Abstract
Purposes
The purposes of this study are to investigate the usefulness of polygraphy (PG) in diagnosing obstructive sleep apnea (OSA) in sleepy/tired snorers compared to polysomnography (PSG) and, further, to search for suspected respiratory arousals in the PG.
Methods
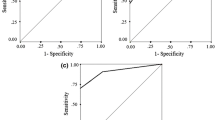
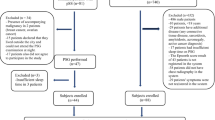
One hundred eighty-seven adults suffering from sleepiness/tiredness and snoring had undergone ambulant PG and were considered to be normal, using American Academy of Sleep Medicine’s 2007 hypopnea criteria A. After approximately 7 months, in-lab PSG was performed using hypopnea criteria B, where arousals are also recognized. Validated questionnaires (Hospital Anxiety and Depression Scale, self-rated general health) were answered. In a subgroup, the sensitivity and specificity were calculated for flow limitation index (FLI) and flattening index (FlatI) in PG compared with the respiratory distress index (RDI) in PSG.
Results
Despite the normal PG, at PSG, the median RDI was 11.0 (range, 0–89.1). One hundred sixty-eight out of one hundred seventy-eight (90 %) were found to have at least mild OSA and 119/187 (64 %) with moderate–severe OSA according to the RDI values. The sensitivity and specificity were low (<70 %) for FLI and FlatI. Forty-nine percent of the patients rated anxiety at borderline or pathological levels, 35 % rated corresponding depression levels, and 45 % rated poor or fair general health.
Conclusions
PG was insufficient to rule out OSA when the respiratory events were mainly associated with arousals. Almost half of these patients experience low general health and psychiatric problems. We recommend a full-night PSG when PG is “normal”, and patients have symptoms of snoring and sleepiness/tiredness.


Similar content being viewed by others
References
Thurnheer R, Bloch KE, Laube I, Gugger M, Heitz M (2007) Respiratory polygraphy in sleep apnoea diagnosis—report of the Swiss respiratory polygraphy registry and systematic review of the literature. Swiss Med Wkly 137:97–102
Guilleminault C, Kirisoglu C, Poyares D, Palombini L, Leger D, Farid-Moayer M, Ohayon MM (2006) Upper airway resistance syndrome: a long-term outcome study. J Psychiatr Res 40:273–279
Jonczak L, Plywaczewski R, Sliwinski P, Bednarek M, Gorecka D, Zielinski J (2009) Evolution of upper airway resistance syndrome. J Sleep Res 18:337–341
Friberg D, Ansved T, Borg K, Carlsson-Nordlander B, Larsson H, Svanborg E (1998) Histological indications of a progressive snorers disease in an upper airway muscle. Am J Respir Crit Care Med 157:586–593
Iber C, Ancoli-Israel S, Chesson A, Quan S (2007) The AASM manual for the scoring of sleep and associated events : rules, terminology and technical specifications. American Academy of Sleep Medicine, Westchester, IL
Berry RB, Budhiraja R, Gottlieb DJ, Gozal D, Iber C, Kapur VK, Marcus CL, Mehra R, Parthasarathy S, Quan SF, Redline S, Strohl KP, Davidson Ward SL, Tangredi MM (2012) Rules for scoring respiratory events in sleep: update of the 2007 AASM Manual for the Scoring of Sleep and Associated Events: deliberations of the sleep apnea definitions task force of the American Academy of Sleep Medicine. J Clin Sleep Med 15:597–619
Johns MW (1991) A new method for measuring daytime sleepiness: the Epworth sleepiness scale. Sleep 14:540–545
Zigmond AS, Sims AC (1983) The effect of the use of the International Classification of Diseases 9th revision: upon hospital in-patient diagnoses. Br J Psychiatry 142:409–413
Idler EL, Russell LB, Davis D (2000) Survival, functional limitations, and self-rated health in the NHANES I Epidemiologic Follow-up Study, 1992. First National Health and Nutrition Examination Survey. Am J Epidemiol 152:874–883
Condos R, Norman RG, Krishnasamy I, Peduzzi N, Goldring RM, Rapoport DM (1994) Flow limitation as a noninvasive assessment of residual upper-airway resistance during continuous positive airway pressure therapy of obstructive sleep apnea. Am J Respir Crit Care Med 150:475–480
Teschler H, Berthon-Jones M, Thompson AB, Henkel A, Henry J, Konietzko N (1996) Automated continuous positive airway pressure titration for obstructive sleep apnea syndrome. Am J Respir Crit Care Med 154:734–740
Ruehland WR, Rochford PD, O’Donoghue FJ, Pierce RJ, Singh P, Thornton AT (2009) The new AASM criteria for scoring hypopneas: impact on the apnea hypopnea index. Sleep 32:150–157
Parrino L, Ferri R, Zucconi M, Fanfulla F (2009) Commentary from the Italian Association of Sleep Medicine on the AASM manual for the scoring of sleep and associated events: for debate and discussion. Sleep Med 10:799–808
Ravesloot MJ, van Maanen JP, Dun L, de Vries N (2013) The undervalued potential of positional therapy in position-dependent snoring and obstructive sleep apnea—a review of the literature. Sleep Breath 17:39–49
Guilleminault C, Black JE, Palombini L, Ohayon M (2000) A clinical investigation of obstructive sleep apnea syndrome (OSAS) and upper airway resistance syndrome (UARS) patients. Sleep Med 1:51–56
Stoohs RA, Knaack L, Blum HC, Janicki J, Hohenhorst W (2008) Differences in clinical features of upper airway resistance syndrome, primary snoring, and obstructive sleep apnea/hypopnea syndrome. Sleep Med 9:121–128
Young T, Peppard PE, Gottlieb DJ (2002) Epidemiology of obstructive sleep apnea: a population health perspective. Am J Respir Crit Care Med 165:1217–1239
Gabbay IE, Lavie P (2012) Age- and gender-related characteristics of obstructive sleep apnea. Sleep Breath 16:453–460
Young T, Palta M, Dempsey J, Skatrud J, Weber S, Badr S (1993) The occurrence of sleep-disordered breathing among middle-aged adults. N Engl J Med 328:1230–1235
Marshall NS, Wong KK, Liu PY, Cullen SR, Knuiman MW, Grunstein RR (2008) Sleep apnea as an independent risk factor for all-cause mortality: the Busselton Health Study. Sleep 31:1079–1085
Young T, Finn L, Peppard PE, Szklo-Coxe M, Austin D, Nieto FJ, Stubbs R, Hla KM (2008) Sleep disordered breathing and mortality: eighteen-year follow-up of the Wisconsin sleep cohort. Sleep 31:1071–1078
Chandra S, Sica AL, Wang J, Lakticova V, Greenberg HE (2013) Respiratory effort-related arousals contribute to sympathetic modulation of heart rate variability. Sleep Breath. doi:10.1007/s11325-013-0823-6
Mosko SS, Dickel MJ, Ashurst J (1988) Night-to-night variability in sleep apnea and sleep-related periodic leg movements in the elderly. Sleep 11:340–348
Chediak AD, Acevedo-Crespo JC, Seiden DJ, Kim HH, Kiel MH (1996) Nightly variability in the indices of sleep-disordered breathing in men being evaluated for impotence with consecutive night polysomnograms. Sleep 19:589–592
Acknowledgments
We thank Ewa Hansson, secretary at the ENT clinic, for assistance with the registers and Paul Murphy, Leah Steinberg, and Carin Sahlin-Ingridsson, RPSGT, for assistance with the polysomnography scoring.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Nerfeldt, P., Aoki, F. & Friberg, D. Polygraphy vs. polysomnography: missing osas in symptomatic snorers—a reminder for clinicians. Sleep Breath 18, 297–303 (2014). https://doi.org/10.1007/s11325-013-0884-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-013-0884-6