Abstract
Purpose
Body mass index (BMI) might be an inaccurate estimate of detailed body composition because it does not differentiate muscle from fat mass. We sought to understand the effect of kidney function decline on alterations of body composition patterns among pre-dialysis CKD patients.
Methods
Body composition was measured by multi-frequency bioelectrical impedance analysis (BIA). Low muscle mass was defined as appendicular muscle mass (kg) adjusted to the square of height in meters < 7.0 and 5.7 kg/m2 in men and women, respectively. The designation of obesity by percent body fat was ≥ 25% in men and ≥ 30% in women. Alternative definition of obesity by BMI was ≥ 25 kg/m2. Visceral fat area cut point was > 100 cm2 as indication of abdominal obesity.
Results
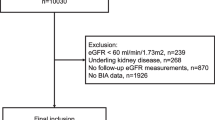
Mean age of participants was 61.3 ± 13.8 years (n = 103). The average glomerular filtration rate (GFR) was 34.0 ± 24.2 mL/min/1.73 m2. By BIA, the prevalence of low muscle mass was 16.5% and was comparable between both sexes. Obesity by percent body fat was identified in 71.8% of patients and 38.2% had abdominal obesity. Using BMI criteria, the prevalence of obesity was less common (55.3%) and associated with under-identification of obesity by 27.0%. Low muscle mass and obesity by percent body fat were more prevalent in the more advanced stages of CKD. By multivariable regression analysis, a 10 mL/min/1.73 m2 decline in GFR was associated with a 0.59 kg reduction of total body muscle mass (p = 0.01), but not fat mass or BMI, after adjusting for confounders.
Conclusion
Low muscle mass was prevalent among pre-dialysis CKD patients. BMI commonly classified obese CKD individuals by percent body fat criteria as non-obese. The reduction of muscle mass was associated with GFR decline.



Similar content being viewed by others
References
Zoccali C, Torino C, Tripepi G, Mallamaci F (2012) Assessment of obesity in chronic kidney disease: what is the best measure? Curr Opin Nephrol Hypertens 21:641–646
Foley RN, Wang C, Ishani A, Collins AJ, Murray AM (2007) Kidney function and sarcopenia in the United States general population: NHANES III. Am J Nephrol 27:279–286
Sharma D, Hawkins M, Abramowitz MK (2014) Association of sarcopenia with eGFR and misclassification of obesity in adults with CKD in the United States. Clin J Am Soc Nephrol 9:2079–2088
Beaudart C, McCloskey E, Bruyere O et al (2016) Sarcopenia in daily practice: assessment and management. BMC Geriatr 16:170
Carrero JJ, Johansen KL, Lindholm B et al (2016) Screening for muscle wasting and dysfunction in patients with chronic kidney disease. Kidney Int 90:53–66
Cruz-Jentoft AJ, Bahat G, Bauer J et al (2019) Sarcopenia: revised European consensus on definition and diagnosis. Age Ageing 48:16–31
Chen LK, Woo J, Assantachai P et al (2020) Asian Working Group for Sarcopenia: 2019 consensus update on sarcopenia diagnosis and treatment. J Am Med Dir Assoc. https://doi.org/10.1016/j.jamda.2019.12.012
Saitoh M, Ogawa M, Kondo H et al (2019) Sarcopenic obesity and its association with frailty and protein-energy wasting in hemodialysis patients: preliminary data from a single center in Japan. Ren Replace Ther 5:46. https://doi.org/10.1186/s41100-019-0240-9
Honda H, Qureshi AR, Axelsson J et al (2007) Obese sarcopenia in patients with end-stage renal disease is associated with inflammation and increased mortality. Am J Clin Nutr 86:633–638
Malhotra R, Deger SM, Salat H et al (2017) Sarcopenic obesity definitions by body composition and mortality in the hemodialysis patients. J Ren Nutr 27:84–90
Tabibi H, As'habi A, Najafi I, Hedayati M (2018) Prevalence of dynapenic obesity and sarcopenic obesity and their associations with cardiovascular disease risk factors in peritoneal dialysis patients. Kidney Res Clin Pract 37:404–413
Levey AS, Stevens LA, Schmid CH et al (2009) A new equation to estimate glomerular filtration rate. Ann Intern Med 150:604–612
Kidney Disease: Improving Global Outcomes (KDIGO) CKD Work Group (2013) KDIGO Clinical practice guideline for the evaluation and management of chronic kidney disease. Kidney Int Suppl 3:1–150
Okorodudu DO, Jumean MF, Montori VM et al (2010) Diagnostic performance of body mass index to identify obesity as defined by body adiposity: a systematic review and meta-analysis. Int J Obes (Lond) 34:791–799
Kanazawa M, Yoshiike N, Osaka T et al (2005) Criteria and classification of obesity in Japan and Asia-Oceania. World Rev Nutr Diet 94:1–12
Japan Society for the Study of Obesity (2002) New criteria for ‘obesity disease’ in Japan. Circ J 66:987–992
Androga L, Sharma D, Amodu A, Abramowitz MK (2017) Sarcopenia, obesity, and mortality in US adults with and without chronic kidney disease. Kidney Int Rep 2:201–211
Rymarz A, Zajbt M, Jeznach-Steinhagen A, Wozniak-Kosek A, Niemczyk S (2019) Body composition and biochemical markers of nutrition in non-dialysis-dependent chronic kidney disease patients. Adv Exp Med Biol. https://doi.org/10.1007/5584_2019_444
Dierkes J, Dahl H, Lervaag Welland N et al (2018) High rates of central obesity and sarcopenia in CKD irrespective of renal replacement therapy—an observational cross-sectional study. BMC Nephrol 19:259
Cruz-Jentoft AJ, Baeyens JP, Bauer JM et al (2010) Sarcopenia: European consensus on definition and diagnosis: report of the European Working Group on Sarcopenia in older people. Age Ageing 39:412–423
Baumgartner RN, Koehler KM, Gallagher D et al (1998) Epidemiology of sarcopenia among the elderly in New Mexico. Am J Epidemiol 147:755–763
Janssen I, Baumgartner RN, Ross R, Rosenberg IH, Roubenoff R (2004) Skeletal muscle cutpoints associated with elevated physical disability risk in older men and women. Am J Epidemiol 159:413–421
Cawthon PM, Peters KW, Shardell MD et al (2014) Cutpoints for low appendicular lean mass that identify older adults with clinically significant weakness. J Gerontol A Biol Sci Med Sci 69:567–575
Saitoh M, Ishida J, Springer J (2017) Considering technique of assessment and method for normalizing skeletal muscle mass. J Cachexia Sarcopenia Muscle 8:853–854
Dufour AB, Hannan MT, Murabito JM, Kiel DP, McLean RR (2013) Sarcopenia definitions considering body size and fat mass are associated with mobility limitations: the Framingham Study. J Gerontol A Biol Sci Med Sci 68:168–174
Dam TT, Peters KW, Fragala M et al (2014) An evidence-based comparison of operational criteria for the presence of sarcopenia. J Gerontol A Biol Sci Med Sci 69:584–590
Delmonico MJ, Harris TB, Lee JS et al (2007) Alternative definitions of sarcopenia, lower extremity performance, and functional impairment with aging in older men and women. J Am Geriatr Soc 55:769–774
World Health Organization (2000) Obesity: preventing and managing the global epidemic. World Health Organization, Geneva (WHO Technical Report Series 894)
Agarwal R, Bills JE, Light RP (2010) Diagnosing obesity by body mass index in chronic kidney disease: an explanation for the "obesity paradox?". Hypertension 56:893–900
Sanches FM, Avesani CM, Kamimura MA et al (2008) Waist circumference and visceral fat in CKD: a cross-sectional study. Am J Kidney Dis 52:66–73
Sheean P, Gonzalez MC (2020) American Society for Parenteral and Enteral Nutrition Clinical Guidelines: the validity of body composition assessment in clinical populations. J Parenter Enter Nutr 44:12–43
Zhou Y, Hellberg M, Svensson P, Hoglund P, Clyne N (2018) Sarcopenia and relationships between muscle mass, measured glomerular filtration rate and physical function in patients with chronic kidney disease stages 3–5. Nephrol Dial Transplant 33:342–348
Zhang L, Wang XH, Wang H, Du J, Mitch WE (2010) Satellite cell dysfunction and impaired IGF-1 signaling cause CKD-induced muscle atrophy. J Am Soc Nephrol 21:419–427
Wang XH, Mitch WE (2014) Mechanisms of muscle wasting in chronic kidney disease. Nat Rev Nephrol 10:504–516
Souza VA, Oliveira D, Barbosa SR et al (2017) Sarcopenia in patients with chronic kidney disease not yet on dialysis: analysis of the prevalence and associated factors. PLoS ONE 12:e0176230
Ling CH, de Craen AJ, Slagboom PE et al (2011) Accuracy of direct segmental multi-frequency bioimpedance analysis in the assessment of total body and segmental body composition in middle-aged adult population. Clin Nutr 30:610–615
Ogawa H, Fujitani K, Tsujinaka T et al (2011) InBody 720 as a new method of evaluating visceral obesity. Hepatogastroenterology 58:42–44
Acknowledgements
We would like to thank Wasan Panyasang, M.Sc. (Applied statistics), as the consulting statistician for this project.
Funding
This work has been made possible in part by a Special Task Force for Activating Research (STAR) in Renal Nutrition, Chulalongkorn University funded grant to Dr. Kittiskulnam.
Author information
Authors and Affiliations
Contributions
PK: research idea and study design. MN, KM, KP: data acquisition. SE, SS data analysis and interpretation. PK: statistical analysis. SE: supervision and mentorship. Each author contributed important intellectual content during manuscript drafting. All authors made substantial contributions, read, and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
None to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kittiskulnam, P., Nitesnoppakul, M., Metta, K. et al. Alterations of body composition patterns in pre-dialysis chronic kidney disease patients. Int Urol Nephrol 53, 137–145 (2021). https://doi.org/10.1007/s11255-020-02599-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-020-02599-4