Abstract
Purpose
The aim of our study was to investigate the impact of the ABO blood groups and blood-based biomarkers on the growth kinetics of renal angiomyolipoma (AML).
Methods
A total of 124 patients with AML who were followed-up between 2010 and 2018 were retrospectively reviewed. The patients’ characteristics were recorded, including age, body mass index (BMI), blood pressure, smoking history, and ABO blood group. Baseline laboratory test results, including serum creatinine, AST, ALT, platelet, neutrophil and lymphocyte count, were used to calculate the estimated glomerular filtration rate (eGFR), neutrophil-to-lymphocyte ratio (NLR), platelet-to-lymphocyte ratio (PLR), and De Ritis ratio. The Cox regression analysis was used to evaluate the relationship between variables and tumor growth.
Results
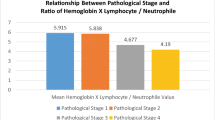
The study population comprised 71 women and 44 men with a median age of 47.3 (28–65) years. Among patients classified according to the blood groups, no significant differences were observed regarding age, BMI, smoking history, co-morbidities, NLR, PLR, De Ritis ratio, eGFR, or tumor size and localisation. The mean growth rate from baseline to the last scan was 0.36 ± 0.27 cm, 0.21 ± 0.21 cm, 0.14 ± 0.11 cm, and 0.19 ± 0.17 cm for blood type O, A, B, and AB, respectively. In multivariate analysis, eGFR < 60 (p = 0.044), central tumor localisation (p = 0.030), presence of blood group-0 (p = 0.038), and De Ritis ratio ≥ 1.24 (p = 0.047) were statistically associated with tumor growth.
Conclusion
Our study demonstrates that both the ABO blood groups and the De Ritis ratio might represent independent predictors of tumor growth rate in patients with renal AML.

Similar content being viewed by others
References
Lane BR, Aydin H, Danforth TL, Zhou M, Remer EM, Novick AC et al (2008) Clinical correlates of renal angiomyolipoma subtypes in 209 patients: classic, fat poor, tuberous sclerosis associated and epithelioid. J Urol 180(3):836–843
Fittschen A, Wendlik I, Oeztuerk S, Kratzer W, Akinli AS, Haenle MM et al (2014) Prevalence of sporadic renal angiomyolipoma: a retrospective analysis of 61,389 in- and out-patients. Abdom Imaging 39(5):1009–1013
Koo KC, Kim WT, Ham WS, Lee JS, Ju HJ, Choi YD (2010) Trends of presentation and clinical outcome of treated renal angiomyolipoma. Yonsei Med J 51(5):728–734
Flum AS, Hamoui N, Said MA, Yang XJ, Casalino DD, McGuire BB et al (2016) Update on the diagnosis and management of renal angiomyolipoma. J Urol 195(4 Pt1):834–846
Bhatt JR, Richard PO, Kim NS, Finelli A, Manickavachagam K, Legere L et al (2016) Natural history of renal angiomyolipoma (AML): most patients with large AMLs> 4 cm can be offered active surveillance as an initial management strategy. Eur Urol 70(1):85–90
Mues AC, Palacios JM, Haramis G, Casazza C, Badani K, Gupta M et al (2010) Contemporary experience in the management of angiomyolipoma. J Endourol 24(11):1883–1886
Yamamoto F, Cid E, Yamamoto M, Blancher A (2012) ABO research in the modern era of genomics. Transfus Med Rev 26(2):103–118
Eastlund T (1998) The histo-blood group ABO system and tissue transplantation. Transfusion 38(10):975–988
Liumbruno GM, Franchini M (2014) Hemostasis, cancer, and ABO blood group: the most recent evidence of association. J Thromb Thrombolysis 38(2):160–166
Marchioni M, Primiceri G, Ingrosso M, Filograna R, Castellan P, De Francesco P et al (2016) The clinical use of the Neutrophil to lymphocyte ratio in urothelial cancer: a systematic review. Clin Genitourin Cancer 14(6):473–484
Lee H, Lee SE, Byun SS, Kim HH, Kwak C, Hong SK (2017) De Ritis ratio (aspartate transaminase/alanine transaminase ratio) as a signifcant prognostic factor after surgical treatment in patients with clear-cell localized renal cell carcinoma: a propensity score-matched study. BJU Int 119(2):261–267
Ljungberg B, Bensalah K, Canfield S, Dabestani S, Hofmann F, Hora M et al (2014) EAU guidelines on renal cell carcinoma: 2014 update. Eur Urol 67(5):913–924
Ouzaid I, Autorino R, Fatica R, Herts BR, McLennan G, Remer EM (2014) Active surveillance for renal angiomyolipoma: outcomes and factors predictive of delayed intervention. BJU Int 114(3):412–417
Champagnac J, Melodelima C, Martinelli T, Pagnoux G, Badet L, Juilard L et al (2016) Microaneurysms in renal angiomyolipomas: can clinical and computed tomography features predict their presence and size? Diagn Interv Imaging 97(3):321–326
Joh HK, Cho E, Choueiri TK (2012) ABO blood group and risk of renal cell cancer. Cancer Epidemiol 36(6):528–532
De Martino M, Waldert M, Haitel A, Schatzl G, Shariat SF, Klatte T (2014) Evaluation of ABO blood group as a prognostic marker in renal cell carcinoma (RCC). BJU Int 113(5b):E62–E66
Kaffenberger SD, Morgan TM, Stratton KL, Boachie AM, Barocas DA, Chang SS et al (2012) ABO blood group is a predictor of survival in patients undergoing surgery for renal cell carcinoma. BJU Int 110(11 Pt B):E641–E646
Ko K, Park YH, Jeong CW, Ku JH, Kim HH, Kwak C (2016) Prognostic significance of blood type A in patients with renal cell carcinoma. Urol J 13(4):2765–2772
Paterson C, Yew-Fung C, Sweeney C, Szewczyk-Bieda M, Lnag S, Nabi G (2017) Predictors of growth kinetics and outcomes in small renal masses (SRM ≤ 4 cm in size): tayside Active Surveillance Cohort (TASC) Study. Eur J Surg Oncol 43(8):1589–1597
Hakomori S (1999) Antigen structure and genetic basis of histo-blood groups A, B and 0: their changes associated with human cancer. Biochim Biophys Acta 1473(1):247–266
Halloran MM, Carley WW, Polverini PJ, Haskell CJ, Phan S, Anderson BJ et al (2000) Ley/H: an endothelial-selective, cytokine-inducible, angiogenic mediator. J Immunol 164(9):4868–4877
Botros M, Sikaris KA (2013) The De Ritis ratio: the test of time. Clin Biochem Rev 34(3):117–130
Ishihara H, Kondo T, Yoshida K, Omae K, Takagi T, Iizuka J et al (2017) Evaluation of preoperative aspartate transaminase/alanine transaminase ratio as an independent predictive biomarker in patients with metastatic renal cell carcinoma undergoing cytoreductive nephrectomy: a propensity score matching study. Clin Genitourin Cancer 15(5):598–604
Vander Heiden MG, Cantley LC, Thompson CB (2009) Understanding the Warburg effect: the metabolic requirements of cell proliferation. Science 324(5930):1029–1033
Greenhouse WV, Lehninger AL (1976) Ocurrence of the malate-aspartate shuttle in various tumor types. Cancer Res 36(4):1392–1396
Li W, Guo L, Bi X, Ma J, Zheng S (2015) Immunohistochemistry of p53 and Ki-67 and p53 mutation analysis in renal epithelioid angiomyolipoma. Int J Clin Exp Pathol 8(8):9446–9451
Bertolini F, Casarotti G, Righi L, Bollito E, Albera C, Racca SA et al (2018) Human renal angiomyolipoma cells of male and female origin can migrate and are influenced by microenviromental factors. PLoS ONE 13(6):e0199371
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All the authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Arslan, B., Gürkan, O., Çetin, B. et al. Evaluation of ABO blood groups and blood-based biomarkers as a predictor of growth kinetics of renal angiomyolipoma. Int Urol Nephrol 50, 2131–2137 (2018). https://doi.org/10.1007/s11255-018-2012-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-018-2012-9