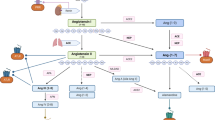
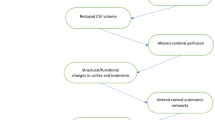
Changes in the osmolality and level of angiotensin II (ANG II) are important peripheral signals modulating appropriate central sympathetic output and maintaining normal arterial pressure during high salt intake. The median preoptic nucleus (MnPO) receives reciprocal inputs from the subfornical organ (SFO) and organum vasculosum of the lamina terminalis (OVLT), the circumventricular organs that have been shown to be necessary in multiple central effects of changes in the osmolality and circulating ANG II directed toward the maintenance of sodium and water homeostasis. We, therefore, hypothesized that the MnPO is a crucial part of the central neuronal mechanisms mediating the blood pressure control by altered osmolality and/or ANG II signaling during chronic high dietary salt intake. Male Sprague–Dawley rats were randomly assigned to either sham (operation) or electrolytic lesion of the MnPO. After a 7-day recovery, rats were instrumented with radiotelemetric transducers and aortic flow probes for measurement of the mean arterial pressure (MAP) + heart rate (HR) and cardiac output (CO), respectively. Femoral venous catheters were also implanted to collect blood for the measurements of plasma osmolality and sodium concentration, as well as plasma renin activity. Rats were given another 10 days to recover and then were subjected to a 28-day-long study protocol that included a 7-day control period (1.0% NaCl diet) followed by 14 days of high salt (4.0% NaCl), and a 7-day recovery period (1.0% NaCl). The data showed, that despite a slight increase in the MAP observed in both MnPO-(n = 12) and sham-lesioned (n = 8) rats during the high-salt period, there were no significant differences between the MAP, HR, and CO in the two groups throughout the study protocol. These findings do not support the hypothesis that the MnPO is necessary to maintain the normal blood pressure during high dietary salt intake. However, MnPO-lesioned rats showed less sodium balance than sham-lesioned rats during the first 4 days of high salt intake. Although these results may be explained partly by the plasma hyperosmolarity and hypernatremia observed in MnPO-lesioned rats, they also shed light on the role of the MnPO in central neuronal control of renal sodium handling during chronic high dietary salt intake.
Similar content being viewed by others
References
V. L. Brooks and J. W. Osborn, “Hormonal-sympathetic interactions in long-term regulation of arterial pressure: An hypothesis,” Am. J. Physiol., 268, R1343–R1358 (1995).
V. L. Brooks, K. E. Scrogin, and D. F. McKeogh, “The interaction of angiotensin II and osmolality in the generation of sympathetic tone during changes in dietary salt intake. An hypothesis,” Ann. New York Acad. Sci., 940, 380–394 (2001).
F. C. Luft, L. I. Rankin, D. P. Henry, et al., “Plasma and urinary norepinephrine values at extremes of sodium intake in normal man,” Hypertension, 1, 261–266 (1979).
M. Bouvier, L. Farley, and J. de Champlain, “Red blood cell catecholamine levels in normotensive and DOCA-salt hypertensive rats,” Am. J. Physiol., 253, H270–H275 (1987).
V. M. Campese, M. S. Romoff, D. Levitan, et al., “Abnormal relationship between sodium intake and sympathetic nervous system activity in salt-sensitive patients with essential hypertension,” Kidney Int., 21, 371–378 (1982).
T. Fujita, K. Ando, and E. Ogata, “Systemic and regional hemodynamics in patients with salt-sensitive hypertension,” Hypertension, 16, 235–244 (1990).
Y. Huang and D. H. Wang, “Role of renin-angiotensinaldosterone system in salt-sensitive hypertension induced by sensory denervation,” Am. J. Physiol. (Heart Circ. Physiol.), 281, H2143–H2149 (2001).
H. K. Jin, R. H. Yang, J. M. Wyss, et al., “Intrahypothalamic clonidine infusion prevents NaCl-sensitive hypertension,” Hypertension, 18, 224–229 (1991).
J. W. Osborn, B. J. Provo, J. S. Montana 3rd, and K. A. Trostel, “Salt-sensitive hypertension caused by long-term alpha-adrenergic blockade in the rat,” Hypertension, 21, 995–999 (1993).
V. L. Brooks, J. R. Haywood, and A. K. Johnson, “Translation of salt retention to central activation of the sympathetic nervous system in hypertension,” Clin. Exp. Pharmacol. Physiol., 32, 426–432 (2005).
G. M. Toney, Q. H. Chen, M. J. Cato, and S. D. Stocker, “Central osmotic regulation of sympathetic nerve activity,” Acta Physiol. Scand., 177, 43–55 (2003).
J. M. Adams, C. J. Madden, A. F. Sved, and S. D. Stocker, “Increased dietary salt enhances sympathoexcitatory and sympathoinhibitory responses from the rostral ventrolateral medulla,” Hypertension, 50, 354–359 (2007).
Q. H. Chen and G. M. Toney, “AT(1)-receptor blockade in the hypothalamic PVN reduces central hyperosmolalityinduced renal sympathoexcitation,” Am. J. Physiol. (Regul. Integrat. Comp. Physiol.), 281, R1844–R1853 (2001).
J. W. Osborn and B. J. Hornfeldt, “Arterial baroreceptor denervation impairs long-term regulation of arterial pressure during dietary salt loading,” Am. J. Physiol., 275, H1558–H1566 (1998).
R. R. Miselis, “The efferent projections of the subfornical organ of the rat: A circumventricular organ within a neural network subserving water balance,” Brain Res., 230, 1–23 (1981).
C. B. Saper and D. Levisohn, “Afferent connections of the median preoptic nucleus in the rat: Anatomical evidence for a cardiovascular integrative mechanism in the anteroventral third ventricular (AV3V) region,” Brain Res., 288, 21–31 (1983).
J. Ciriello, M. M. Caverson, and F. R. Calaresu, “Lateral hypothalamic and peripheral cardiovascular afferent inputs to ventrolateral medullary neurons,” Brain Res., 347, 173–176 (1985).
Z. J. Gieroba and W. W. Blessing, “Abdominal vagal afferents excite A1 area neurons antidromically activated from the region of the supraoptic nucleus in the rabbit,” Brain Res., 616, 181–187 (1993).
Y. W. Li, Z. J. Gieroba, and W. W. Blessing, “Chemoreceptor and baroreceptor responses of A1 area neurons projecting to supraoptic nucleus,” Am. J. Physiol., 263, R310–R317 (1992).
J. Tanaka, J. Nishimura, F. Kimura, and M. Nomura, “Noradrenergic excitatory inputs to median preoptic neurons in rats,” NeuroReport, 3, 946–948 (1992).
M. J. Westerhaus and A. D. Loewy, “Sympathetic-related neurons in the preoptic region of the rat identified by viral transneuronal labeling,” J. Comp. Neurol., 414, 361–378 (1999).
P. E. Sawchenko and L. W. Swanson, “The organization of forebrain afferents to the paraventricular and supraoptic nuclei of the rat,” J. Comp. Neurol., 218, 121–144 (1983).
A. M. Zardetto-Smith, R. L. Thunhorst, M. Z. Cicha, and A. K. Johnson, “Afferent signaling and forebrain mechanisms in the behavioral control of extracellular fluid volume,” Ann. New York Acad. Sci., 689, 161–176 (1993).
S. D. Stocker and G. M. Toney, “Median preoptic neurons projecting to the hypothalamic paraventricular nucleus respond to osmotic, circulating ANG II and baroreceptor input in the rat,” J. Physiol., 568, 599–615 (2005).
M. J. McKinley, E. Badoer, and B. J. Oldfield, “Intravenous angiotensin II induces fosimmunoreactivity in circumventricular organs of the lamina terminalis,” Brain Res., 594, 295–300 (1992).
B. J. Oldfield, E. Badoer, D. K. Hards, and M. J. McKinley, “Fos production in retrogradely neurons of the lamina terminalis following intravenous infusion of either hypertonic saline or angiotensin II,” Neuroscience, 60, 255–262 (1994).
P. D. Potts, Y. Hirooka, and R. A. Dampney, “Activation of brain neurons by circulating angiotensin II: Direct effects and baroreceptor-mediated secondary effects,” Neuroscience, 90, 581–594 (1999).
N. E. Rowland, B. H. Li, A. K. Rozelle, et al., “Localization of changes in immediate early genes in brain in relation to hydromineral balance: Intravenous angiotensin II,” Brain Res. Bull., 33, 427–436 (1994).
S. D. Stocker and G. M. Toney, “Vagal afferent input alters the discharge of osmotic and ANG II-responsive median preoptic neurons projecting to the hypothalamic paraventricular nucleus,” Brain Res., 1131, 118–128 (2007).
J. Tanaka, M. Nomura, K. Kariya, et al., “Median preoptic neurons projecting to the hypothalamic paraventricular nucleus are sensitive to blood pressure changes,” Brain Res., 605, 338–341 (1993).
J. Tanaka, S. Hatakenaka, H. Miyakubo, and M. Nomura, “Noradrenaline release in the median preoptic nucleus area caused by hemorrhage in the rat,” Brain Res. Bull., 60, 233–240 (2003).
J. T. Cunningham, T. Beltz, R. F. Johnson, and A. K. Johnson, “The effects of ibotenate lesions of the median preoptic nucleus on experimentally-induced and circadian drinking behavior in rats,” Brain Res., 580, 325–330 (1992).
T. W. Gardiner, J. G. Verbalis, and E. M. Stricker, “Impaired secretion of vasopressin and oxytocin in rats after lesions of nucleus medianus,” Am. J. Physiol., 249, R681–R688 (1985).
R. W. Lind and A. K. Johnson, “Subfornical organmedian preoptic connections and drinking and pressor responses to angiotensin II,” J. Neurosci., 2, 1043–1051 (1982).
M. L. Mangiapane, T. N. Thrasher, L. C. Keil, et al., “Deficits in drinking and vasopressin secretion after lesions of the nucleus medianus,” Neuroendocrinology, 37, 73–77 (1983).
T. Ployngam and J. P. Collister, “An intact median preoptic nucleus is necessary for chronic angiotensin II-induced hypertension,” Brain Res., 1162, 69–75 (2007).
T. Ployngam and J. P. Collister, “Role of the median preoptic nucleus in chronic angiotensin II-induced hypertension,” Brain Res., 1238, 75–84 (2008).
D. M. Fine, P. Ariza-Nieto, and J. W. Osborn, “Does whole body autoregulation mediate the hemodynamic responses to increased dietary salt in rats with clamped ANG II?” Am. J. Physiol. (Heart Circ. Physiol.), 285, H2670–H2678 (2003).
K. A. Trostel, S. A. Katz, and J. W. Osborn, “Functional evidence for sympathetic nerve activity in conscious cervical spinal rats,” Am. J. Physiol., 261, R434–R441 (1991).
D. A. Fitts, “Misuse of ANOVA with cumulative intakes,” Appetite, 46, 100–102 (2006).
E. Miyajima and R. D. Bunag, “Dietary salt loading produces baroreflex impairment and mild hypertension in rats,” Am. J. Physiol., 249, H278–H284 (1985).
M. L. Weiss, D. E. Claassen, T. Hirai, and M. J. Kenney, “Nonuniform sympathetic nerve responses to intravenous hypertonic saline infusion,” J. Auton. Nerv. Syst., 57, 109–115 (1996).
K. E. Scrogin, E. T. Grygielko, and V. L. Brooks, “Osmolality: A physiological long-term regulator of lumbar sympathetic nerve activity and arterial pressure,” Am. J. Physiol., 276, R1579–R1586 (1999).
S. D. Stocker, K. J. Keith, and G. M. Toney, “Acute inhibition of the hypothalamic paraventricular nucleus decreases renal sympathetic nerve activity and arterial blood pressure in water-deprived rats,” Am. J. Physiol. (Regul. Integrat. Comp. Physiol.), 286, R719–R725 (2004).
K. L. Freeman and V. L. Brooks, “AT(1) and glutamatergic receptors in paraventricular nucleus support blood pressure during water deprivation,” Am. J. Physiol. (Regul. Integrat. Comp. Physiol.), 292, R1675–R1682 (2007).
P. Shi, S. D. Stocker, and G. M. Toney, “Organum vasculosum laminae terminalis contributes to increased sympathetic nerve activity induced by central hyperosmolality,” Am. J. Physiol. (Regul. Integrat. Comp. Physiol.), 293, R2279–R2289 (2007).
S. L. Hochstenbach and J. Ciriello, “Effect of lesions of forebrain circumventricular organs on c-fos expression in the central nervous system to plasma hypernatremia,” Brain Res., 713, 17–28 (1996).
D. J. Sly, M. J. McKinley, and B. J. Oldfield, “Activation of kidney-directed neurons in the lamina terminalis by alterations in body fluid balance,” Am. J. Physiol. (Regul. Integrat. Comp. Physiol.), 281, R1637–R1646 (2001).
Z. Xu and J. Herbert, “Regional suppression by lesions in the anterior third ventricle of c-fos expression induced by either angiotensin II or hypertonic saline,” Neuroscience, 67, 135–147 (1995).
M. D. Hendel and J. P. Collister, “Sodium balance, arterial pressure, and the role of the subfornical organ during chronic changes in dietary salt,” Am. J. Physiol. (Heart. Circ. Physiol.), 289, H426–H431 (2005).
A. K. Johnson, “The sensory psychobiology of thirst and salt appetite,” Med. Sci. Sports Exerc., 39, 1388–1400 (2007).
C. M. Ferrario, I. Abe, and D. B. Averill, “Sodium and vasopressin modulation of renal sympathetic nerve activity,” Clin. Exp. Hypertension, A. 9, Suppl. 1, 59–74 (1987).
J. G. Verbalis, M. P. Mangione, and E. M. Stricker, “Oxytocin produces natriuresis in rats at physiological plasma concentrations,” Endocrinology, 128, 1317–1322 (1991).
K. E. Scrogin, D. F. McKeogh, and V. L. Brooks, “Is osmolality a long-term regulator of renal sympathetic nerve activity in conscious water-deprived rats?” Am. J. Physiol. (Regul. Integrat. Comp. Physiol.), 282, R560–R568 (2002).
G. F. DiBona, “Neurogenic regulation of renal tubular sodium reabsorption,” Am. J. Physiol., 233, F73–F81 (1977).
H. Morita, K. Ishiki, and H. Hosomi, “Effects of hepatic NaCl receptor stimulation on renal nerve activity in conscious rabbits,” Neurosci. Lett., 123, 1–3 (1991).
H. Morita, T. Matsuda, F. Furuya, et al., “Hepatorenal reflex plays an important role in natriuresis after high-NaCl food intake in conscious dogs,” Circ. Res., 72, 552–559 (1993).
Y. Nishida, I. Sugimoto, H. Morita, et al., “Suppression of renal sympathetic nerve activity during portal vein infusion of hypertonic saline,” Am. J. Physiol., 274, R97–R103 (1998).
Y. Yasuda, K. Honda, H. Negoro, et al., “The contribution of the median preoptic nucleus to renal sympathetic nerve activity increased by intracerebroventricular injection of hypertonic saline in the rat,” Brain Res., 867, 107–114 (2000).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ployngam, T., Katz, S.A. & Collister, J.P. Role of the Median Preoptic Nucleus in Arterial Pressure Regulation and Sodium and Water Homeostasis During High Dietary Salt Intake. Neurophysiology 44, 363–375 (2012). https://doi.org/10.1007/s11062-012-9307-8
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11062-012-9307-8