Summary
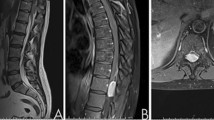
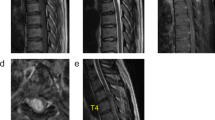
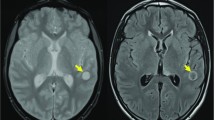
We describe a 29-year-old woman who presented with progressive neck pain, sensory deficit and weakness in both arms. Magnetic resonance imaging (MRI) of the cervical spine revealed an extramedullary tumor with severe spinal cord compression. During surgery an intradural extramedullary tumor was found. Further imaging showed a second lumbar spinal tumor. Microscopy of both tumors showed that both tumors were anaplastic ependymomas, which almost never present as extramedullary tumors. Two years after surgery, an intracranial extracerebral metastasis was found, without evidence of spinal recurrence.
Similar content being viewed by others
References
Akutsu H, Shibata Y, Okazaki M, et al: Intramedullary clear cell ependymoma in the cervical spinal cord: case report Neurosurgery 47:1434–1438, 2000
Duffau H, Gazza M, Kujas M, Fohanno D: Primary intradural extramedullary ependymoma: case report and review of the literature Spine 25:1993–1995, 2000
Fourney DR, Siadati A, Bruner JM, et al: Giant cell ependymoma of the spinal cord: case report and review of the literature J Neurosurg (Spine 1) 100:75–79, 2004
Katoh S, Ikata T, Inoue A, Takahashi M: Intradural extramedullary ependymoma: a case report Spine 20:2036–2038, 1995
Schwartz TH, McCormick PC: Intramedullary ependymomas: clinical pre-sentation, surgical treatment strategies and prognosis J Neuro-Oncol 47:211–218, 2000
Zeidman SM, Ellenbogen RG, Ducker TB: Intradural tumors. In: Clark CR (ed) The Cervical Spine, 3rd edn. Lippincott-Raven Publishers, Philadelphia, pp. 587–601
Robles SGR, Saldaňa C, Boto GR, et al: Intradural extramedullary spinal ependymoma: a benign pathology? Spine 30: E251–254, 2005
Rezai AR, Woo HH, Lee M, et al: Disseminated ependymomas of the central nervous system J Neurosurg 85:618–624, 1996
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Schuurmans, M., Vanneste, J.A., Verstegen, M.J. et al. Spinal extramedullary anaplastic ependymoma with spinal and intracranial metastases. J Neurooncol 79, 57–59 (2006). https://doi.org/10.1007/s11060-005-9114-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-005-9114-9