Abstract
Purpose
The objective was to analyze the capillary glucose (CG) responses of two resistance exercise intensities in type 2 diabetes mellitus (T2DM) individuals undergoing different drug therapies.
Methods
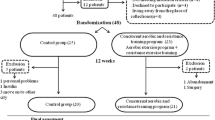
Twelve non-insulin treated (NIT), and six insulin-treated (IT) T2DM individuals (67 ± 7 years) performed two resistance-training sessions (RT-session) at moderate-intensity (MOD, 3 × 10 reps at 70% of 10-RM), high-intensity (HIGH, 3 × 10 reps at 100% of 10-RM), and a non-activity control situation (CONT). The CG was evaluated before, during, and immediately after the experimental situations.
Results
Both MOD and HIGH promoted a superior reduction of CG than CONT in NIT (−37 vs. −33 vs. −4 mg/dl, respectively, p < 0.01). Conversely, in RT-sessions, CG reduction was not statistically different when compared to CONT in IT (−51 vs. −45 vs. −20 mg/dl, respectively, p > 0.05). The higher glycemic reduction was found immediately after rather than during the RT session (p < 0.05). In both RT-sessions, pre-exercise CG levels were directly related to CG reduction (p < 0.01).
Conclusions
A single acute RT-session reduces CG, regardless of intensity, in NIT individuals. In IT individuals, the RT-session did not induce an additional effect on CG. Moreover, participants with the highest pre-exercise CG levels were the most benefited ones by RT-session in reducing glycemia.



Similar content being viewed by others
Availability of data and materials
Data are available on request from the authors.
Code availability
Not applicable.
References
DeFronzo RA, Ferrannini E, Groop L et al (2015) Type 2 diabetes mellitus. Nat Rev Dis Prim 1:15019. https://doi.org/10.1038/nrdp.2015.19
American Diabetes Association (2018) Lifestyle management: Standards of medical care in Diabetes 2018. Diabetes Care 41:S38–S50. https://doi.org/10.2337/dc18-S004
Ahlqvist E, Storm P, Käräjämäki A et al (2018) Novel subgroups of adult-onset diabetes and their association with outcomes: a data-driven cluster analysis of six variables. Lancet Diabetes Endocrinol 6:361–369. https://doi.org/10.1016/S2213-8587(18)30051-2
Gross JL, Kramer CK, Leitão CB et al (2011) Effect of antihyperglycemic agents added to metformin and a sulfonylurea on glycemic control and weight gain in type 2 diabetes: a network meta-analysis. Ann Intern Med 154:672–679. https://doi.org/10.7326/0003-4819-154-10-201105170-00007
van Dijk JW, Manders RJF, Hartgens F et al (2011) Postprandial hyperglycemia is highly prevalent throughout the day in type 2 diabetes patients. Diabetes Res Clin Pract 93:31–37. https://doi.org/10.1016/j.diabres.2011.03.021
Van Dijk JW, Manders RJF, Canfora EE et al (2013) Exercise and 24-h glycemic control: Equal effects for all type 2 diabetes patients? Med Sci Sports Exerc 45:628–635. https://doi.org/10.1249/MSS.0b013e31827ad8b4
Silveira-Rodrigues JG, Perez DV, Aleixo IMS et al (2018) Concurrent training improves the body composition of elderly type 2 diabetic patients treated with insulin. J Phys Educ Sport 18:1661–1668. https://doi.org/10.7752/jpes.2018.03243
Kramer HF, Witczak CA, Taylor EB et al (2006) AS160 regulates insulin- and contraction-stimulated glucose uptake in mouse skeletal muscle. J Biol Chem 281:31478–31485. https://doi.org/10.1074/jbc.M605461200
Boulé NG, Robert C, Bell GJ et al (2011) Metformin and exercise in type 2 diabetes: examining treatment modality interactions. Diabetes Care 34:1469–1474. https://doi.org/10.2337/dc10-2207
Gudat U, Bungert S, Kemmer F et al (1998) The blood glucose lowering effects of exercise and glibenclamide in patients with type 2 diabetes mellitus. Diabet Med 15:194–198. https://doi.org/10.1002/(SICI)1096-9136(199803)15:3%3c194::AID-DIA546%3e3.0.CO;2-2
Pesta DH, Goncalves RLS, Madiraju AK et al (2017) Resistance training to improve type 2 diabetes: working toward a prescription for the future. Nutr Metab (Lond) 14:24. https://doi.org/10.1186/s12986-017-0173-7
DeFronzo RA, Ferrannini E, Sato Y et al (1981) Synergistic interaction between exercise and insulin on peripheral glucose uptake. J Clin Invest 68:1468–1474. https://doi.org/10.1172/JCI110399
Colberg SR, Sigal RJ, Yardley JE et al (2016) Physical activity/exercise and diabetes: a position statement of the American Diabetes Association. Diabetes Care 39:2065–2079. https://doi.org/10.2337/dc16-1728
Jeng C, Ku C-T, Huang W-H (2003) Establishment of a predictive model of serum glucose changes under different exercise intensities and durations among patients with type 2 diabetes mellitus. J Nurs Res 11:287–294. https://doi.org/10.1097/01.JNR.0000347648.58122.9d
Hu Y, Zhang D, Dai L et al (2018) Pre-exercise blood glucose affects glycemic variation of aerobic exercise in patients with type 2 diabetes treated with continuous subcutaneous insulin infusion. Diabetes Res Clin Pract 141:98–105. https://doi.org/10.1016/j.diabres.2018.04.043
Savikj M, Gabriel BM, Alm PS et al (2019) Afternoon exercise is more efficacious than morning exercise at improving blood glucose levels in individuals with type 2 diabetes: a randomised crossover trial. Diabetologia 62:233–237. https://doi.org/10.1007/s00125-018-4767-z
Terada T, Friesen A, Chahal BS et al (2013) Exploring the variability in acute glycemic responses to exercise in type 2 diabetes. J Diabetes Res 2013:1–6. https://doi.org/10.1155/2013/591574
Consitt LA, Dudley C, Saxena G (2019) Impact of endurance and resistance training on skeletal muscle glucose metabolism in older adults. Nutrients 11:2636. https://doi.org/10.3390/nu11112636
Richter EA, Hargreaves M (2013) Exercise, GLUT4, and skeletal muscle glucose uptake. Physiol Rev 93:993–1017. https://doi.org/10.1152/physrev.00038.2012
Sylow L, Kleinert M, Richter EA et al (2017) Exercise-stimulated glucose uptake-regulation and implications for glycaemic control. Nat Rev Endocrinol 13:133–148. https://doi.org/10.1038/nrendo.2016.162
Chapman A, Meyer C, Renehan E et al (2017) Exercise interventions for the improvement of falls-related outcomes among older adults with diabetes mellitus: a systematic review and meta-analyses. J Diabetes Complicat 31:631–645. https://doi.org/10.1016/j.jdiacomp.2016.09.015
Liu Y, Ye W, Chen Q et al (2019) Resistance exercise intensity is correlated with attenuation of hbA1c and insulin in patients with type 2 diabetes: a systematic review and meta-analysis. Int J Environ Res Public Health 16:140. https://doi.org/10.3390/ijerph16010140
Leenders M, Verdijk LB, van der Hoeven L et al (2013) Patients with type 2 diabetes show a greater decline in muscle mass, muscle strength, and functional capacity with aging. J Am Med Dir Assoc 14:585–592. https://doi.org/10.1016/j.jamda.2013.02.006
Lee H, Song W (2018) Exercise and mitochondrial remodeling in skeletal muscle in type 2 diabetes. J Obes Metab Syndr 27:150–157. https://doi.org/10.7570/jomes.2018.27.3.150
Choi J, Akahashi H, Itai Y et al (1998) The difference between effects of power-up and bulk-type strength training exercises. Jpn J Phys Fit Sport Med 47:119–129. https://doi.org/10.7600/jspfsm1949.47.119
Egger A, Niederseer D, Diem G et al (2013) Different types of resistance training in type 2 diabetes mellitus: effects on glycaemic control, muscle mass and strength. Eur J Prev Cardiol 20:1051–1060. https://doi.org/10.1177/2047487312450132
Gonzalez AM, Hoffman JR, Townsend JR et al (2015) Intramuscular anabolic signaling and endocrine response following high volume and high intensity resistance exercise protocols in trained men. Physiol Rep 3:e12466. https://doi.org/10.14814/phy2.12466
Delevatti RS, De Souza NN, Kanitz AC et al (2016) Acute glycemic outcomes along the aerobic training in deep water in patients with type 2 diabetes. Arch Med del Deport 33:233–238
Bacchi E, Negri C, Trombetta M et al (2012) Differences in the acute effects of aerobic and resistance exercise in subjects with type 2 diabetes: Results from the RAED2 randomized trial. PLoS One 7:6–13. https://doi.org/10.1371/journal.pone.0049937
Moreira SR, Simões GC, Moraes JFVN et al (2012) Blood glucose control for individuals with type-2 diabetes: acute effects of resistance exercise of lower cardiovascular-metabolic stress. J Strength Cond Res. https://doi.org/10.1519/JSC.0b013e318242a609
Gibson BS, Colberg SR, Poirier P et al (2013) Development and validation of a predictive model of acute glucose response to exercise in individuals with type 2 diabetes. Diabetol Metab Syndr 5:33. https://doi.org/10.1186/1758-5996-5-33
Juraschek SP, Steffes MW, Selvin E (2012) Associations of alternative markers of glycemia with hemoglobin A 1c and fasting glucose. Clin Chem 58:1648–1655. https://doi.org/10.1373/clinchem.2012.188367
Nakagawa T, Tsuchida A, Itakura Y et al (2000) Brain-derived neurotrophic factor regulates glucose metabolism by modulating energy balance in diabetic mice. Diabetes 49:436–444. https://doi.org/10.2337/diabetes.49.3.436
Banerjee RR, Rangwala SM, Shapiro JS et al (2004) Regulation of fasted blood glucose by resistin. Science (80-) 303:1195–1198. https://doi.org/10.1126/science.1092341
Marliss EB, Vranic M (2002) Intense exercise has unique effects on both insulin release and its roles in glucoregulation: implications for diabetes. Diabetes 51:S271–S283. https://doi.org/10.2337/diabetes.51.2007.S271
Beck TW (2013) The importance of a priori sample size estimation in strength and conditioning research. J Strength Cond Res 27:2323–2337. https://doi.org/10.1519/JSC.0b013e318278eea0
Nathan DM, Buse JB, Davidson MB et al (2009) Medical management of hyperglycemia in type 2 diabetes: a consensus algorithm for the initiation and adjustment of therapy: a consensus statement of the American Diabetes Association and the European Association for the Study of Diabetes. Diabetes Care 32:193–203. https://doi.org/10.2337/dc08-9025
Miranda H, Figueiredo T, Rodrigues B et al (2013) Influence of exercise order on repetition performance among all possible combinations on resistance training. Res Sport Med 21:355–366. https://doi.org/10.1080/15438627.2013.825800
Koopman R, Manders RJF, Zorenc AHG et al (2005) A single session of resistance exercise enhances insulin sensitivity for at least 24 h in healthy men. Eur J Appl Physiol 94:180–187. https://doi.org/10.1007/s00421-004-1307-y
Sagkal Midilli T, Ergın E, Baysal E et al (2019) Comparison of glucose values of blood samples taken in three different ways. Clin Nurs Res 28:436–455. https://doi.org/10.1177/1054773817719379
Battelino T, Danne T, Bergenstal RM et al (2019) Clinical targets for continuous glucose monitoring data interpretation: recommendations from the international consensus on time in range. Diabetes Care 42:1593–1603. https://doi.org/10.2337/dci19-0028
Wallace TM, Levy JC, Matthews DR (2004) Use and abuse of HOMA modeling. Diabetes Care 27:1487–1495. https://doi.org/10.2337/diacare.27.6.1487
Nakagawa T, Ono-Kishino M, Sugaru E et al (2002) Brain-derived neurotrophic factor (BDNF) regulates glucose and energy metabolism in diabetic mice. Diabetes Metab Res Rev 18:185–191. https://doi.org/10.1002/dmrr.290
Gearhart RF, Lagally KM, Riechman SE et al (2009) Strength tracking ssing the OMNI resistance exercise scale in older men and women. J Strength Cond Res 23:1011–1015. https://doi.org/10.1519/JSC.0b013e3181a2ec41
Silveira APS, Bentes CM, Costa PB et al (2014) Acute effects of different intensities of resistance training on glycemic fluctuations in patients with type 1 diabetes mellitus. Res Sport Med 22:75–87. https://doi.org/10.1080/15438627.2013.852096
Gonzalez AM, Hoffman JR, Stout JR et al (2016) Intramuscular anabolic signaling and endocrine response following resistance exercise: implications for muscle hypertrophy. Sport Med 46:671–685. https://doi.org/10.1007/s40279-015-0450-4
Heinonen I, Nesterov SV, Kemppainen J et al (2012) Increasing exercise intensity reduces heterogeneity of glucose uptake in human skeletal muscles. PLoS One. https://doi.org/10.1371/journal.pone.0052191
Turner D, Luzio S, Gray BJ et al (2015) Impact of single and multiple sets of resistance exercise in type 1 diabetes. Scand J Med Sci Sports 25:e99–e109. https://doi.org/10.1111/sms.12202
Rose AJ, Richter EA (2005) Skeletal muscle glucose uptake during exercise: how is it regulated? Physiology 20:260–270. https://doi.org/10.1152/physiol.00012.2005
Marosi K, Mattson MP (2014) BDNF mediates adaptive brain and body responses to energetic challenges. Trends Endocrinol Metab 25:89–98. https://doi.org/10.1016/j.tem.2013.10.006
Geroldi D, Minoretti P, Emanuele E (2006) Brain-derived neurotrophic factor and the metabolic syndrome: more than just a hypothesis. Med Hypotheses 67:195–196. https://doi.org/10.1016/j.mehy.2006.02.001
Levinger I, Goodman C, Matthews V et al (2008) BDNF, metabolic risk factors, and resistance training in middle-aged individuals. Med Sci Sport Exerc 40:535–541. https://doi.org/10.1249/MSS.0b013e31815dd057
Acknowledgements
The authors would like to acknowledge the Laboratório do Movimento and their members by assistance with participant recruitment and data collection. The authors are also grateful to Higher Education Personnel Improvement Coordination (Coordenação de aperfeiçoamento de pessoal de nível superior, CAPES), also for Minas Gerais State Agency for Research and Development (Fundação de amparo à pesquisa de Minas Gerais FAPEMIG, no. APQ-00417-15, and no. APQ-03546-15), National Council for Scientific and Technological Development (Conselho nacional de pesquisa e desevolvimento tecnológico, CNPq, no. 425498/2016-6).
Funding
This study was financed by the Coordenação de Aperfeiçoamento de Pessoal de Nível Superior – Brasil (CAPES) – financial code 001, Minas Gerais State Agency for Research and Development (Fundação de amparo à pesquisa de Minas Gerais FAPEMIG, no. APQ-00417-15, and no. APQ-03546-15), National Council for Scientific and Technological Development (Conselho nacional de pesquisa e desevolvimento tecnológico, CNPq, no. 425498/2016-6). The funding source has not been involved in the conduct of research or preparation of the article.
Author information
Authors and Affiliations
Contributions
All authors contributed to the conceptualization and design of the study, acquisition of data, or analysis/interpretation of data. All authors contributed to revising it critically for intellectual content and, then, granted final approval of the manuscript.
Corresponding author
Ethics declarations
Conflicts of interest
Not applicable.
Ethics approval
The study was approved by the Ethics Committee of Universidade Federal de Minas Gerais/Brazil (register no. 15352613.9.0000.5149 and 66804817.8.0000.5149).
Consent to participate
The individuals who participated in the study signed the informed consent form to participate in the study.
Consent for publication
The individuals who participated in the study signed the informed consent form, which contained a consent statement for the publication of the study data.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Ogando, P.H.M., Silveira-Rodrigues, J.G., Melo, B.P. et al. Effects of high- and moderate-intensity resistance training sessions on glycemia of insulin-treated and non-insulin-treated type 2 diabetes mellitus individuals. Sport Sci Health 19, 625–636 (2023). https://doi.org/10.1007/s11332-022-00931-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11332-022-00931-2