Abstract
Purpose
Selective upper-airway stimulation (UAS) is a novel therapy for patients with obstructive sleep apnea (OSA). The aim of this study was to compare changes in sleep architecture during the diagnostic polysomnography and the post-implantation polysomnography in UAS in patients with OSA.
Methods
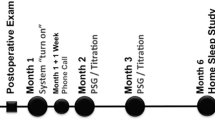
Twenty-six patients who received a UAS device (Inspire Medical Systems) were included. Treatment outcome was evaluated 2 and 3 months after surgery. Data collection included demographics, body mass index (BMI), apnea hypopnea index (AHI), oxygen saturation and desaturation index (ODI), Epworth sleepiness score (ESS), arousal parameter, and sleep patterns.
Results
The mean age was 60.2 years, 25 patients were male, 1 patient was female. Mean BMI was 29.0 kg/m2. The mean pre-implantation AHI of 33.9/h could be reduced to 9.1/h at 2 months post-implantation (p < 0.001). The amount of time spent in N1-sleep could be reduced from 23.2% at baseline to 16.0% at month 3 post-implantation. The amount of time spent in N2- and N3-sleep did not change during the observation period. A significant increase of the amount of REM sleep at month 2 (15.7%) compared to baseline (9.5%; p = 0.010) could be observed. A reduction of the number of arousals and the arousal index could be observed.
Conclusion
In conclusion, significant changes in sleep architecture of patients with OSA and sufficient treatment with UAS could be observed. A reduction of the amount of time spent in N1-sleep could be caused by treatment with UAS and the rebound of REM sleep, observed for the first time in a study on UAS, is also a potential marker of the efficacy of UAS on sleep architecture.
Trial registration
NCT02293746.


Similar content being viewed by others
References
Pengo MF, Steier J (2015) Emerging technology: electrical stimulation in obstructive sleep apnoea. J Thorac Dis 7:1286–1297
Young T, Palta M, Dempsey J, Skatrud J, Weber S, Badr S (1993) The occurrence of sleep-disordered breathing among middle-aged adults. N Engl J Med 328:1230–1235
Peppard PE, Young T, Barnet JH, Palta M, Hagen EW, Hla KM (2013) Increased prevalence of sleep-disordered breathing in adults. Am J Epidemiol 177:1006–1014
Steier J, Martin A, Harris J, Jarrold I, Pugh D, Williams A (2014) Predicted relative prevalence estimates for obstructive sleep apnoea and the associated healthcare provision across the UK. Thorax 69:390–392
Strollo PJ, Rogers RM (1996) Obstructive sleep apnea. N Engl J Med 334:99–104
Philip P, Stoohs R, Guilleminault C (1994) Sleep fragmentation in normals: a model for sleepiness associated with upper airway resistance syndrome. Sleep 17:242–247
Strollo PJ, Soose RJ, Maurer JT, de Vries N, Cornelius J et al (2014) Upper-airway stimulation for obstructive sleep apnea. N Engl J Med 370:139–149
McArdle N, Douglas NJ (2001) Effect of continuous positive airway pressure on sleep architecture in the sleep apnea-hypopnea syndrome: a randomized controlled trial. Am J Respir Crit Care Med 164:1459–1463
Narkiewicz K, Somers VK (1999) Obstructive sleep apnea as a cause of neurogenic hypertension. Curr Hypertens Rep 1:268–273
Martinez D, Klein C, Rahmeier L, da Silva RP, Fiori CZ et al (2012) Sleep apnea is a stronger predictor for coronary heart disease than traditional risk factors. Sleep Breath 16:695–701
Palomäki H, Partinen M, Juvela S, Kaste M (1989) Snoring as a risk factor for sleep-related brain infarction. Stroke 20:1311–1315
Bradley TD, Rutherford R, Grossman RF, Lue F, Zamel N et al (1985) Role of daytime hypoxemia in the pathogenesis of right heart failure in the obstructive sleep apnea syndrome. Am Rev Respir Dis 131:835–839
Lévy P, Bonsignore MR, Eckel J (2009) Sleep, sleep-disordered breathing and metabolic consequences. Eur Respir J 34:243–260
Punjabi NM, Sorkin JD, Katzel LI, Goldberg AP, Schwartz AR, Smith PL (2002) Sleep-disordered breathing and insulin resistance in middle-aged and overweight men. Am J Respir Crit Care Med 165:677–682
Gottlieb DJ, Yenokyan G, Newman AB, O’Connor GT, Punjabi NM et al (2010) Prospective study of obstructive sleep apnea and incident coronary heart disease and heart failure: the sleep heart health study. Circulation 122:352–360
Giles TL, Lasserson TJ, Smith BH, White J, Wright J, Cates CJ (2006) Continuous positive airways pressure for obstructive sleep apnoea in adults. Cochrane Database Syst Rev CD001106
Somiah M, Taxin Z, Keating J, Mooney AM, Norman RG et al (2012) Sleep quality, short-term and long-term CPAP adherence. J Clin Sleep Med 8:489–500
Sawyer AM, Gooneratne NS, Marcus CL, Ofer D, Richards KC, Weaver TE (2011) A systematic review of CPAP adherence across age groups: clinical and empiric insights for developing CPAP adherence interventions. Sleep Med Rev 15:343–356
Lévy P, Kohler M, McNicholas WT, Barbé F, McEvoy RD et al (2015) Obstructive sleep apnoea syndrome. Nat Rev Dis Prim 1:15015
Kent DT, Lee JJ, Strollo PJ, Soose RJ (2016) Upper airway stimulation for OSA: early adherence and outcome results of one center. Otolaryngol Head Neck Surg
Soose RJ, Woodson BT, Gillespie MB, Maurer JT, de Vries N et al (2016) Upper airway stimulation for obstructive sleep apnea: self-reported outcomes at 24 months. J Clin Sleep Med 12:43–48
Strollo PJ, Gillespie MB, Soose RJ, Maurer JT, de Vries N et al (2015) Upper airway stimulation for obstructive sleep apnea: durability of the treatment effect at 18 months. Sleep 38:1593–1598
Heiser C, Knopf A, Bas M, Gahleitner C, Hofauer B (2016) Selective upper-airway stimulation for obstructive sleep apnea—a single center clinical experience. Eur Arch Otorhinolaryngol
Kezirian EJ, Hohenhorst W, de Vries N (2011) Drug-induced sleep endoscopy: the VOTE classification. Eur Arch Otorhinolaryngol 268:1233–1236
Johns MW (1991) A new method for measuring daytime sleepiness: the Epworth sleepiness scale. Sleep 14:540–545
Heiser C, Thaler E, Boon M, Soose RJ, Woodson BT (2016) Updates of operative techniques for upper airway stimulation. Laryngoscope
Heiser C, Hofauer B, Lozier L, Woodson BT, Stark T (2016) Nerve monitoring guided selective hypoglossal nerve stimulation in obstructive sleep apnea. Laryngoscope
Berry RB, Budhiraja R, Gottlieb DJ, Gozal D, Iber C et al (2012) Rules for scoring respiratory events in sleep: update of the 2007 AASM Manual for the Scoring of Sleep and Associated Events. Deliberations of the Sleep Apnea Definitions Task Force of the American Academy of Sleep Medicine. J Clin Sleep Med 8:597–619
Sher AE, Schechtman KB, Piccirillo JF (1996) The efficacy of surgical modifications of the upper airway in adults with obstructive sleep apnea syndrome. Sleep 19:156–177
Woodson BT, Soose RJ, Gillespie MB, Strohl KP, Maurer JT et al (2016) Three-year outcomes of cranial nerve stimulation for obstructive sleep apnea: the STAR trial. Otolaryngol Head Neck Surg 154:181–188
Woodson BT, Gillespie MB, Soose RJ, Maurer JT, de Vries N et al (2014) Randomized controlled withdrawal study of upper airway stimulation on OSA: short- and long-term effect. Otolaryngol Head Neck Surg 151:880–887
Van de Heyning PH, Badr MS, Baskin JZ, Cramer Bornemann MA, De Backer WA et al (2012) Implanted upper airway stimulation device for obstructive sleep apnea. Laryngoscope 122:1626–1633
Verma A, Radtke RA, Van Landingham KE, King JH, Husain AM (2001) Slow wave sleep rebound and REM rebound following the first night of treatment with CPAP for sleep apnea: correlation with subjective improvement in sleep quality. Sleep Med 2:215–223
Redline S, Kirchner HL, Quan SF, Gottlieb DJ, Kapur V, Newman A (2004) The effects of age, sex, ethnicity, and sleep-disordered breathing on sleep architecture. Arch Intern Med 164:406–418
Sagaspe P, Taillard J, Chaumet G, Moore N, Bioulac B, Philip P (2007) Aging and nocturnal driving: better with coffee or a nap? A randomized study. Sleep 30:1808–1813
Koo BB, Wiggins R, Molina C (2012) REM rebound and CPAP compliance. Sleep Med 13:864–868
Aldrich M, Eiser A, Lee M, Shipley JE (1989) Effects of continuous positive airway pressure on phasic events of REM sleep in patients with obstructive sleep apnea. Sleep 12:413–419
Grimaldi D, Beccuti G, Touma C, Van Cauter E, Mokhlesi B (2014) Association of obstructive sleep apnea in rapid eye movement sleep with reduced glycemic control in type 2 diabetes: therapeutic implications. Diabetes Care 37:355–363
Mokhlesi B, Finn LA, Hagen EW, Young T, Hla KM et al (2014) Obstructive sleep apnea during REM sleep and hypertension. Results of the Wisconsin sleep cohort. Am J Respir Crit Care Med 190:1158–1167
Fietze I, Quispe-Bravo S, Hänsch T, Röttig J, Baumann G, Witt C (1997) Arousals and sleep stages in patients with obstructive sleep apnoea syndrome: changes under nCPAP treatment. J Sleep res 6:128–133
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No funding was received for this research.
Conflict of interest
Benedikt Hofauer, Markus Wirth, and Clemens Heiser received research support from Inspire Medical Systems. The article submitted is related to this relationship. Pierre Philip has a relationship with UCB, Sanofi, Takeda, Bastide, and Vital-Aire as a consultant. The article submitted is not related to this relationship. Andreas Knopf received research support from Optima Pharmazeutische GmbH. The article submitted is not related to this relationship. The trial was registered as NCT02293746 (Inspire Upper Airway Stimulation System German Post-Market Study) on clinicaltrial.gov as a sub-investigation of the German Post-Market Study.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Hofauer, B., Philip, P., Wirth, M. et al. Effects of upper-airway stimulation on sleep architecture in patients with obstructive sleep apnea. Sleep Breath 21, 901–908 (2017). https://doi.org/10.1007/s11325-017-1519-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-017-1519-0