Abstract
Purpose
Optimal cognitive performance might prevent vehicle accidents. Identifying time-related circadian and homeostatic parameters having an impact on cognitive performance of drivers may be crucial to optimize drivers’ performance.
Methods
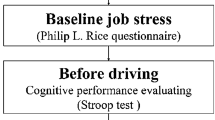
In this prospective study conducted on bus drivers, two drivers alternated driving during a 24-h round trip and were accompanied by an interviewer. Each driver was tested using Karolinska Sleepiness Scale (KSS) and the reversed digit span Wechsler Working Memory test before the start of his shift and then every 6 h during a “work/driving” day. Psychomotor Vigilance Task (PVT) was assessed before and after the journey. Linear mixed model was used to explore the factors affecting cognitive performance and sleepiness in univariate and multivariate analysis.
Results
Among 35 bus drivers, the effect of time of day on working memories was statistically significant (p = 0.001), with the lowest working memory scores at 04:00 am (± 1). The highest score of subjective sleepiness was also at 04:00 am (± 1). The time on task parameter affected sleepiness significantly (p = 0.024) and sleepiness was significantly associated with decreased working memory. Psychomotor Vigilance Task reaction time mean and the number of minor lapses were significantly increased after the journey, which suggested decreased vigilance. In multivariable analysis, a longer interval between the beginning of working hours and testing time (B (95% CI) = 15.25 (0.49 to 30), p = 0.043) was associated with higher (i.e., slower) PVT reaction time mean.
Conclusions
These results suggest that optimizing bus drivers’ working schedules may improve drivers’ sleepiness and cognitive performance and thus increase road safety.

Similar content being viewed by others
Data availability
All our data and analyses are available.
Code availability
Not applicable.
References
Bastida JL, Aguilar PS, González BD (2004) The economic costs of traffic accidents in Spain. J Trauma 56(4):883–8 (discussion 888-9)
Kapp C (2003) WHO acts on road safety to reverse accident trends. Traffic accidents kill 1.26 million people each year; 2nd leading cause of death among those aged 15-29. Lancet 3(9390):1125
Lowrie J, Brownlow H (2020) The impact of sleep deprivation and alcohol on driving: a comparative study. BMC Public Health 20(1):980
Fritz J et al (2020) A chronobiological evaluation of the acute effects of daylight saving time on traffic accident risk. Curr Biol 30(4):729-735.e2
Bioulac S et al (2017) Risk of motor vehicle accidents related to sleepiness at the wheel: a systematic review and meta-analysis. Sleep 40(10):28958002
Connor J et al (2002) Driver sleepiness and risk of serious injury to car occupants: population based case control study. BMJ 324(7346):1125
Tefft BC (2012) Prevalence of motor vehicle crashes involving drowsy drivers, United States, 1999–2008. Accid Anal Prev 45:180–186
Anund A et al (2016) Factors associated with self-reported driver sleepiness and incidents in city bus drivers. Ind Health 54(4):337–346
Filtness AJ et al (2020) Sleep loss and change detection in simulated driving. Chronobiol Int 1(11):1430–1440
Sagaspe P et al (2008) Extended driving impairs nocturnal driving performances. PLoS ONE 3(10):e3493–e3493
Balkin TJ et al (2002) The process of awakening: a PET study of regional brain activity patterns mediating the re-establishment of alertness and consciousness. Brain 125(Pt 10):2308–2319
Reteig LC et al (2019) Sustaining attention for a prolonged period of time increases temporal variability in cortical responses. Cortex 117:16–32
Greenlee ET, DeLucia PR, Newton DC (2019) Driver vigilance in automated vehicles: effects of demands on hazard detection performance. Hum Factors 61(3):474–487
Vetter C et al (2015) Aligning work and circadian time in shift workers improves sleep and reduces circadian disruption. Curr Biol 25(7):907–911
Wong LR, Flynn-Evans E, Ruskin KJ (2018) Fatigue risk management: the impact of anesthesiology residents’ work schedules on job performance and a review of potential countermeasures. Anesth Analg 126(4):1340–1348
Pettersson K et al (2019) Saccadic eye movements estimate prolonged time awake. J Sleep Res 28(2):e12755
Gupta S, Kumar P, Yuga Raju G (2021) A fuzzy causal relational mapping and rough set-based model for context-specific human error rate estimation. Int J Occup Saf Ergon 27(1):63–78
Lefebvre CD et al (2005) Assessment of working memory abilities using an event-related brain potential (ERP)-compatible digit span backward task. Clin Neurophysiol 116(7):1665–1680
Bartolacci C et al (2020) The influence of sleep quality, vigilance, and sleepiness on driving-related cognitive abilities: a comparison between young and older adults. Brain Sci 10(6):327
Huffmyer JL et al (2020) Impact of caffeine ingestion on the driving performance of anesthesiology residents after 6 consecutive overnight work shifts. Anesth Analg 130(1):66–75
Jackson ML et al (2013) Cognitive components of simulated driving performance: sleep loss effects and predictors. Accid Anal Prev 50:438–444
Durmer JS, Dinges DF (2005) Neurocognitive consequences of sleep deprivation. Semin Neurol 25(1):117–129
Bartolacci C et al (2020) The influence of sleep quality, vigilance, and sleepiness on driving-related cognitive abilities: a comparison between young and older adults. Brain Sci 10(6):327
Jongen S et al (2015) Sensitivity and validity of psychometric tests for assessing driving impairment: effects of sleep deprivation. PLoS One 10(2):e0117045
Johns MW (1991) A new method for measuring daytime sleepiness: the Epworth sleepiness scale. Sleep 14(6):540–545
Johns M, Hocking B (1997) Daytime sleepiness and sleep habits of Australian workers. Sleep 20(10):844–849
Sadeghniiat Haghighi K et al (2013) The Epworth Sleepiness Scale: translation and validation study of the Iranian version. Sleep Breath 17(1):419–426
Akerstedt T, Gillberg M (1990) Subjective and objective sleepiness in the active individual. Int J Neurosci 52(1–2):29–37
Gharagozlou F et al (2013) Investigating EEG alpha variations for mental fatigue detection on car driving simulator. Iran-J-Ergon 1(1):5–13
Netzer NC et al (1999) Using the Berlin Questionnaire to identify patients at risk for the sleep apnea syndrome. Ann Intern Med 131(7):485–491
Amra B et al (2013) Validation of the Persian version of Berlin sleep questionnaire for diagnosing obstructive sleep apnea. Int J Prev Med 4(3):334–339
Kaufman AS, Lichtenberger EO, McLean JE (2001) Two- and three-factor solutions of the WAIS-III. Assessment 8(3):267–280
Moradi AR et al (2012) Overgeneral autobiographical memory recollection in Iranian combat veterans with posttraumatic stress disorder. Behav Res Ther 50(6):435–441
Basner M, Dinges DF (2011) Maximizing sensitivity of the psychomotor vigilance test (PVT) to sleep loss. Sleep 34(5):581–591
Perez-Chada D et al (2005) Sleep habits and accident risk among truck drivers: a cross-sectional study in Argentina. Sleep 28(9):1103–1108
de Pinho RS et al (2006) Hypersomnolence and accidents in truck drivers: a cross-sectional study. Chronobiol Int 23(5):963–971
Baulk SD, Fletcher A (2012) At home and away: measuring the sleep of Australian truck drivers. Accid Anal Prev 45(Suppl):36–40
Krishnaswamy UM, Chhabria MS, Rao A (2016) Excessive sleepiness, sleep hygiene, and coping strategies among night bus drivers: a cross-sectional study. Indian J Occup Environ Med 20(2):84–87
Maia Q et al (2013) Short and long sleep duration and risk of drowsy driving and the role of subjective sleep insufficiency. Accid Anal Prev 59:618–622
Lewandowska K et al (2018) Would you say “yes” in the evening? Time-of-day effect on response bias in four types of working memory recognition tasks. Chronobiol Int 35(1):80–89
Sandberg D et al (2011) The characteristics of sleepiness during real driving at night–a study of driving performance, physiology and subjective experience. Sleep 34(10):1317–1325
Berthie G et al (2015) The restless mind while driving: drivers’ thoughts behind the wheel. Accid Anal Prev 76:159–165
Lowe CJ, Safati A, Hall PA (2017) The neurocognitive consequences of sleep restriction: a meta-analytic review. Neurosci Biobehav Rev 80:586–604
Basner M et al (2008) Effects of night work, sleep loss and time on task on simulated threat detection performance. Sleep 31(9):1251–1259
Findley LJ, Suratt PM, Dinges DF (1999) Time-on-task decrements in “steer clear” performance of patients with sleep apnea and narcolepsy. Sleep 22(6):804–809
Büttner A, Randerath W, Rühle KH (2000) The driving simulation test “carsim” for assessing vigilance. Effect of driving practice and other factors in health subjects and in patients with sleep apnea syndrome. Pneumologie 54(8):33844
Büttner A, Randerath W, Rühle KH (2003) Two simulation programs to measure continuous attention in obstructive sleep apnea syndrome. Pneumologie 57(12):722–728
Ayas N et al (2014) Obstructive sleep apnea and driving: a Canadian Thoracic Society and Canadian Sleep Society position paper. Can Respir J 21(2):114–123
Strohl KP et al (2013) An official American Thoracic Society Clinical Practice Guideline: sleep apnea, sleepiness, and driving risk in noncommercial drivers. An update of a 1994 Statement. Am J Respir Crit Care Med 187(11):125966
Zhang D et al (2021) Excessive daytime sleepiness in depression and obstructive sleep apnea: more than just an overlapping symptom. Front Psychiatry 12:710435
Bonsignore MR et al (2021) European Respiratory Society statement on sleep apnoea, sleepiness and driving risk. Eur Respir J 572:2001272
Jermann F et al. (2021) Quality of life and subjective sleep-related measures in bipolar disorder and major depressive disorder. Qual Life Res
Centofanti SA et al (2016) The impact of short night-time naps on performance, sleepiness and mood during a simulated night shift. Chronobiol Int 33(6):706–715
Naismith S et al (2004) Neurobehavioral functioning in obstructive sleep apnea: differential effects of sleep quality, hypoxemia and subjective sleepiness. J Clin Exp Neuropsychol 26(1):43–54
Lim J, Dinges DF (2008) Sleep deprivation and vigilant attention. Ann N Y Acad Sci 1129:305–322
Dixit A, Mittal T (2015) Executive functions are not affected by 24 hours of sleep deprivation: a color-word stroop task study. Indian J Psychol Med 37(2):165–168
Smolensky MH et al (2011) Sleep disorders, medical conditions, and road accident risk. Accid Anal Prev 43(2):533–548
Gonçalves M et al (2015) Sleepiness at the wheel across Europe: a survey of 19 countries. J Sleep Res 24(3):242–253
Mulhall MD et al (2019) Sleepiness and driving events in shift workers: the impact of circadian and homeostatic factors. Sleep 42(6)
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
The study has been approved by the ethics committee of the University of Social Welfare and Rehabilitation Sciences and has been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments. All participants gave their informed consent prior to their inclusion in the study.
Consent to participate
The participants gave written consent prior to their inclusion in the study.
Consent for publication
The participants gave written consent for the publication of the study prior to their inclusion in the study.
Conflict of interest
None of the authors of this paper has a financial or personal relationship with other people or organizations that could inappropriately influence or bias the content of the paper. Dr. Malhotra is funded by the NIH. He reports income related to medical education from Merck and Livanova. ResMed provided a philanthropic donation to UC San Diego.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Maghsoudipour, M., Moradi, R., Moghimi, S. et al. Time of day, time of sleep, and time on task effects on sleepiness and cognitive performance of bus drivers. Sleep Breath 26, 1759–1769 (2022). https://doi.org/10.1007/s11325-021-02526-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-021-02526-6