Abstract
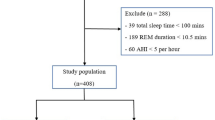
Sleep disordered breathing occurring predominantly in rapid eye movement REM sleep (rapid-eye-movement-related sleep-disordered breathing, REM SDB) is present in 10 to 36% of patients undergoing polysomnography (PSG) for suspected obstructive sleep apnea (O’Connor et al. in Am J Respir Crit Care Med 161:1465–1472, 2000; Resta et al. in J Respir Medicine 99:91–96, 2005; Haba-Rubio et al. in Chest 128:3350–3357, 2005; Juvelekian and Golish, American Academy of Sleep Medicine, abstract, 2004). We hypothesize that REM SDB is an age-related condition in women and, additionally, more prevalent in women than in men. Subjects with REM SDB were identified retrospectively among 1,540 obstructive sleep apnea (OSA) patients with an apnea–hypopnea index (AHI) ≥ 5. Inclusion criteria for REM SDB were age >18, AHI ≥ 5, NREM AHI < 15, and REM AHI/NREM AHI > 2. PSG data included sleep latency, REM latency, total sleep time (TST), AHI, REM AHI, NREM AHI, and sleep stage percentages. Demographic data and medical and psychiatric histories were also obtained. Statistical comparisons were made between men and women and women older and younger than 55 years, a marker for menopausal status. Two hundred twenty-one subjects fulfilled the criteria for REM SDB, yielding a prevalence of 14.4%. Overall, female apneics had a significantly higher prevalence of REM SDB than did men (24.5 vs 7.9%; p < 0.001). Younger women had a significantly higher prevalence than did older women (27.2 vs 18.6%; p = 0.008); younger men had a significantly higher prevalence of REM SDB than did older men (9.9 vs 4.5%; p = 0.002). Women were significantly older and more obese than were men. Younger women were more likely to be depressed and were significantly more obese than were older women. REM SDB is more prevalent in women than in men and more prevalent in men and women younger than 55 than those older than 55. In this population, women are more obese and older than men, while younger women were more obese than older women. These descriptive distinctions suggest differences in mechanism which may depend on gender and age.
Similar content being viewed by others
References
O’Connor C, Thornley K, Hanly P (2000) Gender differences in the polysomnographic features of obstructive sleep apnea. Am J Respir Crit Care Med 161:1465–1472
Resta O, Carpanano G, Lacedonia D, DiGioia G, Gilberti T, Stefano A, Bonfitto P (2005) Gender difference in sleep profile of severely obese patients with obstructive sleep apnea. Respir Medicine 99:91–96
Haba-Rubio J, Janssens J, Rochat T, Sforza E (2005) Rapid eye movement-related disordered breathing: clinical and polysomnographic features. Chest 128:3350–3357
Juvelekian G, Golish J (2004) Prevalence and characteristics of rapid eye movement related obstructive sleep apnea syndrome. American Academy of Sleep Medicine, abstract
Young T, Palta M, Dempsey J, Skatrud J, Weber S, Badr S (1993) The occurrence of sleep-disordered breathing among middle-aged adults. N Engl J Med 328:1230–1235
Bixler E, Vgontzas A, Ten Have T, Tyson K, Kales A (1998) Effects of age on sleep apnea in men: I. Prevalence and severity. Am J Respir Crit Care Med 157:144–148
Xiao Y, Huang X, Qiu C, Zhu X, Liu Y (1999) Angiotensin-1-converting enzyme gene polymorphism in Chinese patients with obstructive sleep apnea syndrome. Chin Med 112:701–704
Redline S, Leitner J, Arnold J, Tishler P, Altose M (1997) Ventilatory-control abnormalities in familial sleep apnea. Am J Respir Crit Care Med 156:155–160
Katz E, White D (2004) Genioglossus activity during sleep in normal control subjects and children with obstructive sleep apnea. Am J Respir Crit Care Med 170(5):553–560
White D, Douglas N, Pickett C, Weil J, Zwillich C (1982) Hypoxic ventilatory response decreases during sleep in normal men. Am Rev Respir Dis 125:286–89
Douglas N, White D, Weil J, Pickett C, Zwillich C (1982) Hypercapnic ventilatory response in sleeping adults. Am Rev Respir Dis 126:758–762
Series F, Cormier Y, La Forge J (1990) Influence of apnea type and sleep stage on nocturnal postapneic desaturation. Am Rev Respir Dis 141(6):1522–1526
Rechtschaffen A, Kales A (1968) A manual of standardized terminology, techniques, and scoring system for sleep stages of human subjects. US Department of Health, Education, and Welfare Public Health Service-NIH/NIND
American Academy of Sleep Medicine Task Force (1999) Sleep-related breathing disorders in adults: recommendations for syndrome definition and measurement techniques in clinical research. Sleep 22:667–669
Redline S, Tishler PV, Hans MG, Tosteson TD, Strohl KP, Spry K (1997) Racial differences in sleep-disordered breathing in African-Americans and Caucasians. Am J Respir Crit Care Med 155(1):186–192
Pinheiro SP, Holmes MD, Pollak MN, Barbieri RL, Hankinson SE (2005) Racial differences in premenopausal endogenous hormones. Cancer Epidemiol Biomark Prev 14(9):2147–53
Lamon-Fava S, Barnett JB, Woods MN, McCormack C, McNamara JR, Schaefer EJ, Longcope C, Rosner B, Gorbach SL (2005) Differences in serum sex hormone and plasma lipid levels in Caucasian and African-American premenopausal women. J Clin Endocrinol Metab 90(8):4516–20
Quintana-Gallego E, Carmona-Bernal C, Capote F, Sanchez-Armengol A, Botebol-Benhamou G, Polo-Padillo J, Castillo-Gomez J (2004) Gender differences in obstructive sleep apnea syndrome: a clinical study of 1166 patients. Respir Med 98(10):984–989
Shepertycky MR, Banno K, Kryger MH (2005) Differences between men and women in the clinical presentation of patients diagnosed with obstructive sleep apnea syndrome. Sleep 28(3):309–314
Johnson EO, Roth T, Breslau N (2006) The association of insomnia with anxiety disorders and depression: exploration of the direction of risk. J Psychiatr Res 40(8):700–8
Kupfer DJ (1976) REM latency: a psychobiologic marker for primary depressive disease. Biol Psychiatry 11(2):159–174
Gottesmann C, Gottesman I (2007) The neurobiological characteristics of rapid eye movement (REM) sleep are candidate endophenotypes of depression, schizophrenia, mental retardation and dementia. Prog Neurobiol 81(4):237–250
Netzer NC, Eliasson AH, Strohl KP (2003) Women with sleep apnea have lower levels of sex hormones. Sleep Breath 7(1):25–29
Resta O, Caratozzolo G, Pannacciulli N, Stefano A, Giliberti T, Carpagnano GE, De Pergola G (2003) Gender, age and menopause effects on the prevalence and the characteristics of obstructive sleep apnea in obesity. Eur J Clin Investig 33(12):1084–1089
Popovic R, White D (1998) Upper airway muscle activity in normal women: influence of hormonal status. J Appl Physiol 84(3):1055–1062
Brooks LJ, Strohl KP (1992) Size and mechanical properties of the pharynx in healthy men and women. Am Rev Respir Dis 146(6):1394–1397
Zwillich C, Natalino M, Sutton F, Weil J (1978) Effect of progesterone on chemosensitivity in normal man. J Lab Clin Med 92:262–69
Shahar E, Redline S, Young T et al (2003) Hormone replacement therapy and sleep-disordered breathing. Am J Respir Crit Care Med 167:1186–92
Yamazaki H, Haji A, Ohi Y, Takeda R (2005) Effects of progesterone on apneic events during behaviorally defined sleep in male rats. Life Sci 78(4):383–8
Kryger M, Roth T, Dement W (2005) Principles and practice of sleep medicine. Elsevier, Philadelphia
Eikermann M, Jordan AS, Chamberlin NL, Gautam S, Wellman A, Lo YL, White DP, Malhotra A (2007) The influence of aging on pharyngeal collapsibility during sleep. Chest 131(6):1702–1709
Anttalainen U, Saaresranta T, Aittokallio J, Kalleinen N, Vahlberg T, Virtanen I, Polo O (2006) Impact of menopause on the manifestation and severity of sleep-disordered breathing. Acta Obstet Gynecol Scand 85(11):1381–1388
Acknowledgments
The authors would like to thank Nancy Foldvary-Schaefer for her help in the initial stages of project design as well as Tyler Bedford for his technical expertise.
Author information
Authors and Affiliations
Corresponding author
Additional information
The authors have no financial disclosures or conflicts of interest to offer.
Rights and permissions
About this article
Cite this article
Koo, B.B., Dostal, J., Ioachimescu, O. et al. The effects of gender and age on REM-related sleep-disordered breathing. Sleep Breath 12, 259–264 (2008). https://doi.org/10.1007/s11325-007-0161-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-007-0161-7