Abstract
Purpose
To conduct a linguistic and psychometric evaluation of a Chinese version of the Nonrestorative Sleep Scale (NRSS).
Methods
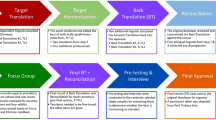
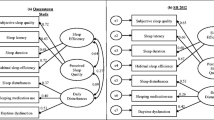
The Chinese NRSS was created from a standard forward–backward translation and trialed on 10 Chinese adults. Telephone interviews were then conducted with 100 adults, who completed the Chinese NRSS, the Pittsburgh Sleep Quality Index (PSQI), the Athens Insomnia Scale (AIS), the Center for Epidemiological Studies Depression Scale (CES-D), and the Toronto Hospital Alertness Test (THAT). A household survey was conducted with 20 subjects, followed by a confirmatory factor analysis (CFA), and a bifactor model was developed to evaluate the reliability and validity of the NRSS.
Results
The bifactor model had the root mean square error of approximation (RMSEA), standardized root mean square residual (SRMR), and comparative fit index (CFI) of 0.06, 0.06, and 0.97, respectively. Convergent validity was shown from the moderate associations with PSQI (r = − 0.66, P < 0.01), AIS (r = − 0.65, P < 0.01), CES-D (r = − 0.54, P < 0.01), and THAT (r = 0.68, P < 0.01). The coefficient omega (0.92), omega hierarchical (0.81), factor determinacy (0.93), H value (0.91), explained common variance (0.63), and percentage of uncontaminated correlations (0.80) derived from the bifactor CFA supported the essential unidimensionality of NRSS.
Conclusions
The Chinese NRSS is a valid and reliable essential unidimensional tool for the assessment of nonrestorative sleep in the Chinese population.


Similar content being viewed by others
References
Stone, K. C., Taylor, D. J., McCrae, C. S., Kalsekar, A., & Lichstein, K. L. (2008). Nonrestorative sleep. Sleep Medicine Reviews, 12(4), 275–288. https://doi.org/10.1016/j.smrv.2007.12.002.
American Psychiatric Association. (1994). Diagnostic and statistical manual of mental disorders (4th ed). Washington, DC: American Psychiatric Association.
Sateia, M. J. (2014). International classification of sleep disorders-third edition: Highlights and modifications. Chest, 146(5), 1387–1394. https://doi.org/10.1378/chest.14-0970.
Sarsour, K., Van Brunt, D. L., Johnston, J. A., Foley, K. A., Morin, C. M., & Walsh, J. K. (2010). Associations of nonrestorative sleep with insomnia, depression, and daytime function. Sleep Medicine, 11(10), 965–972. https://doi.org/10.1016/j.sleep.2010.08.007.
American Psychiatric Association. (2013). Diagnostic and Statistical Manual of Mental Disorders (5th ed). Arlington: American Psychiatric Association.
Roth, T., Jaeger, S., Jin, R., Kalsekar, A., Stang, P. E., & Kessler, R. C. (2006). Sleep problems, comorbid mental disorders, and role functioning in the national comorbidity survey replication. Biological Psychiatry, 60(12), 1364–1371. https://doi.org/10.1016/j.biopsych.2006.05.039.
Ohayon, M. M. (2005). Prevalence and correlates of nonrestorative sleep complaints. Archives of Internal Medicine, 165(1), 35–41. https://doi.org/10.1001/archinte.165.1.35.
Chiu, H. Y., Wang, M. Y., Chang, C. K., Chen, C. M., Chou, K. R., Tsai, J. C., et al. (2014). Early morning awakening and nonrestorative sleep are associated with increased minor non-fatal accidents during work and leisure time. Accident Analysis & Prevention, 71, 10–14. https://doi.org/10.1016/j.aap.2014.05.002.
Kawada, T. (2012). Feeling refreshed by sleep can predict psychological wellbeing assessed using the general health questionnaire in male workers: A 3-year follow-up study. Psychiatry Investigation, 9(4), 418–421. https://doi.org/10.4306/pi.2012.9.4.418.
Liedberg, G. M., Bjork, M., & Borsbo, B. (2015). Self-reported nonrestorative sleep in fibromyalgia: Relationship to impairments of body functions, personal function factors, and quality of life. Journal of Pain Research, 8, 499–505. https://doi.org/10.2147/JPR.S86611.
Park, J. H., Yoo, J. H., & Kim, S. H. (2013). Associations between non-restorative sleep, short sleep duration and suicidality: Findings from a representative sample of Korean adolescents. Psychiatry and Clinical Neurosciences, 67(1), 28–34. https://doi.org/10.1111/j.1440-1819.2012.02394.x.
Okamoto, M., Kobayashi, Y., Nakamura, F., & Musha, T. (2017). Association between nonrestorative sleep and risk of diabetes: A cross-sectional study. Behavioural Sleep Medicine, 15(6), 483–490. https://doi.org/10.1080/15402002.2016.1163701.
Zhang, J., Lam, S. P., Li, S. X., Li, A. M., & Wing, Y. K. (2012). The longitudinal course and impact of non-restorative sleep: A five-year community-based follow-up study. Sleep Medicine, 13(6), 570–576. https://doi.org/10.1016/j.sleep.2011.12.012.
Mariman, A. N., Vogelaers, D. P., Tobback, E., Delesie, L. M., Hanoulle, I. P., & Pevernagie, D. A. (2013). Sleep in the chronic fatigue syndrome. Sleep Medicine Reviews, 17(3), 193–199. https://doi.org/10.1016/j.smrv.2012.06.003.
Vernon, M. K., Dugar, A., Revicki, D., Treglia, M., & Buysse, D. (2010). Measurement of non-restorative sleep in insomnia: A review of the literature. Sleep Medicine Reviews, 14(3), 205–212. https://doi.org/10.1016/j.smrv.2009.10.002.
Wilkinson, K., & Shapiro, C. (2012). Nonrestorative sleep: symptom or unique diagnostic entity? Sleep Medicine, 13(6), 561–569. https://doi.org/10.1016/j.sleep.2012.02.002.
Wilkinson, K., & Shapiro, C. (2013). Development and validation of the Nonrestorative Sleep Scale (NRSS). Journal of Clinical Sleep Medicine, 9(9), 929–937. https://doi.org/10.5664/jcsm.2996.
National Sleep Foundation. (2010). Sleep differences among ethnic groups revealed in new poll. ScienceDaily. Retrieved March 27, 2010 from https://www.sciencedaily.com/releases/2010/03/100308081740.htm.
Chen, X., Wang, R., Zee, P., Lutsey, P. L., Javaheri, S., Alcantara, C., et al. (2015). Racial/ethnic differences in sleep disturbances: The multi-ethnic study of atherosclerosis (MESA). Sleep, 38(6), 877–888. https://doi.org/10.5665/sleep.4732.
Anthoine, E., Moret, L., Regnault, A., Sebille, V., & Hardouin, J. B. (2014). Sample size used to validate a scale: A review of publications on newly-developed patient reported outcomes measures. Health and Quality Life Outcomes, 12, 176. https://doi.org/10.1186/s12955-014-0176-2.
Tsang, S., Royse, C. F., & Terkawi, A. S. (2017). Guidelines for developing, translating, and validating a questionnaire in perioperative and pain medicine. Saudi Journal of Anaesthesia, 11(Suppl 1), S80–S89. https://doi.org/10.4103/sja.SJA_203_17.
Chong, A. M. L., & Cheung, C.-K. (2012). Factor structure of a Cantonese-version pittsburgh sleep quality index. Sleep and Biological Rhythms, 10(2), 118–125. https://doi.org/10.1111/j.1479-8425.2011.00532.x.
Chung, K. F., Kan, K. K., & Yeung, W. F. (2011). Assessing insomnia in adolescents: Comparison of Insomnia Severity Index, Athens Insomnia Scale and Sleep Quality Index. Sleep Medicine, 12(5), 463–470. https://doi.org/10.1016/j.sleep.2010.09.019.
Soldatos, C. R., Dikeos, D. G., & Paparrigopoulos, T. J. (2000). Athens Insomnia Scale: Validation of an instrument based on ICD-10 criteria. Journal of Psychosomatic Research, 48(6), 555–560. https://doi.org/10.1016/S0022-3999(00)00095-7.
Chin, W. Y., Choi, E. P., Chan, K. T., & Wong, C. K. (2015). The psychometric properties of the center for epidemiologic studies depression scale in Chinese primary care patients: factor structure, construct validity, reliability, sensitivity and responsiveness. PLoS ONE, 10(8), e0135131. https://doi.org/10.1371/journal.pone.0135131.
Vilagut, G., Forero, C. G., Barbaglia, G., & Alonso, J. (2016). Screening for depression in the general population with the center for epidemiologic studies depression (CES-D): A systematic review with meta-analysis. PLoS ONE, 11(5), e0155431. https://doi.org/10.1371/journal.pone.0155431.
Shapiro, C. M., Auch, C., Reimer, M., Kayumov, L., Heslegrave, R., Huterer, N., et al. (2006). A new approach to the construct of alertness. Journal of Psychosomatic Research, 60(6), 595–603. https://doi.org/10.1016/j.jpsychores.2006.04.012.
Terwee, C. B., Bot, S. D., de Boer, M. R., et al. (2007). Quality criteria were proposed for measurement properties of health status questionnaires. Journal of Clinical Epidemiology, 60(1), 34–42. https://doi.org/10.1016/j.jclinepi.2006.03.012.
Anastasios, S., Theodoros, A. K., Vasiliki, Y., & Konstantina, P. (2018). Using bifactor EFA, bifactor CFA and exploratory structural equation modeling to validate factor structure of the meaning in life questionnaire, Greek version. Psychology, 9(3), 348–371. https://doi.org/10.4236/psych.2018.93022.
Fong, D. Y., Lam, C. L., Mak, K. K., Lo, W. S., Lai, Y. K., Ho, S. Y., et al. (2010). The Short Form-12 Health Survey was a valid instrument in Chinese adolescents. Journal of Clinical Epidemiology, 63(9), 1020–1029. https://doi.org/10.1016/j.jclinepi.2009.11.011.
Hu, L. T., & Bentler, P. M. (1999). Cutoff criteria for fit indexes in covariance structure analysis: Conventional criteria versus new alternatives. Structural Equation Modeling: A Multidisciplinary Journal, 6(1), 1–55. https://doi.org/10.1080/10705519909540118.
Rodriguez, A., Reise, S. P., & Haviland, M. G. (2016). Applying bifactor statistical indices in the evaluation of psychological measures. Journal of Personality Assessment, 98(3), 223–237. https://doi.org/10.1080/00223891.2015.1089249.
Gu, H. L., Wen, Z. L., & Fan, X. T. (2017). Structural validity of the Machiavellian Personality Scale: A bifactor exploratory structural equation modeling approach. Personality and Individual Differences, 105, 116–123. https://doi.org/10.1016/j.paid.2016.09.042.
Rosseel, Y., Oberski, D., Vanbrabant, L., Vanbrabant, L., Savalei, V., Merkle, E., et al.(2012). Package ‘lavaan’. R package version 0.6-3. Retrieved from https://cran.r-project.org/web/packages/lavaan/lavaan.pdf.
Dueber, D. M. (2017). Bifactor Indices Calculator: A Microsoft Excel-based tool to calculate various indices relevant to bifactor CFA models. https://doi.org/10.13023/edp.tool.01. Retrieved from http://sites.education.uky.edu/apslab/resources/.
2016 Population By-census Office Census and Statistics Department. (2017). 2016 Population By-census-Main Results. Hong Kong, HKSAR: Website of the Census and Statistics Department, 2017. Retrieved from https://www.bycensus2016.gov.hk/data/16bc-main-results.pdf.
Nunnally, J. N. (1978). Psychometric Theory (2nd edn.). New York: McGraw-Hill.
Wilkinson, K. (2012). The Psychometric Properties of the Nonrestorative Sleep Scale and a Prospective Observational Study of the Physiological Correlates of Nonrestorative Sleep. University of Toronto. Retrieved from https://tspace.library.utoronto.ca/bitstream/ 1807/32639/6/Wilkinson_Caitlin_20126_MSc_thesis.pdf.
Acknowledgements
Miss Tiffany Kwok and Mr Cecil Wong, respectively, conducted the forward and backward translations, and are gratefully acknowledged.
Funding
This study was financially supported by a Seed Funding for Basic Research Grant (201511159061) from The University of Hong Kong.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Li, S., Fong, D.Y.T., Wong, J.Y.H. et al. Nonrestorative sleep scale: reliable and valid for the Chinese population. Qual Life Res 28, 1685–1692 (2019). https://doi.org/10.1007/s11136-019-02134-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-019-02134-8