Abstract
Background
It is still controversial if the continuous positive airway pressure (CPAP) treatment for patients with obstructive sleep apnea (OSA) can markedly influence an effect on visceral adipose tissue (VAT). The current study aimed to assess the efficacy of CPAP interventions in reducing VAT in OSA patients.
Methods
The Web of Science, PubMed, Embase, and Cochrane Library (up to December, 2019) were searched for randomized trials that assessed the effect of CPAP therapy in decreasing VAT in OSA patients. Information on the study, pre- and post-CPAP treatment of VAT, and patient characteristics were extracted for analysis. The standardized mean difference (SMD) was applied to measure the summary estimates. The analysis was conducted with STATA 13.0 and RevMan v.5.3.
Results
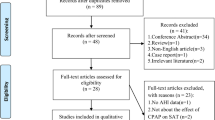
Five studies (6 cohorts) that involved 169 patients were enrolled in the meta-analysis. There was no significant change of VAT in patients with OSA before and after CPAP treatment (SMD = − 0.00, 95% CI = − 0.21 to 0.21, z = 0.01, p = 0.99). Subgroup analyses further demonstrated that the results were not influenced by CPAP therapy duration, patient age, sample size, or baseline body mass index.
Conclusions
Among the patients with OSA, our meta-analysis revealed that treatment with CPAP does not significantly lead to a reduction of VAT. High-quality randomized controlled trials may provide further clarifying information.





Similar content being viewed by others

References
Heinzer R, Vat S, Marques-Vidal P, Marti-Soler H, Andries D, Tobback N, Mooser V, Preisig M, Malhotra A, Waeber G, Vollenweider P, Tafti M, Haba-Rubio J (2015) Prevalence of sleep-disordered breathing in the general population: the HypnoLaus study. Lancet Respir Med 3:310–318. https://doi.org/10.1016/S2213-2600(15)00043-0
Peppard PE, Young T, Barnet JH, Palta M, Hagen EW, Hla KM (2013) Increased prevalence of sleep-disordered breathing in adults. Am J Epidemiol 177:1006–1014. https://doi.org/10.1093/aje/kws342
Dewan NA, Nieto FJ, Somers VK (2015) Intermittent hypoxemia and OSA: implications for comorbidities. Chest 147:266–274. https://doi.org/10.1378/chest.14-0500
Somers VK, White DP, Amin R, Abraham WT, Costa F, Culebras A, Daniels S, Floras JS, Hunt CE, Olson LJ, Pickering TG, Russell R, Woo M, Young T (2008) Sleep apnea and cardiovascular disease: an American Heart Association/american College Of Cardiology Foundation Scientific Statement from the American Heart Association Council for High Blood Pressure Research Professional Education Committee, Council on Clinical Cardiology, Stroke Council, and Council On Cardiovascular Nursing. In collaboration with the National Heart, Lung, and Blood Institute National Center on Sleep Disorders Research (National Institutes of Health). Circulation 118:1080–1111. https://doi.org/10.1161/CIRCULATIONAHA.107.189375
Grunstein R, Wilcox I, Yang TS, Gould Y, Hedner J (1993) Snoring and sleep apnoea in men: association with central obesity and hypertension. Int J Obes Relat Metab Disord 17:533–540
Van Gaal LF, Mertens IL, De Block CE (2006) Mechanisms linking obesity with cardiovascular disease. Nature 444:875–880. https://doi.org/10.1038/nature05487
Neeland IJ, Turer AT, Ayers CR, Berry JD, Rohatgi A, Das SR, Khera A, Vega GL, McGuire DK, Grundy SM, de Lemos JA (2015) Body fat distribution and incident cardiovascular disease in obese adults. J Am Coll Cardiol 65:2150–2151. https://doi.org/10.1016/j.jacc.2015.01.061
Neeland IJ, Turer AT, Ayers CR, Powell-Wiley TM, Vega GL, Farzaneh-Far R, Grundy SM, Khera A, McGuire DK, de Lemos JA (2012) Dysfunctional adiposity and the risk of prediabetes and type 2 diabetes in obese adults. JAMA 308:1150–1159. https://doi.org/10.1001/2012.jama.11132
Britton KA, Massaro JM, Murabito JM, Kreger BE, Hoffmann U, Fox CS (2013) Body fat distribution, incident cardiovascular disease, cancer, and all-cause mortality. J Am Coll Cardiol 62:921–925. https://doi.org/10.1016/j.jacc.2013.06.027
Ogretmenoglu O, Suslu AE, Yucel OT, Onerci TM, Sahin A (2005) Body fat composition: a predictive factor for obstructive sleep apnea. Laryngoscope 115:1493–1498. https://doi.org/10.1097/01.mlg.0000172204.82314.c3
Qaseem A, Holty JE, Owens DK, Dallas P, Starkey M, Shekelle P (2013) Management of obstructive sleep apnea in adults: a clinical practice guideline from the American College of Physicians. Ann Intern Med 159:471–483. https://doi.org/10.7326/0003-4819-159-7-201310010-00704
Zhang J, Weaver TE, Zhong Z, Nisi RA, Martin KR, Steffen AD, Karaman MM, Zhou XJ (2019) White matter structural differences in OSA patients experiencing residual daytime sleepiness with high CPAP use: a non-Gaussian diffusion MRI study. Sleep Med 53:51–59. https://doi.org/10.1016/j.sleep.2018.09.011
Dursunoglu N, Dursunoglu D, Ozkurt S, Kuru O, Gur S, Kiter G, Evyapan F (2007) Effects of CPAP on left ventricular structure and myocardial performance index in male patients with obstructive sleep apnoea. Sleep Med 8:51–59. https://doi.org/10.1016/j.sleep.2006.04.007
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 6:e1000097. https://doi.org/10.1371/journal.pmed.1000097
Juni P, Altman DG, Egger M (2001) Systematic reviews in health care: assessing the quality of controlled clinical trials. BMJ 323:42–46. https://doi.org/10.1136/bmj.323.7303.42
Higgins JPT, Green S (ed) (2011) Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0 [updated March 2011]. The Cochrane Collaboration. Available from http://handbook.cochrane.org.
Ng SS, Liu EK, Ma RC, Chan TO, To KW, Chan KK, Ngai J, Yip WH, Ko FW, Wong CK, Hui DS (2017) Effects of CPAP therapy on visceral fat thickness, carotid intima-media thickness and adipokines in patients with obstructive sleep apnoea. Respirology 22:786–792. https://doi.org/10.1111/resp.12963
Kritikou I, Basta M, Tappouni R, Pejovic S, Fernandez-Mendoza J, Nazir R, Shaffer ML, Liao D, Bixler EO, Chrousos GP, Vgontzas AN (2013) Sleep apnoea and visceral adiposity in middle-aged male and female subjects. Eur Respir J 41:601–609. https://doi.org/10.1183/09031936.00183411
Hoyos CM, Killick R, Yee BJ, Phillips CL, Grunstein RR, Liu PY (2012) Cardiometabolic changes after continuous positive airway pressure for obstructive sleep apnoea: a randomised sham-controlled study. Thorax 67:1081–1089. https://doi.org/10.1136/thoraxjnl-2011-201420
Sivam S, Phillips CL, Trenell MI, Yee BJ, Liu PY, Wong KK, Grunstein RR (2012) Effects of 8 weeks of continuous positive airway pressure on abdominal adiposity in obstructive sleep apnoea. Eur Respir J 40:913–918. https://doi.org/10.1183/09031936.00177011
Lam JC, Lam B, Yao TJ, Lai AY, Ooi CG, Tam S, Lam KS, Ip MS (2010) A randomised controlled trial of nasal continuous positive airway pressure on insulin sensitivity in obstructive sleep apnoea. Eur Respir J 35:138–145. https://doi.org/10.1183/09031936.00047709
Ross R, Bradshaw AJ (2009) The future of obesity reduction: beyond weight loss. Nat Rev Endocrinol 5:319–325. https://doi.org/10.1038/nrendo.2009.78
Tchernof A, Despres JP (2013) Pathophysiology of human visceral obesity: an update. Physiol Rev 93:359–404. https://doi.org/10.1152/physrev.00033.2011
Flegal KM, Kit BK, Orpana H, Graubard BI (2013) Association of all-cause mortality with overweight and obesity using standard body mass index categories: a systematic review and meta-analysis. JAMA 309:71–82. https://doi.org/10.1001/jama.2012.113905
Vgontzas AN, Bixler EO, Chrousos GP (2005) Sleep apnea is a manifestation of the metabolic syndrome. Sleep Med Rev 9:211–224. https://doi.org/10.1016/j.smrv.2005.01.006
Zhao X, Xu H, Qian Y, Liu Y, Zou J, Yi H, Guan J, Yin S (2019) Abdominal obesity is more strongly correlated with obstructive sleep apnea than general obesity in China: results from two separated observational and longitudinal studies. Obes Surg. https://doi.org/10.1007/s11695-019-03870-z
Vgontzas AN, Bixler EO, Chrousos GP (2003) Metabolic disturbances in obesity versus sleep apnoea: the importance of visceral obesity and insulin resistance. J Intern Med 254:32–44
Owens RL, Malhotra A, Eckert DJ, White DP (1985) Jordan AS (2010) The influence of end-expiratory lung volume on measurements of pharyngeal collapsibility. J Appl Physiol 108:445–451. https://doi.org/10.1152/japplphysiol.00755.2009
Munzer T, Hegglin A, Stannek T, Schoch OD, Korte W, Buche D, Schmid C, Hurny C (2010) Effects of long-term continuous positive airway pressure on body composition and IGF1. Eur J Endocrinol 162:695–704. https://doi.org/10.1530/EJE-09-0919
Vgontzas AN, Zoumakis E, Bixler EO, Lin HM, Collins B, Basta M, Pejovic S, Chrousos GP (2008) Selective effects of CPAP on sleep apnoea-associated manifestations. Eur J Clin Investig 38:585–595. https://doi.org/10.1111/j.1365-2362.2008.01984.x
Hunter GR, Gower BA, Kane BL (2010) Age related shift in visceral fat. Int J Body Compos Res 8:103–108
Kotani K, Tokunaga K, Fujioka S, Kobatake T, Keno Y, Yoshida S, Shimomura I, Tarui S, Matsuzawa Y (1994) Sexual dimorphism of age-related changes in whole-body fat distribution in the obese. Int J Obes Relat Metab Disord 18:202–207
Shuster A, Patlas M, Pinthus JH, Mourtzakis M (2012) The clinical importance of visceral adiposity: a critical review of methods for visceral adipose tissue analysis. Br J Radiol 85:1–10. https://doi.org/10.1259/bjr/38447238
Funding
This work was supported by the Chinese National Natural Science Foundation (grant number 81870074), Science and Technology Projects of Quanzhou (grant number 2019N099S), and Startup Fund for Scientific Research, Fujian Medical University (grant number 2017XQ1102).
Author information
Authors and Affiliations
Contributions
All authors directly participated in the study and have reviewed and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
Additional informed consent was obtained from all individual participants for whom identifying information is included in this article.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chen, Q., Lin, G., Chen, Y. et al. Impact of CPAP treatment for obstructive sleep apnea on visceral adipose tissue: a meta-analysis of randomized controlled trials. Sleep Breath 25, 555–562 (2021). https://doi.org/10.1007/s11325-020-02181-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-020-02181-3