Northeast China. Biol Trace Elem Res 191(1):61–69. https://doi.org/10.1007/s12011-018-1604-7
Zhou TT, Hu B, Meng XL, Sun L, Li HB, Xu PR, Cheng BJ, Sheng J, Tao FB, Yang LS, Wu QS (2021) The associations between urinary metals and metal mixtures and kidney function in Chinese community-dwelling older adults with diabetes mellitus. Ecotoxicol Environ Saf 226:112829. https://doi.org/10.1016/j.ecoenv.2021.112829
Zhu X, Hua R (2020) Serum essential trace elements and toxic metals in Chinese diabetic retinopathy patients. Medicine 99(47):e23141. https://doi.org/10.1097/MD.0000000000023141
Acknowledgements
Thanks to all the subjects participated in this research. This work was supported by The Project for Top Disciplinary Talents of Majors in Universities of Anhui Province [grant numbers gxbjZD09].
Funding
This work was supported by The Project for Top Disciplinary Talents of Majors in Universities of Anhui Province [grant number gxbjZD09].
Author information
Authors and Affiliations
Contributions
Yan-Qing Li, Si-Tian Zhang, Nai-Yu Ke, Fen Huang, and Yan-Feng Zhou contributed to the study conception and design. Material preparation and data collection were performed by Yan-Qing Li, Si-Tian Zhang, Nai-Yu Ke, and Wen-Lei Hu. Yan-Feng Zhou, Fen Huang, Wen-Lei Hu, and Guo-Ao Li analyzed and interpreted the data. Yan-Qing Li, Si-Tian Zhang, and Nai-Yu Ke wrote the first draft of the manuscript and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The study had been approved by the Ethics Committee of Anhui Medical University (Approval No: 20170305), and the participants had signed written informed consent.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Responsible Editor: Lotfi Aleya
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Yan-Qing Li, Si-Tian Zhang, Nai-Yu Ke, and Yan-Cheng Fang contributed equally to this work and should be considered co-first authors.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Li, YQ., Zhang, ST., Ke, NY. et al. The impact of multiple metals exposure on the risk of developing proliferative diabetic retinopathy in Anhui, China: a case–control study. Environ Sci Pollut Res 30, 112132–112143 (2023). https://doi.org/10.1007/s11356-023-30294-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11356-023-30294-1