Abstract
Background and objective
Obstructive sleep apnea (OSA) is associated with hypertension, psychological impairment, neurocognitive dysfunction, and poor quality of sleep. Continuous positive airway pressure (CPAP) has been confirmed to effectively improve OSA, while the effects of supplemental oxygen therapy on OSA have still remained controversial. This meta-analysis aimed to compare the effects of supplemental oxygen therapy and CPAP on patients with OSA.
Methods
PubMed, Cochrane library, EMBASE, and Web of Science databases were systematically searched from inception until April 2020. Randomized controlled trials (RCTs) that compared the effects of supplemental oxygen therapy and CPAP on patients with OSA were selected without language restriction.
Results
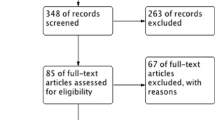
In this meta-analysis, 8 RCTs that involved 887 patients were found eligible for further analyses. Pooled data showed that there was no significant difference in improving nocturnal oxygen saturation (SpO2) level (95% confidence interval (CI) = − 1.17 to 1.53) or symptoms of depression (95%CI = − 0.69 to 1.19) between supplemental oxygen therapy and CPAP. Supplemental oxygen therapy was found less effective in reducing apnea-hypopnea index (AHI), time of SpO2 < 90%, blood pressure, and improving quality of sleep compared with CPAP. A subgroup analysis based on flow rate of oxygen indicated that the effects of supplemental oxygen therapy on blood pressure significantly differed. Furthermore, an improvement in overall time of SpO2 < 90% was correlated to duration of supplemental oxygen therapy.
Conclusions
CPAP is clinically effective for the treatment of patients with OSA. However, supplemental oxygen therapy can be cautiously used for improving nocturnal hypoxia and symptoms of depression when CPAP is not acceptable or not tolerated. Supplemental oxygen therapy is a promising option to alleviate partial disorders of OSA. Further studies need to focus on flow rate of oxygen and duration of supplemental oxygen therapy.







Similar content being viewed by others
Data availability
All data generated or analyzed in this study are included.
References
Peppard PE, Young T, Barnet JH, Palta M, Hagen EW, Hla KM (2013) Increased prevalence of sleep-disordered breathing in adults. Am J Epidemiol 177:1006–1014
Heinzer R, Vat S, Marques-Vidal P, Marti-Soler H, Andries D, Tobback N, Mooser V, Preisig M, Malhotra A, Waeber G et al (2015) Prevalence of sleep-disordered breathing in the general population: the HypnoLaus study. Lancet Respir Med 3:310–318
Dumitrascu R, Heitmann J, Seeger W, Weissmann N, Schulz R (2013) Obstructive sleep apnea, oxidative stress and cardiovascular disease: lessons from animal studies. Oxidative Med Cell Longev 2013:234631
Nadeem R, Molnar J, Madbouly EM, Nida M, Aggarwal S, Sajid H, Naseem J, Loomba R (2013) Serum inflammatory markers in obstructive sleep apnea: a meta-analysis. J Clin Sleep Med 9:1003–1012
Ryan S, McNicholas WT (2008) Intermittent hypoxia and activation of inflammatory molecular pathways in OSAS. Arch Physiol Biochem 114:261–266
Marin JM, Carrizo SJ, Vicente E, Agusti AG (2005) Long-term cardiovascular outcomes in men with obstructive sleep apnoea-hypopnoea with or without treatment with continuous positive airway pressure: an observational study. Lancet 365:1046–1053
Shahar E, Whitney CW, Redline S, Lee ET, Newman AB, Nieto FJ, O'Connor GT, Boland LL, Schwartz JE, Samet JM (2001) Sleep-disordered breathing and cardiovascular disease: cross-sectional results of the Sleep Heart Health Study. Am J Respir Crit Care Med 163:19–25
Sharafkhaneh A, Giray N, Richardson P, Young T, Hirshkowitz M (2005) Association of psychiatric disorders and sleep apnea in a large cohort. Sleep 28:1405–1411
Ohayon MM (2003) The effects of breathing-related sleep disorders on mood disturbances in the general population. J Clin Psychiatry 64:1195–1200 quiz, 1274-1196
Lam JCM, Lai AYK, Tam TCC, Yuen MMA, Lam KSL, Ip MSM (2017) CPAP therapy for patients with sleep apnea and type 2 diabetes mellitus improves control of blood pressure. Sleep Breath 21:377–386
Kendzerska T, Gershon AS, Hawker G, Tomlinson G, Leung RS (2014) Obstructive sleep apnea and incident diabetes. A historical cohort study. Am J Respir Crit Care Med 190:218–225
Wu Z, Chen F, Yu F, Wang Y, Guo Z (2018) A meta-analysis of obstructive sleep apnea in patients with cerebrovascular disease. Sleep Breath 22:729–742
Bucks RS, Olaithe M, Eastwood P (2013) Neurocognitive function in obstructive sleep apnoea: a meta-review. Respirology 18:61–70
Kerner NA, Roose SP (2016) Obstructive sleep apnea is linked to depression and cognitive impairment: evidence and potential mechanisms. Am J Geriatr Psychiatry 24:496–508
Fava C, Dorigoni S, Dalle Vedove F, Danese E, Montagnana M, Guidi GC, Narkiewicz K, Minuz P (2014) Effect of CPAP on blood pressure in patients with OSA/hypopnea a systematic review and meta-analysis. Chest 145:762–771
Neikrug AB, Liu L, Avanzino JA, Maglione JE, Natarajan L, Bradley L, Maugeri A, Corey-Bloom J, Palmer BW, Loredo JS, Ancoli-Israel S (2014) Continuous positive airway pressure improves sleep and daytime sleepiness in patients with Parkinson disease and sleep apnea. Sleep 37:177–185
Loredo JS, Ancoli-Israel S, Dimsdale JE (1999) Effect of continuous positive airway pressure vs placebo continuous positive airway pressure on sleep quality in obstructive sleep apnea. Chest 116:1545–1549
Martinez-Garcia MA, Capote F, Campos-Rodriguez F, Lloberes P, Diaz de Atauri MJ, Somoza M, Masa JF, Gonzalez M, Sacristan L, Barbe F et al (2013) Effect of CPAP on blood pressure in patients with obstructive sleep apnea and resistant hypertension: the HIPARCO randomized clinical trial. JAMA 310:2407–2415
Guo J, Sun Y, Xue LJ, Huang ZY, Wang YS, Zhang L, Zhou GH, Yuan LX (2016) Effect of CPAP therapy on cardiovascular events and mortality in patients with obstructive sleep apnea: a meta-analysis. Sleep Breath 20:965–974
Rosenberg R, Doghramji P (2009) Optimal treatment of obstructive sleep apnea and excessive sleepiness. Adv Ther 26:295–312
Stepnowsky CJ Jr, Moore PJ (2003) Nasal CPAP treatment for obstructive sleep apnea: developing a new perspective on dosing strategies and compliance. J Psychosom Res 54:599–605
Mehta V, Vasu TS, Phillips B, Chung F (2013) Obstructive sleep apnea and oxygen therapy: a systematic review of the literature and meta-analysis. J Clin Sleep Med 9:271–279
Turnbull CD, Sen D, Kohler M, Petousi N, Stradling JR (2019) Effect of supplemental oxygen on blood pressure in obstructive sleep apnea (SOX) a randomized continuous positive airway pressure withdrawal trial. Am J Respir Crit Care Med 199:211–219
Sands SA, Edwards BA, Terrill PI, Butler JP, Owens RL, Taranto-Montemurro L, Azarbarzin A, Marques M, Hess LB, Smales ET, de Melo CM, White DP, Malhotra A, Wellman A (2018) Identifying obstructive sleep apnoea patients responsive to supplemental oxygen therapy. Eur Respir J 52:1800674
Wellman A, Malhotra A, Jordan AS, Stevenson KE, Gautam S, White DP (2008) Effect of oxygen in obstructive sleep apnea: role of loop gain. Respir Physiol Neurobiol 162:144–151
Loredo JS, Ancoli-Israel S, Kim EJ, Lim WJ, Dimsdale JE (2006) Effect of continuous positive airway pressure versus supplemental oxygen on sleep quality in obstructive sleep apnea: a placebo-CPAP-controlled study. Sleep 29:564–571
Higgins JP, Altman DG, Gotzsche PC, Juni P, Moher D, Oxman AD, Savovic J, Schulz KF, Weeks L, Sterne JA et al (2011) The Cochrane collaboration's tool for assessing risk of bias in randomised trials. BMJ 343:d5928
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327:557–560
Farney RJ, Walker JM, Elmer JC, Viscomi VA, Ord RJ (1992) Transtracheal oxygen, nasal CPAP and nasal oxygen in five patients with obstructive sleep apnea. Chest 101:1228–1235
Kempf P, Mossinger B, Muller B, Kirchheiner T, Ruhle KH (1991) Comparisons between nCPAP, theophylline and O2-therapy in patients with sleep-apnea syndrome. Pneumologie 45:279–282
Arzt M, Schulz M, Wensel R, Montalvàn S, Blumberg FC, Riegger GAJ, Pfeifer M (2005) Nocturnal continuous positive airway pressure improves ventilatory efficiency during exercise in patients with chronic heart failure. Chest 127:794–802
Robison JG, Wilson C, Otteson TD, Chakravorty SS, Mehta DK (2013) Analysis of outcomes in treatment of obstructive sleep apnea in infants. Laryngoscope 123:2306–2314
Leonardis RL, Robison JG, Otteson TD (2013) Evaluating the management of obstructive sleep apnea in neonates and infants. JAMA Otolaryngol Head Neck Surg 139:139–146
Phillips BA, Schmitt FA, Berry DT, Lamb DG, Amin M, Cook YR (1990) Treatment of obstructive sleep apnea. A preliminary report comparing nasal CPAP to nasal oxygen in patients with mild OSA. Chest 98:325–330
Norman D, Loredo JS, Nelesen RA, Ancoli-Israel S, Mills PJ, Ziegler MG, Dimsdale JE (2006) Effects of continuous positive airway pressure versus supplemental oxygen on 24-hour ambulatory blood pressure. Hypertension 47:840–845
Mills PJ, Kennedy BP, Loredo JS, Dimsdale JE, Ziegler MG (2006) Effects of nasal continuous positive airway pressure and oxygen supplementation on norepinephrine kinetics and cardiovascular responses in obstructive sleep apnea. J Appl Physiol (1985) 100:343–348
Bardwell WA, Norman D, Ancoli-Israel S, Loredo JS, Lowery A, Lim W, Dimsdale JE (2007) Effects of 2-week nocturnal oxygen supplementation and continuous positive airway pressure treatment on psychological symptoms in patients with obstructive sleep apnea: a randomized placebo-controlled study. Behav Sleep Med 5:21–38
Lim W, Bardwell WA, Loredo JS, Kim EJ, Ancoli-Israel S, Morgan EE, Heaton RK, Dimsdale JE (2007) Neuropsychological effects of 2-week continuous positive airway pressure treatment and supplemental oxygen in patients with obstructive sleep apnea: a randomized placebo-controlled study. J Clin Sleep Med 3:380–386
Gottlieb DJ, Punjabi NM, Mehra R, Patel SR, Quan SF, Babineau DC, Tracy RP, Rueschman M, Blumenthal RS, Lewis EF, Bhatt DL, Redline S (2014) CPAP versus oxygen in obstructive sleep apnea. N Engl J Med 370:2276–2285
Lewis EF, Wang R, Punjabi N, Gottlieb DJ, Quan SF, Bhatt DL, Patel SR, Mehra R, Blumenthal RS, Weng J, Rueschman M, Redline S (2017) Impact of continuous positive airway pressure and oxygen on health status in patients with coronary heart disease, cardiovascular risk factors, and obstructive sleep apnea: a Heart Biomarker Evaluation in Apnea Treatment (HEARTBEAT) analysis. Am Heart J 189:59–67
Redline S, Min NI, Shahar E, Rapoport D, O'Connor G (2005) Polysomnographic predictors of blood pressure and hypertension: is one index best? Sleep 28:1122–1130
Bao G, Metreveli N, Fletcher EC (1999) Acute and chronic blood pressure response to recurrent acoustic arousal in rats. Am J Hypertens 12:504–510
Ringler J, Basner RC, Shannon R, Schwartzstein R, Manning H, Weinberger SE, Weiss JW (1990) Hypoxemia alone does not explain blood pressure elevations after obstructive apneas. J Appl Physiol (1985) 69:2143–2148
Ali NJ, Davies RJ, Fleetham JA, Stradling JR (1992) The acute effects of continuous positive airway pressure and oxygen administration on blood pressure during obstructive sleep apnea. Chest 101:1526–1532
Sundbom F, Janson C, Malinovschi A, Lindberg E (2018) Effects of coexisting asthma and obstructive sleep apnea on sleep architecture, oxygen saturation, and systemic inflammation in women. J Clin Sleep Med 14:253–259
Lee SH, Lee YJ, Kim S, Choi JW, Jeong DU (2017) Depressive symptoms are associated with poor sleep quality rather than apnea-hypopnea index or hypoxia during sleep in patients with obstructive sleep apnea. Sleep Breath 21:997–1003
Wheaton AG, Perry GS, Chapman DP, Croft JB (2012) Sleep disordered breathing and depression among U.S. adults: National Health and Nutrition Examination Survey, 2005-2008. Sleep 35:461–467
Kjelsberg FN, Ruud EA, Stavem K (2005) Predictors of symptoms of anxiety and depression in obstructive sleep apnea. Sleep Med 6:341–346
Habukawa M, Uchimura N, Kakuma T, Yamamoto K, Ogi K, Hiejima H, Tomimatsu K, Matsuyama S (2010) Effect of CPAP treatment on residual depressive symptoms in patients with major depression and coexisting sleep apnea: contribution of daytime sleepiness to residual depressive symptoms. Sleep Med 11:552–557
Edwards BA, Sands SA, Owens RL, Eckert DJ, Landry S, White DP, Malhotra A, Wellman A (2016) The combination of supplemental oxygen and a hypnotic markedly improves obstructive sleep apnea in patients with a mild to moderate upper airway collapsibility. Sleep 39:1973–1983
Funding
This work was supported by grant no. 20170541026 from the Natural Science Foundation of Liaoning Province.
Author information
Authors and Affiliations
Contributions
All the authors actively participated in the study and read and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Code availability
Not applicable.
Additional information
Comment
Although the meta analysis has demonstrated that supplemental oxygen may be considered where compliance with CPAP fails, the oxygen flow rate required may mean an individual’s tolerance of the delivery mode may be an issue in itself. Further studies are required to get a true picture of the effect of oxygen and to explain the physiology.
Margot Skinner
New Zealand
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sun, X., Luo, J. & Wang, Y. Comparing the effects of supplemental oxygen therapy and continuous positive airway pressure on patients with obstructive sleep apnea: a meta-analysis of randomized controlled trials. Sleep Breath 25, 2231–2240 (2021). https://doi.org/10.1007/s11325-020-02245-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-020-02245-4