Abstract
Aim
Obstructive sleep apnea syndrome (OSAS) is characterized by recurrent respiratory disorders in the upper airways during sleep. Although continuous positive airway pressure (CPAP) has been accepted to be the most effective treatment for OSAS, its role on inflammation remains debatable. In this study, our aim was to examine the influence of 3 months of CPAP treatment on tumor necrosis factor-alpha (TNF-α), interleukin-6 (IL-6), 8-isoprostane, and peroxynitrite levels in exhaled breathing condensates (EBC) and serum.
Methods
Thirty-five patients who were newly diagnosed as moderate or severe OSAS with full night polysomnography and used CPAP therapy regularly for 3 months were included in the study. Polysomnography, spirometric tests, fasting blood samples, and EBC were ascertained on entry into the study and after 3 months of treatment. All patients were assessed monthly for treatment adherence and side effects.
Results
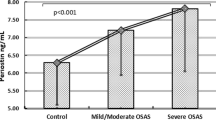
We found that all polysomnographic parameters were normalized after CPAP therapy in the control polysomnogram. Also, all markers in EBC and nitrotyrosine and 8-isoprostane levels in serum were decreased significantly with CPAP treatment. Sedimentation rate, C-reactive protein, IL-6, and TNF-α remained unchanged in serum after treatment. We found that baseline nitrotyrosine levels were significantly correlated with apnea–hypopnea index, oxygen desaturation index, and percent time in SpO2 < 90 % (p < 0.01).
Conclusions
CPAP therapy has primarily a relevant impact on airways, and nitrotyrosine levels correlated well with severity of OSAS. This treatment decreases both inflammation and oxidative stress levels in airways in OSAS patients. Also, this treatment helps to decrease systemic oxidative stress levels in serum.

Similar content being viewed by others
References
Young T, Palta M, Dempsey J, Skatrud J, Weber S, Badr S (1993) The occurrence of sleep-disordered breathing among middle-aged adults. N Engl J Med 328:1230–1235
Kohler M, Stradling JR (2010) Mechanisms of vascular damage in obstructive sleep apnea. Nat Rev Cardiol 7:677–685
Ryan S, Taylor CT, McNicholas WT (2009) Systemic inflammation: a key factor in the pathogenesis of cardiovascular complications in obstructive sleep apnoea syndrome? Postgrad Med J 85:693–698
Quercioli A, Mach F, Montecucco F (2010) Inflammation accelerates atherosclerotic processes in obstructive sleep apnea syndrome (OSAS). Sleep Breath 14:261–269
Takama N, Kurabayasi M (2009) Influence of untreated sleep-disordered breathing on the long-term prognosis of patients with cardiovascular disease. Am J Cardiol 103:730–734
Foresi A, Leone C, Olivieri D, Cremona G (2007) Alveolar-derived exhaled nitric oxide is reduced in obstructive sleep apnea syndrome. Chest 132:860–867
Alberti A, Sarchielli P, Gallinella E, Floridi A, Floridi A, Mazzotta G, Gallai V (2003) Plasma cytokine levels in patients with obstructive sleep apnea syndrome: a preliminary study. J Sleep Res 12:305–311
Ciftci TU, Kokturk O, Bukan N, Bilgihan A (2004) Relationship between serum cytokine levels with obesity and obstructive sleep apnea syndrome. Cytokine 21:87–91
Kushida CA, Littner MR, Hirshkowitz M, Morgenthaler TI, Alessi CA, Bailey D, Boehlecke B, Brown TM, Coleman J Jr, Friedman L, Kapen S, Kapur VK, Kramer M, Lee-Chiong T, Owens J, Pancer JP, Swick TJ, Wise MS (2006) American Academy of Sleep Medicine Practice parameters for the use of continuous and bilevel positive airway pressure devices to treat adult patients with sleep-related breathing disorders. Sleep 29:375–380
Kushida CA, Morgenthaler TI, Littner MR, Alessi CA, Bailey D, Coleman J Jr, Friedman L, Hirshkowitz M, Kapen S, Kramer M, Lee-Chiong T, Owens J, Pancer JP (2006) American Academy of Sleep Practice parameters for the treatment of snoring and obstructive sleep apnea with oral appliances. Sleep 29:240–243
Skoczyński S, Ograbek-Król M, Tazbirek M, Semik-Orzech A, Pierzchała W (2008) Short-term CPAP treatment induces a mild increase in inflammatory cells in patients with sleep apnoea syndrome. Rhinology 46:144–150
Kohler M, Ayers L, Pepperell JC, Packwood KL, Ferry B, Crosthwaite N, Craig S, Siccoli MM, Davies RJ, Stradling JR (2009) Effects of continuous positive airway pressure on systemic inflammation in patients with moderate to severe obstructive sleep apnoea: a randomised controlled trial. Thorax 64:67–73
Fortuna AM, Miralda R, Calaf N, González M, Casan P, Mayos M (2011) Airway and alveolar nitric oxide measurements in obstructive sleep apnea syndrome. Respir Med 105:630–636
Tamaki S, Yamauchi M, Fukuoka A, Makinodan K, Koyama N, Tomoda K, Yoshikawa M, Kimura H (2007) Production of inflammatory mediators by monocytes in patients with obstructive sleep apnea syndrome. Intern Med 48:1255–1262
Iber C, Ancoli-Israel S, Chesson A, Quan SF (2007) The AASM manual for the scoring of sleep and associated events: rules, terminology, and technical specification. 1st ed. American Academy of Sleep Medicine, Westchester
McNicholas WT (2009) Obstructive sleep apnea and inflammation. Prog Cardiovasc Dis 51:392–399
Salerno FG, Carpagnano E, Guido P, Bonsignore MR, Roberti A, Aliani M, Vignola AM, Spanevello A (2004) Airway inflammation in patients affected by obstructive sleep apnea syndrome. Respir Med 98:25
Guasti L, Marino F, Cosentino M, Maroni L, Maresca AM, Colombo F, Maio RC, Castiglioni L, Saporiti F, Loraschi A, Gaudio G, Bernasconi A, Laurita E, Grandi AM, Venco A (2011) Cytokine production from peripheral blood mononuclear cells and polymorphonuclear leukocytes in patients studied for suspected obstructive sleep apnea. Sleep Breath 15:3–11
Devouassoux G, Lévy P, Rossini E, Pin I, Fior-Gozlan M, Henry M, Seigneurin D, Pépin JL (2007) Sleep apnoea is associated with bronchial inflammation and continuous positive airway pressure-induced airway hyperresponsiveness. J Allergy Clin Immunol 119:597–603
Vgontzas AN, Zoumakis E, Bixler EO, Lin HM, Collins B, Basta M, Pejovic S, Chrousos GP (2008) Selective effects of CPAP on sleep apnoea-associated manifestations. Eur J Clin Invest 38:585–595
Mota PC, Drummond M, Winck JC, Santos AC, Almeida J, Marques JA (2011) APAP impact on metabolic syndrome in obstructive sleep apnea patients. Sleep Breath 15:665–672
Hegglin A, Schoch OD, Korte W, Hahn K, Hürny C, Münzer T (2012) Eight months of continuous positive airway pressure (CPAP) decrease tumor necrosis factor alpha (TNFA) in men with obstructive sleep apnea syndrome. Sleep Breath 16:405–412
Yokoe T, Minoguchi K, Matsuo H, Oda N, Minoguchi H, Yoshino G, Hirano T, Adachi M (2003) Elevated levels of C-reactive protein and interleukin-6 in patients with obstructive sleep apnea syndrome are decreased by nasal continuous positive airway pressure. Circulation 107:1129–1134
Carpagnano GE, Spanevello A, Sabato R, Depalo A, Turchiarelli V, Foschino MP (2008) Exhaled pH, exhaled nitric oxide, and induced sputum cellularity in obese patients with obstructive sleep apnea syndrome. Transl Res 151:45–50
Weaver TE, Maislin G, Dinges DF, Bloxham T, George CF, Greenberg H, Kader G, Mahowald M, Younger J, Pack AI (2007) Relationship between hours of CPAP use and achieving normal levels of sleepiness and daily functioning. Sleep 30:711–719
Hunt J (2007) Exhaled breath condensate: an overview. Immunol Allergy Clin North Am 27:587–596
Rosias PP, Robroeks CM, Kester A, den Hartog GJ, Wodzig WK, Rijkers GT, Zimmermann LJ, van Schayck CP, Jöbsis Q, Dompeling E (2008) Biomarker reproducibility in exhaled breath condensate collected with different condensers. Eur Respir J 31:934–942
Yamauchi M, Kimura H (2008) Oxidative stress in obstructive sleep apnea: putative pathways to the cardiovascular complication. Antioxid Redox Signal 10:735–768
Petrosyan M, Perraki E, Simoes D, Koutsourelakis I, Vagiakis E, Roussos C, Gratziou C (2008) Exhaled breath markers in patients with obstructive sleep apnea. Sleep Breath 12:207–215
Acknowledgments
This study is supported by Fatih University Scientific Research Fund under project no. P53011005_2.
Conflict of interest
All authors have indicated no financial conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Karamanlı, H., Özol, D., Ugur, K.S. et al. Influence of CPAP treatment on airway and systemic inflammation in OSAS patients. Sleep Breath 18, 251–256 (2014). https://doi.org/10.1007/s11325-012-0761-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-012-0761-8