Abstract
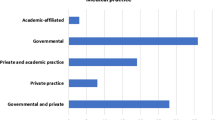
Pituitary surgery involves operating in the nasal cavity, which is considered a clean-contaminated wound. In the absence of evidence-based guidelines for preventing surgical site infections in trans-sphenoidal surgery, a survey of current opinion on prophylactic antibiotics might help elucidate the current acceptable practices and identify opportunities for prospective clinical trials that could lead to the development of practice guidelines. An on-line, 10-question, multiple-choice survey was distributed by e-mail link to the membership of the International Society of Pituitary Surgeons. Sixty-nine members responded to the survey. Ninety-one percent indicated that there was no strong evidence supporting antibiotic use, but 81% used them to be safe. Ninety percent of respondents used intravenous prophylactic antibiotics, while only 16% used intranasal antibiotics. The most commonly used antibiotics were cephalosporins (72%) and penicillins (21%). Seventy-six percent used antibiotics for 24 h or less after surgery. The most commonly reported indications for prophylactic antibiotics were prevention of meningitis and sinusitis. The results of the survey describe current acceptable practices for chemoprophylaxis in patients undergoing transsphenoidal pituitary surgery.


Similar content being viewed by others
References
Brown SM, Anand VK, Tabaee A, Schwartz TH (2007) Role of perioperative antibiotics in endoscopic skull base surgery. Laryngoscope 117:1528–1532
Ciric I, Ragin A, Baumgartner C, Pierce D (1997) Complications of transsphenoidal surgery: results of a national survey, review of the literature, and personal experience. Neurosurgery 40:225–236
Kelly DF (2007) Commentary: retrospective analysis of a new antibiotic chemoprophylaxis regimen in 170 patients undergoing endoscopic endonasal transsphenoidal surgery. Surg Neurol 68:148
Korinek AM, Baugnon T, Golmard JL, van Effenterre R, Coriat P, Puybasset L (2008) Risk factors for adult nosocomial meningitis after craniotomy: role of antibiotic prophylaxis. Neurosurgery 62(Suppl 2):532–539
Korinek AM, Golmard JL, Elcheick A, Bismuth R, van Effenterre R, Coriat P, Puybasset L (2005) Risk factors for neurosurgical site infections after craniotomy: a critical reappraisal of antibiotic prophylaxis on 4,578 patients. Br J Neurosurg 19:155–162
Mangram AJ, Horan TC, Pearson ML, Silver LC, Jarvis WR (1999) Guidelines for the prevention of surgical site infection. Centers for Disease Control and Prevention, U.S. Department of Health and Human Services, USA
Nelson RL, Gelnny AM, Song F (2010) Antimicrobial prophylaxis for colorectal surgery. The Cochrane Database of Systematic Reviews, Oxford
Orlando R, Cappabianca P, Tosone G, Esposito F, Piazza M, de Divitiis E (2007) Retrospective analysis of a new antibiotic chemoprophylaxis regimen in 170 patients undergoing endoscopic endonasal transsphenoidal surgery. Surg Neurol 68:145–148
Ratilal BO, Costa J, Sampaio C (2006) Antibiotic prophylaxis for preventing meningitis in patients with basilar skull base fractures. The Cochrane Database of Systematic Reviews, Oxford
Smaill FM, Gyte GML (2010) Antibiotic prophylaxis versus no prophylaxis for preventing infection after cesarean section. The Cochrane Database of Systematic Reviews, Oxford
Verschuur HP, Wever W, van Benthem PP (2004) Antibiotic prophylaxis in clean and clean-contaminated ear surgery. The Cochrane Database of Systematic Reviews, Oxford
Acknowledgments
The authors thank the staff of the Neurosciences Publications Office of Barrow Neurological Institute for assistance with manuscript preparation. The authors also thank Nelson Oyesiku, MD, for permission to survey the ISPS membership.
Disclosures
The authors report no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Little, A.S., White, W.L. Prophylactic antibiotic trends in transsphenoidal surgery for pituitary lesions. Pituitary 14, 99–104 (2011). https://doi.org/10.1007/s11102-010-0256-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11102-010-0256-1