Abstract
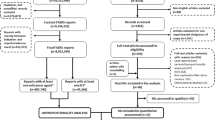
Background Although immune-related adverse events (irAEs) have been reported in patients receiving immune checkpoint inhibitor (ICI) therapy, sex differences in irAEs are not known. Aim The present study described, evaluated and compared differences in irAEs between females and males treated with ICIs. Method irAE reports were obtained from the FDA Adverse Event Reporting System (FAERS) from January 2004 to December 2020. Disproportionality analysis and Bayesian analysis were used to explore differences in irAEs between females and males. The onset time and fatality proportion of irAEs in different ICIs between females and males were further evaluated. Results A total of 30,342 irAE cases were obtained, including 11,097 female cases and 19,245 male cases. Consistent disproportionality signals were detected in females and males, including endocrine toxicity, hepatitis, lung toxicity, nervous system toxicity, and ocular toxicity. Renal toxicity was only detected in male patients receiving ICI therapy (PRR 2.37, 95% CI: 2.25–2.51; IC: 1.24, 95% CI: 1.05–1.43). Males had a longer onset time (females 35 days [IQR 14–87] vs. males 39 days [IQR 14–92], P = 0.041) and higher fatality proportion (females 20.5% vs. males 25.6%, P < 0.01). Conclusion This analysis revealed that males had a higher chance of exhibiting ICI-associated renal toxicity, longer median onset time and worse prognosis of irAEs than females. Greater attention to sex differences in ICI therapy is needed.



Similar content being viewed by others
References
Klein SL, Flanagan KL. Sex differences in immune responses. Nat Rev Immunol. 2016;16(10):626–38.
Triggianese P, Novelli L, Galdiero MR, et al. Immune checkpoint inhibitors-induced autoimmunity: The impact of gender. Autoimmun Rev. 2020; 19(8).
Fish EN. The X-files in immunity: sex-based differences predispose immune responses. Nat Rev Immunol. 2008;8(9):737–44.
Oertelt-Prigione S. The influence of sex and gender on the immune response. Autoimmun Rev. 2012;11(6–7):A479–85.
Roberts CW, Walker W, Alexander J. Sex-associated hormones and immunity to protozoan parasites. Clin Microbiol Rev. 2001;14(3):476-+.
Conforti F, Pala L, Bagnardi V, et al. Cancer immunotherapy efficacy and patients’ sex: a systematic review and meta-analysis. Lancet Oncol. 2018;19(6):737–46.
Wallis CJD, Butaney M, Satkunasivam R, et al. Association of Patient Sex With Efficacy of Immune Checkpoint Inhibitors and Overall Survival in Advanced Cancers A Systematic Review and Meta-analysis. JAMA Oncol. 2019;5(4):529–36.
Conforti F, Pala L, Bagnardi V, et al. Sex-Based Heterogeneity in Response to Lung Cancer Immunotherapy: A Systematic Review and Meta-Analysis. J Natl Cancer Inst. 2019;111(8):772–81.
Wang S, Cowley LA, Liu X-S. Sex Differences in Cancer Immunotherapy Efficacy, Biomarkers, and Therapeutic Strategy. J Natl Cancer Inst Molecules. 2019; 24(18).
Duma N, Abdel-Ghani A, Yadav S, et al. Sex Differences in Tolerability to Anti-Programmed Cell Death Protein 1 Therapy in Patients with Metastatic Melanoma and Non-Small Cell Lung Cancer: Are We All Equal? Oncologist. 2019;24(11):E1148–55.
Chen C, Wu B, Zhang C, et al. Immune-related adverse events associated with immune checkpoint inhibitors: An updated comprehensive disproportionality analysis of the FDA adverse event reporting system. Int Immunopharmacol. 2021; 95.
Raschi E, Gatti M, Gelsomino F, et al. Lessons to be Learnt from Real-World Studies on Immune-Related Adverse Events with Checkpoint Inhibitors: A Clinical Perspective from Pharmacovigilance. Target Oncol. 2020;15(4):449–66.
Ye X, Hu F, Zhai Y, et al. Hematological toxicities in immune checkpoint inhibitors: A pharmacovigilance study from 2014 to 2019. Hematol Oncol. 2020;38(4):565–75.
Thi Thu Ha N, Roussin A, Rousseau V, et al. Role of Serotonin Transporter in Antidepressant-Induced Diabetes Mellitus: A Pharmacoepidemiological-Pharmacodynamic Study in VigiBase((R)). Drug Saf. 2018;41(11):1087–96.
Polanczyk MJ, Hopke C, Vandenbark AA, et al. Estrogen-mediated immunomodulation involves reduced activation of effector T cells, potentiation of Treg cells, and enhanced expression of the PD-1 costimulatory pathway. J Neurosci Res. 2006;84(2):370–8.
Polanczyk MJ, Hopke C, Vandenbark AA, et al. Treg suppressive activity involves estrogen-dependent expression of programmed death-1 (PD-1). Int Immunol. 2007;19(3):337–43.
Carrero JJ, Hecking M, Chesnaye NC, et al. Sex and gender disparities in the epidemiology and outcomes of chronic kidney disease. Nat Rev Nephrol. 2018;14(3):151–64.
Hu R, Chen M, Xu Y, et al. Renal immune-related adverse events of immune checkpoint inhibitor. Asia Pac J Clin Oncol. 2020;16(6):305–11.
Nishimura H, Nose M, Hiai H, et al. Development of lupus-like autoimmune diseases by disruption of the PD-1 gene encoding an ITIM motif-carrying immunoreceptor. Immunity. 1999;11(2):141–51.
Waeckerle-Men Y, Starke A, Wuethrich RP. PD-L1 partially protects renal tubular epithelial cells from the attack of CD8(+)cytotoxic T cells. Nephrol Dial Transplant. 2007;22(6):1527–36.
Tivol EA, Borriello F, Schweitzer AN, et al LOSS OF CTLA-4 leads to massive lymphoproliferation and fatal multiorgan tissue destruction, revealing a critical negative regulatory role of CTLA-4. Immunity. 1995;3(5):541–7.
Riella LV, Paterson AM, Sharpe AH, et al. Role of the PD-1 Pathway in the Immune Response. Am J Transplant. 2012;12(10):2575–87.
Jaworska K, Ratajczak J, Huang L, et al. Both PD-1 Ligands Protect the Kidney from Ischemia Reperfusion Injury. J Immunol. 2015;194(1):325–33.
Pardoll DM. The blockade of immune checkpoints in cancer immunotherapy. Nat Rev Cancer. 2012;12(4):252–64.
Buchbinder EI, Desai A. CTLA-4 and PD-1 Pathways Similarities, Differences, and Implications of Their Inhibition. Am J Clin Oncol-Canc. 2016;39(1):98–106.
Reck M, Rodriguez-Abreu D, Robinson AG, et al. Pembrolizumab versus Chemotherapy for PD-L1-Positive Non-Small-Cell Lung Cancer. N Engl J Med. 2016;375(19):1823–33.
Borghaei H, Paz-Ares L, Horn L, et al. Nivolumab versus Docetaxel in Advanced Nonsquamous Non-Small-Cell Lung Cancer. N Engl J Med. 2015;373(17):1627–39.
Robert C, Thomas L, Bondarenko I, et al. Ipilimumab plus Dacarbazine for Previously Untreated Metastatic Melanoma. N Engl J Med. 2011;364(26):2517–26.
Lai L-T, Gu W-G, Hu M-B, et al. Sex-related differences in the efficacy of immune checkpoint inhibitors in malignancy: a systematic review and meta-analysis. Aging-Us. 2021;13(11):15413–32.
Botticelli A, Onesti CE, Zizzari I, et al. The sexist behaviour of immune checkpoint inhibitors in cancer therapy? Oncotarget. 2017;8(59):99336–46.
Schulz GB, Rodler S, Szabados B, et al. Safety, efficacy and prognostic impact of immune checkpoint inhibitors in older patients with genitourinary cancers. J Geriatr Oncol. 2020;11(7):1061–6.
Corbaux P, Maillet D, Boespflug A, et al. Older and younger patients treated with immune checkpoint inhibitors have similar outcomes in real-life setting. Eur J Cancer. 2019;121:192–201.
Elias R, Hartshorn K, Rahma O, et al. Aging, immune senescence, and immunotherapy: A comprehensive review. Semin Oncol. 2018;45(4):187–200.
Cortazar FB, Marrone KA, Troxell ML, et al. Clinicopathological features of acute kidney injury associated with immune checkpoint inhibitors. Kidney Int. 2016;90(3):638–47.
Wanchoo R, Karam S, Uppal NN, et al. Adverse Renal Effects of Immune Checkpoint Inhibitors: A Narrative Review. Am J Nephrol. 2017;45(2):160–9.
Sise ME, Seethapathy H, Reynolds KL. Diagnosis and Management of Immune Checkpoint Inhibitor-Associated Renal Toxicity: Illustrative Case and Review. Oncologist. 2019;24(6):735–42.
Zheng K, Qiu W, Wang H, et al. Clinical recommendations on diagnosis and treatment of immune checkpoint inhibitor-induced renal immune-related adverse events. Thorac Cancer. 2020;11(6):1746–51.
Kumar V, Chaudhary N, Garg M, et al. Current Diagnosis and Management of Immune Related Adverse Events (irAEs) Induced by Immune Checkpoint Inhibitor Therapy. Front Pharmacol. 2017; 8.
Chen G, Qin Y, Fan Q-Q, et al. Renal adverse effects following the use of different immune checkpoint inhibitor regimens: A real-world pharmacoepidemiology study of post-marketing surveillance data. Cancer Med. 2020;9(18):6576–85.
Sakaeda T, Tamon A, Kadoyama K, et al. Data Mining of the Public Version of the FDA Adverse Event Reporting System. Int J Med Sci. 2013;10(7):796–803.
Acknowledgements
Not applicable.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Funding
This study was supported by the National Key Research and Development Program of China (NO: 2020YFC2008302).
Conflicts of interest
The authors declare that they had no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Chen, C., Zhang, C., Jin, Z. et al. Sex differences in immune-related adverse events with immune checkpoint inhibitors: data mining of the FDA adverse event reporting system. Int J Clin Pharm 44, 689–697 (2022). https://doi.org/10.1007/s11096-022-01395-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11096-022-01395-7