Abstract
Purpose
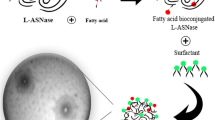
Mucopolysaccharidosis I is a genetic disorder caused by alpha-L-iduronidase deficiency. Its primary treatment is enzyme replacement therapy (ERT), which has limitations such as a high cost and a need for repeated infusions over the patient's lifetime. Considering that nanotechnological approaches may enhance enzyme delivery to organs and can reduce the dosage thereby enhancing ERT efficiency and/or reducing its cost, we synthesized laronidase surface-functionalized lipid-core nanocapsules (L-MLNC).
Methods
L-MLNCs were synthesized by using a metal complex. Size distributions were evaluated by laser diffraction and dynamic light scattering. The kinetic properties, cytotoxicity, cell uptake mechanisms, clearance profile and biodistribution were evaluated.
Results
Size distributions showed a D[4,3] of 134 nm and a z-average diameter of 71 nm. L-MLNC enhanced the Vmax and Kcat in comparison with laronidase. L-MLNC is not cytotoxic, and nanocapsule uptake by active transport is not only mediated by mannose-6-phosphate receptors. The clearance profile is better for L-MLNC than for laronidase. A biodistribution analysis showed enhanced enzyme activity in different organs within 4 h and 24 h for L-MLNC.
Conclusions
The use of lipid-core nanocapsules as building blocks to synthesize surface-functionalized nanocapsules represents a new platform for producing decorated soft nanoparticles that are able to modify drug biodistribution.






Similar content being viewed by others
Abbreviations
- BS:
-
Backscattering
- CNS:
-
Central Nervous System
- ERT:
-
Enzyme Replacement Therapy
- IDUA:
-
Alpha-L-iduronidase
- L1-MLNC1 :
-
Multiple-wall nanocapsule with 0.05% chitosan and 11 μg/mL of laronidase
- L1-MLNC2 :
-
Multiple-wall nanocapsule with 0.075% chitosan and 11 μg/mL of laronidase
- L2-MLNC1 :
-
Multiple-wall nanocapsule with 0.05% chitosan and 96 μg/mL of laronidase
- L2-MLNC2 :
-
Multiple-wall nanocapsule with 0.075% chitosan and 96 μg/mL of laronidase
- L-MLNC:
-
Laronidase surface-functionalized lipid-core nanocapsules
- LNC:
-
Lipid core nanocapsules
- LNC-CS0.03 :
-
LNC coated with 0.03% (w/v) chitosan
- LNC-CS0.05 :
-
LNC coated with 0.05% (w/v) chitosan
- LNC-CS0.075 :
-
LNC coated with 0.075% (w/v) chitosan
- MPS I:
-
Mucopolysaccharidosis type I
- MTT:
-
3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyl tetrazolium bromide
- PCS:
-
Photon Correlation Spectroscopy
- PDI:
-
Polydispersity Index
- T:
-
Transmission
- ∆BS:
-
Relative Backscattering
References
Tan ML, Choong PF, Dass CR. Recent developments in liposomes, microparticles and nanoparticles for protein and peptide drug delivery. Peptides. 2010;31(1):184–93.
Carino GP, Jacob JS, Mathiowitz E. Nanosphere based oral insulin delivery. J Control Release. 2000;65(1–2):261–9.
Torchilin VP. Drug targeting. Eur J Pharm Sci. 2000;11 Suppl 2:S81–91.
Caruthers SD, Wickline SA, Lanza GM. Nanotechnological applications in medicine. Curr Opin Biotechnol. 2007;18(1):26–30.
Kreuter J. Nanoparticulate systems for brain delivery of drugs. Adv Drug Deliv Ver. 2001;47(1):65–81.
Di Marco M, Shamsuddin S, Razak KA, et al. Overview of the main methods used to combine proteins with nanosystems: absorption, bioconjugation, and encapsulation. Int J Nanomedicine. 2010;5:37–49.
Jonkheijn P, Weinrich D, Schröder H, Niemeyer CM, Waldmann H. Chemical strategies for generating protein biochips. Angew Chem Int Ed Engl. 2008;47(50):9618–47.
Rana S, Yeh YC, Rotello VM. Engineering the nanoparticle–protein interface: applications and possibilities. Curr Opin Chem Biol. 2010;14(6):828–34.
Jager E, Venturini CG, Poletto FS, et al. Sustained release from lipid-core nanocapsules by varying the core viscosity and the particle surface area. J Biomed Nanotechnol. 2009;5(1):130–40.
Venturini CG, Jäger E, Oliveira CP, et al. Formulation of lipid core nanocapsules. Colloids and Surf A: Physicochem Eng Aspects. 2011;375:200–8.
Jornada DS, Fiel LA, Bueno K, et al. Lipid-core nanocapsules: mechanism of self-assembly, control of size and loading capacity. Soft Matter. 2012;8:6646–55.
Fiel LA, Rebelo LM, Santiago TM, et al. Diverse deformation properties of polymeric nanocapsules and lipid-core nanocapsules. Soft Matter. 2011;7:7240–7.
Bernardi A, Frozza RL, Horn AP, et al. Protective effects of indomethacin-loaded nanocapsules against oxygen-glucose deprivation in organotypic hippocampal slice cultures: involvement of neuroinflammation. Neurochem Int. 2010;57(6):629–36.
Bernardi A, Zilberstein AC, Jager E, et al. Effects of indomethacin-loaded nanocapsules in experimental models of inflammation in rats. Br J Pharmacol. 2009;158(4):1104–11.
Bernardi A, Braganhol E, Jager E, et al. Indomethacin-loaded nanocapsules treatment reduces in vivo glioblastoma growth in a rat glioma model. Cancer Lett. 2009;281(1):53–63.
Ourique AF, Azoubel S, Ferreira CV, et al. Lipid-core nanocapsules as a nanomedicine for parenteral administration of tretinoin: development and in vitro antitumor activity on human myeloid leukaemia cells. J Biomed Nanotechnol. 2010;6(3):214–23.
Frozza RL, Bernardi A, Paese K, et al. Characterization of trans-resveratrol-loaded lipid-core nanocapsules and tissue distribution studies in rats. J Biomed Nanotechnol. 2010;6(6):3694–703.
Bender EA, Adorne MD, Colome LM, et al. Hemocompatibility of poly(epsilon-caprolactone) lipid-core nanocapsules stabilized with polysorbate 80-lecithin and uncoated or coated with chitosan. Int J Pharm. 2012;426(1–2):271–9.
Bender EA, Cavalcante MF, Adorne MD, et al. New strategy to surface functionalization of polymeric nanoparticles: one-pot synthesis of scFv anti-LDL(-)-functionalized nanocapsules. Res: Pharm; 2014. doi:10.1007/s11095-014-1392-5.
Reynaud F, Tsapis N, Deyme M, et al. Spray-dried chitosan-metal microparticles for ciprofloxacin adsorption: Kinetic and equilibrium studies. Soft Matter. 2011;7:7304–12.
Neufeld EF, Muenzer J. The Mucopolysaccharidosis. In: Scriver CR, Beaudet AL, Sly WS, Valle D, editors. The Metabolic and Molecular Bases of Inherited Disease. New York: McGraw-Hill; 2001. p. 3421–52.
Giugliani R, Ferderhen A, Carvalho CG, Artigalas O. Enzyme replacement therapy for Mucopolysaccharidosis type I: Laronidase. Pediatr Health. 2010;4:133–45.
Souza MV, Krug BC, Picon P, Schwartz IVD. Medicamentos de alto custo para doenças raras no Brasil: o exemplo das doenças lisossômicas. Ciência e Saúde Coletiva. 2010;15(3):3443–554.
Giugliani R, Federhen A, Muñoz Rojas MV, et al. Enzyme replacement therapy for mucopolysaccharidoses I, II and VI: recommendations from a group of Brazilian F experts. Rev Assoc Med Bras. 2010;56(3):271–7.
Mengual O, Meunier G, Cayre I, Puech K, Snabre P. TURBISCAN MA 2000: multiple light scattering measurement for concentrated emulsion and suspension instability analysis. Talanta. 1999;50(2):445–56.
Mosmann T. Rapid colorimetric assay for cellular growth and survival: application to proliferation and cytotoxicity assays. J Immunol Methods. 1983;65:55–63.
Hopwood JJ, Muller V, Smithson A, Baggett N. A fluorometric assay using 4-methylumbelliferyl alpha-L-iduronide for the estimation of alpha-L-iduronidase activity and the detection of Hurler and Scheie syndromes. Clin Chim Acta. 1979;92(2):257–65.
Lowry OH, Rosebrough NJ, Farr AL, Randall RJ. Protein measurement with the Folin phenol reagent. J Biol Chem. 1951;193(1):265–75.
The European Commission, 2011/696/EU, Official Journal of the European Union, ISSN 1977-0677. 2011;54:L275.
Siqueira NM, Contri RV, Paese K, et al. Innovative sunscreen formulation based on benzophenone-3-loaded chitosan-coated polymeric nanocapsules. Skin Pharmacol Physiol. 2011;24(3):166–74.
Nelson DL, Cox MM. Enzimas. In: Nelson DL, Cox MM, editors. Princípios de bioquímica de Lehninger. São Paulo: Sarvier; 2006. p. 202–12.
Celia C, Trapasso E, Cosco D, Paolino D, Fresta M. Turbiscan lab expert analysis of the stability of ethosomes and ultradeformable liposomes containing a bilayer fluidizing agent. Colloids Surf B: Biointerfaces. 2009;72(1):155–60.
Ipe BI, Niemeyer CM. Nanohybrids composed of quantum dots and cytochrome P450 as photocatalysts. Angew Chem Int Ed Engl. 2006;45(3):504–7.
de Graaf AJ, Kooijman M, Hennink WE, Mastrobattista E. Nonnatural amino acids for site-specific protein conjugation. Bioconjug Chem. 2009;20(7):1281–95.
Hong R, Fischer NO, Verma A, et al. Control of protein structure and function through surface recognition by tailored nanoparticle scaffolds. J Am Chem Soc. 2004;126(3):739–43.
Abad JM, Mertens SF, Pita M, Fernandez VM, Schiffrin DJ. Functionalization of thioctic acid-capped gold nanoparticles for specific immobilization of histidine-tagged proteins. J Am Chem Soc. 2005;127(15):5689–94.
Rempel BP, Clarke LA, Withers SG. A homology model for human alpha-l-iduronidase: insights into human disease. Mol Genet Metab. 2005;85(1):28–37.
Goldberg M, Langer R, Jia X. Nanostructured materials for applications in drug delivery and tissue engineering. J Biomater Sci Polym Ed. 2007;18(3):241–68.
Giugliani R, Rojas VM, Martins AM, et al. A dose-optimization trial of laronidase (Aldurazyme) in patients with mucopolysaccharidosis I. Mol Genet Metab. 2009;96(1):13–9.
Garnacho C, Dhami R, Simone E, et al. Delivery of acid sphingomyelinase in normal and niemann-pick disease mice using intercellular adhesion molecule-1-targeted polymer nanocarriers. J Pharmacol Exp Ther. 2008;325(2):400–8.
Hsu J, Serrano D, Bhowmick T, et al. Enhanced endothelial delivery and biochemical effects of α-galactosidase by ICAM-1-targeted nanocarriers for Fabry disease. J Control Release. 2011;149:323–31.
ACKNOWLEDGMENTS AND DISCLOSURES
The authors are grateful for the financial support of the Fundo de Incentivo à Pesquisa (FIPE-HCPA), PRONEX and PRONEM FAPERGS/CNPq, INCT-if CNPq, Universal CNPq, FAPERGS and Rede Nanobiotec CAPES. The sponsors had no involvement in the study design, data collection, analysis, interpretation, writing and decision to publish the data.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Fabiana Quoos Mayer and Márcia Duarte Adorne contributed equally to this study
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
Supplementary figure 1
Particle size distribution profiles (μm) by laser diffraction (Mastersizer 2000, Malvern): (A) LNC-CS0.03; (B) LNC-CS0.05 and (C) LNC-CS0.075. (JPEG 73 kb)
Supplementary figure 2
Relative backscattering profiles of multiple wall nanocapsules over 24 h. A. L1-MLNC1 and B. L2-MLNC2. Only one profile of each suspension is shown. Both formulations showed the same profile. No significant changes were observed in the BS signal at the center of the cuvette. (JPEG 34 kb)
Supplementary figure 3
A cytotoxicity analysis of laronidase, L1-MLNC1 and LNC-CS0.05. Laronidase caused no cytotoxicity at any of the tested concentrations. L1-MLNC1 and LNC-CS0.05 caused approximately 30% cell death at higher concentrations and 90-100% cell viability was reached at concentrations lower than 0.0232 μg/mL. (GIF 55 kb)
Supplementary figure 4
Enzyme uptake by the MPS I patient’s fibroblasts. Laronidase and L1-MLNC1 could be internalized, restoring enzyme activity to the MPS I patient’s fibroblasts. *p < 0.01 compared with Control group, ANOVA with Tukey’s post hoc test. (GIF 21 kb)
Rights and permissions
About this article
Cite this article
Mayer, F.Q., Adorne, M.D., Bender, E.A. et al. Laronidase-Functionalized Multiple-Wall Lipid-Core Nanocapsules: Promising Formulation for a More Effective Treatment of Mucopolysaccharidosis Type I. Pharm Res 32, 941–954 (2015). https://doi.org/10.1007/s11095-014-1508-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-014-1508-y