Abstract
Purpose
The purpose of the study was to investigate health-related quality of life (HRQOL) and its associated factors among elderly individuals with dyslipidemia in rural Northern China.
Methods
A cross-sectional study was conducted on 457 elderly individuals. The EQ-5D-5L questionnaire was used to assess HRQOL. Sociodemographic, anthropometric, lifestyle and health information was collected using a structured and standardized questionnaire. The Tobit regression model and multiple linear regression analysis were used to assess factors associated with HRQOL parameters including utility index and visual analogue score (EQ-VAS).
Results
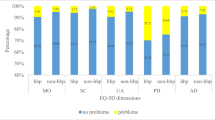
The mean age of the participating individuals was 68.04 ± 5.98 years. The median utility index and EQ-VAS scores were 0.942 (P25-P75: 0.876–1.000) and 80 (P25-P75: 70–90), respectively. Pain/discomfort was the most frequently reported complaint among the five health dimensions (50.5%). Illiterate and primary education levels, unemployed, widowed, smoking, secondhand smoke exposure, with hypertension or DM, chronic disease core knowledge scores < 8, and daily sedentary time ≥ 6 h were associated with lower HRQOL.
Conclusion
Pain/discomfort dimension was the most affected problems. Education, occupation, marital status, smoking, secondhand smoke exposure, chronic disease core knowledge, comorbidities, and daily sedentary time were significantly associated with HRQOL in the present study.

Similar content being viewed by others
References
Handelsman, Y., Jellinger, P. S., Guerin, C. K., Bloomgarden, Z. T., Brinton, E. A., Budoff, M. J., et al. (2020). Consensus Statement by the American Association of Clinical Endocrinologists and American College of Endocrinology on the Management of Dyslipidemia and Prevention of Cardiovascular Disease Algorithm - 2020 Executive Summary. Endocrine Practice, 26(10), 1196–1224.
Opoku, S., Gan, Y., Fu, W., Chen, D., Addo-Yobo, E., Trofimovitch, D., et al. (2019). Prevalence and risk factors for dyslipidemia among adults in rural and urban China: Findings from the China National Stroke Screening and prevention project (CNSSPP). BMC Public Health, 19(1), 1500.
Jellinger, P. S., Handelsman, Y., Rosenblit, P. D., Bloomgarden, Z. T., Fonseca, V. A., Garber, A. J., et al. (2017). American association of clinical endocrinologists and American college of endocrinology guidelines for management of dyslipidemia and prevention of cardiovascular disease. Endocrine practice, 23(Suppl 2), 1–87.
White, B. E., Druce, M. R., Grozinsky-Glasberg, S., Srirajaskanthan, R., Gamper, E. M., Gray, D., et al. (2020). Health-related quality of life in neuroendocrine neoplasia: A critical review. Endocrine-related Cancer, 27(7), R267–R280.
Jonak, C., Porkert, S., Oerlemans, S., Papadavid, E., Molloy, K., Lehner-Baumgartner, E., et al. (2019). Health-related quality of life in cutaneous lymphomas: past, present and future. Acta dermato-venereologica, 99(7), 640–646.
Lapin, B. R. (2020). Considerations for reporting and reviewing studies including health-related quality of life. Chest, 158(1S), S49–S56.
Luo, N., Liu, G., Li, M., Guan, H., Jin, X., & Rand-Hendriksen, K. (2017). Estimating an EQ-5D-5L value set for China. Value in Health, 20(4), 662–669.
Jarab, A. S., Alefishat, E. A., Al-Qerem, W., Mukattash, T. L., & Abu-Zaytoun, L. (2021). Variables associated with poor health-related quality of life among patients with dyslipidemia in Jordan. Quality of life research, 30(5), 1417–1424.
Xi, Y., Niu, L., Cao, N., Bao, H., Xu, X., Zhu, H., et al. (2020). Prevalence of dyslipidemia and associated risk factors among adults aged ≥35 years in northern China: A cross-sectional study. BMC Public Health, 20(1), 1068.
Wilson, I. B., & Cleary, P. D. (1995). Linking clinical variables with health-related quality of life A conceptual model of patient outcomes. JAMA, 273(1), 59–65.
Ferrans, C. E., Zerwic, J. J., Wilbur, J. E., & Larson, J. L. (2005). Conceptual model of health-related quality of life. Journal of Nursing Scholarship, 37(4), 336–342.
Damayanthi, H., Moy, F. M., Abdullah, K. L., & Dharmaratne, S. D. (2018). Health related quality of life and its associated factors among community-dwelling older people in Sri Lanka: A cross-sectional study. Archives of Gerontology and Geriatrics, 76, 215–220.
Liao, W., Liu, X., Kang, N., Song, Y., Yuchi, Y., Hu, Z., et al. (2022). Associations between healthy lifestyle score and health-related quality of life among Chinese rural adults: variations in age, sex, education level, and income. Quality of Life Research, 32(1), 81–92.
Aschalew, A. Y., Yitayal, M., & Minyihun, A. (2020). Health-related quality of life and associated factors among patients with diabetes mellitus at the University of Gondar referral hospital. Health Quality Life Outcomes, 18(1), 62.
Su, F., Fan, B., Song, N., Dong, X., Wang, Y., Li, J., et al. (2021). Survey on public psychological intervention demand and influence factors analysis. International Journal of Environmental Research and Public Health, 18(9), 4808.
WS/T 428–2013. Health industry standard of the people's Republic of China.
Qin, L., & Xu, H. (2016). A cross-sectional study of the effect of health literacy on diabetes prevention and control among elderly individuals with prediabetes in rural China. British Medical Journal Open, 6(5), e11077.
WHO. (2006). Defifinition and Diagnosis of Diabetes Mellitus and Intermediate Hyperglycemia. Geneva.
Guo, J., Guan, T., Shen, Y., Chao, B., Li, M., Wang, L., et al. (2018). Lifestyle factors and gender-specific risk of stroke in adults with diabetes mellitus: a case-control study. Journal of stroke and cerebrovascular diseases, 27(7), 1852–1860.
Yang, Y., Yang, X. Y., Yang, T., He, W., Peng, S., & Rockett, I. R. (2021). Social deprivation and secondhand smoke exposure among urban male residents: A nationwide study in China. Tobacco Induced Diseases, 19, 21.
Luo, B., Zhang, J., Hu, Z., Gao, F., Zhou, Q., Song, S., et al. (2018). Diabetes-related behaviours among elderly people with pre-diabetes in rural communities of Hunan, China: A cross-sectional study. British Medical Journal Open, 8(1), e15747.
Barreno, M., Sisa, I., Yepez, G. M., Shen, H., Villar, M., Kovalskys, I., et al. (2021). Association between built environment and physical activity in Latin American countries: A multicentre cross-sectional study. British Medical Journal Open, 11(11), e46271.
Pan, Y. (2017). Study on Nutrition Status and Risk Factors of Major Chronic Diseases in Tianjin. Tianjin Medical University.
Kittikraisak, W., Kingkaew, P., Teerawattananon, Y., Yothasamut, J., Natesuwan, S., Manosuthi, W., et al. (2012). Health related quality of life among patients with tuberculosis and HIV in Thailand. PLoS ONE, 7(1), e29775.
Machon, M., Larranaga, I., Dorronsoro, M., Vrotsou, K., & Vergara, I. (2017). Health-related quality of life and associated factors in functionally independent older people. BMC geriatrics, 17(1), 19.
Wu, S., Pan, F. (2014). The spss statistical analysis book: Beijing: Tsinghua University Press.
Park, H. (2019). The impact of dyslipidemia on the health-related quality of life of Korean females aged 50 years and older. Iranian Journal of Public Health, 48(3), 556–558.
Chen, C., Liu, G. G., Shi, Q. L., Sun, Y., Zhang, H., Wang, M. J., et al. (2020). Health-related quality of life and associated factors among oldest-old in China. The Journal of Nutrition, Health & Aging, 24(3), 330–338.
Zare, F., Ameri, H., Madadizadeh, F., & Reza, A. M. (2020). Health-related quality of life and its associated factors in patients with type 2 diabetes mellitus. SAGE Open Medicine, 8, 2108037314.
Deng, Q., & Liu, W. (2020). Multilevel analysis of health related quality of life of patients with cardiovascular disease and its determinants. Journal of Shandong University (Health Sciences), 58(07), 115–121.
van Leeuwaarde, R. S., Pieterman, C., May, A. M., Dekkers, O. M., van der Horst-Schrivers, A. N., Hermus, A. R., et al. (2021). Health-related quality of life in patients with multiple endocrine neoplasia Type 1. Neuroendocrinology, 111(3), 288–296.
Rizal, H., Said, M. A., Abdul, M. H., Su, T. T., Maw, P. T., Ismail, R., et al. (2022). Health-related quality of life of younger and older lower-income households in Malaysia. PLoS ONE, 17(2), e263751.
Almasri, D. M., Noor, A. O., Ghoneim, R. H., Bagalagel, A. A., Almetwazi, M., Baghlaf, N. A., et al. (2020). The impact of diabetes mellitus on health-related quality of life in Saudi Arabia. Saudi Pharmaceutical Journal, 28(12), 1514–1519.
Vogl, M., Wenig, C. M., Leidl, R., & Pokhrel, S. (2012). Smoking and health-related quality of life in English general population: Implications for economic evaluations. BMC Public Health, 12, 203.
Miguez, M. C., Lopez-Duran, A., Martinez-Vispo, C., Fernandez, D. R. E., Martinez, U., Rodriguez-Cano, R., et al. (2018). Health-related quality of life among smoking relapsers. Psicothema, 30(1), 27–32.
Schmitz, N., Kruse, J., & Kugler, J. (2003). Disabilities, quality of life, and mental disorders associated with smoking and nicotine dependence. American Journal of Psychiatry, 160(9), 1670–1676.
Weeks, S. G., Glantz, S. A., De Marco, T., Rosen, A. B., & Fleischmann, K. E. (2011). Secondhand smoke exposure and quality of life in patients with heart failure. Archives of internal medicine, 171(21), 1887–1893.
Zhang, X. (2020). Study on the Correlation between TCM Health Literacy and HRQoL of Residents in Jiangxi Province. Jiangxi University of Chinese Medicine.
Dahl, K. G., Wahl, A. K., Urstad, K. H., Falk, R. S., & Andersen, M. H. (2021). Changes in Health Literacy during the first year following a kidney transplantation: Using the Health Literacy Questionnaire. Patient Education and Counseling, 104(7), 1814–1822.
Huang, W., Yu, H., Liu, C., Liu, G., Wu, Q. & Zhou, J., et al. (2017). Assessing Health-Related Quality of Life of Chinese Adults in Heilongjiang Using EQ-5D-3L. International journal of environmental research and public health, 14(3), 224
Romero-Naranjo, F., Espinosa-Uquillas, C., Gordillo-Altamirano, F., & Barrera-Guarderas, F. (2019). Which factors may reduce the health-related quality of life of ecuadorian patients with diabetes? Puerto Rico Health Sciences Journal, 38(2), 102–108.
Lalonde, L., O’Connor, A., Joseph, L., & Grover, S. A. (2004). Health-related quality of life in cardiac patients with dyslipidemia and hypertension. Quality of Life Research, 13(4), 793–804.
Hu, Z., Qin, L., Kaminga, A. C., & Xu, H. (2020). Relationship between multiple lifestyle behaviors and health-related quality of life among elderly individuals with prediabetes in rural communities in China: A STROBE-compliant article. Medicine (Baltimore), 99(15), e19560.
Huang, Y., Chatooah, N. D., Qi, T., Wang, G., Ma, L., Ying, Q., et al. (2018). Health-related quality of life and its associated factors in Chinese middle-aged women. Climacteric, 21(5), 483–490.
Donini, L. M., Rosano, A., Di Lazzaro, L., Lubrano, C., Carbonelli, M., Pinto, A., et al. (2020). Impact of disability, psychological status, and comorbidity on health-related quality of life perceived by subjects with obesity. Obesity Facts, 13(2), 191–200.
Liao, M., Rand, K., Yang, Z., Hsu, C. N., Lin, H. W., & Luo, N. (2023). Censoring in the time trade-off valuation of worse-than-dead EQ-5D-5L health states: Can a time-based willingness-to-accept question be the solution? Quality of Life Research, 32(4), 1165–1174.
Xu, R. H., Dong, D., Luo, N., Wong, E. L., Yang, R., Liu, J., et al. (2022). Mapping the Haem-A-QoL to the EQ-5D-5L in patients with hemophilia. Quality of Life Research, 31(5), 1533–1544.
Winship, C., & Radbill, L. M. (1994). Sampling weights and regression analysis. Sociological Methods & Research, 23, 230–257.
Acknowledgements
We would like to thank our project collaborators of Linyi Center for Disease Control and Prevention for helpful performs the project as a part of the initiative. We acknowledge the National Natural Science Foundation of China for the support of this study. There are no financial relationships or issues to disclose.
Funding
This research was funded by National Natural Science Foundation of China, and Grant Number was 82003456.
Author information
Authors and Affiliations
Contributions
Yage Du wrote the initial draft. Yanhui Lu contributed to study conceptualisation, design and approval. Liuqing Yang contributed to survey implementation. Yu An contributed to manuscript review. Ying Song contributed to data analysis and interpretation. All authors revised and approved the final version.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no potential competing interests.
Ethical approval
The authors declare that all procedures carried out in studies involving human participants were in accordance with the ethical standards of the Biomedical Ethics Committee, Peking University, as well as the 1964 Helsinki Declaration and its subsequent amendments or comparable ethical standards. All procedures involving human participants were approved by the Biomedical Ethics Committee, Peking University (IRB00001052-21131).
Informed consent from participants
Based on inclusion and exclusion criteria, evaluate whether participants were eligible to participate in study. The researchers explained to the subjects the possible risks and requirements during the study, requiring the subjects to sign an informed consent before participating in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Du, Y., Yang, L., An, Y. et al. Health-related quality of life and associated factors in elderly individuals with dyslipidemia in rural Northern China. Qual Life Res 32, 3547–3555 (2023). https://doi.org/10.1007/s11136-023-03489-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-023-03489-9